Voriconazole-induced periostitis
Updates to Article Attributes
Voriconozole-incuded periostitis is a type of drug-induced periostitis and is a rare cause of diffuse bone pain in those on high dose or prolonged voriconozole therapy.
Epidemiology
Voriconozole-induced periostitis primarily occurs in the immunocompromised and transplant patient populations, however it has also been described in immunocompetent hosts 1.
Clinical presentation
Clinical presentation includes:
- diffuse bone pain 1
- dental fluorosis 2
- whitish specks and discolouration
- fractures
- high serum ALP level and plasma fluoride concentration 3,4
Pathology
Voriconazole is a broad-spectrum triazole antifungal medication. Triazole antifungal agents contain varying amounts of fluorine. Voriconazole contains three fluorine atoms, and a 400-mg dose of voriconazole contains a substantial 65 mg of fluoride 5. In comparison, the fluoride content of the municipal tap water is 1 mg per litre 6; and, thus daily fluoride consumption from municipal tap water has been estimated at only 2 to 4 mg per day 6.Absorbed excess fluoride is incorporated into the crystal structure of bony matrix called hydroxyapatite, forming fluorapatite 7. Unlike normal calcium hydroxyapatite, high fluroapatite deposit causes disorganised osteoblastic reaction, resulting in periosteal thickening or ossification, exostosis, and osteosclerosis, a condition known as skeletal fluorosis 2.
Radiographic features
Voriconozole-induced periostitis has been described as having a variable appearance of periosteal reaction including a fluffy, feathery, nodular or irregular morphology on imaging with an asymmetric distribution 8.
Common locations include the clavicles, ribs, proximal long bones, scapula, hands and acetabula.
The mainstay of imaging modality include plain x-ray, CT and nuclear medicine bone scan. Advanced imaging modalities such as MRI and PET can be utilised if the diagnosis remains elusive, however is not recommended as first line 9.
X-ray
- periosteal reaction with elevation and thickening 1
Nuclear medicine
- technetium 99m bone scan demonstrates high radiotracer uptake due to increased osteoblastic activity 1
Treatment and prognosis
Discontinuation of voriconazole usually results in rapid resolution of symptoms. No known mortality has been associated with voriconazole-induced periostitis.
Differential diagnosis
General imaging differential considerations include:
-</ul><h4>Pathology</h4><p>Voriconazole is a broad-spectrum triazole antifungal medication. Triazole antifungal agents contain varying amounts of fluorine. Voriconazole contains three fluorine atoms, and a 400-mg dose of voriconazole contains a substantial 65 mg of fluoride <sup>5</sup>. In comparison, the fluoride content of the municipal tap water is 1 mg per litre <sup><font size="1">6</font></sup>; and, thus daily fluoride consumption from municipal tap water has been estimated at only 2 to 4 mg per day <sup><font size="1">6</font></sup>.<br><br>Absorbed excess fluoride is incorporated into the crystal structure of bony matrix called hydroxyapatite, forming fluorapatite <sup><font size="1">7</font></sup>. Unlike normal calcium hydroxyapatite, high fluroapatite deposit causes disorganised osteoblastic reaction, resulting in periosteal thickening or ossification, <a title="Exostosis" href="/articles/exostosis">exostosis</a>, and osteosclerosis, a condition known as skeletal fluorosis<sup> 2</sup>. </p><h4>Radiographic features</h4><p>Voriconozole-induced periostitis has been described as having a variable appearance of periosteal reaction including a fluffy, feathery, nodular or irregular morphology on imaging with an asymmetric distribution <sup>8</sup>. </p><p>Common locations include the clavicles, ribs, proximal long bones, scapula, hands and acetabula.</p><p>The mainstay of imaging modality include plain x-ray, CT and nuclear medicine bone scan. Advanced imaging modalities such as MRI and PET can be utilised if the diagnosis remains elusive, however is not recommended as first line <sup>9</sup>.</p><h5>X-ray</h5><ul><li>-<a title="Periosteal reaction" href="/articles/periosteal-reaction">periosteal reaction</a> with elevation and thickening <sup>1</sup>- +</ul><h4>Pathology</h4><p>Voriconazole is a broad-spectrum triazole antifungal medication. Triazole antifungal agents contain varying amounts of fluorine. Voriconazole contains three fluorine atoms, and a 400-mg dose of voriconazole contains a substantial 65 mg of fluoride <sup>5</sup>. In comparison, the fluoride content of the municipal tap water is 1 mg per litre <sup>6</sup>; and, thus daily fluoride consumption from municipal tap water has been estimated at only 2 to 4 mg per day <sup>6</sup>.<br><br>Absorbed excess fluoride is incorporated into the crystal structure of bony matrix called hydroxyapatite, forming fluorapatite <sup>7</sup>. Unlike normal calcium hydroxyapatite, high fluroapatite deposit causes disorganised osteoblastic reaction, resulting in periosteal thickening or ossification, <a href="/articles/exostosis">exostosis</a>, and osteosclerosis, a condition known as skeletal fluorosis<sup> 2</sup>. </p><h4>Radiographic features</h4><p>Voriconozole-induced periostitis has been described as having a variable appearance of periosteal reaction including a fluffy, feathery, nodular or irregular morphology on imaging with an asymmetric distribution <sup>8</sup>. </p><p>Common locations include the clavicles, ribs, proximal long bones, scapula, hands and acetabula.</p><p>The mainstay of imaging modality include plain x-ray, CT and nuclear medicine bone scan. Advanced imaging modalities such as MRI and PET can be utilised if the diagnosis remains elusive, however is not recommended as first line <sup>9</sup>.</p><h5>X-ray</h5><ul><li>
- +<a href="/articles/periosteal-reaction">periosteal reaction</a> with elevation and thickening <sup>1</sup>
-</li></ul><h5> </h5><h4>Treatment and prognosis</h4><p>Discontinuation of voriconazole usually results in rapid resolution of symptoms. No known mortality has been associated with voriconazole-induced periostitis.</p><h4>Differential diagnosis</h4><p>General imaging differential considerations include:</p><ul>-<li><a title="Hypertrophic osteoarthropathy" href="/articles/hypertrophic-osteoarthropathy">hypertrophic osteoarthropathy</a></li>-<li><a title="Metastases to bone" href="/articles/bone-metastases-1">metastases</a></li>-<li><a title="Thyroid acropachy" href="/articles/thyroid-acropachy">thyroid aropachy</a></li>- +</li></ul><h4>Treatment and prognosis</h4><p>Discontinuation of voriconazole usually results in rapid resolution of symptoms. No known mortality has been associated with voriconazole-induced periostitis.</p><h4>Differential diagnosis</h4><p>General imaging differential considerations include:</p><ul>
- +<li><a href="/articles/hypertrophic-osteoarthropathy">hypertrophic osteoarthropathy</a></li>
- +<li><a href="/articles/bone-metastases-1">metastases</a></li>
- +<li><a href="/articles/thyroid-acropachy">thyroid aropachy</a></li>
References changed:
- 1. Guarascio A, Bhanot N, Min Z. Voriconazole-Associated Periostitis: Pathophysiology, Risk Factors, Clinical Manifestations, Diagnosis, and Management. World J Transplant. 2021;11(9):356-71. <a href="https://doi.org/10.5500/wjt.v11.i9.356">doi:10.5500/wjt.v11.i9.356</a> - <a href="https://www.ncbi.nlm.nih.gov/pubmed/34631468">Pubmed</a>
- 2. Peres Buzalaf C, de Lima Leite A, Buzalaf M. CHAPTER 4. Fluoride Metabolism. Food and Nutritional Components in Focus. 2015;:54-72. <a href="https://doi.org/10.1039/9781782628507-00054">doi:10.1039/9781782628507-00054</a>
- 3. Khokher M & Dandona P. Fluoride Stimulates [3H]thymidine Incorporation and Alkaline Phosphatase Production by Human Osteoblasts. Metabolism. 1990;39(11):1118-21. <a href="https://doi.org/10.1016/0026-0495(90)90081-m">doi:10.1016/0026-0495(90)90081-m</a>
- 4. Buzalaf M & Whitford G. Fluoride Metabolism. Monogr Oral Sci. 2011;22:20-36. <a href="https://doi.org/10.1159/000325107">doi:10.1159/000325107</a> - <a href="https://www.ncbi.nlm.nih.gov/pubmed/21701189">Pubmed</a>
- 5. Wermers R, Cooper K, Razonable R et al. Fluoride Excess and Periostitis in Transplant Patients Receiving Long-Term Voriconazole Therapy. Clin Infect Dis. 2011;52(5):604-11. <a href="https://doi.org/10.1093/cid/ciq188">doi:10.1093/cid/ciq188</a> - <a href="https://www.ncbi.nlm.nih.gov/pubmed/21239842">Pubmed</a>
- 6. From the Centers for Disease Control. Public Health Service Report on Fluoride Benefits and Risks. JAMA. 1991;266(8):1061-2, 1066. - <a href="https://www.ncbi.nlm.nih.gov/pubmed/1865532">Pubmed</a>
- 7. Lindsay R. Fluoride and Bone--Quantity Versus Quality. N Engl J Med. 1990;322(12):845-6. <a href="https://doi.org/10.1056/NEJM199003223221210">doi:10.1056/NEJM199003223221210</a> - <a href="https://www.ncbi.nlm.nih.gov/pubmed/2308618">Pubmed</a>
- 8. Cubbison A, Obara P, Demos T. Voriconazole-Induced Periostitis: A Radiographic Progression. A J Diagn Imaging. 2017;1(1):31. <a href="https://doi.org/10.5455/ajdi.20170608104413">doi:10.5455/ajdi.20170608104413</a>
- 9. Tan I, Lomasney L, Stacy G, Lazarus M, Mar W. Spectrum of Voriconazole-Induced Periostitis With Review of the Differential Diagnosis. AJR Am J Roentgenol. 2019;212(1):157-65. <a href="https://doi.org/10.2214/AJR.18.19991">doi:10.2214/AJR.18.19991</a> - <a href="https://www.ncbi.nlm.nih.gov/pubmed/30403528">Pubmed</a>
Systems changed:
- Musculoskeletal
Image 1 Nuclear medicine (Lower leg static and SPECT/CT) ( create )
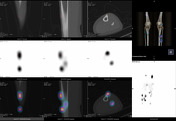
Image 2 X-ray (Frontal) ( create )

Image 3 X-ray (Oblique) ( create )







 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.