Air-space opacification (summary)
Updates to Article Attributes
This
-
this is a basic article
which is aimed atfor medical students and non-radiologistsin training grades. If you've arrived here by accident, and need more information, head to the mainconsolidationarticle.
Consolidation is a radiological sign that refers to non-specific air-space opacification on a chest radiograph or chest CT. Many things can fill the alveolar spaces, including fluid (heart failure), pus (pneumonia), blood (pulmonary haemorrhage) and cells (lung cancer).
Clinical presentation
Presentation is dependent on the underlying cause. Symptoms may include shortness of breath, productive cough +/- haemoptosis, fevers/chills/rigors and weight loss, particularly if malignancy is suspected.
On examination, decreased chest expansion may be noted on the affected side and dullness to percussion. On auscultation, findings include bronchial breath sounds, inspiratory crackles or crepitations, increased vocal resonance and pleural rub.
Pathology
Pneumonia with pus filling the alveoli is the most common cause of acute consolidation. Other acute causes include blood from haemorrhage or contusions and transudative fluid from pulmonary oedema seen in heart failure.
Chronic consolidation will be likely due to a malignant process. Bronchoalveolar carcinoma, lymphoma and lung neoplasms with post-obstructive pneumonia result in malignant cells causing the consolidation seen on radiograph. Chronic post-infection diseases such as organising penumonia or eosinophilic pneumonia as also causes, with alveolar proteinosis a rare cause resulting in alveoli filled with protein.
Radiographic features
Consolidated areas are radio opaque on chest radiograph and chest CT compared to normally air filled lung tissue. The distribution pattern of consolidation can aid in narrowing the potential differential diagnosis.
Lobar consolidation
Where increased density/opacity is seen in individual lung lobes. Sharp delineation can be seen when consolidation reaches a fissure, since it does not cross. Air bronchograms can also be seen due to bronchi becoming visible against the dense diseased tissue. Volume loss is usually not seen.
Diffuse consolidation
Most commonly due to heart failure, resulting in other signs such increased cardiac size, Kerley B-lines, redistribution on pulmonary blood flow and pleural fluid. Other findings can include multiple ill defined opacities progressing to diffuse spread seen in bronchopenumonia and "white out" of a lung due to progressive consolidation from bronchoalveolar carcinoma.
Multi-focal consolidation
Multiple areas of opacity seen throughout the lung most often is due to bronchopneumonia, starting from bronchi and spreading outwards. Usually ill defined with peripheral distribution. Neoplasms such as a primary malignancy or metastasis can also cause this picture.
Treatment and prognosis
Treatment and prognosis is entirely dependent on the underlying cause, as consolidation seen on radiograph or CT must be clinically correlated with the patient's history, examination and other investigations. Other prognostic factors include the patients pre-morbid state and availability to treatment options.
See also
-<p>This is a <em>basic article</em> which is aimed at medical students and non-radiologists in training grades. If you've arrived here by accident, and need more information, head to the main <a href="/articles/air-space-opacification-1">consolidation</a> article.</p><p><strong>Consolidation</strong> is a radiological sign that refers to non-specific air-space opacification on a chest radiograph or chest CT. Many things can fill the alveolar spaces, including fluid (heart failure), pus (pneumonia), blood (pulmonary haemorrhage) and cells (lung cancer).</p><h4>Clinical presentation</h4><p>Presentation is dependent on the underlying cause. Symptoms may include shortness of breath, productive cough +/- haemoptosis, fevers/chills/rigors and weight loss, particularly if malignancy is suspected.</p><p>On examination, decreased chest expansion may be noted on the affected side and dullness to percussion. On auscultation, findings include bronchial breath sounds, inspiratory crackles or crepitations, increased vocal resonance and pleural rub.</p><h4>Pathology</h4><p>Pneumonia with pus filling the alveoli is the most common cause of acute consolidation. Other acute causes include blood from haemorrhage or contusions and transudative fluid from pulmonary oedema seen in heart failure.</p><p>Chronic consolidation will be likely due to a malignant process. Bronchoalveolar carcinoma, lymphoma and lung neoplasms with post-obstructive pneumonia result in malignant cells causing the consolidation seen on radiograph. Chronic post-infection diseases such as organising penumonia or eosinophilic pneumonia as also causes, with alveolar proteinosis a rare cause resulting in alveoli filled with protein.</p><h4>Radiographic features</h4><p>Consolidated areas are radio opaque on chest radiograph and chest CT compared to normally air filled lung tissue. The distribution pattern of consolidation can aid in narrowing the potential differential diagnosis.</p><h5>Lobar consolidation</h5><p>Where increased density/opacity is seen in individual lung lobes. Sharp delineation can be seen when consolidation reaches a fissure, since it does not cross. Air bronchograms can also be seen due to bronchi becoming visible against the dense diseased tissue. Volume loss is usually not seen.</p><h5>Diffuse consolidation</h5><p>Most commonly due to heart failure, resulting in other signs such increased cardiac size, Kerley B-lines, redistribution on pulmonary blood flow and pleural fluid. Other findings can include multiple ill defined opacities progressing to diffuse spread seen in bronchopenumonia and "white out" of a lung due to progressive consolidation from bronchoalveolar carcinoma. </p><h5>Multi-focal consolidation</h5><p>Multiple areas of opacity seen throughout the lung most often is due to bronchopneumonia, starting from bronchi and spreading outwards. Usually ill defined with peripheral distribution. Neoplasms such as a primary malignancy or metastasis can also cause this picture.</p><h4>Treatment and prognosis</h4><p>Treatment and prognosis is entirely dependent on the underlying cause, as consolidation seen on radiograph or CT must be clinically correlated with the patient's history, examination and other investigations. Other prognostic factors include the patients pre-morbid state and availability to treatment options.</p><p> </p>- +<ul><li>this is a <em>basic article</em> for medical students and non-radiologists</li></ul><p><strong>Consolidation</strong> is a radiological sign that refers to non-specific air-space opacification on a chest radiograph or chest CT. Many things can fill the alveolar spaces, including fluid (heart failure), pus (pneumonia), blood (pulmonary haemorrhage) and cells (lung cancer).</p><h4>Clinical presentation</h4><p>Presentation is dependent on the underlying cause. Symptoms may include shortness of breath, productive cough +/- haemoptosis, fevers/chills/rigors and weight loss, particularly if malignancy is suspected.</p><p>On examination, decreased chest expansion may be noted on the affected side and dullness to percussion. On auscultation, findings include bronchial breath sounds, inspiratory crackles or crepitations, increased vocal resonance and pleural rub.</p><h4>Pathology</h4><p>Pneumonia with pus filling the alveoli is the most common cause of acute consolidation. Other acute causes include blood from haemorrhage or contusions and transudative fluid from pulmonary oedema seen in heart failure.</p><p>Chronic consolidation will be likely due to a malignant process. Bronchoalveolar carcinoma, lymphoma and lung neoplasms with post-obstructive pneumonia result in malignant cells causing the consolidation seen on radiograph. Chronic post-infection diseases such as organising penumonia or eosinophilic pneumonia as also causes, with alveolar proteinosis a rare cause resulting in alveoli filled with protein.</p><h4>Radiographic features</h4><p>Consolidated areas are radio opaque on chest radiograph and chest CT compared to normally air filled lung tissue. The distribution pattern of consolidation can aid in narrowing the potential differential diagnosis.</p><h5>Lobar consolidation</h5><p>Where increased density/opacity is seen in individual lung lobes. Sharp delineation can be seen when consolidation reaches a fissure, since it does not cross. Air bronchograms can also be seen due to bronchi becoming visible against the dense diseased tissue. Volume loss is usually not seen.</p><h5>Diffuse consolidation</h5><p>Most commonly due to heart failure, resulting in other signs such increased cardiac size, Kerley B-lines, redistribution on pulmonary blood flow and pleural fluid. Other findings can include multiple ill defined opacities progressing to diffuse spread seen in bronchopenumonia and "white out" of a lung due to progressive consolidation from bronchoalveolar carcinoma. </p><h5>Multi-focal consolidation</h5><p>Multiple areas of opacity seen throughout the lung most often is due to bronchopneumonia, starting from bronchi and spreading outwards. Usually ill defined with peripheral distribution. Neoplasms such as a primary malignancy or metastasis can also cause this picture.</p><h4>Treatment and prognosis</h4><p>Treatment and prognosis is entirely dependent on the underlying cause, as consolidation seen on radiograph or CT must be clinically correlated with the patient's history, examination and other investigations. Other prognostic factors include the patients pre-morbid state and availability to treatment options.</p><h4>See also</h4><ul><li><a title="Lung consolidation" href="/articles/air-space-opacification-1">consolidation</a></li></ul>
Tags changed:
- curriculum
Image ( create )
Image 1 X-ray (Frontal) ( create )
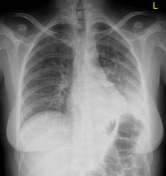
Image 2 X-ray (Frontal) ( create )

Image 3 X-ray (Frontal) ( create )

Image 4 X-ray (Frontal) ( create )








 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.