MRI - Pituitary MRI
When can you confidently predict cavernous sinus invasion?
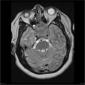
It is not as easy as it sounds, as the medial wall of the cavernous sinus can be significantly distorted and pushed laterally without frank invasion. Using the degree of encasement of the internal carotid artery has been shown to be useful. Less than 90 degrees makes involvement of the sinus very unlikely, where as greater than 270 degrees makes involvement almost certain. In this case both carotids are completely surrounded.
Which type of tumour most often invades the cavernous sinus and what can be done to further confirm this?
Prolactin secreting tumours are most frequently responsible for cavernous sinus extension. Typically prolactin level increase significantly (by orders of magnitude) when the tumour gains access to the sinus, and thus performing a serum prolactin level is useful.
What treatment options exist for prolactinomas?
Medical management of prolactinomas relies on administering a dopamine agonist (e.g. bromocriptine or cabergoline). Although it can dramatically reduce the size of a macroadenoma, it has been associated with increased incidence of haemorrhage into the tumour (especially bromocriptine). If significant visual impairment is present then surgical debulking may be necessary.
Why do dopamine agonists work?
Unlike other anterior pituitary hormones which are controlled by releasing factors produced by the hypothalamus, prolactin is tonically inhibited by prolactine inhibitory factor (which is dopamine).
What is 'stalk effect'?
Distortion of the infundibulum by an adjacent mass can result in interruption of normal hypothalamic-pituitary portal circulation. The most common effect is a mildly elevated prolactin level due to absence of the normal inhibition of its release by prolactin inhibitory factor (dopamine).
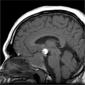
A large predominantly solid multilobulated mass measuring 3.6 x 3.8 x 4.1cm is centred in an expanded sella, with no separate pituitary gland identified. The mass is predominantly isointense to cerebral parenchyma on T1 and T2 weighted imaging and heterogenously contrast enhancing. No diffusion restriction. It extends into sphenoid and posterior ethmoid sinuses, and the suprasellar and interpeduncular cisterns, compressing and displacing superiorly the right aspect of the optic chiasm and surrounds the cavernous carotids within the cavernous sinuses without cavernous carotid narrowing. The soft tissue reaches the orbital apices without intraorbital invasion.
A 12mm T1 heterogeneously hyperintense, peripherally T2 hypointense component lies in the suprasellar cistern and just above the level of the tip of the basilar artery. The MRA examination demonstrates that the T1 hyperintense components is separate from the basilar tip.
No hydrocephalus although the floor of the 3rd ventricle is distorted.