Alveolar haemorrhage and possible lymphocytic interstitial pneumonitis in systemic lupus erythematosus
Presentation
History of SLE, presents with haemoptysis and shortness of breath.
Patient Data
Admission CXR
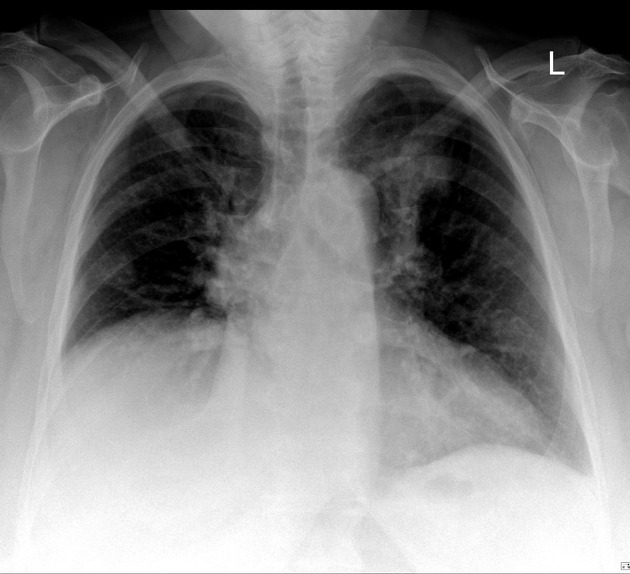
There is a patchy airspace infiltrate in the left upper zone.
CT pulmonary angiography




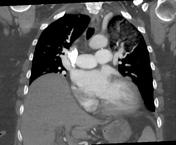


Numerous intrapulmonary cysts, the largest measuring 3 cm in the left lower lobe. Left upper lobe ground glass opacity occupies most of the apical segment. Regional cysts demonstrate air-fluid levels. Several pulmonary nodules: 17 x 14mm right lower lobe anterior segment (image 23 se 6); this nodule is of fluid attenuation 7 x 7mm right upper lobe (image 14 se 6) 6 x 6mm right apex (image 9 se 6) 7 x 6mm right lower lobe anterior basal segment (image 25 se 6) No thoracic lymphadenopathy. Moderately severe cardiomegaly.
Dense pleural calcification, right medial basal region. Mild central pulmonary arterial dilation. 2 low attenuation hepatic lesions: 14mm segment 2 anterior subcapsular, 8mm segment 7 posterior subcapsular
CONCLUSION:
Appearances suggest lymphoid interstitial pneumonia. The left upper lobe GGO has a relatively wide DDx including haemorrhage and less likely aspiration or infection. Malignancy is considered unlikely.
Pulmonary hypertension.
The patient deteriorated &...
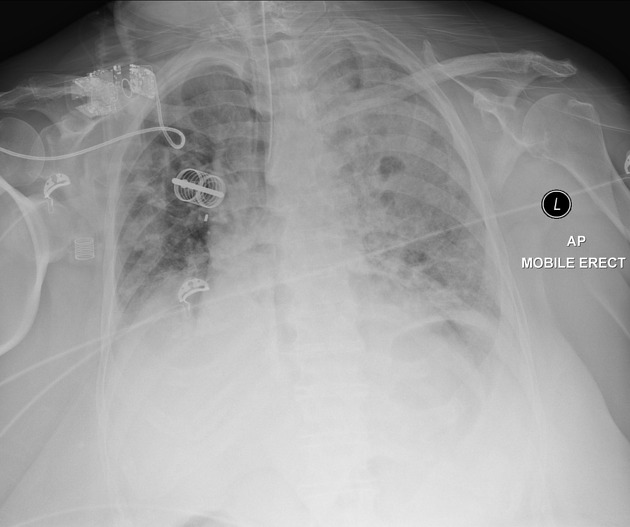
The patient deteriorated & was intubated. Haemoptysis became massive.
Extensive airspace opacification L>R compatible with alveolar haemorrhage. ETT adequate.
Case Discussion
The patient deteriorated; the haemoptysis became massive and the patient died shortly after ICU admission. A post-mortem was carried out and confirmed massive alveolar haemorrhage, a recognised complication of systemic lupus erythematosus.
The central lung cysts are suggestive of lymphocytic interstitial pneumonitis, of which SLE is one of the associations.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.