Cerebral cavernous venous malformations, also commonly known as cavernous hemangiomas or cavernomas, are common cerebral vascular malformations, usually with characteristic appearances on MRI. It is the third most common cerebral vascular malformation after developmental venous anomaly and capillary telangiectasia.
Cavernous malformations are found throughout the body. This article focuses on cerebral cavernous venous malformations. For a general discussion and links to cavernomas in other locations, please refer to the general article on cavernous venous malformation.
On this page:
Terminology
Many alternative terms have been used over the years including cavernous hemangioma, cerebral cavernous malformation or simply cavernoma. As these lesions are not neoplastic, it has been argued that the terms 'hemangioma' and 'cavernoma' should be avoided. Additionally, it is important to note that according to newer nomenclature (ISSVA classification of vascular anomalies) these lesions are now officially termed slow flow venous malformations.
Having said all that, it is probably helpful in reports to include the word 'cavernous' as this term is ubiquitous in the literature and most familiar to many clinicians.
For clarity and brevity, the term cavernous malformation is used for the remainder of this article.
Epidemiology
Most patients who present symptomatically do so at 40-60 years of age. Most patients have single lesions. Multiple lesions may be familial and screening of family members may be indicated (see familial multiple cavernous malformation syndrome). Additionally, cavernous malformations, along with capillary telangiectasias, are commonly seen following cerebral radiotherapy 3. Around 40% (range 20-50%) of cavernous malformations are incidental findings on neuro-imaging 13,14.
Clinical presentation
The majority of lesions remain asymptomatic throughout life and are found incidentally. Presentation due to hemorrhage may cause a headache, seizure or focal neurological deficit. The risk of hemorrhage is 1% per patient-year for familial cases, somewhat less for sporadic lesions, and very rare (<0.1% per patient-year) for incidental lesions 14.
Pathology
Histologically cavernous malformations are composed of a "mulberry-like" cluster of hyalinized dilated thin-walled capillaries, with surrounding hemosiderin 3. These vessels are thrombosed to varying degrees. Unlike CNS capillary telangiectasia, there is no normal brain between the interstices of these lesions.
Associations
On occasion, they are intimately associated with a developmental venous anomaly (DVA), in which case they are known as a mixed vascular malformation.
Radiographic features
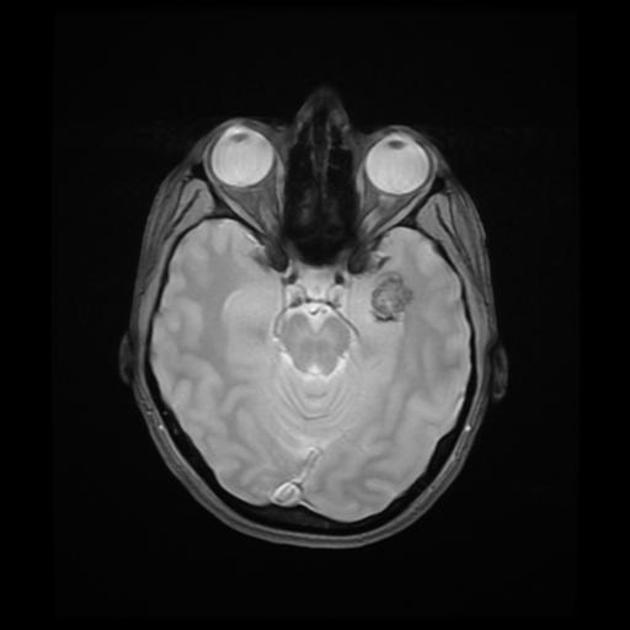
Cerebral cavernous malformations tend to be supratentorial (~80% cases) but can be found anywhere including the brainstem. They are usually solitary, although up to one-third of patients with sporadic lesions have more than one 2.
Brain MRI with SWI or GRE is recommended for the investigation and follow-up of cerebral cavernous malformations 14. For investigation of new symptoms suspicious for cerebral hemorrhage, CT can be used within 1 week of onset and MRI after 1 week 14.
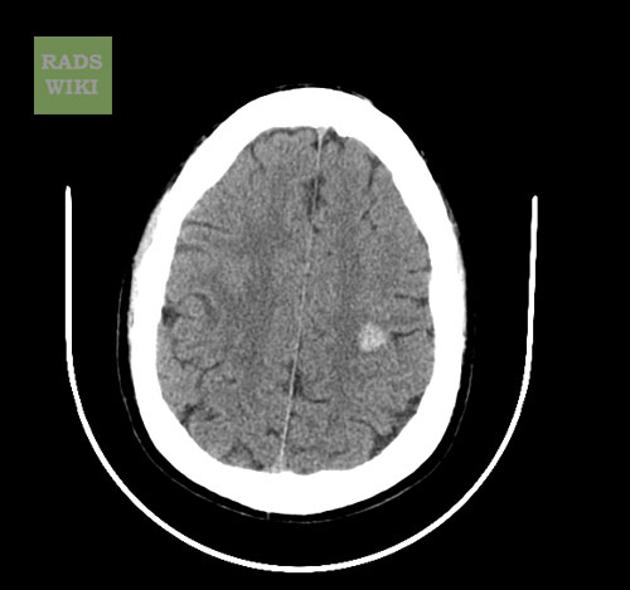
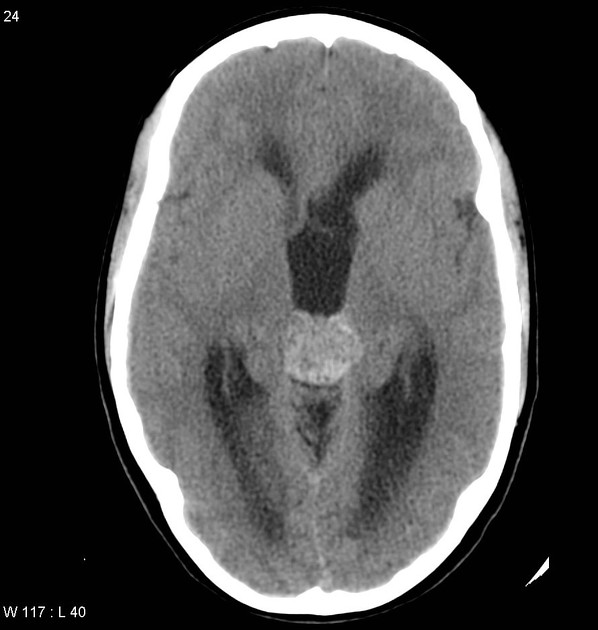
CT
Unless large, these lesions are difficult to see on CT. They may be well-defined and round in shape. If large they appear as a region of hyperdensity resembling blood products and speckles of calcification. They show minimal or no enhancement. They are not usually associated with edema or mass effect, except if there has been a recent bleed, then they may be surrounded by a mantle of edema 15.
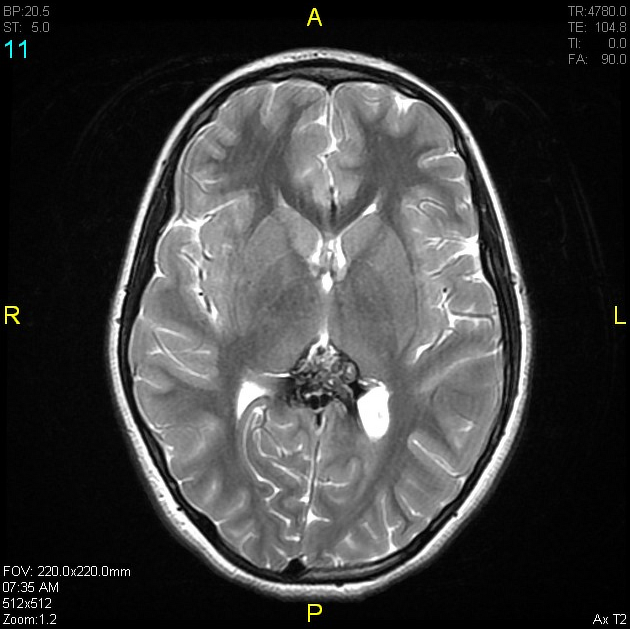
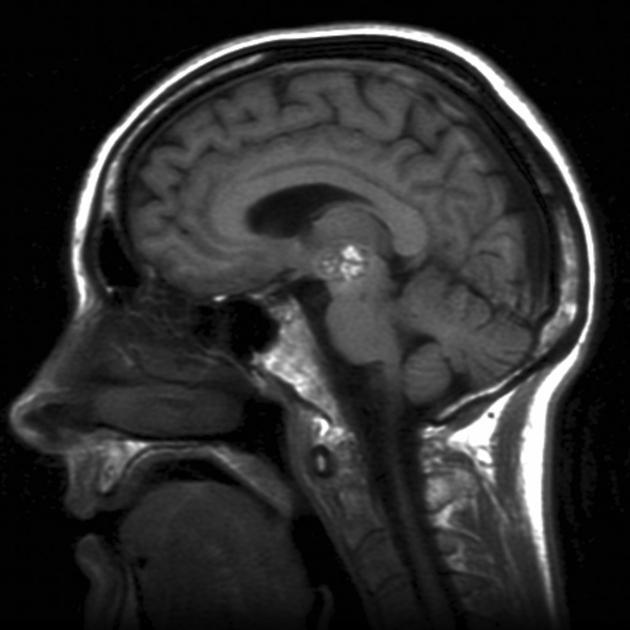
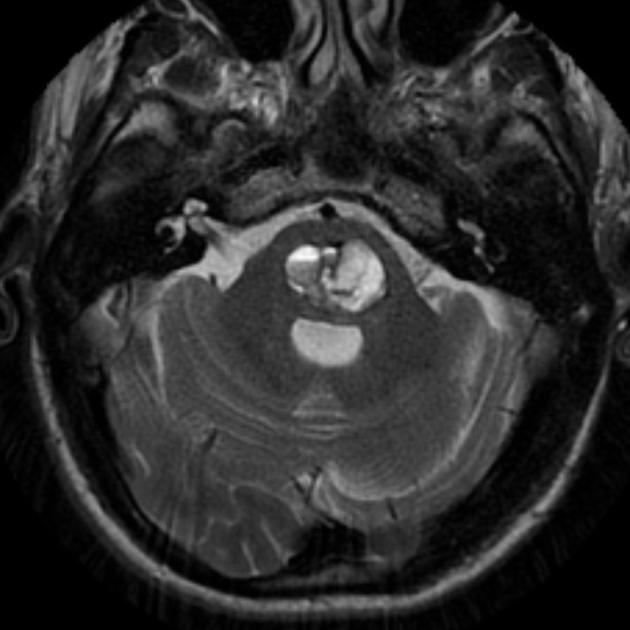
MRI
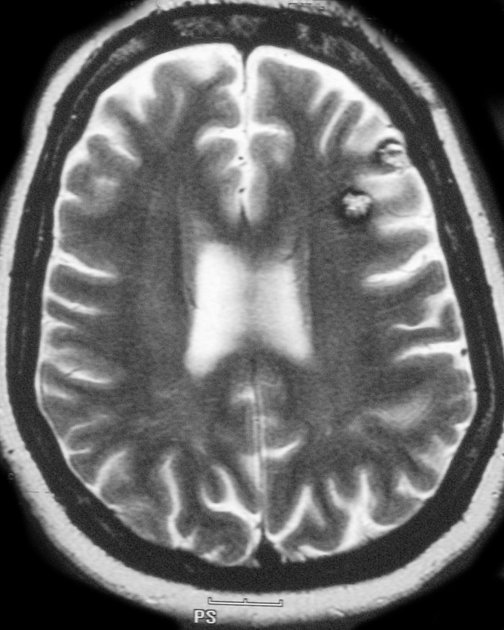
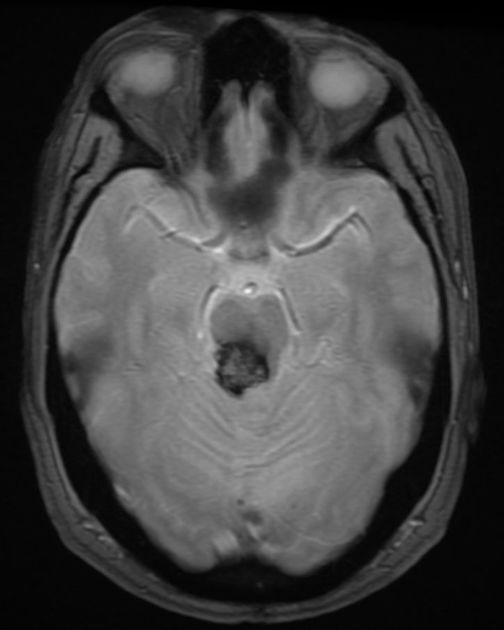
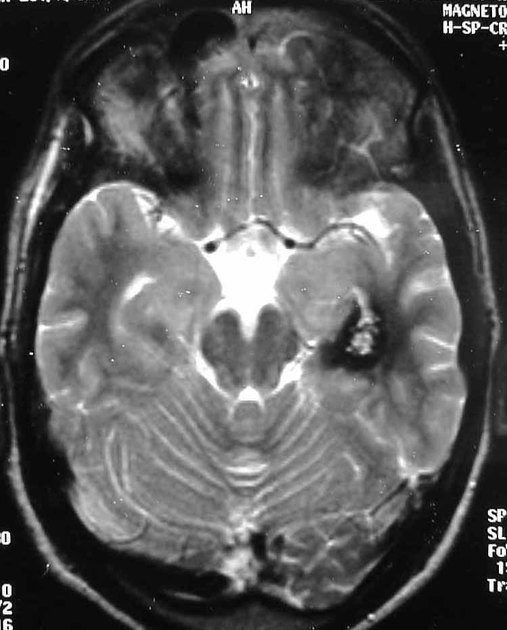
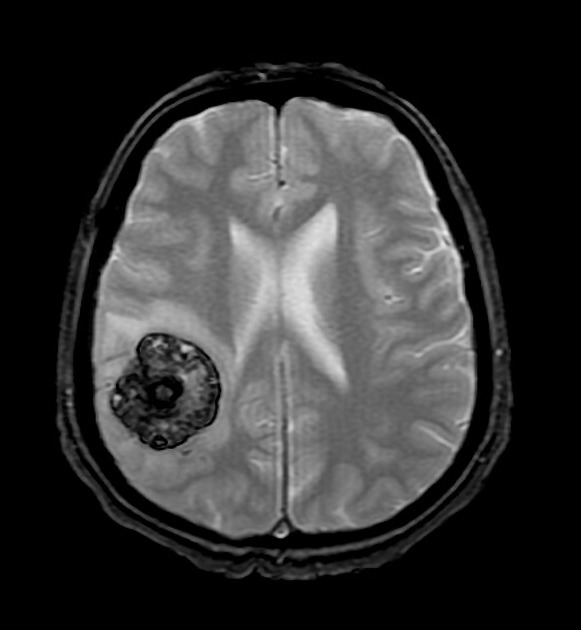
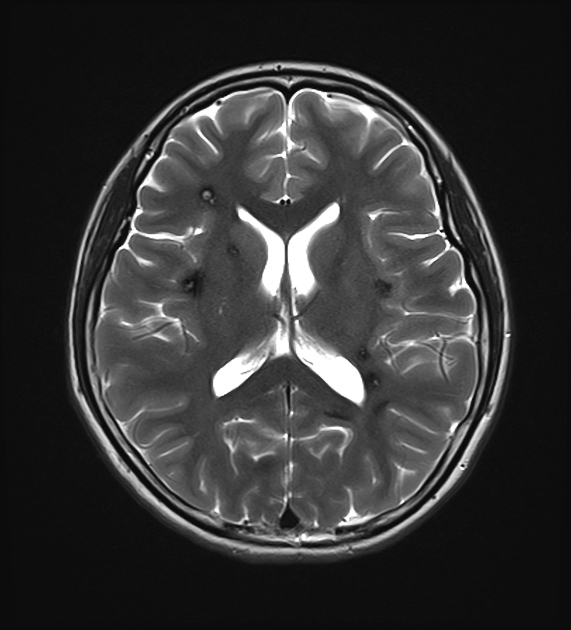
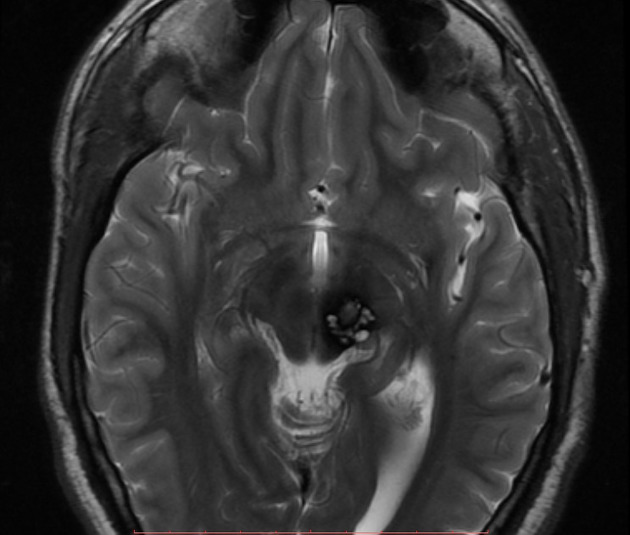
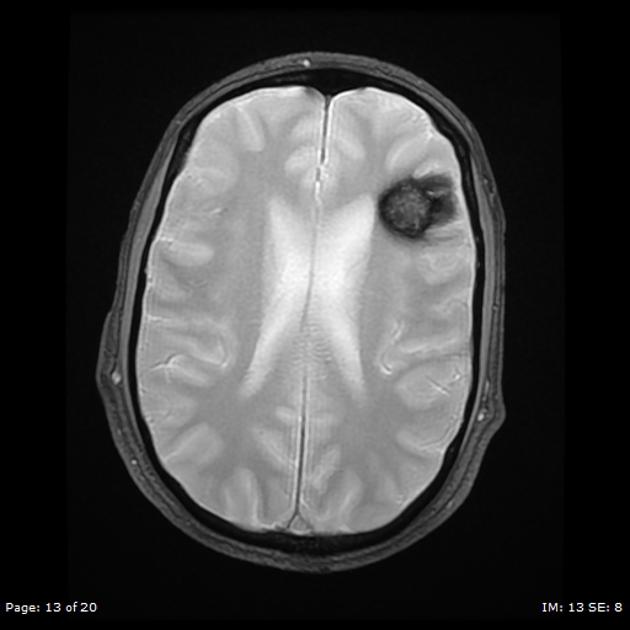
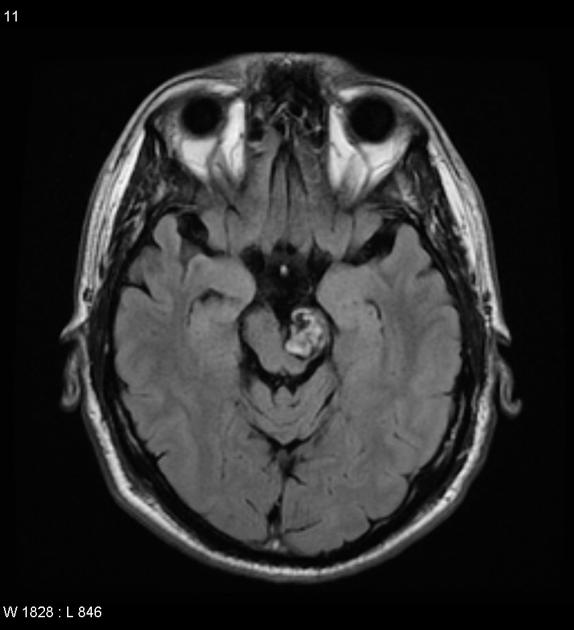
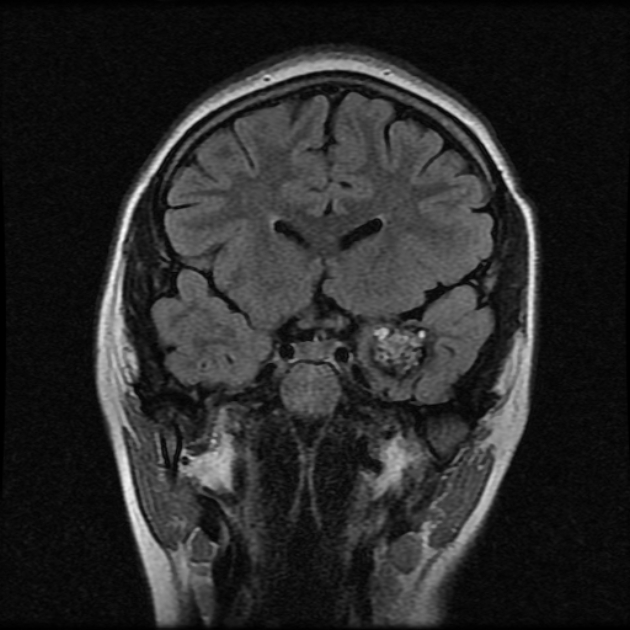
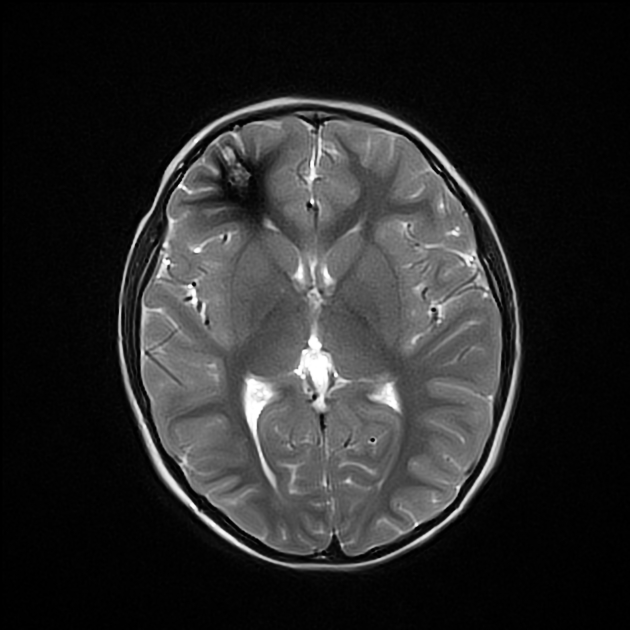
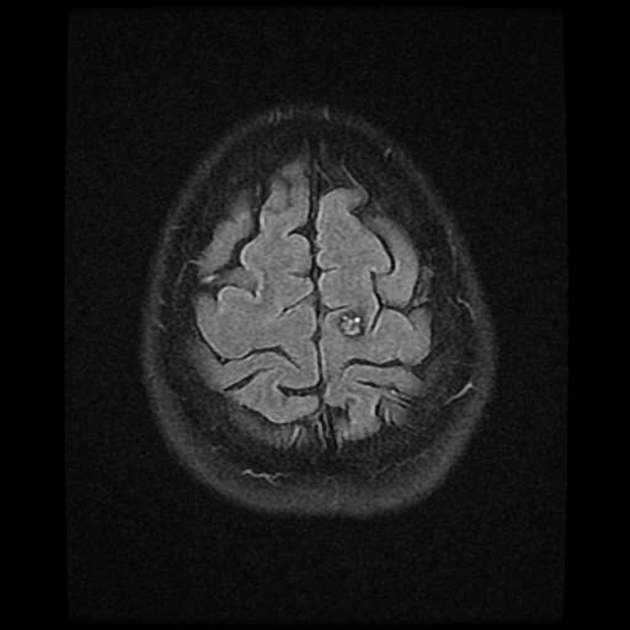
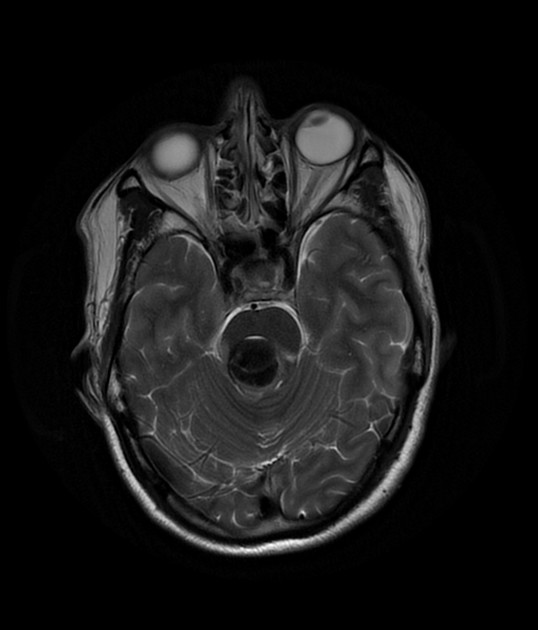
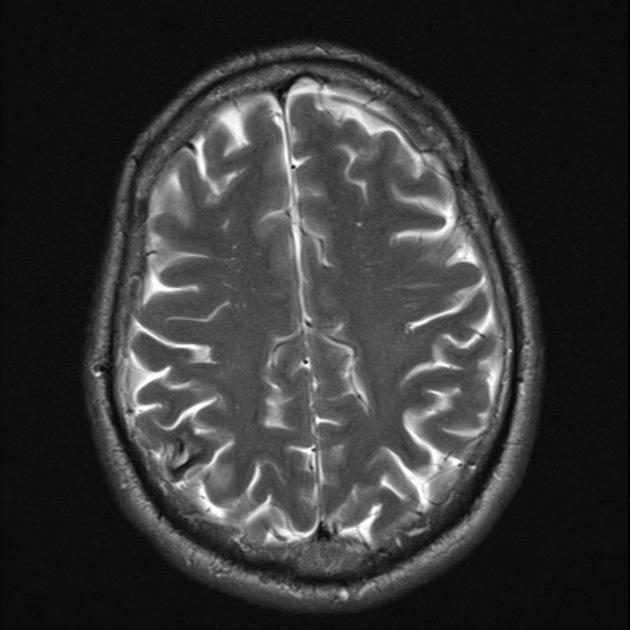
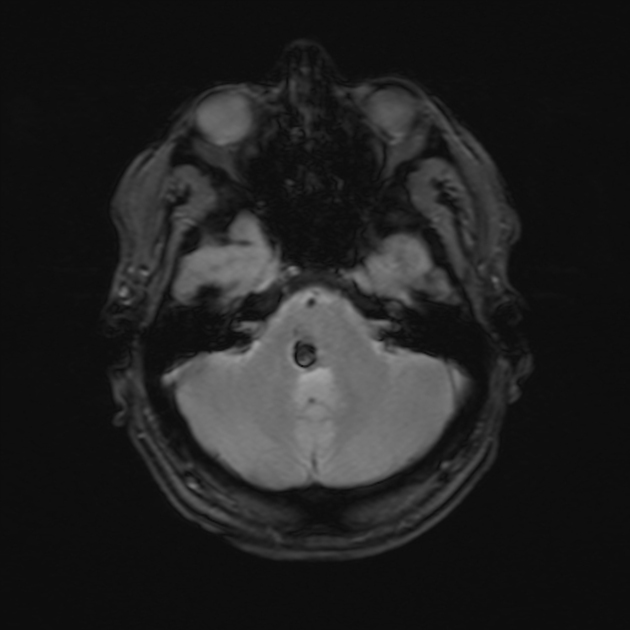
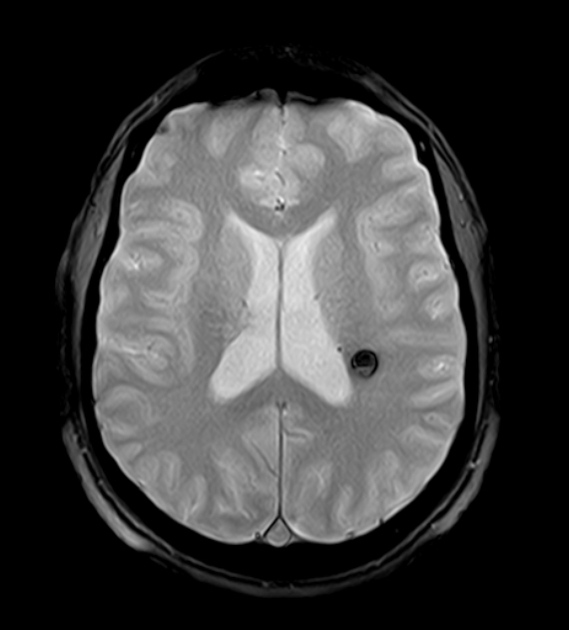
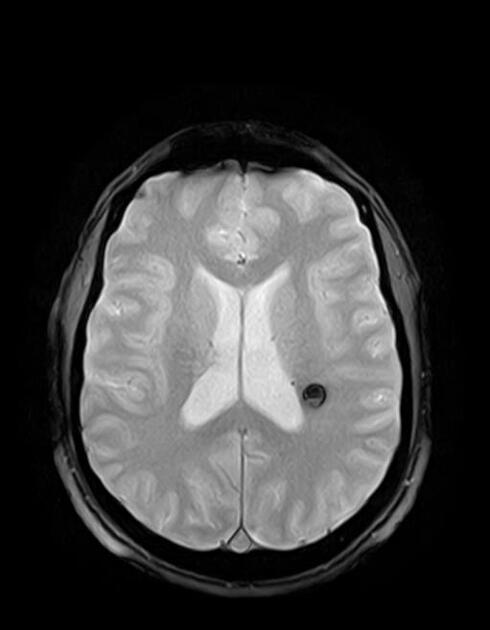
MRI is the modality of choice, demonstrating a characteristic “popcorn” or "berry" appearance with a rim of signal loss due to hemosiderin.
-
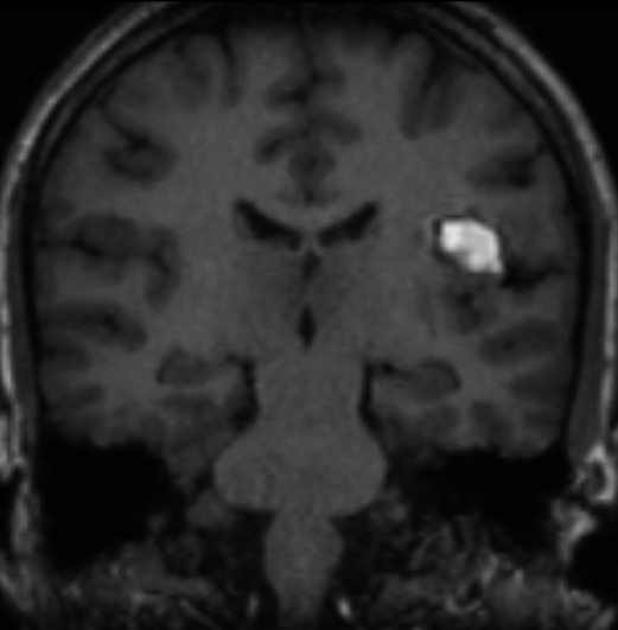
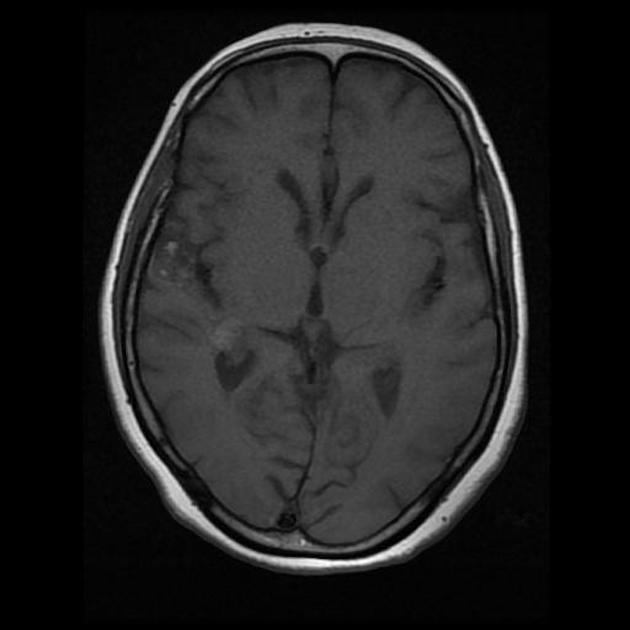
T1
varied signal depending on the age of the blood products, small fluid-fluid levels may be evident
-
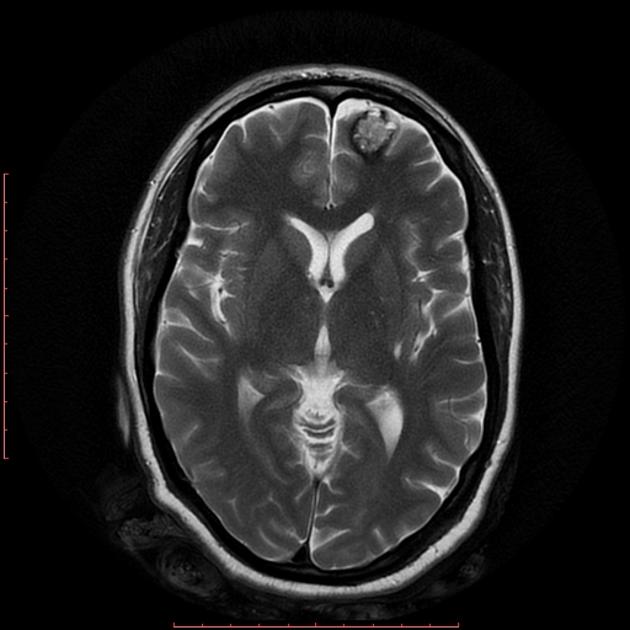
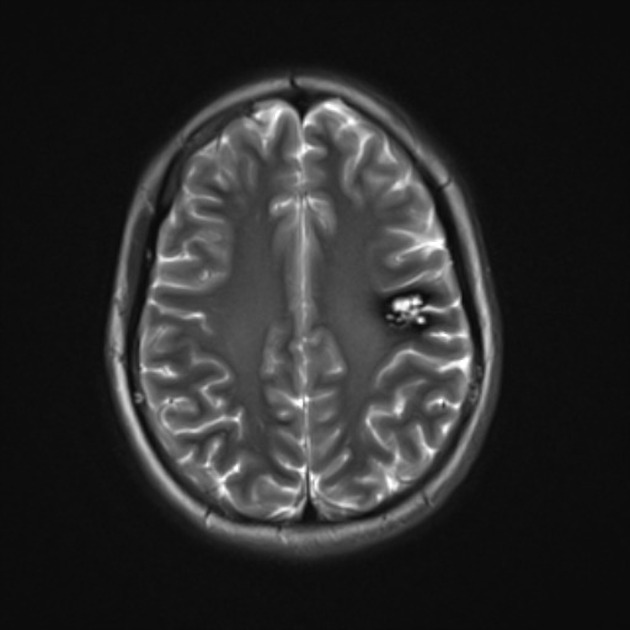
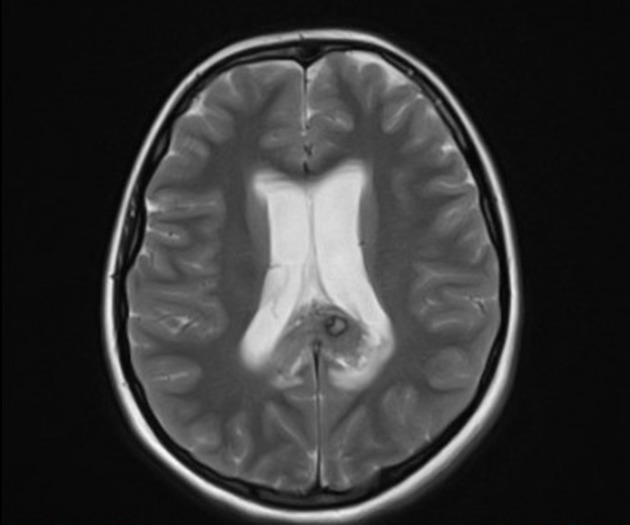
T2
hypointense rim
varied signal internally depending on the age of blood products
blood locules with fluid-fluid levels may be seen
if a recent bleed has occurred, surrounding edema may be present
-
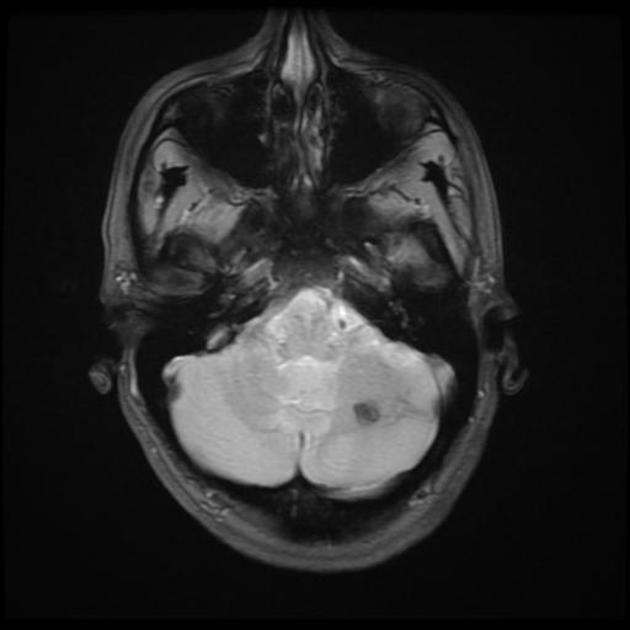
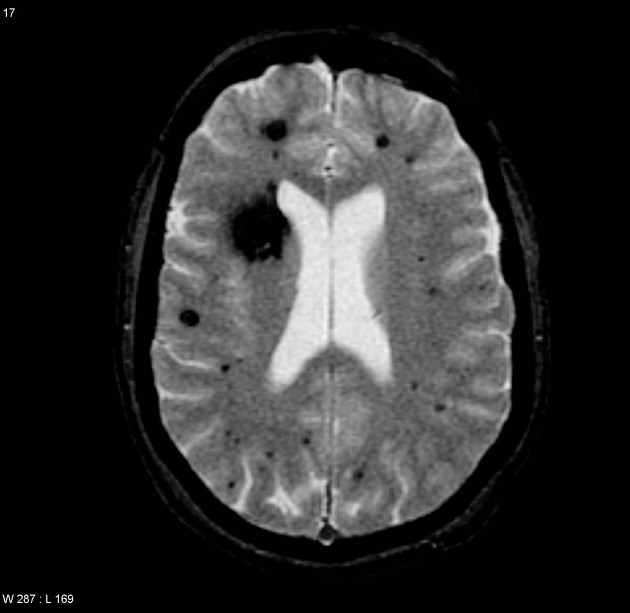
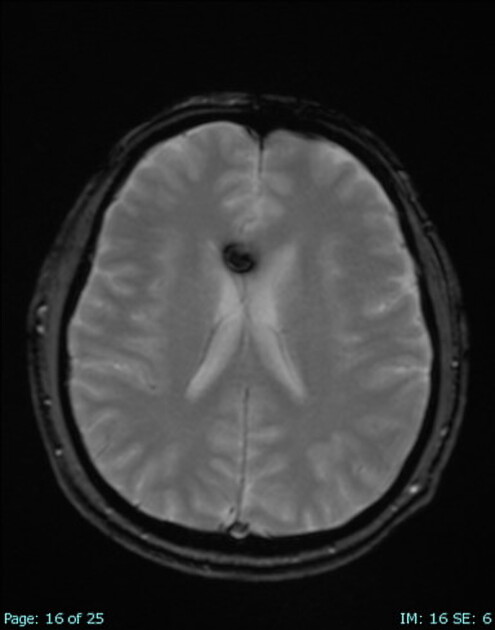
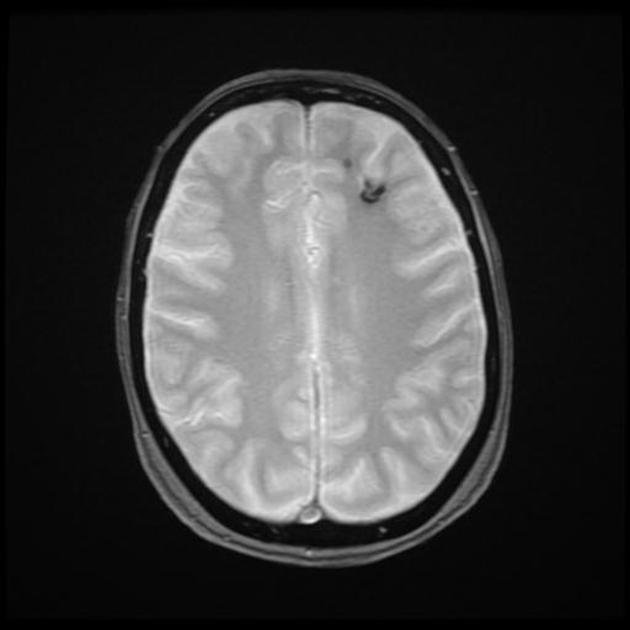
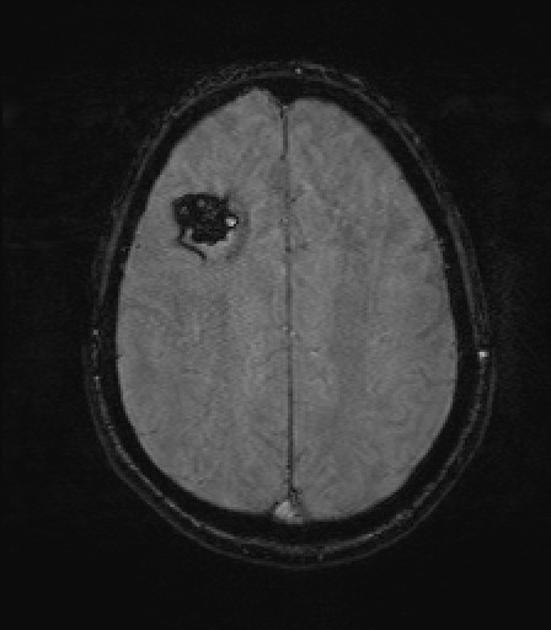
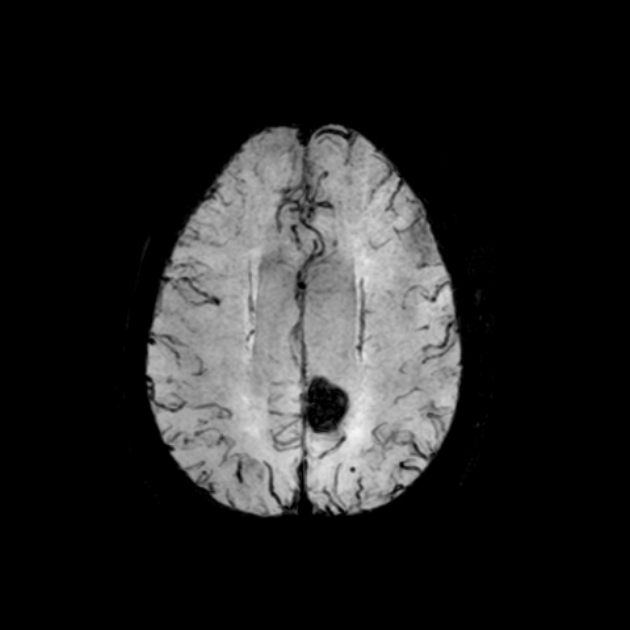
GRE T2*/SWI
prominent blooming
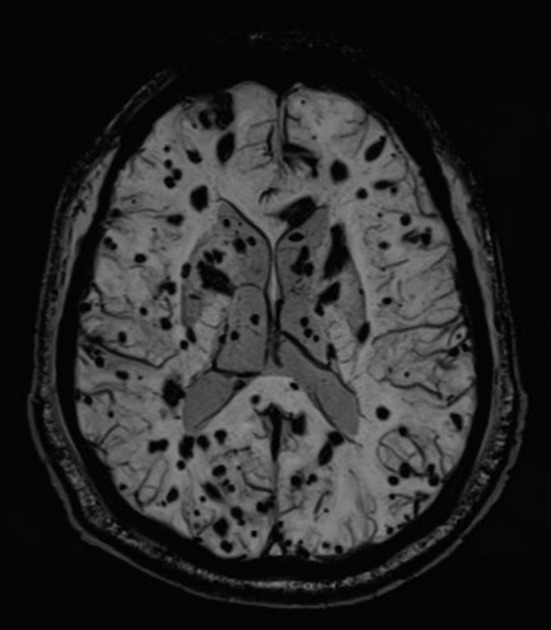
useful for detecting smaller lesions otherwise missed by conventional spin echo sequences, especially in patients with familial or multiple cavernous malformations
-
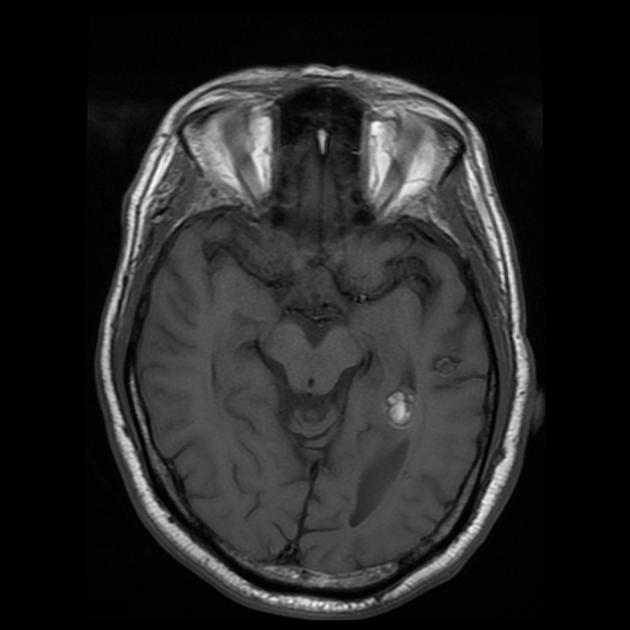
T1 C+ (Gd)
generally no enhancement, although possible 7
Cavernous malformations can be grouped into four types based on MRI appearances using the Zabramski classification 11.
Angiography (DSA)
Cavernous malformations are angiographically occult and do not demonstrate arteriovenous shunting. DSA is useful to differentiate a cerebral cavernous malformation from an arteriovenous malformation or developmental venous anomaly 14,15.
Radiology report
When reporting cerebral cavernous malformations, the following information is recommended for inclusion 14:
field strength and sequences
when single or few, signal characteristics, size (measured on spin-echo sequences), and location
when multiple, an estimate of number (e.g. 20-30, more than 50) is considered more helpful than "too many to count" or "innumerable"
presence/absence of any associated developmental venous anomaly
presence of acute/subacute hemorrhage (intralesional and/or extralesional), or intraventricular extension
Treatment and prognosis
Many cavernous malformations are asymptomatic and can be treated conservatively. Symptoms can relate to mass effect, epileptic activity or repeated hemorrhage. Symptomatic lesions should, when possible, be resected and complete resection is curative 9.
Differential diagnosis
The differential, when cavernous malformations are numerous, is that of other causes of cerebral microhemorrhages, including 2:
cerebral amyloid angiopathy: usually numerous small foci
chronic hypertensive encephalopathy: more common in the basal ganglia
Larger lesions can mimic:
Calcified lesions, such as old neurocysticercosis, or other infections (e.g. tuberculoma) should also be considered.
Practical points
when numerous cerebral cavernous malformations are found around the periphery of a developmental venous anomaly, these are likely to be part of one sporadic mixed vascular malformation rather than represent familial disease 14







 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.