MRI
What are the different types of cord herniation?
Cord herniations typically manifest in two primary types: 1) post-surgical cord herniation, which can emerge at any level but is more frequently observed dorsally in the cervical region following laminectomy; 2) ventral cord herniation, also known as spontaneous thoracic cord herniation, or idiopathic spinal cord herniation, which occurs due to the herniation of the thoracic cord through a defect in the anterior or anterolateral dura mater.
Which are the segments affected by ventral cord herniation?
This entity occurs in the anterior aspect of the mid to upper thoracic spine, between T2 and T8, where the normal thoracic kyphosis leads to the thoracic cord being near the ventral theca.
What clinical symptoms are associated with ventral cord herniation?
The patient's symptoms and physical examination are nonspecific. Patients usually present with features of myelopathy due to the distortion of the cord parenchyma, formation of adhesions, and vascular compromise, which leads to neurological dysfunction. Some initial clinical features are numbness, chronic progressive paraparesis, spastic monoparesis, gait disturbance, ataxia, pain, and incontinence, which often worsen over time. Progressive hemicord syndrome (Brown-Séquard syndrome) usually occurs due to herniation of one side of the cord, and it is the most common clinical manifestation of ventral cord herniation, including ipsilateral hemiparesis of the lower limb, with loss of proprioception, pain, and temperature sensation on the other side.
What are CT myelography and MR findings in ventral cord herniation?
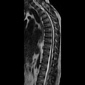
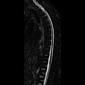
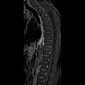
The CT myelography and MR findings reveal a local tear in the ventral dura, causing a cord segment to protrude into the epidural space, which leads to an acute anterior kink and distortion of the thoracic spinal cord, often spanning one to two thoracic segments. Cord atrophy and signal change may be present. No CSF is visualized between the cord and ventral theca and there may be a widened dorsal subarachnoid space with CSF pulsation artifacts, which suggests the absence of a space-occupying lesion posterior to the cord. Thin-section MR imaging commonly displays the location of the dural defect and herniated cord. The "nuclear trail" sign, a calcification from nucleus pulposus leakage, appears as hyperattenuating in CT or signal hyperintensity in MRI.
What is the treatment for ventral cord herniation?
Surgery is the primary treatment to correct the herniation, which consists of surgical reduction and release of the spinal cord, followed by closure or occasionally widening of the dural defect. The symptoms may improve after surgery; however, complete recovery may not occur in some cases. Patients with a focal T2 signal change in the cord may have a poor prognostic for full recovery. Some patients with mild nonprogressive symptoms may be eligible for conservative management.
The five-year post-surgical follow-up MRI demonstrated the absence of the anterior cord kink, which was present in the preoperative images, indicative of complete resolution of the ventral cord herniation. The focal area of T2 high signal intensity in the cord may be due to edema, gliosis, or postoperative changes.
Impression: Surgical resolution of the ventral cord herniation.