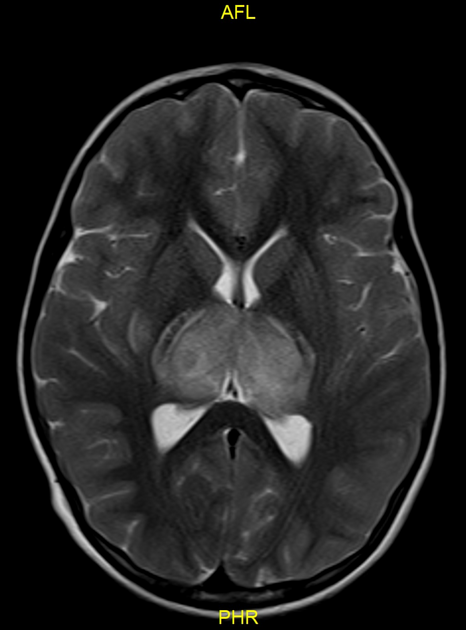
Acute necrotizing encephalopathy, also referred as acute necrotizing encephalopathy of childhood (ANEC), is a rare type of encephalopathy characterized by multiple bilateral brain lesions, mainly involving the thalami, but also the putamina, internal and external capsules, cerebellar white matter, and the brainstem tegmentum.
On this page:
Epidemiology
Acute necrotizing encephalitis is a rare condition. From the first case described in 1995, many cases have been reported in Asia as well as in many Western countries. Most cases are sporadic; however, a few cases of recurrent and/or familial episodes have been reported, secondary to mutations in the RANBP2 gene 10.
Although the initial publications were in the pediatric population, multiple further reports showed the condition to also occur in adulthood 8.
Clinical presentation
Clinically, it is characterized by acute encephalopathy, with dramatic neurological deficits/symptoms. A viral etiology has been proposed in some cases; viral prodrome may therefore precede the neurological deficits.
Pathology
The etiology and the pathogenesis of acute necrotizing encephalitis are only partially clear. Usually, it develops secondary to viral infections, including influenza A and influenza B, parainfluenza, varicella, enterovirus, and SARS-CoV-2 9.
Pathologically, the lesions show edema, hemorrhage and necrosis. Acute necrotizing encephalopathy is characterized by the lack of inflammatory cells in affected brain parenchyma in comparison to the more common entities of acute disseminated encephalomyelitis and acute hemorrhagic encephalitis 1.
Radiographic features
CT
On CT, the corresponding thalamic, putamina, cerebral, cerebellar and brainstem abnormalities are hypodense.
Intracranial hemorrhage and cavitation may also be seen, both of which are associated with a worse prognosis.
MRI
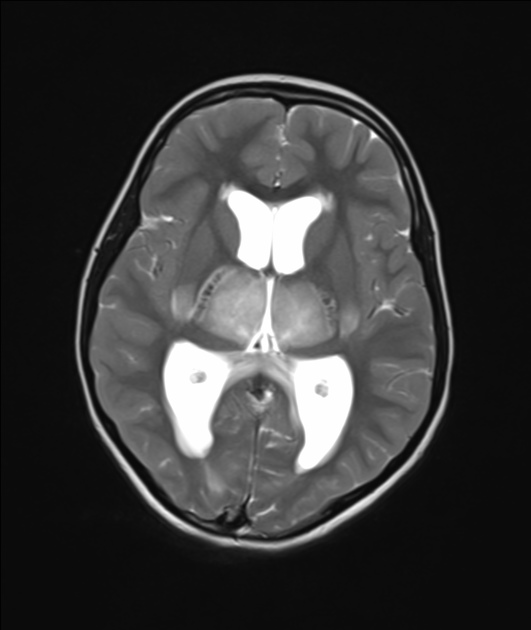
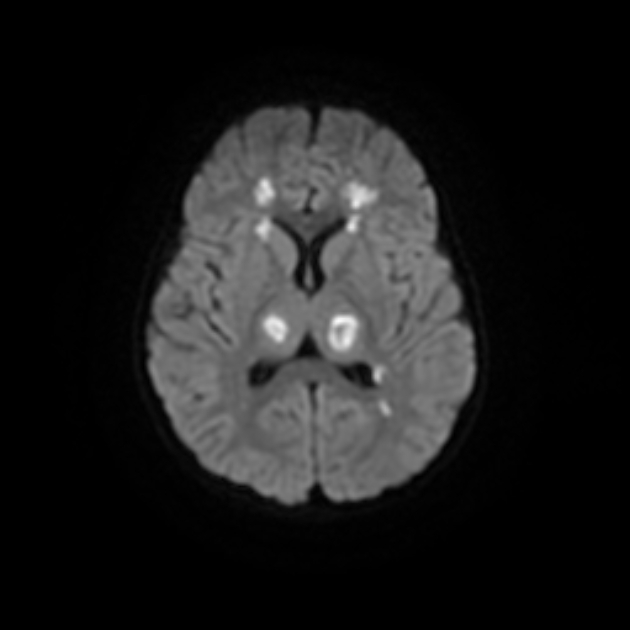
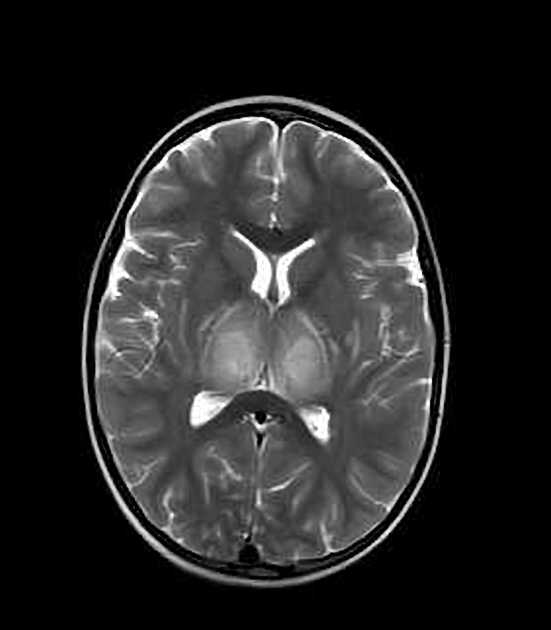
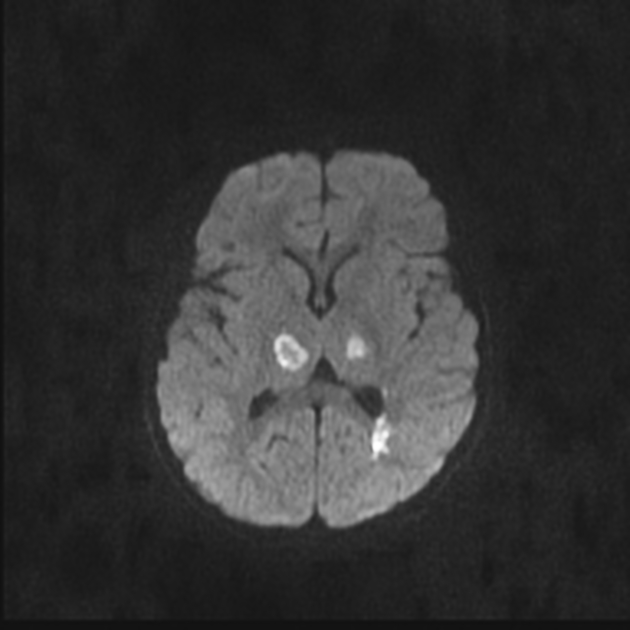
In most cases of the disease, there is bilateral symmetrical thalamic involvement. Abnormal signals on MRI are hypointense on T1 and hyperintense on T2. Restricted diffusion of the involved regions can be seen, often with the characteristic trilaminar sign 7,12. These findings can be quite extensive. Hemorrhage, cavitation, and post-contrast enhancement are also seen. MR spectroscopy can show elevated lipid/lactate and glutamine/glutamate peaks 11.
Treatment and prognosis
Acute necrotizing encephalitis carries a very poor prognosis; the mortality rate is near 70%. Treatment is mainly supportive, as the precise etiology remains unknown.
Differential diagnosis
If characteristic symmetric imaging findings are present, the differential diagnosis is limited. Lactic acidosis is not a classic finding of acute necrotizing encephalitis. Otherwise, the differential diagnoses include:
-
associated with hypoglycemia, hyperammonemia and lactic acidosis
-
associated with hypoglycemia, hyperammonemia and lactic acidosis
viral encephalitides such as Japanese encephalitis or dengue encephalitis
Clinically, acute necrotizing encephalitis may be differentiated from acute disseminated encephalomyelitis by an early onset of encephalitic features just after the prodromal illness while they may take 1 to 2 weeks to develop in acute disseminated encephalomyelitis.