Presentation
Diabetic patient with history of bee-sting to the right middle finger which was incised, drained and treated with antibiotics at the time of plain film. MRI was obtained 2 months later.
Patient Data

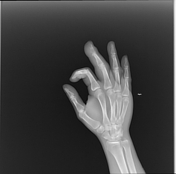
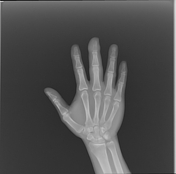
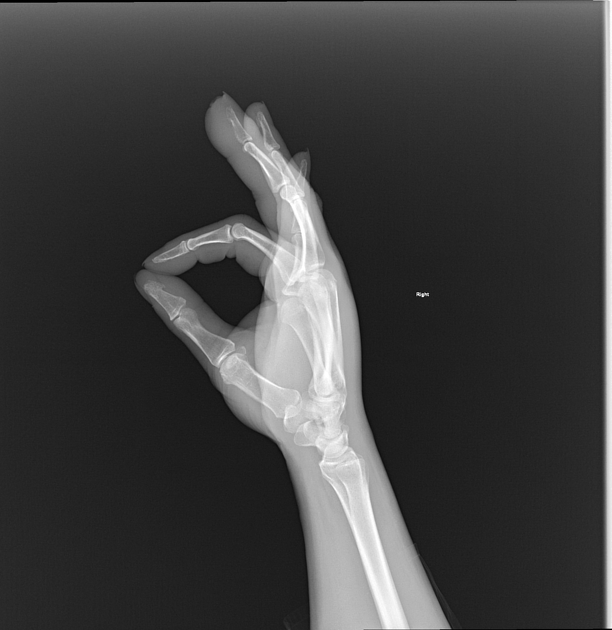
There is marked soft-tissue swelling of the right middle finger. Loss of density and cortical definition at the tip of the 3rd distal phalanx is noted, consistent with osseous erosion.
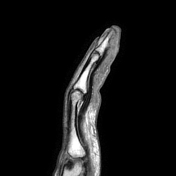

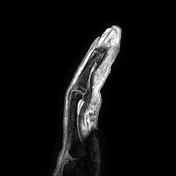

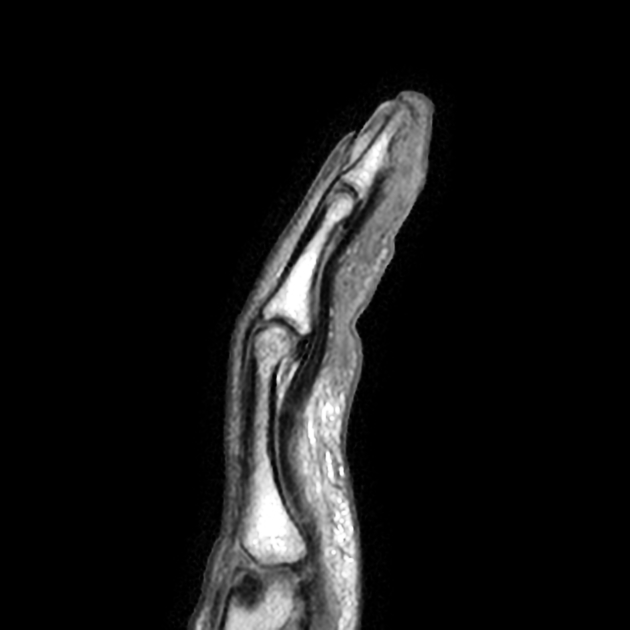
Edema of the bone marrow and surrounding soft-tissue and cortical disruption of the distal phalanx are more conspicuous on the fat saturated sequence. The post-gadolinium sequence from this study was not included because it was not fat-saturated, but did show surrounding soft-tissue enhancement.
Case Discussion
The earliest features of osteomyelitis are seen on MRI, manifesting as bone marrow edema, which can be seen in as little as 24-48 hours from the onset of infection. This is at a time where the only plain film findings would be surrounding soft-tissue swelling. Even nuclear medicine bone scans take a few days before showing increased uptake. Later on as time progresses, sclerosis and/or lucency and periosteal reaction may be evident on plain films, at which time MR demonstrates more well-defined edema, bone abscesses (Brodie abscess) with peripheral contrast enhancement, and similar findings in the soft-tissues. The hallmarks of chronicity are bony sequestra (dead bone) within an involucrum (essentially a cavity), cloaca (cortical break in involucrum allowing for decompression into the soft-tissues), and sinus tracts. A sequestrum may be seen on plain films, CT, and MRI.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.