Presentation
Status post cardiac arrest with suspected subarachnoid hemorrhage from outside hospital.
Patient Data


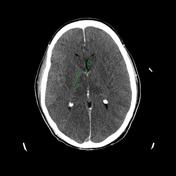

Non-contrast head CT reveals global hypoattenuation of brain parenchyma compatible with diffuse cerebral edema. There is loss of gray-white differentiation and reversal of the normal hyperdense basal ganglia and hypodense internal capsules (ROI 1 - 22 HU; ROI 2 - 29 HU). There is complete loss of sulci. The lateral ventricles are markedly effaced appearing slit-like. The basal cisterns are similary effaced concerning for early transtentorial herniation. Relative hyperdense appearance of the suprasellar cistern, intracranial vessels and tentorium mimicks subarachnoid hemorrhage. Findings are compatible with hypoxic-ischemic brain injury in the setting of cardiac arrest.
Case Discussion
This case demonstrates hypoxic-ischemic brain injury following cardiac arrest. In the literature many terms are often used interchangeably and may be confusing. Anoxia refers to absence of oxygen in the blood for more than 5 minutes and hypoxia is partial but more prolonged hypoxemia 2. Both situations may be further complicated by hypotension as in cardiac arrest.
In the brain more metabolically active areas will be affected first, specifically grey matter, e.g. cerebral cortex, basal ganglia, thalami, hippocampi. Very simply, a lack of oxygen leads to a breakdown of normal cellular function resulting in uptake of water into the cells and swelling. This is manifested by hypoattenuation of the involved parenchyma on CT.
Early on it may become difficult to differentiate basal ganglia from internal capsule as the basal ganglia becomes hypoattenuating or less dense 2. Remember the basal ganglia of a normal brain on CT are more dense than the internal capsules. Over time hypodensity will become more apparent and diffuse edema and increased intracranial pressure will result in obliteration of subarachnoid spaces - sulci and subarachnoid cisterns - and effacement of the ventricles. Ultimately, herniation may result 1.
As in our case, relative hyperdense appearance of the subarachnoid cisterns, intracranial vessels, and dural reflections can mimic subarachnoid hemorrhage, termed pseudo-subarachnoid hemorrhage. Please see a classic case of subarachnoid hemorrhage for comparison.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.