Presentation
Patient presents with recurring dull ache in left lower quadrant.
Patient Data
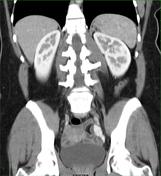

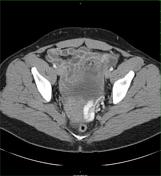
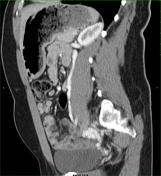

Contrast enhanced images of the abdomen and pelvis demonstrate dilatation and tortuosity of the left ovarian vein and parauterine veins.
- Note: This case has been tagged as "legacy" as it no longer meets image preparation and/or other case publication guidelines.
Case Discussion
Women suffering from pelvic congestion syndrome (PCS) typically present with non-cyclical, chronic, lower abdominal pain that is dull in nature. The pain can be described as a “fullness” or “heaviness” but may also be more sharp and acute (Knuttinen et al., 2015). It can be aggravated by sitting, standing, or intercourse (Ignacio et al., 2008) and is often exacerbated around the time of menses or pregnancy (Knuttinen et al., 2015). Additionally, PCS is known to decrease in intensity around menopause (Knuttinen et al., 2015).
Chronic pelvic pain is a significant problem, with nearly 40% of women suffering from it during their lifetime and its implication as a cause of nearly 10 to 15% of gynecologic visits in the United States. PCS typically affects multiparious women who are of childbearing age (Philips et al., 2014). Risk factors include anatomic variants, pregnancy, pelvic surgery, estrogen therapy, obesity, phlebitis, prolonged standing or heavy lifting (Philips et al., 2014).
PCS is thought to be caused by pelvic varicosities whose incompetent valves promote reflux flow (Philips et al., 2014). Similar to the varicocele in males, PCS is most often observed on the left side as the left ovarian vein generally drains into the left renal vein whereas the right ovarian vein drains directly into the inferior vena cava. Furthermore, dilation of the pelvic and ovarian veins is implicated and these veins are susceptible to enlargement, engorgement, and congestion (Knuttinen et al., 2015), promoting further venous incompetence.
Generally, PCS is a diagnosis of exclusion (Ignacio et al.). Following physical examination, pelvic ultrasound is typically the first modality utilized. Computed tomography may provide high quality pelvic imaging (Ignacio et al., 2008). Additionally, magnetic resonance imaging or magnetic resonance venography provides a higher degree of detail and is capable of detecting features that may not be easily ascertained on abdominal ultrasound. One can expect to see “dilated, torturous, enhancing tubular structures” located near the uterus, ovaries, broad ligament, and pelvic sidewall (Ignacio et al., 2008). There is also a role for minimally invasive imaging modalities such as catheter venography, which may distinctly demonstrate PCS (Lopez et al., 2015).
Treatment of PCS involves medical management with analgesics and hormones, surgical repair, surgical ligation, or percutaneous embolization (Ignacio et al., 2008).
Case Co-Authored By: Mithil B. Pandhi




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.