Presentation
Incidental renal mass.
Patient Data
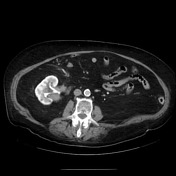

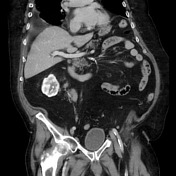



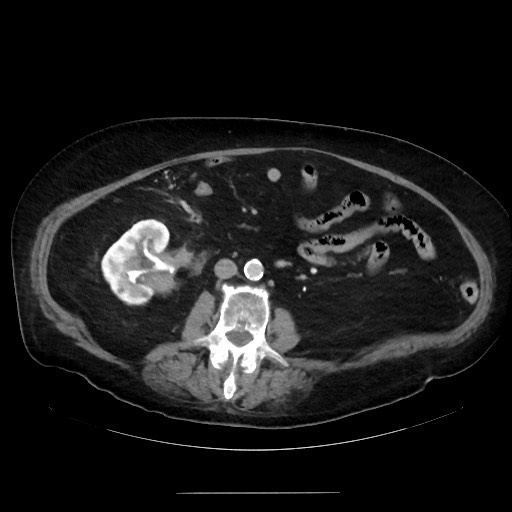
Medium to large right pleural effusion with collapse of the RLL.
Infiltrative mass in the right renal hilum extending caudally along the course of the proximal ureter. Right upper calyceal dilation.
Smaller but similar infiltrative mass in the left renal hilum with a lobulated component along the upper cortex (see coronals).
No urinary obstruction/hydro.
No adenopathy.
Case Discussion
This case provides a great platform to discuss possibilities for bilateral renal/perirenal masses.
The differential and what makes a diagnosis likely/unlikely is as follows:
- Lymphoma - often bilateral, diffuse cortical involvement; can have perihilar/perirenal infiltration as in this case. Despite the size and extent of tumor there is often minimal obstruction of the urinary system, and in this case there is only mild dilation of the right upper pole calyces. Adenopathy would help to really favor this diagnosis.
- Plasmacytomas - this would be a consideration and can have an overlapping appearance if this patient had a diagnosis of multiple myeloma or bone disease to support this diagnosis (if not yet made).
- Erdheim-Chester - Often expect to see a more pronounced peri-renal infiltration with a "hairy kidney" appearance rather than soft tissue masses, more commonly obstructs the kidney, common presentation of bone pain with long bone metaphyseal lesions.
- RPF/IgG4 - RPF commonly starts near the aortic bifurcation, ascends along the aorta, medializes and obstructs the ureters
- Sarcoidosis - while you can have renal involvement it is very rare compared to hepatosplenomegaly or adenopathy
- Urothelial carcinoma - It does not have such a large peri-renal component, much less common to have bilateral involvement
- EMH - rare, but possible if the patient has myeldysplasia/splenomegaly
- Amyloid - also rare, would have expected calcifications, hepatosplenomegaly, the correct clinical context
Based on the appearance it would be appropriate to favor lymphoma in this case. However, the trouble is confirming that diagnosis, as there are no superficial or nodal targets. It would be worthwhile to do a chest CT or physical exam to see if there is axillary or supraclavicular adenopathy before proceeding with a deeper biopsy.
In this case, the bulk of the soft tissue is around and below the right kidney. Therefore, with proper patient positioning and firm pressure of the probe, hypoechoic extra-renal retroperitoneal soft tissue was adequately seen with US and biopsied, confirming "Follicular lymphoma, grade 1-2". CT biopsy with posterior approach would also be reasonable, but we prefer ultrasound-guided techniques when possible at my institution.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.