Presentation
Recurrent sacral chordoma.
Patient Data
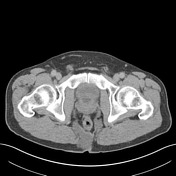





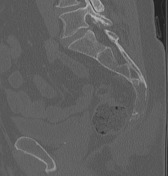

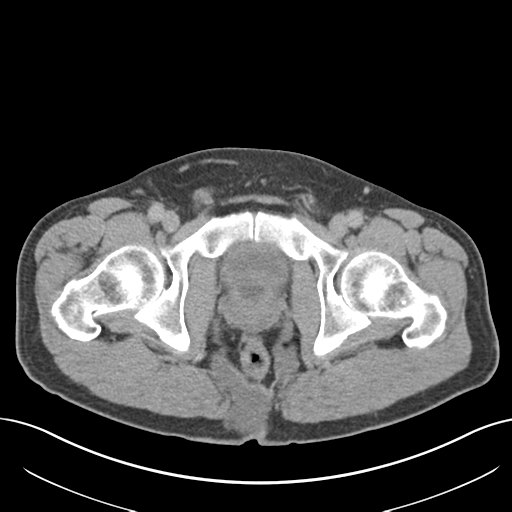
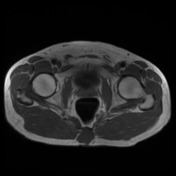
The known, lobulated, moderately well-defined, infiltrating soft tissue mass is again demonstrated involving the tip of the coccyx and extending inferiorly and anteriorly into both ischiorectal fossae as well as posteriorly into the surrounding fat, deep to the superior aspect of the natal cleft. The perirectal fat, although narrowed in places, is preserved with no definite breach.
The mass measures up to 9.8cm in maximum craniocaudal dimension and inferiorly on the right side measures up to 7.7 x 4.2cm.
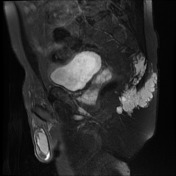
Superiorly, there is evidence of invasion of the coccyx. Ill-defined soft tissue infiltrate continues superiorly into the right side and midline of the coccyx over a distance of approximately 5.2cm with associated erosion.
No free intraperitoneal fluid or focal collection. No pelvic or inguinal lymphadenopathy.
Features suggest a previous TURP.
Mild degenerative change in the lower lumbar spine and sacroiliac joints bilaterally.
Conclusion: The features would be in keeping with the clinical history of recurrent chordoma and are unaltered from the recent MRI.
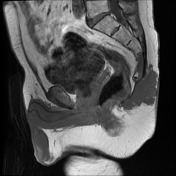





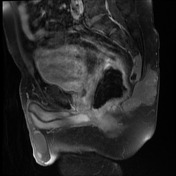

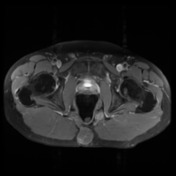

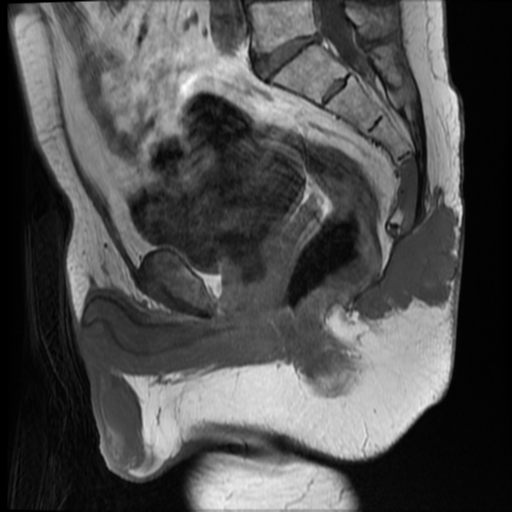
Comparison is made to an outside MRI and the previous CT from this hospital.
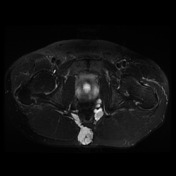
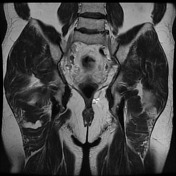
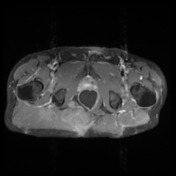
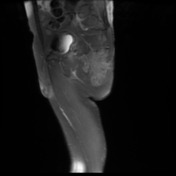
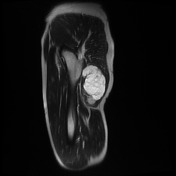
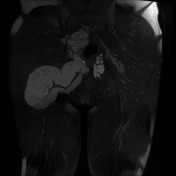
Recurrent chordoma is documented-with markedly hyperintense signal on T2 weighted scans, best demonstrated on the fat saturated axial and coronal T2 images, with tumor in the midline and on the right 6.7 x 3.2 cm, in continuity with multiple contiguous nodules in both ischio rectal fossae, on the left with displacement of the levator ani complex superiorly, and with a high suspicion for tumor invasion across this fascial plane. More inferiorly from the ischio rectal fossa, tracking between the gluteus maximus and medius muscles, is a tongue of tumor that reaches to the subcutaneous tissues laterally on the buttock, 1.3 cm wide, and 12 cm long (extending along a surgical plane? ). Tumor extends into the central and right side of the sacrum - both bone and canal.
Enhancement is moderate. Tumor does not reach to the lumbar spine, and there is no involvlement of the bony pelvis outside the sacrum.
Conclusion: Local tumor spread demonstrated, in gluteal region, perineum, sacrum, ischiorectal fossa, and likely spread through the left levator ani abutting the rectum.
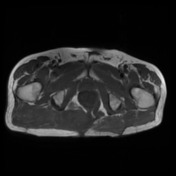







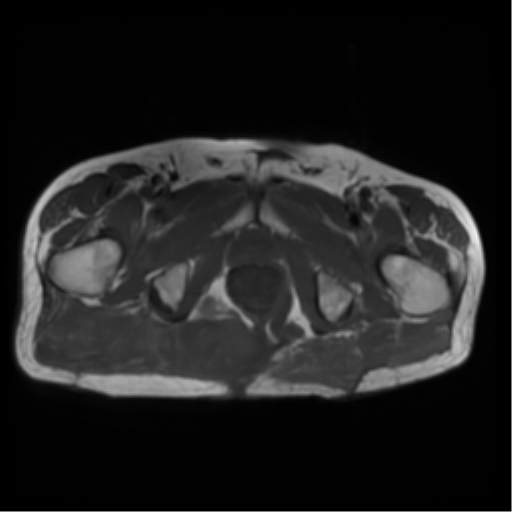
Reference is made to the prior scan.
As previously demonstrated, there is a large chordoma arising from the inferior aspect of the right sacral ala with inferolateral extension into the mesorectal fat, the ischiorectal fossa and the gluteus maximus muscle. There has been increase in extent and dimensions of the mass. Superiorly, there is increase in the component within the right posterolateral aspect of the mesorectal fat with obliteration of the fat plane between the mass and the rectum. There is no extension within the lumen of the rectum. There is increase in the component within piriformis muscle and also increase in the AP diameter of the gluteus maximus muscle invasive component.
There is interval small exophytic nodule extending from the mass in the right ischiorectal fat.
Prior sacral surgery and fat grafting in the sacral spinal canal are unchanged.
Conclusion: There is further increase in the size of the right sacral chordoma as detailed.
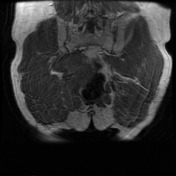

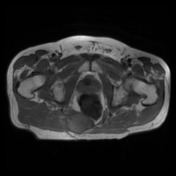

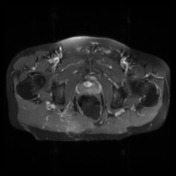

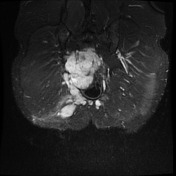

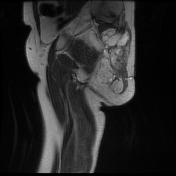

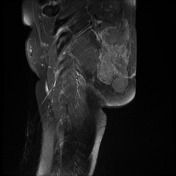

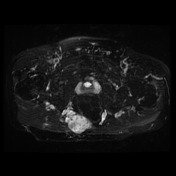





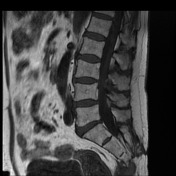

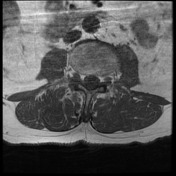

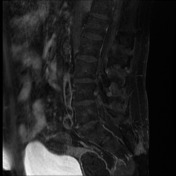

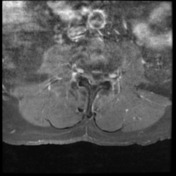


MRI lumbar spine, sacrum and pelvis
Pre-and post contrast sequences have been obtained, with comparison to the previous MRI.
The sacrum is again truncated at the S3 level, consistent with previous tumor debulking. The lobulated T2 hyperintense tumor in the ischiorectal fossae, right piriformis and abutting partially resected sacrum remains in situ, but the large component which had previously extended inferolaterally posterior to the right ischial tuberosity and right hip joint has been debulked. Mild edema in the operated region is expected postsurgical finding.
There is stable indentation of the mesorectal fascia by the right ischiorectal fossa component of tumor. No proximal extension into the remaining portion of the sacral canal.
Conclusion: Debulking of the right gluteal portion of the large sacral chordoma.
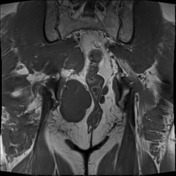

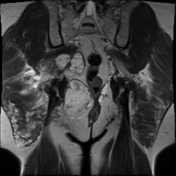



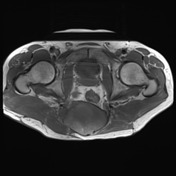

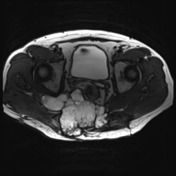

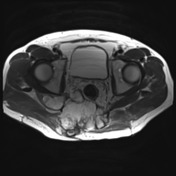

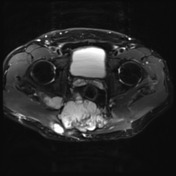

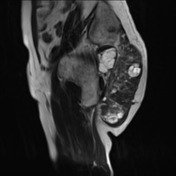

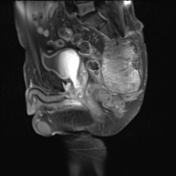

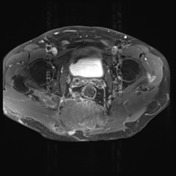

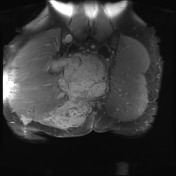

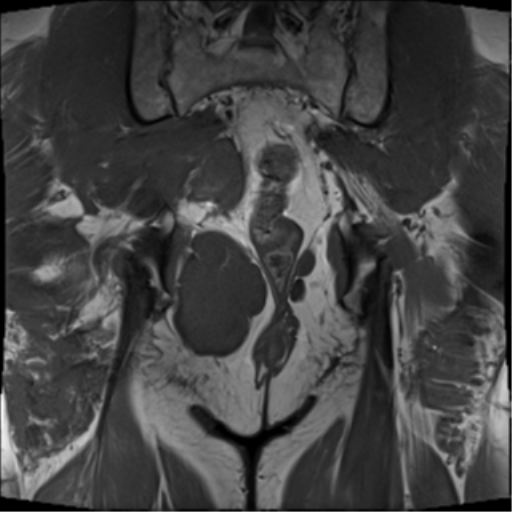
No evidence of distal sacrectomy at the level of S3. The lobulated T2 hyperintense and enhancing tumor in the right gluteal region involving the ischiorectal fossae, right piriformis and abutting partially resected sacrum is larger. Today the largest more central component measures 11 x 11.7 x 10.7 cm (AP x LR x CC) and there 2 large tongues of tumor extending inferiorly and laterally into the gluteus musculature on the right which have markedly increased in size.
The tumor no above the right lateral wall of the rectum however there is preservation of the mesorectal fat plane. This
Enlarging enhancing bony lesions in the posterior right ilium in keeping with progressive metastatic disease.
Conclusion: Progressive local and metastatic disease.
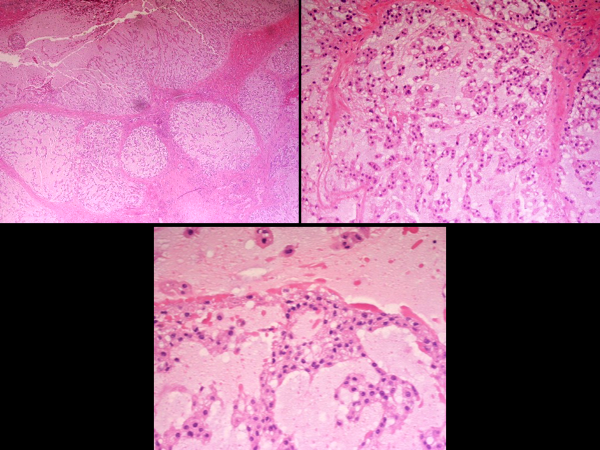
MICROSCOPIC DESCRIPTION: Sections show a multi-lobulated, circumscribed tumor with a fibrous pseudocapsule in areas. The tumor is moderately cellular composed of sheets of eosinophilic tumor cells set within extracellular matrix material. There are focal areas of hemorrhage and necrosis present. Tumor cells contain round-to-oval nuclei with finely granular chromatin and prominent nucleoli. Physalliferous cells containing vacuolated cytoplasm are present. No atypia or mitoses are seen. No skeletal muscle, lymphovascular or perineural invasion is seen. Margins are unable to be accurately assessed due to fragmentation.
DIAGNOSIS: Sacrum: Recurrent chordoma.
Case Discussion
Chordomas correspond to ~4% of all primary bone tumors.
Traditionally surgical resection has been the first line of treatment
Prognosis is typically poor, due to the locally aggressive nature of these tumors, with the




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.