Presentation
Palpaple, smooth mass lesion at the middle of the neck at the level of the hyoid bone. Non painful. Mobile.
Patient Data
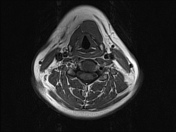

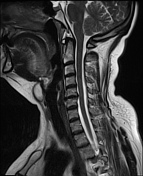

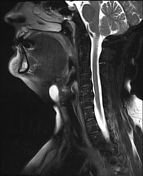

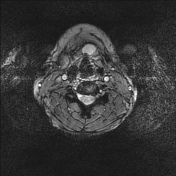

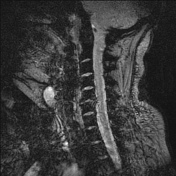

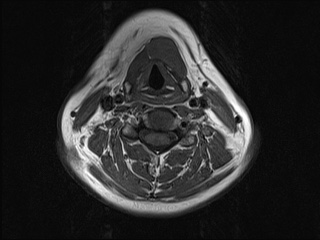
There is a thin-walled round cystic, well-circumscribed lesion at the middle of the neck, attached to the body of the hyoid bone, sized 26 x 14 x 18 mm. The signal is low at T1-weighted and high at the T2-weighted sequences. No prefixal edema and/or infiltration found.
Case Discussion
Thyroglossal duct cyst (TDC) is usually diagnosed clinically, but ultrasonography is the preferred imaging technique in children. The 2 most common complications of TDC are infection and malignancy, the latter of which occurs in 1-4% of cases. TDC is the most common nonodontogenic cyst in the neck, representing approximately 70% of all congenital neck abnormalities. It occurs as a result of anomalous development and migration of the thyroid gland during the fourth through eighth weeks of gestation. It is a cystic remnant along the course of the thyroglossal duct between the foramen cecum of the tongue base and the thyroid bed in the visceral space of the infrahyoid neck.
Approximately 65% of TDCs are located between the hyoid bone and thyroid gland. 50% occur at the level of the hyoid bone and 20% occur above it. Lingual TDCs are rare, accounting for 1-2% of all TDCs. In a series of 300 TDCs only 2 (0.67%) were in the region of the foramen cecum. Cysts in this location may be associated with dysphagia and respiratory arrest. The low incidence of lingual TDC may be because the thyroglossal duct begins to atrophy from the oral side.
At MR imaging, thyroglossal duct cysts demonstrate low signal intensity with T1-weighted sequences and high signal intensity with T2-weighted sequences and do not restrict diffusion. The wall of a thyroglossal duct cyst can be thick, with rim enhancement, on both CT and MR images if the cyst is currently or was previously infected.
Complete resection of the cyst and duct up to the foramen cecum is curative. The Sistrunk procedure includes resection of the middle third of the hyoid bone. There is small risk of recurrence (approximately 2-3%).




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.