Presentation
Three days cough, myalgias and fever. No recent overseas travel. Only sick contact was her husband who was recently hospitalized with presumed community-acquired pneumonia but not tested for COVID-19. Past history of vascath in-situ for dialysis on a background of chronic end-stage renal failure with dysfunctional A-V fistula.
Patient Data
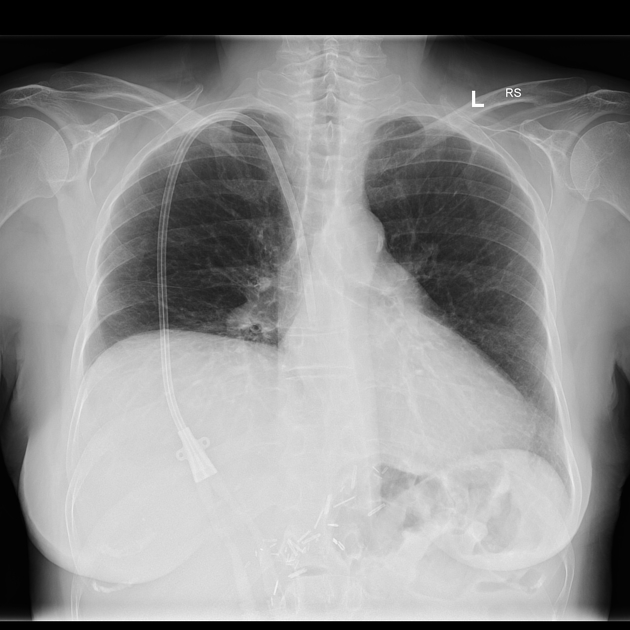
Vascath in-situ. Upper abdominal surgical clips. Lungs and pleural spaces are clear. Elevated right hemidiaphragm.
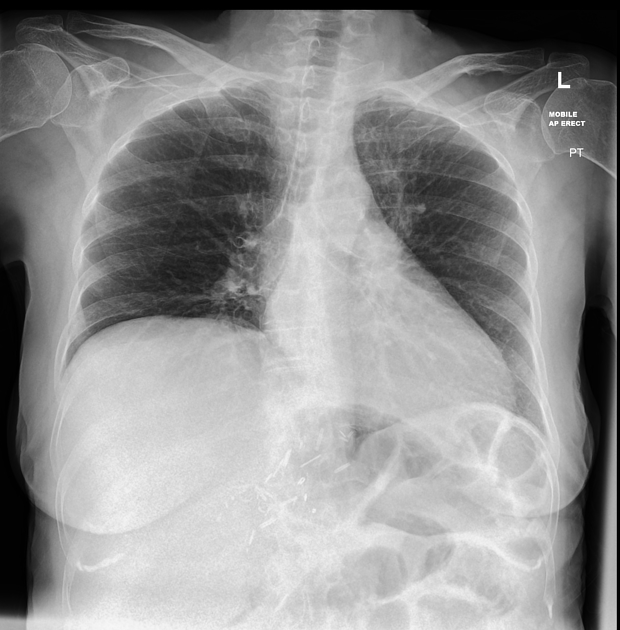
There is mild left peri-hilar and upper lobe interstitial opacity consistent with developing consolidation.
Serial chest x-ray was taken four days after the first x-ray, and seven days since the onset of symptoms. By this stage, the patient has had a positive nasopharyngeal swab for COVID-19 virus.
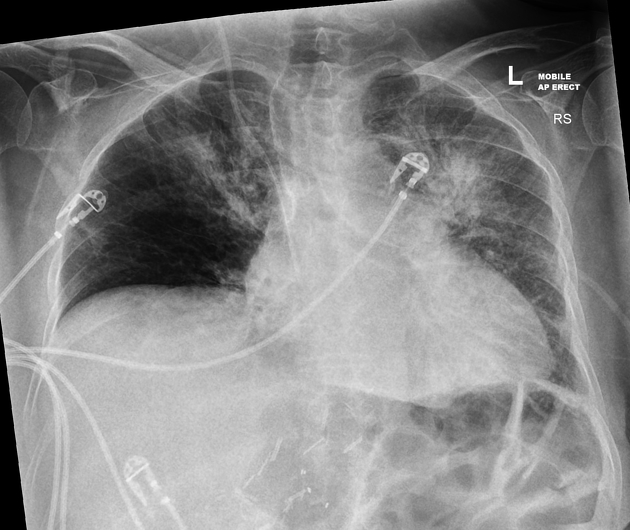
There is established left upper lobe and now progressive patchy consolidation in left lower, right upper and middle lobes.
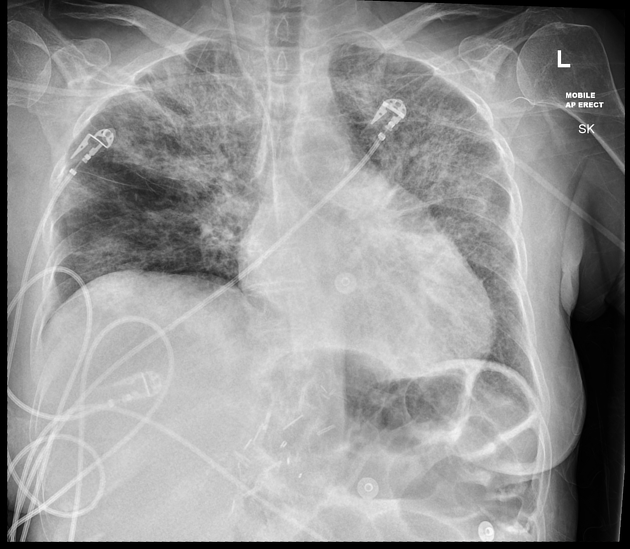
There is progression of right side opacity and, clinically, the patient is desaturating with increased work of breathing higher supplemental oxygen requirements.
Little more than 24 hours from the previous x-ray the patient has increased work of breathing, fatigue and low oxygen saturations on 10-15 L/min of supplemental oxygen. Progressive acute respiratory failure. Patient intubated and mechanically ventilated.
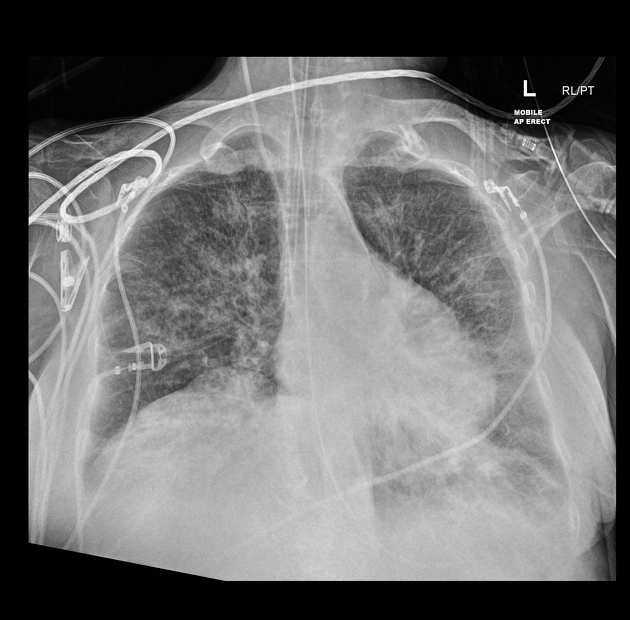
The endotracheal tube is just above the carina and there is a nasogastric tube within the stomach. There is a right jugular central line with the tip in the superior vena cava.
There is now widespread interstitial and alveolar opacity diffusely spread through both lung fields.
Case Discussion
This 70-year-old woman presented to hospital for revision of her A-V fistula in the setting of chronic end-stage renal failure requiring hemodialysis.
She was noted to have three days of concurrent odynophagia and dry cough. She had a temperature of 38 degrees on admission. Her only sick contact was her husband, who had recently been hospitalized with presumed community-acquired pneumonia at another hospital. He was not tested for COVID-19. Neither patient had recent overseas travel of contact with known COVID-19 positive patients.
This patient had progression from mild central and apical consolidation to diffuse bilateral consolidation resulting in acute respiratory failure needing intubation within seven days of symptom onset. She developed septic shock and was on high vasopressor requirements.
Imaging has limited sensitivity for COVID-19, as up to 18% demonstrate normal chest radiographs or CT when mild or early in the disease course, but this decreases to 3% in severe disease. The initial chest x-ray changes were more confined to the pulmonary interstitium, a clue suggesting early atypical pneumonia; although non-specific imaging findings are common. Nasopharyngeal swabs returned positive for COVID-19 on two serial tests. Testing for other typical and atypical organisms was negative.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.