Obliterative bronchiolitis - chronic lung allograft dysfunction
Presentation
Shortness of breath.
Patient Data
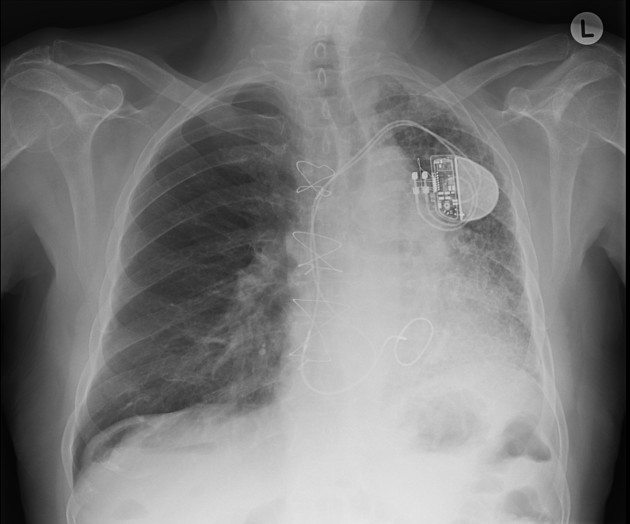
The left lung has reduced volume and peripheral reticular markings with a craniocaudal gradient of distribution. There is a mild shift of the mediastinal structures to the left. The right lung appears expanded, somewhat compensating the smaller contralateral lung, and is clear. Pleural spaces are clear. Sternotomy wires, prosthetic mitral valve, and left-sided single lead pacing device noted.
This patient received single lung transplantation some years ago due to his severe pulmonary fibrosis. He has been experiencing a decline in the forced expiratory volume in the first second of expiration (FEV1) along the last months.
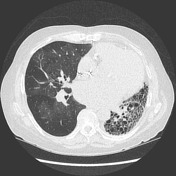



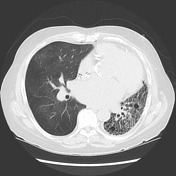

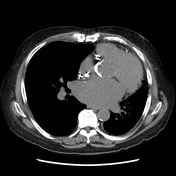

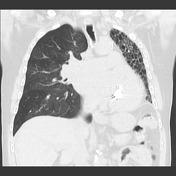

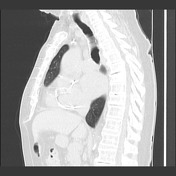

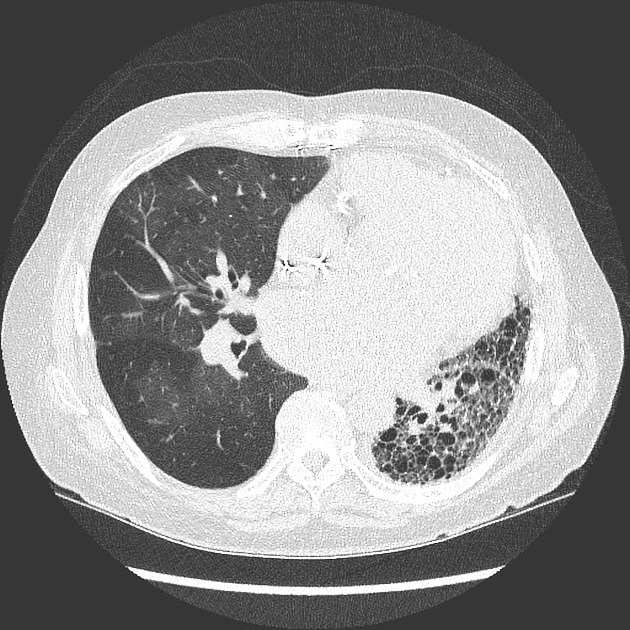
The transplanted lung has a diffuse mosaic pattern of attenuation that is accentuated on the expiratory acquisition, where sharply defined areas of decreased lung attenuation are consistent with air-trapping. A component of oligemia is also present with the areas of low attenuation (mosaic perfusion appearance). No relevant bronchiectasis or bronchial wall thickening. The left lung shows features of advanced fibrosis.
Case Discussion
This patient has had a drop of lung function in the last months, particularly with a sustained drop of the FEV1 in more than 20%. The HRCT has corroborative findings that support bronchiolitis obliterans: diffuse air-trapping and mosaic perfusion appearances.
The left lung shows diffuse architectural distortion and volume loss consistent with the known pulmonary fibrosis.
Bronchiolitis obliterans is the most common form of chronic lung allograft dysfunction (CLAD), accounting for about three quarters. Also, studies have shown that about 50% of post-lung transplant patients develop BOS within 5 years 1.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.