Epidural lipomatosis refers to an excessive accumulation of fat within the spinal epidural space resulting in compression of the thecal sac. In severe cases, compression may be symptomatic. The lumbar region is most frequently affected.
On this page:
Epidemiology
The demographics of affected individuals reflect the underlying causes 5:
- glucocorticoid excess
- long term steroid administration (e.g. for asthma): 55% - most common
- endogenous Cushing syndrome: 3%
- obesity: 25%
- idiopathic: 17%
- Scheuermann disease 10
- following spinal surgery 10
Clinical presentation
Symptoms are often non-specific and may be similar to other degenerative spinal conditions resulting in stenosis. Patients may present with a combination of pain, radicular symptoms, weakness, and paresthesia.
Pathology
Macroscopic pathology is characterized by the abnormal accumulation of unencapsulated adipose tissue in the extradural space.
Radiographic features
Epidural lipomatosis typically involves the lower lumbar and/or lower thoracic levels. Although the disease can be visualized with both CT and MRI, the latter is better able to identify impingement upon the cauda equina.
MRI
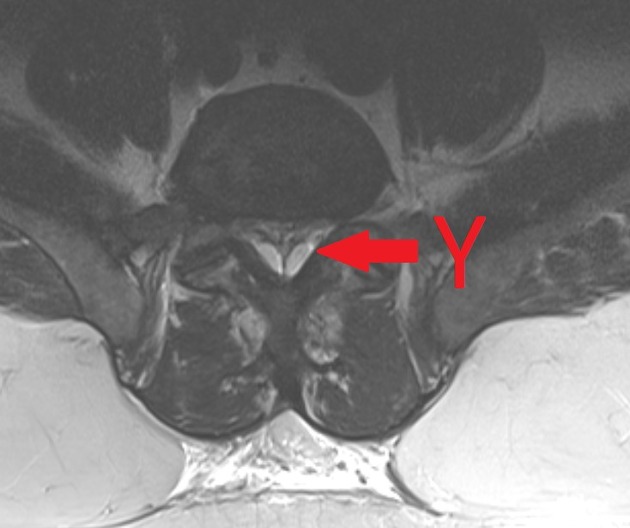
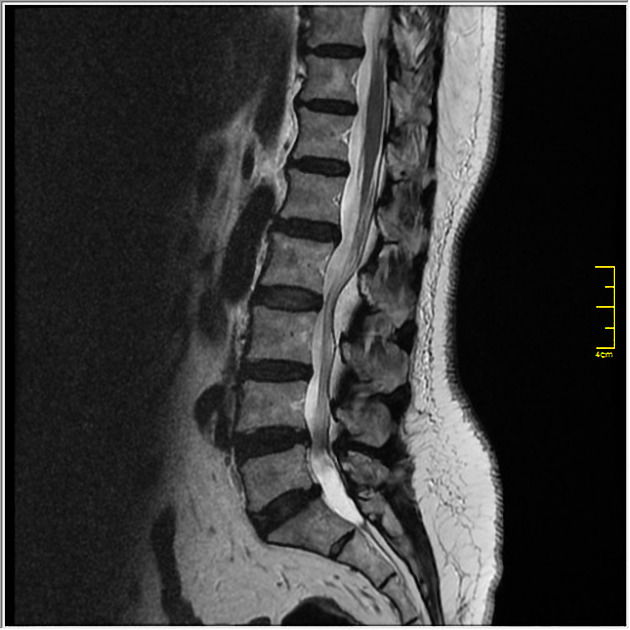
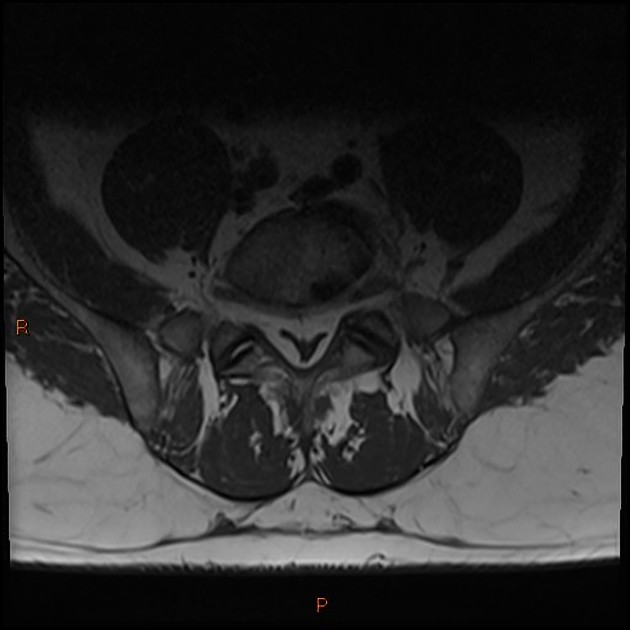
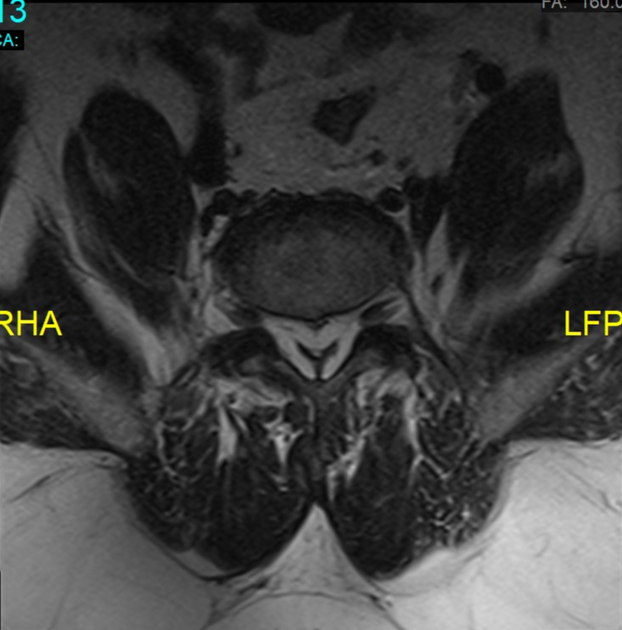
There is an often generalized excess of fat seen in the extradural space. As a result, the dural sac can appear narrowed or even resemble a "Y" shaped configuration.
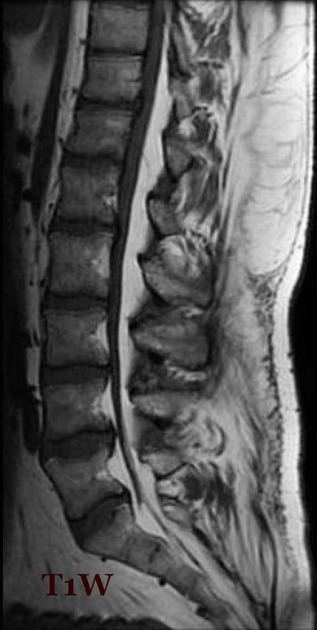
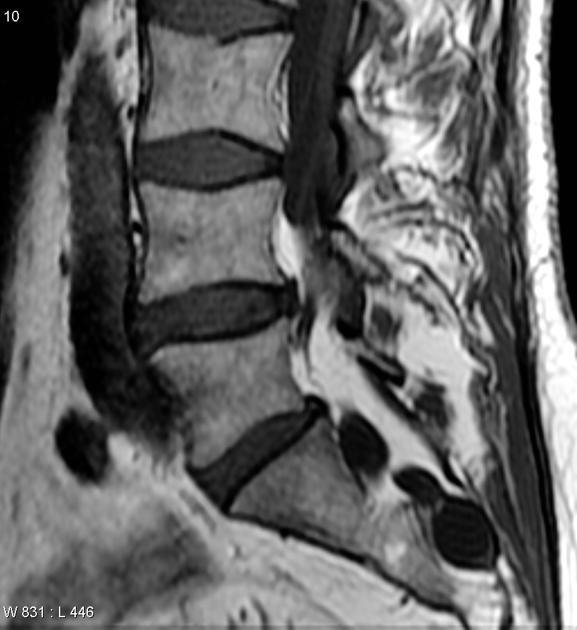
Signal characteristics follow fat on all sequences:
- T1: high signal
- T1 (FS): shows fat suppression
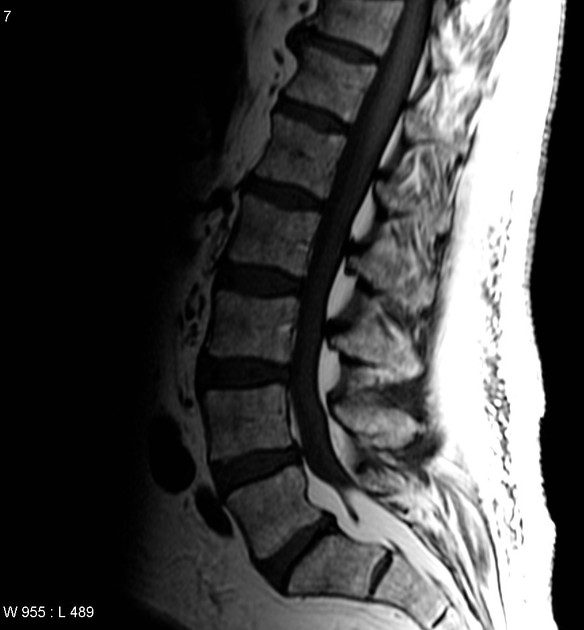
- T2: high signal
Treatment and prognosis
In most instances, no specific treatment is required, although a review of the need for steroid and weight loss are sensible interventions.
The use of epidural steroid injection is controversial. Some authors argue against it, on the grounds of existing compression and implication of steroids in the pathogenesis of epidural lipomatosis 5. Others report successful pain management 6,9. A single epidural steroid injection is not thought to induce epidural lipomatosis 9.
In some patients symptoms are severe and operative decompression is required and is usually successful 7,8,10.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.