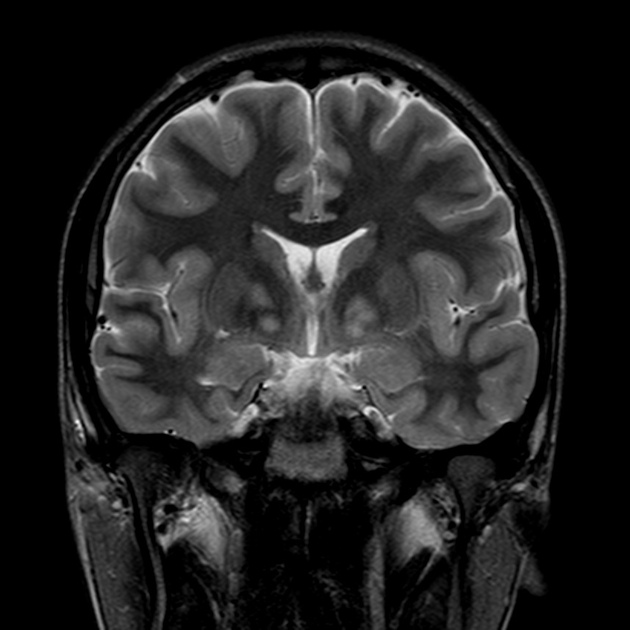
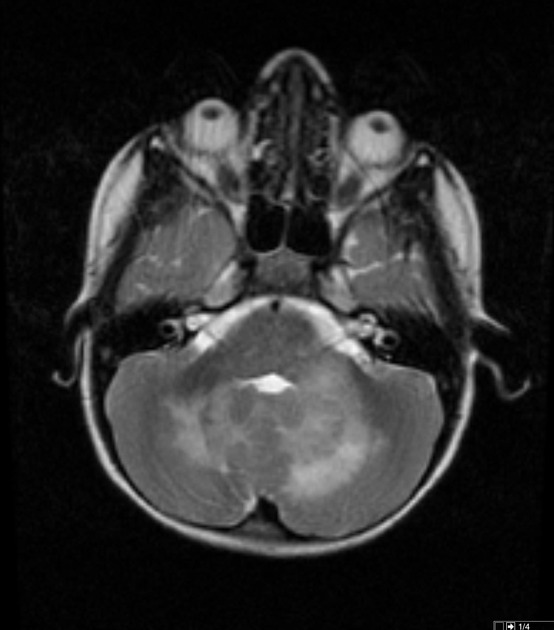
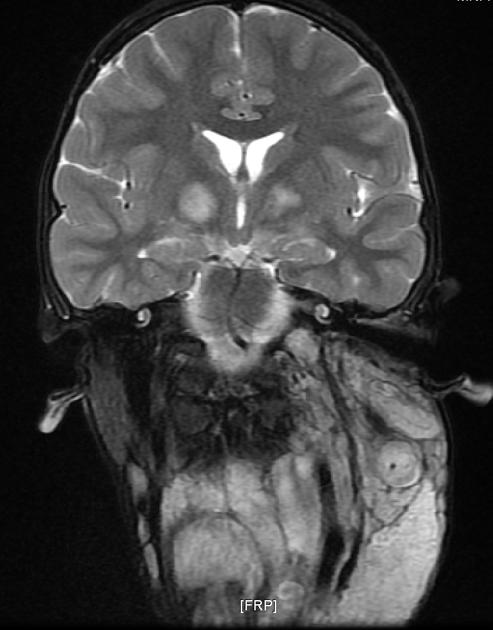
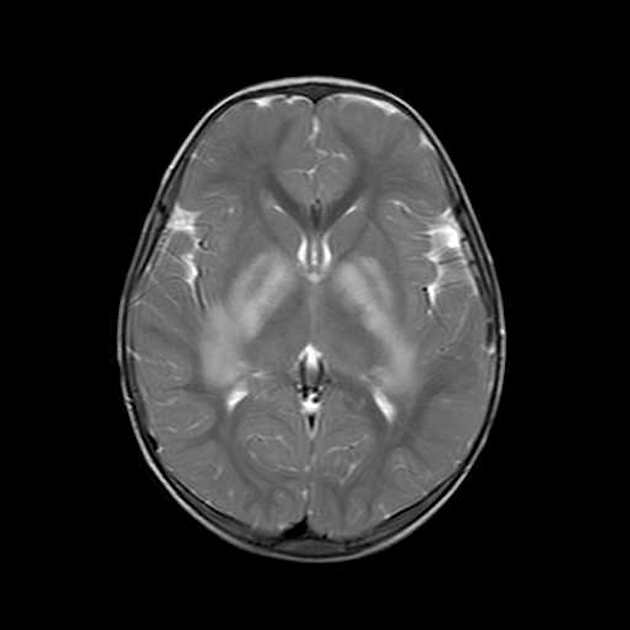
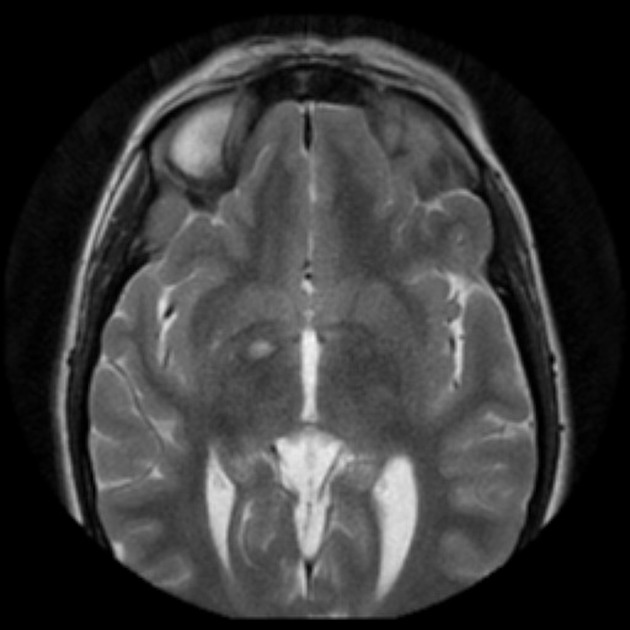
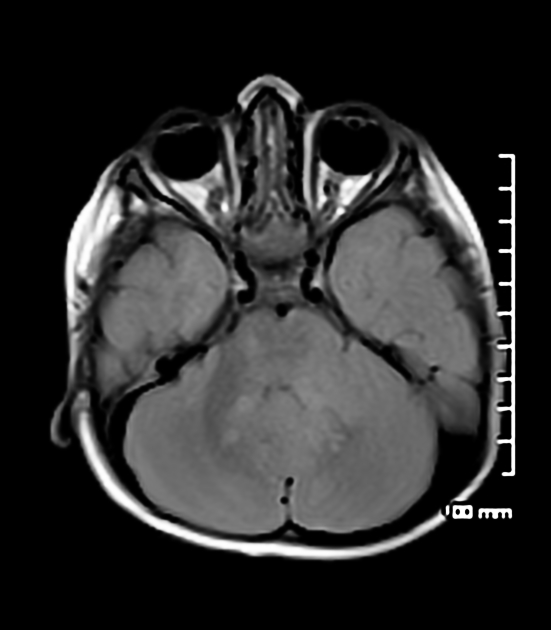
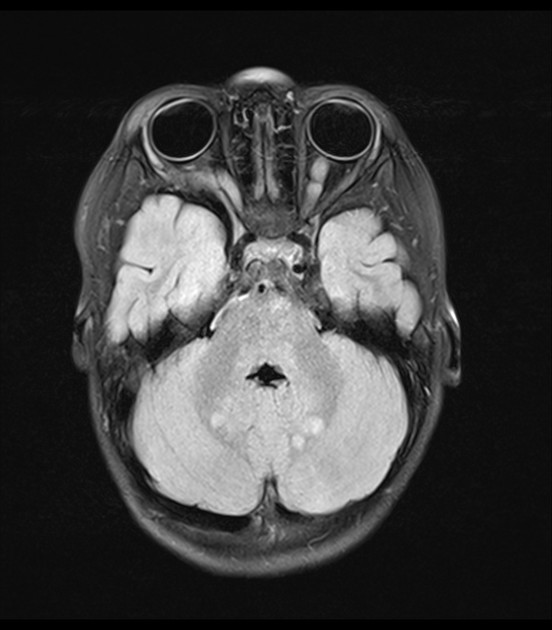
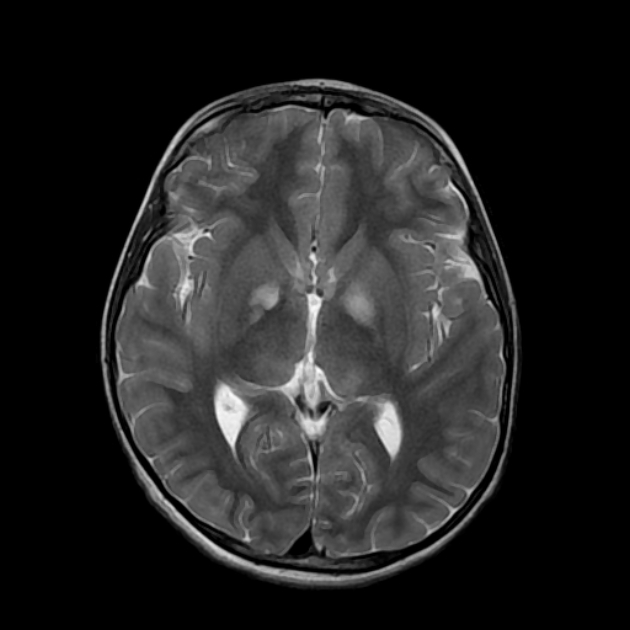
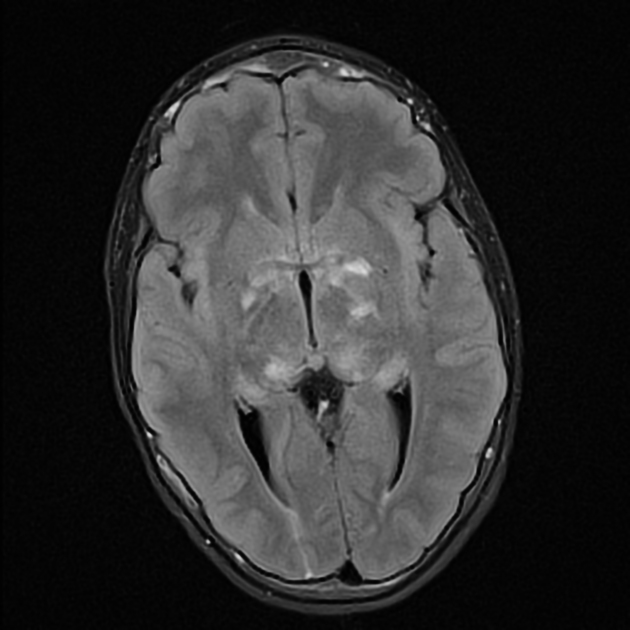
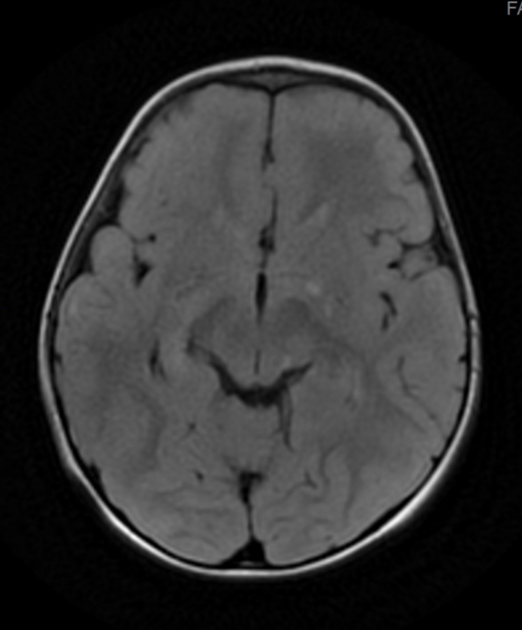
Focal areas of signal intensity (FASI), also known as focal abnormal signal intensity or unidentified bright objects (UBO), are bright areas on T2-weighted images commonly identified in the basal ganglia (often the globus pallidus), thalamus, brainstem (pons), cerebellum, and subcortical white matter in children with neurofibromatosis type 1 (NF1).
On this page:
Epidemiology
Focal areas of signal intensity are the most common neuroimaging feature in NF1 patients 1. A study in 2008 showed a significant frequency (86%) of one or more FASI in children with NF1 2. Patients younger than 10 commonly have an increase in either size or number of lesions, but such an increase beyond 10 years of age raises concern for a neoplasm 10.
In 2023, a study suggested that FASI may occur in Noonan syndrome in addition to NF1 14.
Clinical presentation
There is controversy about the relationship of FASI with cognitive dysfunction in NF1 3. Some studies in the early 2000s suggested a relationship between cognitive impairment, and the presence, number, and location of FASI, but only thalamic lesions seem to be strongly associated with cognitive impairment 3-6.
Pathology
In 1995 Di Paolo et al. published the findings of a FASI on pathology study as characterized by spongiform myelinopathy or vacuolar change of myelin with no inflammatory reaction in the surrounding tissue and no frank demyelination. The high T2 signal was explained by the vacuoles being filled with water. It remains unclear why FASI sometimes regress 7. Further studies are needed to establish the real origin of FASI 1.
Radiographic features
MRI
T1: isointense to hyperintense
T2/FLAIR: hyperintense
T1 C+ (Gd): usually no enhancement, although enhancing FASI (including potential of regression over time) have been reported 13
MR spectroscopy: normal (useful to distinguish from tumors 9)
Typically FASI have been described to not have mass effect or enhancement. They most commonly occur in the basal ganglia, brainstem, thalamus, optic tracts, cerebellum, and infrequently cerebral hemispheres 11,12.
There are case series that show that occasionally FASI can have mass effect/enhancement, and in these cases the FASI become difficult to distinguish from a low-grade glioma.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.