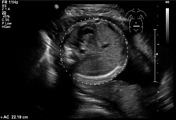
Intrauterine growth restriction
Updates to Article Attributes
Intra-uterine growth restriction (IUGR) is commonly defined as an estimated fetal weight (EFW) at one point in time during pregnancy being at or below the 10th percentile for gestational age 2.
Some authors define the term IUGR when fetal biometric parameters fall under the 5th centile or fall below two standard deviations 12.
Some authors consider this definition synonymous with the term small for gestational age (SGA).
An IUGR can be broadly divided into two main types:
- type I: symmetrical intra-uterine growth restriction
- type II: asymmetrical intra-uterine growth restriction
Some authors also enlist a 3rd type termed: femur sparing intra-uterine growth restriction 10.
Epidemiology
By its standard definition itself, it carries a prevalence of 10% of all births (if the 5th centile is used it will affect 5% of all births instead).
Pathology
Causes
IUGR can result from a vast number of causes:
- maternal conditions
- maternal narcotic/alcohol use/smoking
- maternal diabetes: when the maternal diabetes severe, there can be a paradoxical IUGR as opposed to fetal macrosomia
- maternal malnutrition/starvation
- maternal vascular conditions
- certain medications
- placental insufficiency: commonest cause overall
- other placental causes
- increased incidence with a single umbilical artery
- fetal conditions
- multifetal pregnancy
- intra-uterine infections
-
chromosomal anomalies
- trisomy 13
- trisomy 18
- triploidy: IUGR is of early onset
- Down syndrome: not a dominant feature
- chromosome 4p deletion syndrome
- confined placental mosaicism (CPM) 13
- other syndromic anomalies
- in utero substance exposure
Radiographic features
Antenatal ultrasound
Sonographic parameters include:
-
non Doppler features
- presence of oligohydramnios without ruptured membranes
- increased head circumference (HC) to abdominal circumference (AC) ratio (in asymmetrical type)
- decreased total intrauterine volumes
- advanced placental grade
-
Doppler features: will require a chart to calculate absolute values
-
umbilical artery Doppler assessment
- increased S/D ratio(s)
- increased resistive index (RI)
-
umbilical venous Doppler assessment
- presence of pulsatility
-
uterine arterial Doppler assessment
- presence of notching in mid to late pregnancy
- increased S/D ratio(s)
-
umbilical artery Doppler assessment
Complications
They are many which include:
- chronic fetal hypoxaemia 6
- neurodevelopmental delay
ManagementTreatment and prognosis
While there is no cure, management is reliant on a structured antenatal surveillance program with timely intervention in order to minimize fetal compromise.
Differential diagnosis
General considerations include:
- incorrect dates
See also
-<li><a href="/articles/edward-syndrome">trisomy 18</a></li>- +<li><a href="/articles/edwards-syndrome-1">trisomy 18</a></li>
-<li>in utero substance exposure<ul><li>e.g <a href="/articles/fetal-hydantoin-syndrome">fetal hydantoin syndrome</a>- +<li>in utero substance exposure<ul><li>e.g. <a href="/articles/fetal-hydantoin-syndrome">fetal hydantoin syndrome</a>
-</ul><h4>Management</h4><p>While there is no cure, management is reliant on a structured antenatal surveillance program with timely intervention in order to minimize fetal compromise.</p><h4>Differential diagnosis</h4><p>General considerations include:</p><ul><li>incorrect dates</li></ul><h4>See also</h4><ul><li><a href="/articles/small-for-date-fetus">small for dates fetus</a></li></ul>- +</ul><h4>Treatment and prognosis</h4><p>While there is no cure, management is reliant on a structured antenatal surveillance program with timely intervention in order to minimize fetal compromise.</p><h4>Differential diagnosis</h4><p>General considerations include:</p><ul><li>incorrect dates</li></ul><h4>See also</h4><ul><li><a href="/articles/small-for-date-fetus">small for dates fetus</a></li></ul>
Image ( create )
Image 2 Ultrasound ( create )