Pericardial abscesses are a rare and severe condition in which a collection of pus forms within the pericardium, the sac that surrounds the heart 1.
On this page:
Epidemiology
Pericardial abscesses are rare, with incidence rapidly decreasing after the development of broad-spectrum antibiotics. They can occur in people of any age but are more likely to occur in older adults. The risk of developing a pericardial abscess is increased in individuals with certain underlying conditions, such as infections, trauma, surgery, or other medical conditions, such as cancer or autoimmune disorders 1,2.
Diagnosis
The diagnosis of a pericardial abscess typically involves a combination of imaging tests, such as CT or MRI, as well as laboratory tests to determine the underlying cause. Pericardiocentesis may be performed to identify the type of bacteria or other pathogens responsible for the infection 3.
Clinical presentation
The clinical presentation of a pericardial abscess may include symptoms such as chest pain, difficulty breathing, fever, and fatigue. The pericardium may also become thickened and inflamed, leading to pericarditis 2.
Pathology
The most common pathogens that can cause a pericardial abscess are Staphylococcus aureus and Streptococcus pyogenes. However, other bacteria such as Escherichia coli, Pseudomonas aeruginosa, Mycobacterium tuberculosis and Klebsiella pneumoniae can also cause pericardial abscess 4.
Pericardial abscess can develop in several ways. One way is through the spread of infection from a nearby source, such as the lungs or chest wall. Another way is through the blood, where bacteria can enter the pericardium through the bloodstream and cause an infection 1,5.
Pericardial abscess can also occur as a complication of a procedure such as cardiac surgery, where bacteria can enter the pericardium through the incision site 1,5.
Pericardial abscess usually occurs in the right atrioventricular groove, in 75% of cases 3.
Radiographic findings
CT
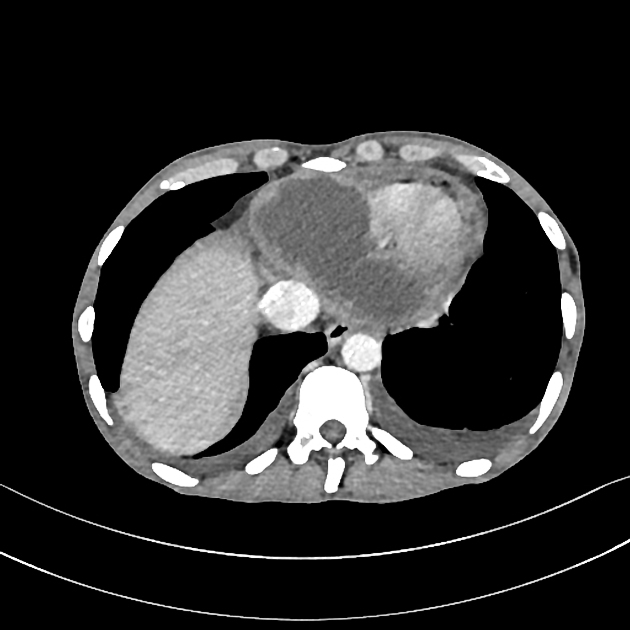
CT can be used to diagnose pericardial abscess and assess the extent of the infection. Some of the CT findings that may be seen in pericardial abscess include 3,6:
fluid collection within the pericardium
thickening and enhancement of the pericardium
displacement of the heart
other signs of infection, for example in the lungs or chest wall
MRI
MRI can be used to diagnose pericardial abscess and assess the extent of the infection. The T1, T2, DWI, ADC, and T1 C+ signal intensities of a pericardial abscess may vary depending on the stage of the infection and the characteristics of the abscess 3.
-
T1
early stages - low signal intensity
as the abscess progresses and becomes a more complex mixture of fluid and solid material, the solid component may have a higher signal intensity
-
T2
early stages - high signal intensity
as the abscess progresses and becomes more complex, it may have areas of both high and low signal intensity
-
DWI/ADC
high DWI signal intensity, with corresponding low ADC values
-
T1 C+ (Gd)
enhancement of the abscess capsular rim
Treatment and prognosis
Treatment options for pericardial abscess may include 4,5
antibiotics, depending on the type of bacteria causing the infection, as well as the susceptibility of the bacteria to different antibiotics
percutaneous drainage, often in combination with antibiotics
In some cases, surgery may be necessary to drain the abscess. This may be done through an open surgical procedure or laparoscopic surgery, depending on the location and extent of the abscess.
The prognosis for pericardial abscess depends on the underlying cause of the infection, the extent of the infection, and the overall health of the patient. With appropriate treatment, the prognosis is generally good. However, untreated or inadequately treated pericardial abscess can lead to serious complications, such as pericarditis (inflammation of the pericardium), heart failure, and death 5.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.