Pneumocephalus (plural: pneumocephali), also known as pneumocranium, pneumocrania, pneumatocephalus, and intracranial pneumatocele, refers to the presence of intracranial gas, and in the vast majority of cases, the gas is air. The term encompasses gas in any of the intracranial compartments and is most commonly encountered following trauma or surgery.
On this page:
Epidemiology
The demographics of affected patients depend on the underlying cause (see below).
Clinical presentation
In the vast majority of cases, pneumocephalus is asymptomatic. Tension pneumocephalus, trapped expansion of intracranial gas due to a ball valve effect resulting in mass effect, can result in a headache and signs and symptoms of increased intracranial pressure 1,4.
In either case, a minority of patients describe 'bruit hydroaerique' (a splashing noise on head movement, equivalent to the succussion splash of pyloric stenosis) 4. This noise may also be audible to the examiner with the aid of a stethoscope.
Pathology
Etiology
mechanical trauma (common)
-
instrumentation, e.g. neurosurgery, external ventricular drain insertion, sinus surgery, peridural anesthesia
after supratentorial craniotomy, pneumocephalus may persist in a minority of patients in the 3rd postoperative week, but is not expected to persist beyond this 6
barotrauma 3
meningitis from a gas-forming organism (rare) 2,4
sneezing 7,8
Location
Pneumocephalus can be divided by location:
-
extra-axial
epidural
subdural
subarachnoid
-
intra-axial
parenchymal
intraventricular
intravascular
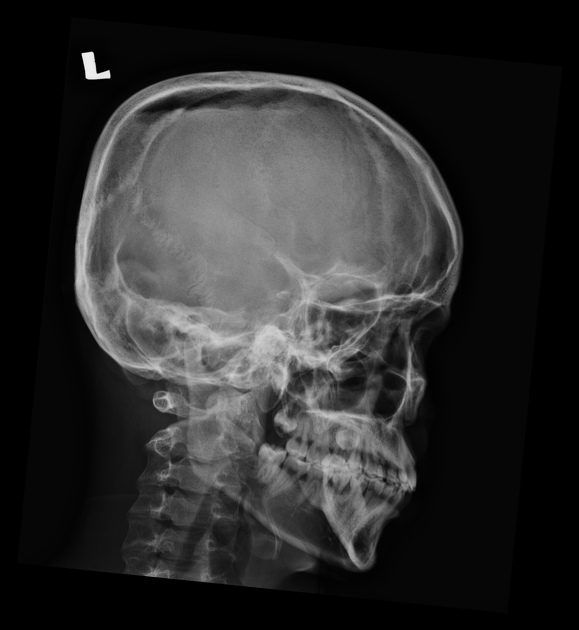
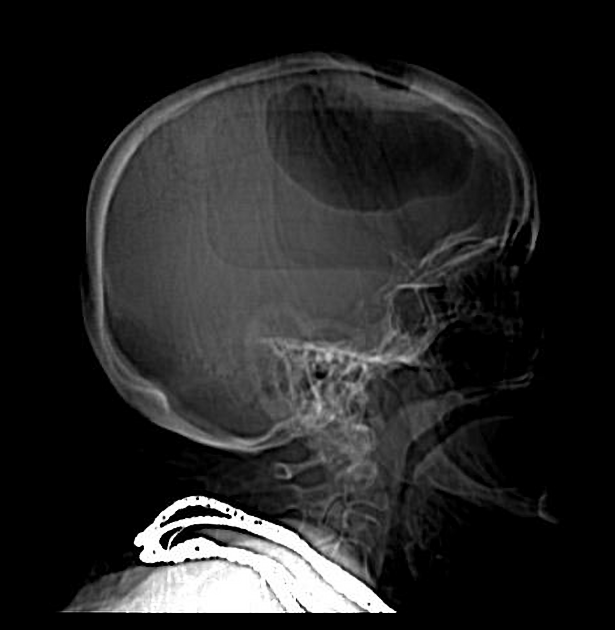
Radiographic features
The diagnosis is simple provided care is taken to ensure that gas density/intensity is actually confirmed.
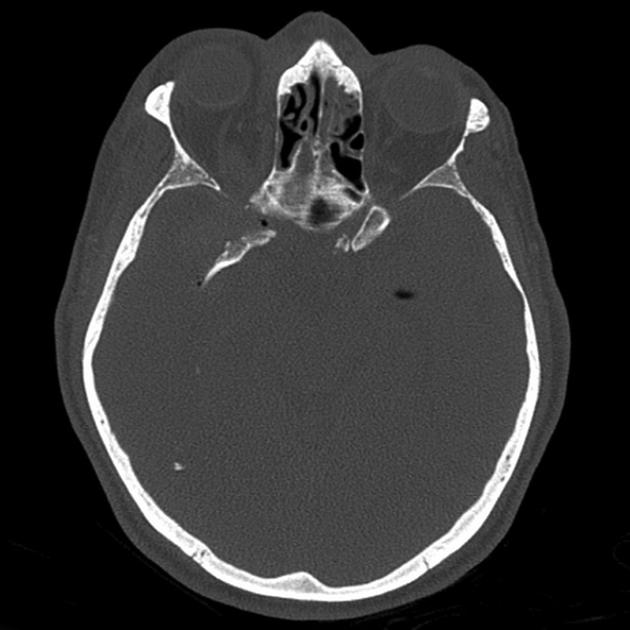
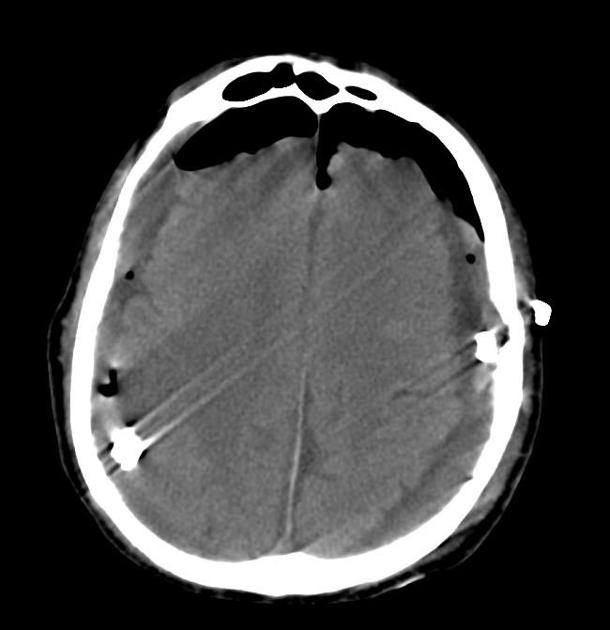
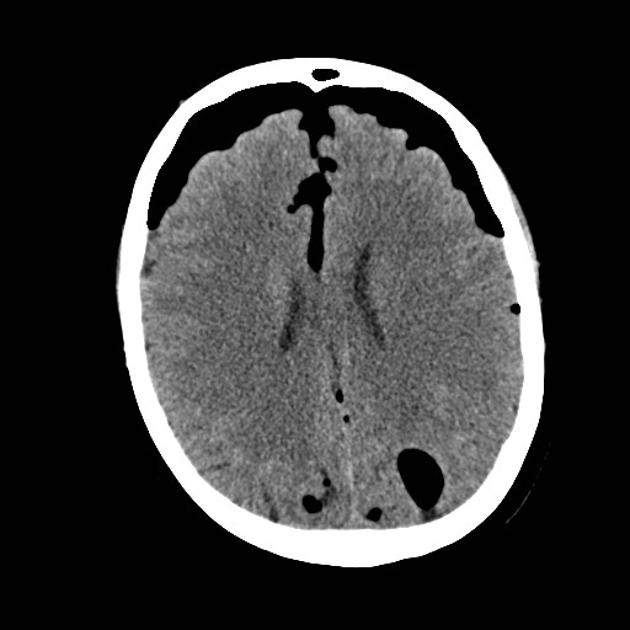
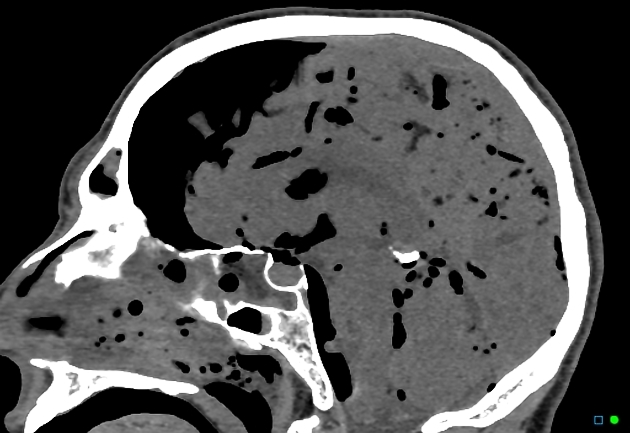
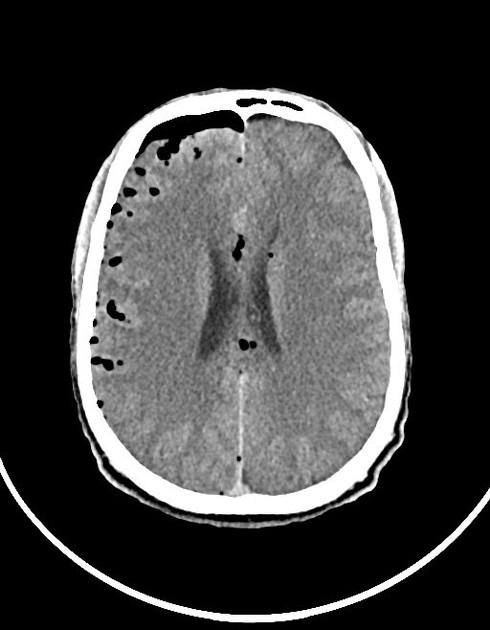
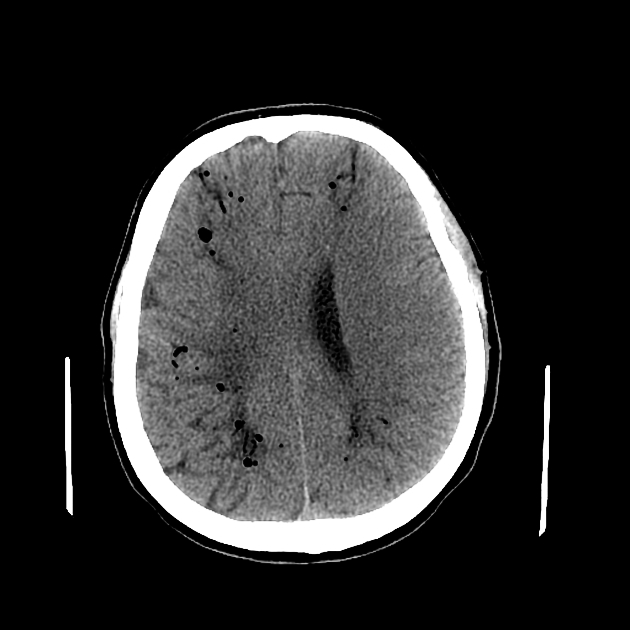
CT
Gas on CT will have a very low density (~ -1000HU) but care needs to be taken in ensuring that it is not fat which although of much higher density (-90HU) also appear completely black on routine brain windows.
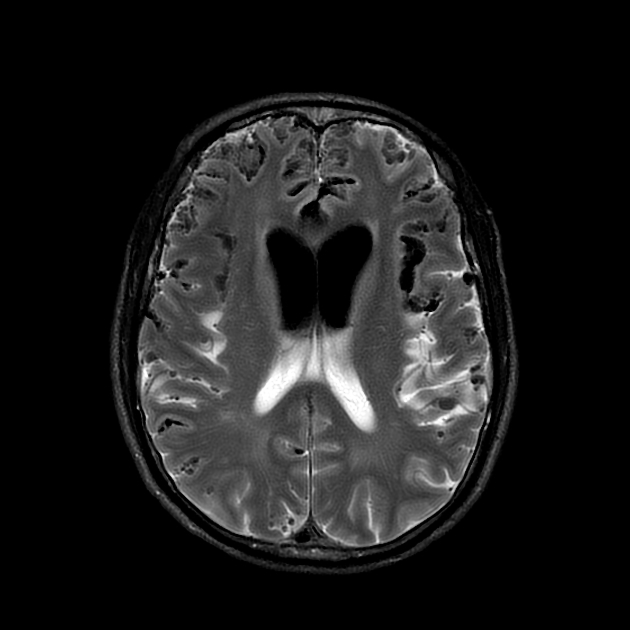
MRI
On MRI the diagnosis may be more difficult as there is no 'objective' density measurement. Gas will appear completely black on all sequences, but depending on the location and morphology can be mistaken for blood product or flow voids 5.
Treatment and prognosis
Treatment depends on the cause, and in many instances, no treatment is necessary with the gas being gradually resorbed. This is the case in the vast majority of post-operative pneumocephalus, an expected finding in essentially all post-craniotomy patients.
In cases of tension pneumocephalus then a burr hole may need to be performed to relieve pressure.
When pneumocephalus results from a CSF leak then identification of the leak site and surgical repair is usually required.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.