Primary sclerosing cholangitis (PSC) is an uncommon inflammatory condition that affects the biliary tree resulting in multiple strictures, liver damage, and eventually cirrhosis.
On this page:
Epidemiology
Primary sclerosing cholangitis is strongly associated with inflammatory bowel disease (IBD) (in 70% of cases 6), especially ulcerative colitis, and thus shares similar demographics: young to middle-aged males (~4th decade) are most frequently affected 4.
Associations
-
-
70-80% of patients with primary sclerosing cholangitis develop inflammatory bowel disease
87% of these develop ulcerative colitis 18
-
autoimmune hepatitis (AIH-PSC overlap)
Diagnosis
The diagnosis can be made when there are classical imaging features in the correct clinical context, and secondary causes of cholangitis have been excluded 16.
Clinical presentation
The average age of diagnosis of primary sclerosing cholangitis is 54 years (range 6-93) with increased occurrence in men (63%) 15. A large number of asymptomatic individuals are identified upon investigation of persistently deranged liver function tests. Symptomatic individuals commonly present non-specifically with fatigue. More specific symptoms include pruritus, jaundice or gastrointestinal bleeding 16.
Pathology
Unfortunately, no histological findings are pathognomonic for primary sclerosing cholangitis 2. Frequent findings include 2-4:
periductal fibrosis (onion skin lesions)
periportal eosinophilic infiltrate
paucity of ducts
Markers
Liver function tests will usually have a cholestatic pattern with an elevated alkaline phosphatase (ALP) and bilirubin 2.
Most patients demonstrate at least one type of autoantibody, typically anti-smooth muscle antibody (ASMA) and antinuclear antibody (ANA), which are seen in up to 75%. p-ANCA is also positive in up to 80% of patients with primary sclerosing cholangitis 19.
Radiographic features
The entire biliary tree (both intra- and extrahepatic) may be involved, with multiple strictures scattered along its length. In ~20% only the intrahepatic and proximal extrahepatic bile ducts are involved 4.
The end result of primary sclerosing cholangitis is cirrhosis which is usually characterised by a markedly distorted biliary tract and atrophy of the entire liver with the exception of the caudate lobe which is hypertrophied in almost all cases (68-98%) 1-5. Atrophy involving the left lobe is a feature that somewhat distinguishes it from cirrhosis from other causes, in which the left lobe is usually hypertrophied 1.
Ultrasound
Ultrasound is able to demonstrate both the changes of cirrhosis and irregularity of bile duct calibre. Additionally, brightly echogenic portal triads may be visible.
Primary sclerosing cholangitis is a risk factor for developing gallbladder cancer, so gallbladder polyps should be considered malignancy until proven otherwise.
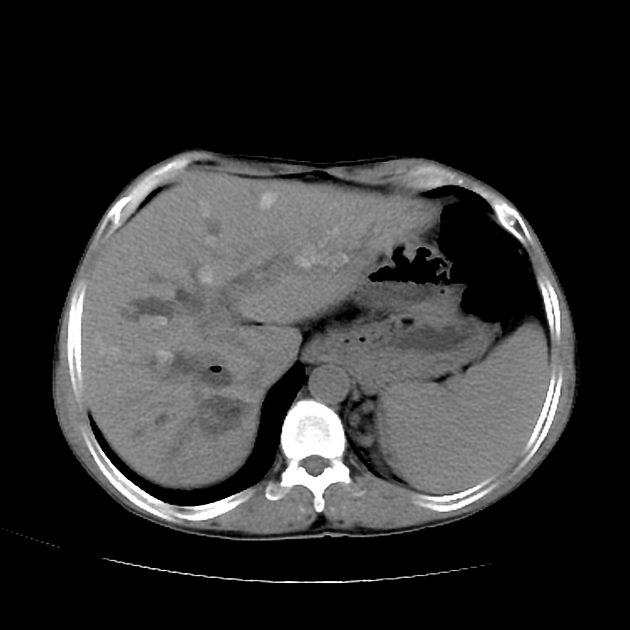
CT
contour abnormalities and atrophy (see above)
marked caudate lobe hypertrophy
the atrophied liver is of lower density than the hypertrophied caudate lobe 1
multiple linear discontinuous low-density regions representing dilated intrahepatic bile duct segments 1
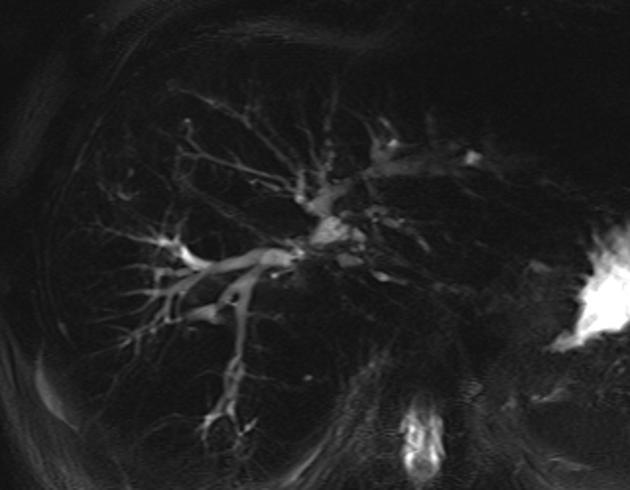
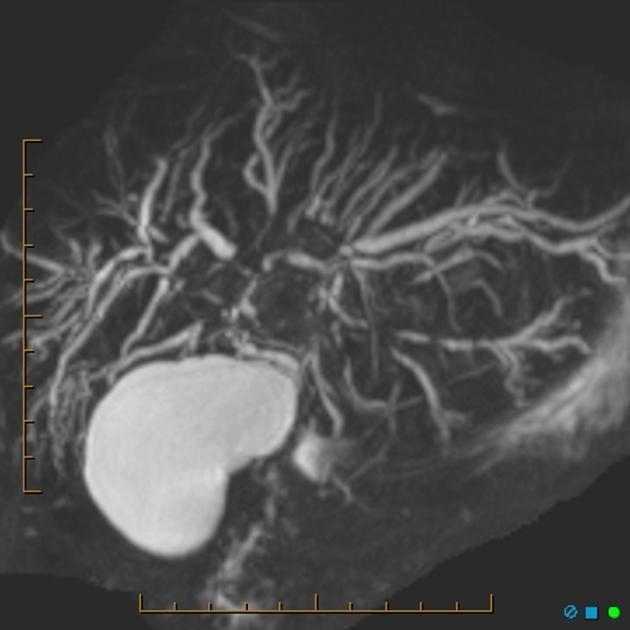
MRCP and ERCP
ERCP has traditionally been the gold standard for the depiction of the biliary tree, and also offers the ability to perform cholangioplasty, if necessary. In practice, however, MRCP is used before ERCP since it is non-invasive, can assess the liver, and avoids the 10% risk of hospitalisation from ERCP in primary sclerosing cholangitis patients 17.
The characteristic findings on direct imaging of the biliary tree are 2,3,5:
-
multiple segmental strictures
typically short segment
intervening segments are of normal calibre or slightly dilated (beading)
-
biliary dilatation: may be present in ~85% of cases 9
general: ~35%
segmental: ~50%
biliary diverticula
mural irregularities
distortion of the biliary tree due to associated cirrhosis
Treatment and prognosis
The only cure available at present is orthotopic liver transplantation (OLT) with 5-year survival rates approaching 80% 10,11. However, there is evidence that primary sclerosing cholangitis may recur in 5-20% of patients post-transplantation 10-12.
No medical therapy has stood the test of time, with ursodeoxycholic acid, immunosuppression, chelation and antifibrolytic therapy unable to demonstrate consistent benefits over placebo 8.
Cholangioplasty of dominant strictures is usually performed in a retrograde fashion via ERCP or via a transhepatic approach 6,7.
Complications
cholangiocarcinoma develops in ~15% of patients 6
-
4x greater risk compared to IBD patients without primary sclerosing cholangitis
10x greater risk compared to general population
hepatocellular carcinoma: appears to be not increased beyond other causes of cirrhosis 14
Differential diagnosis
General imaging differential considerations include:
-
cirrhosis from other causes
caudate lobe not as frequently or as markedly enlarged
left lobe usually also hypertrophied
-
IgG4-related sclerosing cholangitis
these patients tend to be older and more symptomatic with involvement of other systems besides the bile ducts 17
IgG4 levels 4x normal; ratio of IgG4 to immunoglobulin 1 of >0.24 17
responds to steroid therapy
-
secondary sclerosing cholangitis
biliary strictures from other causes, e.g. surgery, ischaemia
cholangiocarcinoma (can also occur as a later complication)
-
especially difficult to distinguish when primary sclerosing cholangitis is limited to the intrahepatic biliary tree
young women more frequently affected
high antibody titres 4
Alagille syndrome (arteriohepatic dysplasia)
hepatic sarcoidosis: see abdominal manifestations of sarcoidosis
















 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.