Solid pseudopapillary tumors of the pancreas are rare and usually benign pancreatic cystic neoplasms that are most commonly seen in young females.
On this page:
Terminology
The tumor has been referred to with multiple different names, including:
solid pseudopapillary tumor (SPT) of the pancreas
solid pseudopapillary neoplasm (SPN)
solid pseudopapillary epithelial neoplasm (SPEN)
papillary cystic neoplasm of the pancreas
Hamoudi tumor
Gruber-Frantz tumor (or just Frantz tumor)
Epidemiology
They are rare and thought to account for 1-2% of exocrine pancreatic tumors. They tend to present in young non-White females around the 2nd and 3rd decades of life (the "daughter" tumor) 10.
Associations
pancreatic dorsal agenesis: possible association 5
Clinical presentation
Most patients are asymptomatic at diagnosis. They may occasionally present with a gradually enlarging abdominal mass or vague abdominal pain.
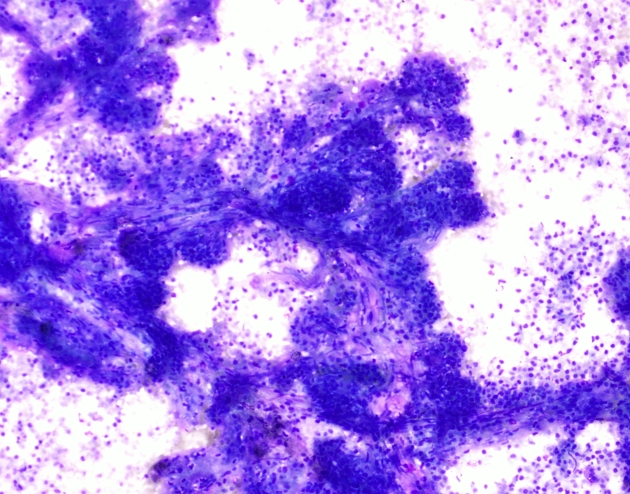
Pathology
The tumors frequently contain varying amounts of necrosis, hemorrhage, and cystic change. Lesions can be large at the time of diagnosis (median size ~8 cm) 2.
Location
There is a greater predilection to occur at the pancreatic tail.
Radiographic features
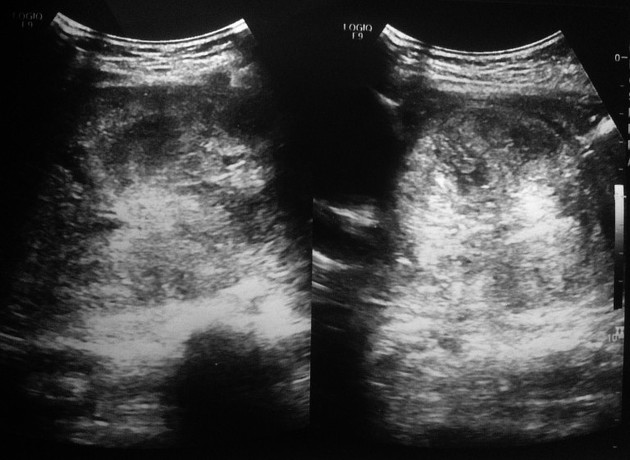
Ultrasound
Large well-defined mass with heterogeneous appearances, due to its solid and cystic composition.
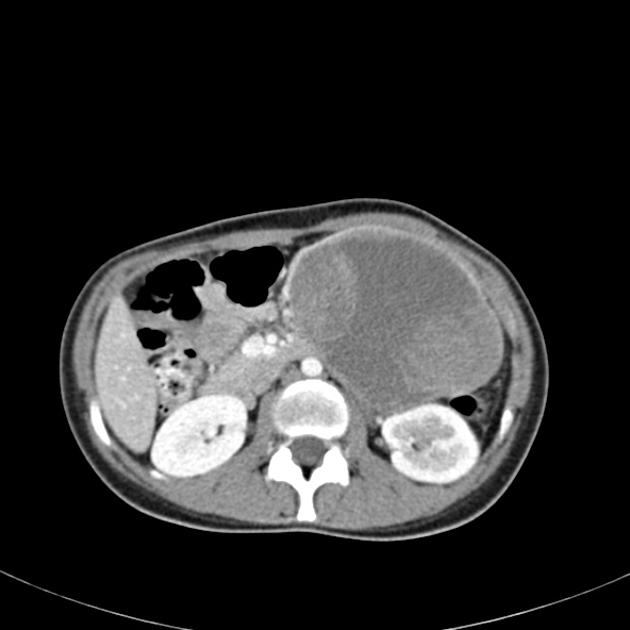
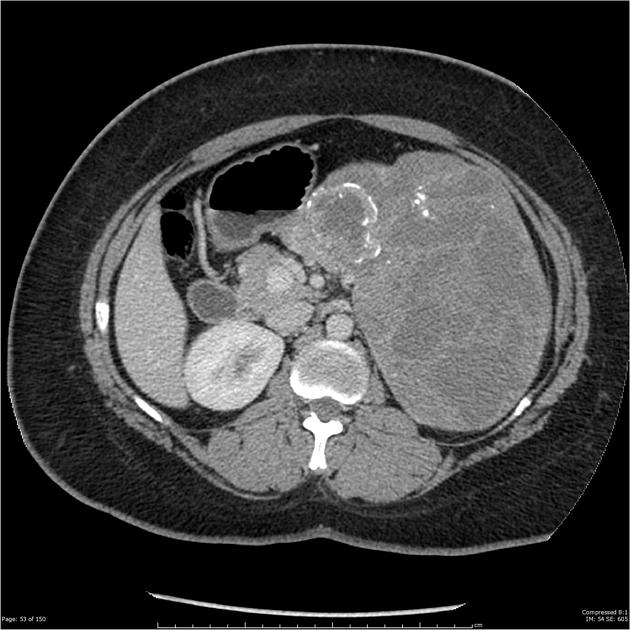
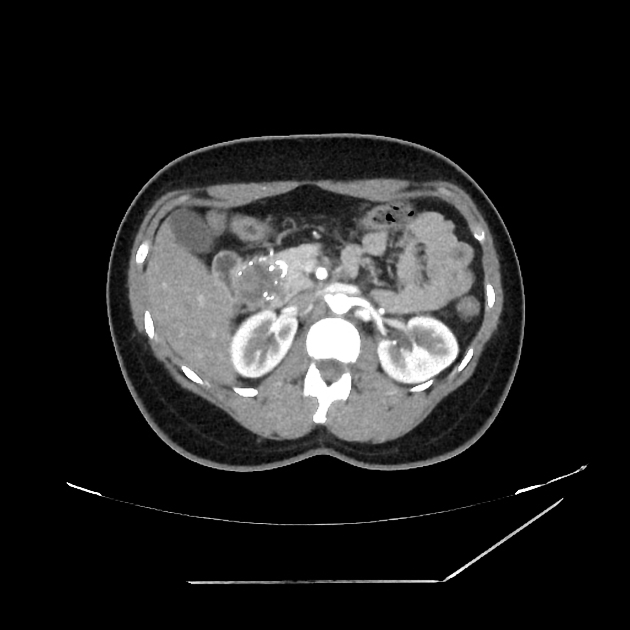
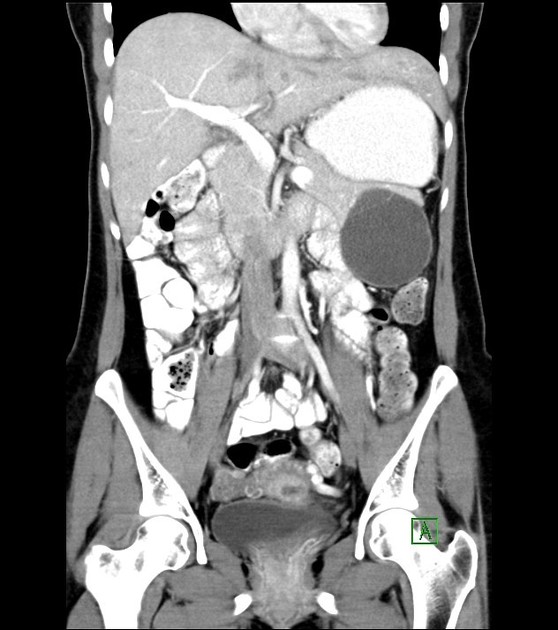
CT
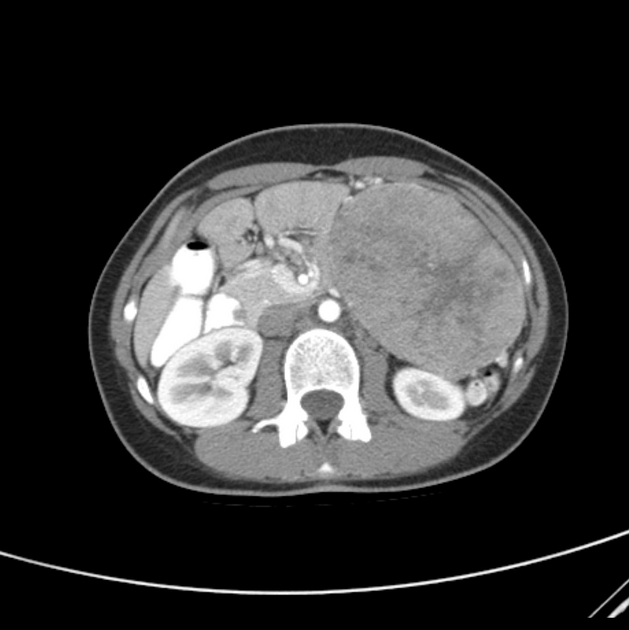
Usually seen as a well-encapsulated lesion with varying solid and cystic components owing to hemorrhagic degeneration. Following IV contrast administration, enhancing solid areas are typically noted peripherally, whereas cystic spaces are usually more centrally located. Calcifications and enhancing solid areas may be present at the periphery of the mass.
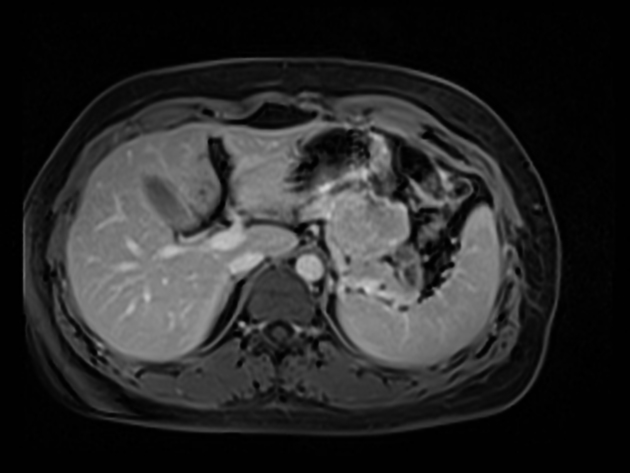
MRI
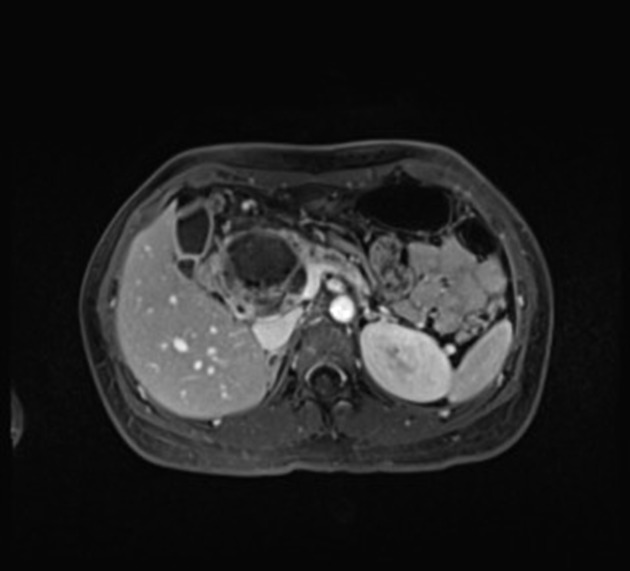
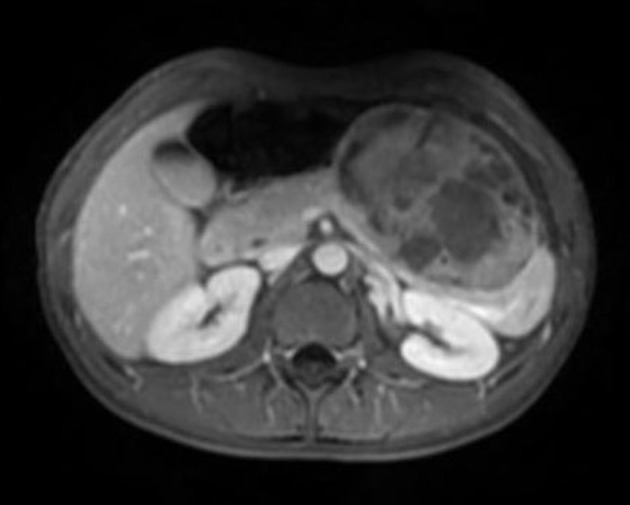
Typically demonstrates a well-defined lesion. May show a pure solid consistency in ~80% of cases 6.
Reported signal characteristics include:
T1: low to heterogeneous signal intensity 1,6
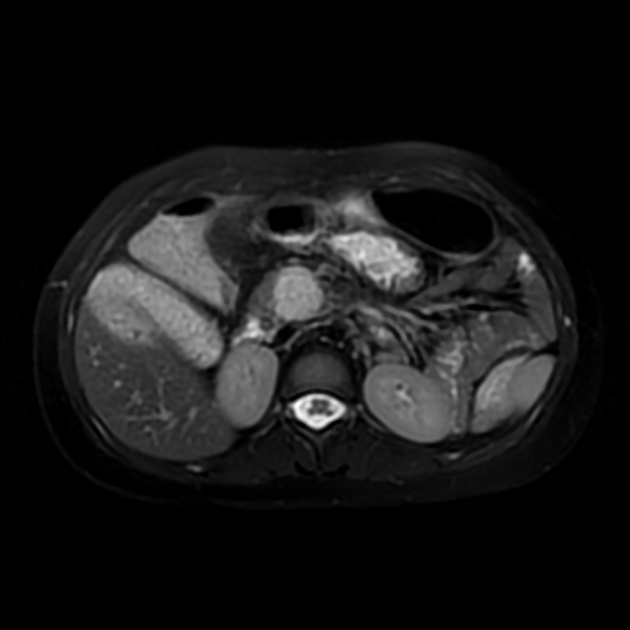
T2: heterogeneous to high signal intensity 1,6
T1 C+ (Gd): can show early heterogeneous and slowly progressive enhancement 11
Treatment and prognosis
While most lesions are benign, ~15% can be malignant. Complete resection is associated with long-term survival even in the presence of metastatic disease.
History and etymology
It was first described by renowned American surgical pathologist, Virginia K Frantz (1896-1967) 9 et al. in 1959, hence the historical name "Frantz tumor" 4,5.
Differential diagnosis
pancreatic neuroendocrine tumor: can have similar imaging features and be difficult to differentiate on imaging 12,13




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.