Solvent abuse (toluene being the major component) is remarkably common, especially in young people with psychosocial stressors, and with chronic use can lead to numerous ill-effects, particularly affecting the central nervous system.
On this page:
Epidemiology
Solvent abuse is geographically widespread, and is particularly common among children and young adults with psychosocial stressors 1.
Clinical presentation
Clinical presentation is varied and depends on chronicity.
Acute exposure at high enough concentrations results initially in delirium, confusion and incoordination, and eventually (when higher concentrations are reached) hallucinations and psychosis. Decreased consciousness and coma can occur at still higher concentrations 3.
Chronic use, typically of a number of years, results in permanent neurological signs and symptoms including 1,3:
- insomnia: most common
- memory impairment
- anosmia
- cerebellar dysfunction
- tremor
- ataxia
- dysarthria
- nystagmus
- hyperreflexia
- rigidity
- tinnitus
- temporal lobe epilepsy
Pathology
The main constituent in most modern solvents is toluene (C7H8), also known as methylbenzene, a lipid-soluble aromatic hydrocarbon. When inhaled, toluene is rapidly absorbed into the bloodstream and distributed to lipid-rich tissues (including the brain) where it accumulates. Demyelination and gliosis are histologically demonstrable in regions of abnormal T2 signal.
The cause of low T2 signal in the basal ganglia and thalami (see below) is uncertain, and could relate to iron deposition 1.
Radiographic features
CT
CT changes are non-specific and often absent. Generalized, age-inappropriate, cerebral volume loss may be seen 1.
MRI
MRI is the modality of choice for evaluation of cerebral changes related to toluene toxicity.
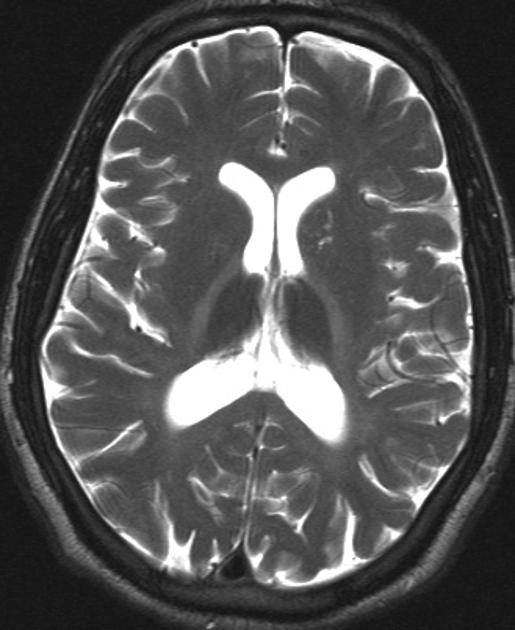
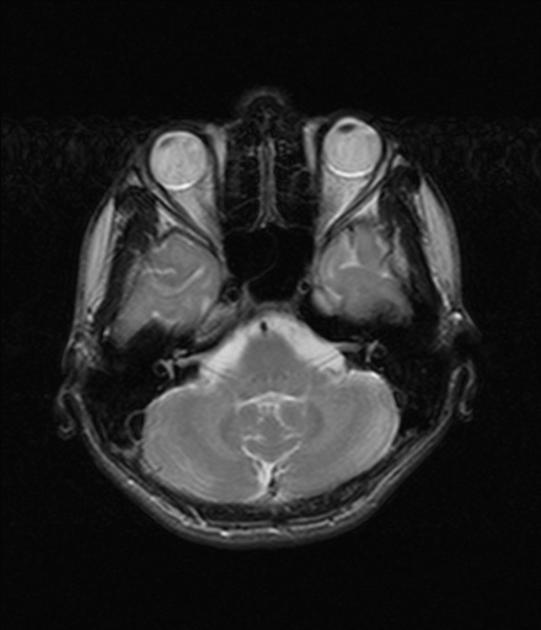
White matter T2 hyperintensity (focal and diffuse) is the most common finding, seen in approximately 50% of patients, typically after at least 4 years of abuse. Distribution of changes is widespread, typically affecting the periventricular / centrum semiovale, cerebellar hemispheres, internal capsule and brain-stem 1.
Thalamic hypointensity (best seen on T2 weighted images) is seen in 20%, with greater than expected reduced signal also seen in the red nuclei, substantia nigra and dentate nuclei 1.
Cerebral and cerebellar volume loss, including thinning of the corpus callosum, with associate sulcal and ventricular dilatation is also recognized 1.
Differential diagnosis
Other causes of thalamic hypointensity include metabolic disorders such as ceruloplasmin deficiency and lysosomal storage disorders 2.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.