Presentation
Cardiac arrest, pulseless left arm. Preceeded by chest pain.
Patient Data










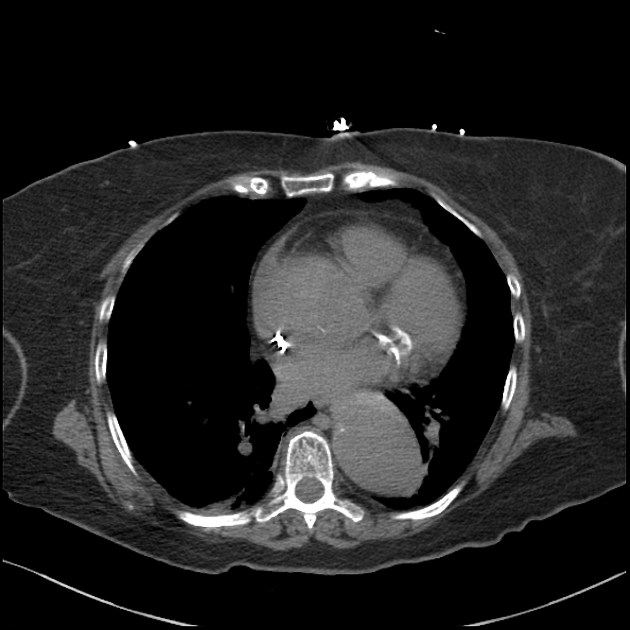
Eccentric increased density on the non-contrast study (best in the arch) represents acute aortic intramural hematoma, commencing at the aortic root, and extends into the descending thoracic aorta at the level of T10. No acute dissection flap is seen. Intramural hematoma extends into bilateral common carotid arteries proximally to the level of C5; vessel patency and opacification above this level appear maintained. Intramural hematoma extends for a short distance (approximately 1 cm) into the proximal left vertebral artery, with preservation of distant vessel patency. A large intramural hematoma causes near-complete occlusion of the left subclavian, axillary and brachial arteries with a thin sliver of enhancing lumen remaining present. Right upper limb arteries are well opacified.
Just proximal to the dissection in the proximal descending aorta, a small contrast focus in the right posterolateral aspect of the intramural hematoma is seen in continuity with a right posterior intercostal artery and represents an intramural blood pool (IMBP).
Thin pericardial effusion and stranding in the superior epicardial fat. No features of pericardial tamponade.
The chronic type B aortic dissection appears similar in extent to the prior studies. This commences just distal to the left subclavian artery origin, and is chronically thrombosed from the level of the mid-thoracic aorta inferiorly. The opacified true lumen extending further distally to the level of L3 is similar in extent to the initial study performed 6 years prior. The celiac trunk, superior and inferior mesenteric arteries are supplied by the true lumen. Hypoattenuation indicating hypoperfusion of the right renal parenchyma.
Other findings
Dual-lead pacemaker in a left pectoral position. Scattered coronary artery calcification. No significant mediastinal or hilar lymphadenopathy. Bilateral lower lobe subsegmental atelectasis. Mild dependent ground-glass opacity within the upper lobes bilaterally suggest mild pulmonary edema. No pleural effusion or pneumothorax.
The liver, gallbladder, spleen, pancreas and right adrenal gland appear normal. 18 mm left adrenal nodule is stable. Small splenunculus. Noninflamed distal colonic diverticulosis. No intraperitoneal free fluid, free air or lymphadenopathy.
No acute bony abnormalities.
IMPRESSION
- Acute type A aortic intramural hematoma, on a background of chronic type B aortic dissection. Intramural hematoma extends from the aortic root to approximately the T10 level. Small intramural blood pool in the proximal descending aorta. Near-complete occlusion of the left subclavian, axillary and brachial arteries secondary to intramural hematoma extension. Intramural hematoma also extends into bilateral common carotid arteries to the level of C5, and proximal aspect of the left vertebral artery, without causing significant stenosis of these vessels. No pericardial effusion.
- Mild pulmonary edema
Case Discussion
Aortic intramural hematoma is part of the acute aortic syndrome spectrum and is a precursor to frank dissection.
This case also has an excellent example of an intramural blood pool that occur within an intramural hematoma.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.