Presentation
Painful lump on the medial aspect of his left knee.
Patient Data
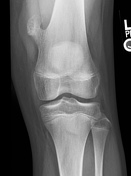
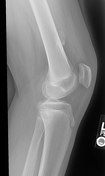
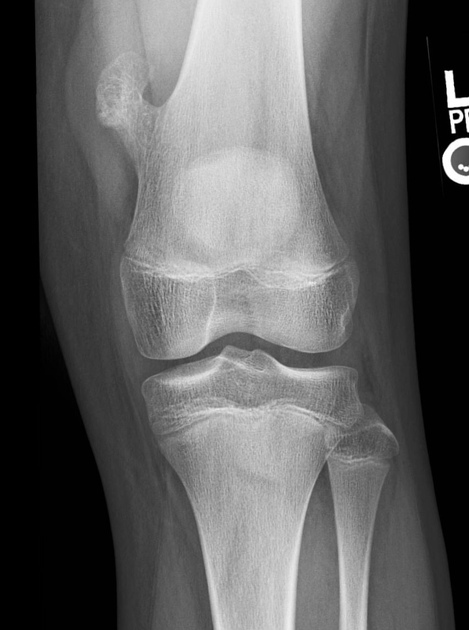
There is a pedunculated osteochondroma measuring approximately 3.5 x 3 cm arising from the medial cortex of the distal femur at the meta-diaphyseal junction. No discrete associated soft tissue mass. No joint effusion or abnormal soft tissue calcifications
The bone density is normal and there is no acute osseous injury.
Case Discussion
Osteochondromas are benign bone tumors that represent 10-15% of all bone tumor diagnoses. They are often solitary, sporadic, and asymptomatic which results in them most commonly being discovered as an incidental finding.
They develop during childhood (a period of rapid skeletal growth) and remain for life (i.e. they do not involute). Most commonly, they appear in the appendicular skeleton in the femur (30% of cases), tibia (15-20%), and humerus (10-20%), and less commonly they will appear in the hands, scapula, feet, pelvis, and spine.
The most feared sequela of an osteochondroma is malignant transformation to chondrosarcoma, and this occurs between approximately 1% (if solitary and sporadic) to 5-25% of the time (hereditary osteochondromatous syndromes, such as hereditary multiple exostoses i.e. diaphyseal aclasis and Trevor disease i.e. dysphasia epiphysealis hemimelica).
Post-pubertal pain at the site of the mass, localized soft tissue swelling, and a cartilage cap measuring greater than 1.5 cm all increase the likelihood of malignant transformation.
Most osteochondromas require no treatment, particularly if they are incidental findings. However, some patients undergo resection for cosmetic reasons, and all masses with malignant potential should undergo limb-sparing wide local excision. All excision should be executed thoughtfully, as local recurrence is estimated at 2-15%.
The primary role of the radiologist in assessing an osteochondroma is evaluating the malignant potential of the mass and to assist in possible surgical planning. To assess the number of osteochondromas to determine the possibility of a familial osteochondromatous syndrome as well as the lucency of the bone, any cortical destruction, and surrounding soft tissue swelling is critical.
This case was submitted with supervision and input from:
Soni C. Chawla, M.D.
Associate Professor
Department of Radiological Sciences
David Geffen School of Medicine at UCLA
Olive View - UCLA Medical Center




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.