Acromioclavicular joint injuries, commonly shortened to ACJ injuries, are characterized by damage to the acromioclavicular joint and surrounding structures. Almost invariably traumatic in etiology, they range in severity from a mild sprain to complete disruption.
On this page:
Epidemiology
Acromioclavicular joint injuries can occur at any age but most frequently occur in the 20-40 year age group, being 5x more common in males than females. They are a common contact sports injury in young male athletes 9.
Clinical presentation
Patients can present with non-specific shoulder pain and swelling. A visible deformity is uncommon. Low-grade injuries can often be overlooked both clinically and radiologically. Pain may be provoked with the cross-body and/or O'Brien active compression test 9.
Pathology
There are two main mechanisms of acromioclavicular joint injury 7,9:
direct: direct blow or fall onto the shoulder with an adducted arm results in a superior force onto the acromion with clavicular movement restricted at the sternoclavicular joint results in the acromion pushed forcibly inferiorly and medially with respect to the clavicle
indirect: can occur from a fall onto an outstretched hand or elbow resulting in the humerus being pushed into the acromion, which in turn results in lower-grade injuries typically involving the AC ligaments but sparing the coracoclavicular ligament
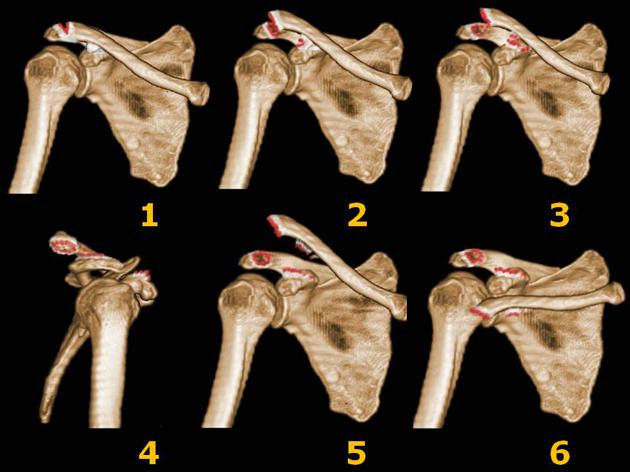
Classification
Imaging can be used to classify acromioclavicular injuries, with the Rockwood system most commonly used to classify injuries into six types. Other described systems include the Tossy and the Allman grading system.
Radiographic features
In most cases, plain radiographs (including an axillary view) are sufficient for accurate grading although CT or MRI may be useful in cases where plain films are thought to underrepresent the degree of injury.
Plain radiograph
Standard acromioclavicular joint radiographs consist of a clavicle series including an AP and cephalic angled oblique (10-15º) views. Additional weight-bearing stress views may be of benefit if:
initial radiographs are normal, but an injury is suspected
surgical intervention on a type III injury would be contemplated (see below) 7
These are performed with the patient erect and holding a weight in the arm. If the joint is normal, then acromioclavicular alignment should remain normal and symmetric.
Features of acromioclavicular joint injury include 6:
-
soft tissue swelling/stranding
may be the only finding in type I injuries
-
widening of the acromioclavicular joint
normal: 5-8 mm (narrower in the elderly)
greater than 2-4 mm asymmetry (compared to radiographs of the contralateral side)
-
increased coracoclavicular distance
normal: 10-13 mm
greater than 5 mm asymmetry (compared to the contralateral side)
-
superior displacement of the distal clavicle
the inferior edge of the acromion should be level with the inferior edge of the clavicle
Treatment and prognosis
Treatment largely depends on the age and lifestyle of the patient as well as the type of injury according to the Rockwood classification. Around 80% (range 70-90%) of acromioclavicular joint injuries are "low grade" 9. In general types I and II are treated conservatively, types IV, V, and VI are treated surgically, and type III injuries are variably treated 4.
type I and II: conservative management consists of ice, analgesics and shoulder rest in a sling
type III: the evidence does not support surgical intervention on type III injuries as a general rule; the selection of which patients with type III injuries for surgical intervention is difficult, but patients who are particularly thin, require a great range of motion or do heavy lifting may benefit from operative repair 4,5
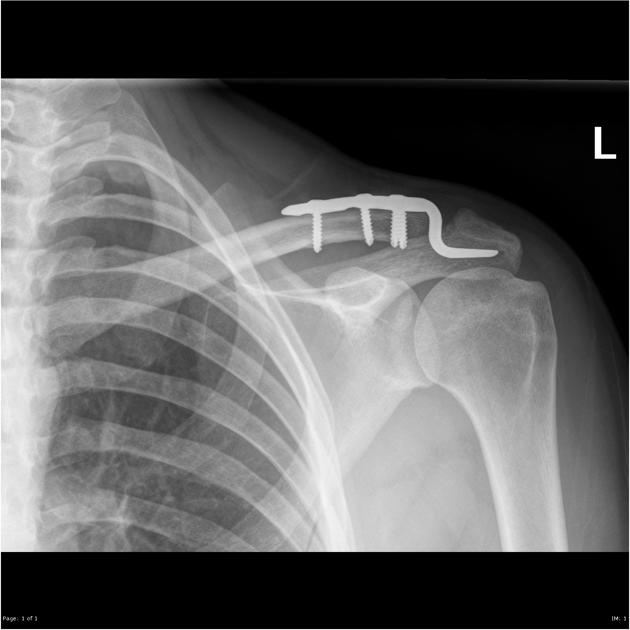
types IV-VI: surgical internal fixation is typically achieved with a hook plate, which in most cases needs to be eventually removed. K-wires have also been used, although rare cases of wire migration into vital organs, has dissuaded many surgeons from using them 4
Complications
Just as an injury to other joints, prior acromioclavicular dislocation predisposes the joint to osteoarthritis. Surgical complications include migration of hardware and infection.
Practical points
In addition to commenting on whether or not a subluxation/dislocation is present a number of features should be examined and commented upon:
presence of soft tissue swelling
-
degree of subluxation of the clavicle
type II: inferior border of clavicle not elevated beyond the superior border of the acromion
type III: inferior border of the clavicle is elevated beyond the superior border of the acromion, but the coracoclavicular distance is not greatly increased (less than twice normal)
type V: marked superior elevation of the clavicle with coracoclavicular distance more than twice normal
-
direction of dislocation (use axillary view)
posteriorly into trapezius: type IV
inferiorly below the coracoid process: type VI
any fractures present
A careful inspection of the periphery of the image is also required, to ensure no rib fracture, pneumothorax or incidental lung, mediastinal or osseous lesion is present. These do not usually constitute 'relevant negatives' and as such, no comment is required.
Mnemonic
A helpful mnemonic for causes of acromioclavicular dissociation is SHIRT:
S: Scleroderma
H: Hyperparathyroidism
I: Infection
R: Rheumatoid arthritis
T: Trauma












 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.