Carotidynia, also known as Fay syndrome, is a rare syndrome characterized by neck pain in the region of the carotid bifurcation.
It was classified by the International Headache Society (IHS) in 1988 as an idiopathic neck pain syndrome associated with tenderness over the carotid bifurcation without structural abnormality.
On this page:
Terminology
A discrete clinicoradiological entity has been described and named transient perivascular inflammation of the carotid artery syndrome (TIPIC syndrome) 14.
There remains confusion in the literature as to what the term carotidynia actually refers to, with some authors suggesting that the term should be reserved for a pain syndrome with no structural abnormality, whilst others contend that it is a defined inflammatory condition of the carotid (TIPIC syndrome). The latter seems to be more useful as it correlates to a specific syndrome with defined imaging features (thickening and inflammation around the carotid bifurcation) and prognosis (spontaneous resolution within 1-2 weeks).
Epidemiology
The age of onset is thought to commonly range between 30 and 50 years 18.
Clinical presentation
Patients with carotidynia present with unilateral neck pain in the region of the carotid bifurcation 1. The pain typically tends to be dull and throbbing in nature, continuous, and usually localized over the carotid bifurcation, although it may radiate to the ipsilateral mandibular, buccal, ocular, or auricular regions and is usually associated with tenderness on palpation in the region of the affected area (usually around the level of the carotid bifurcation). Carotidynia is usually a diagnosis of exclusion 16.
Pathology
The etiology of carotidynia remains unclear, however, it appears to be an inflammatory process involving the carotid wall, including the adventitia 1.
Classification
Carotidynia may be classified into three distinct entities 10:
migrainous
non-migrainous (or classic)
arteriosclerotic
Markers
Many inflammatory markers tend to be elevated, including 4:
serum amyloid A protein (SAP)
fibrin degradation products/D-dimer
Radiographic features
Contrary to the diagnostic criteria proposed by the Headache Classification Subcommittee of the International Headache Society (IHS) 3, which suggests that a carotid structural abnormality should be absent, relatively consistent imaging findings are encountered 1,2.
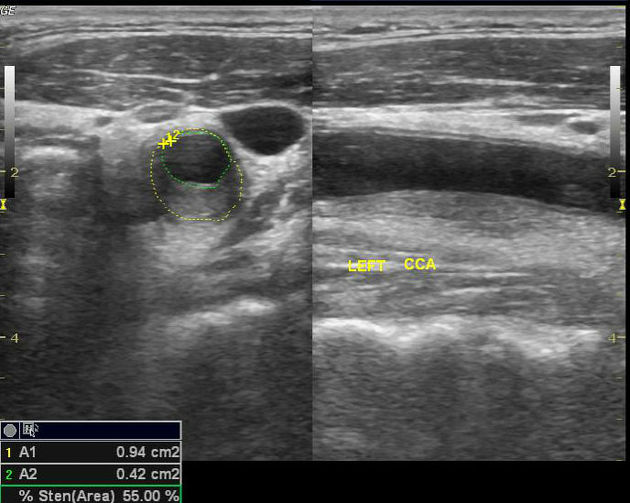
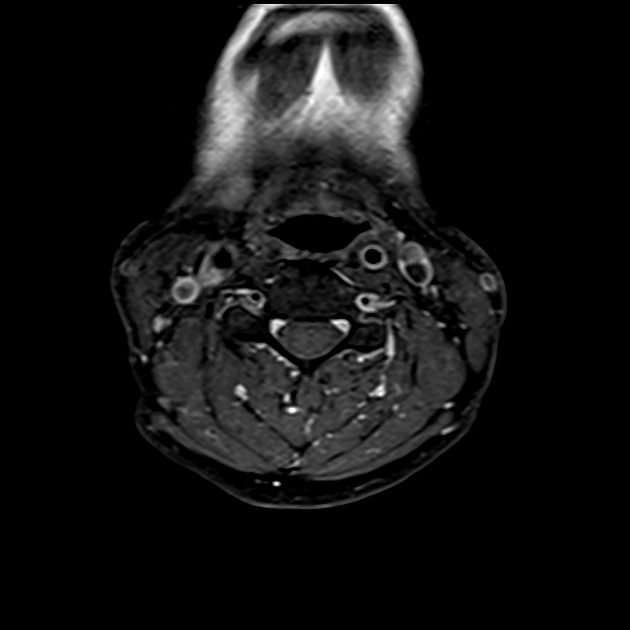
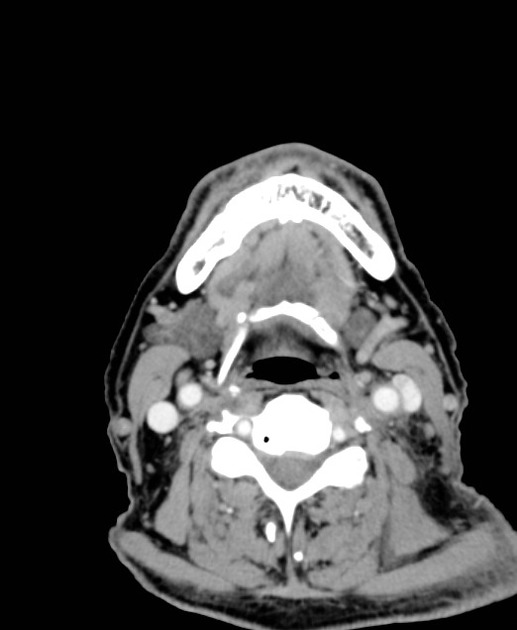
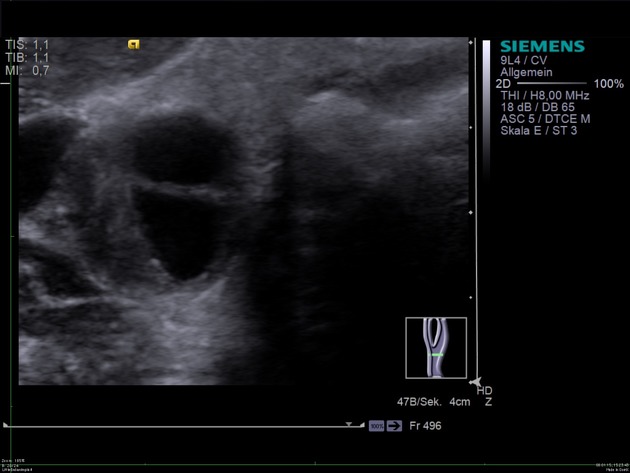
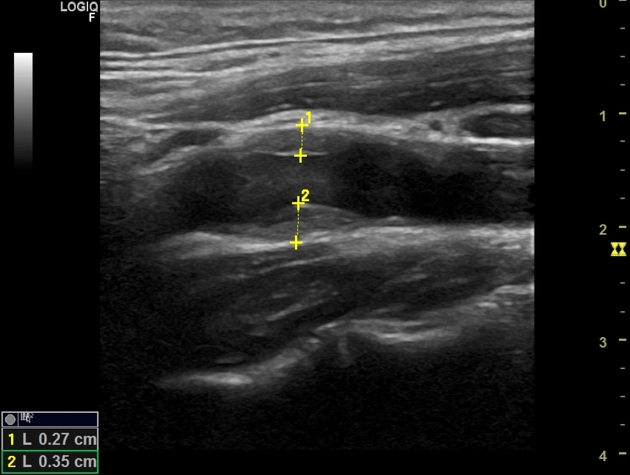
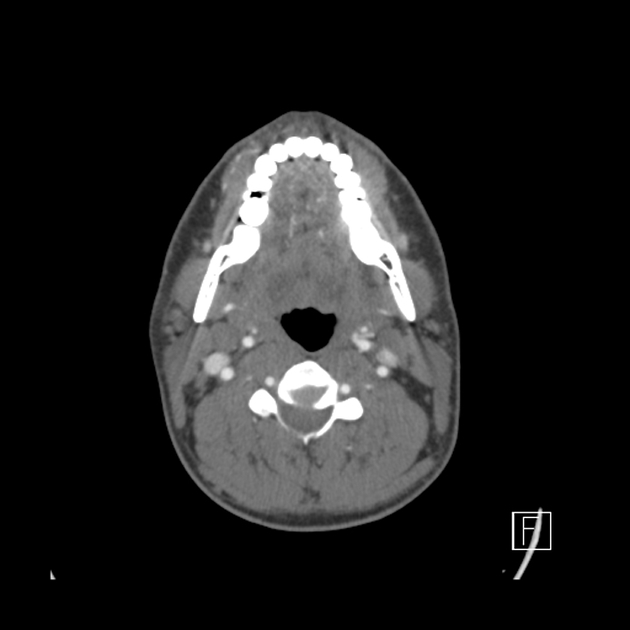
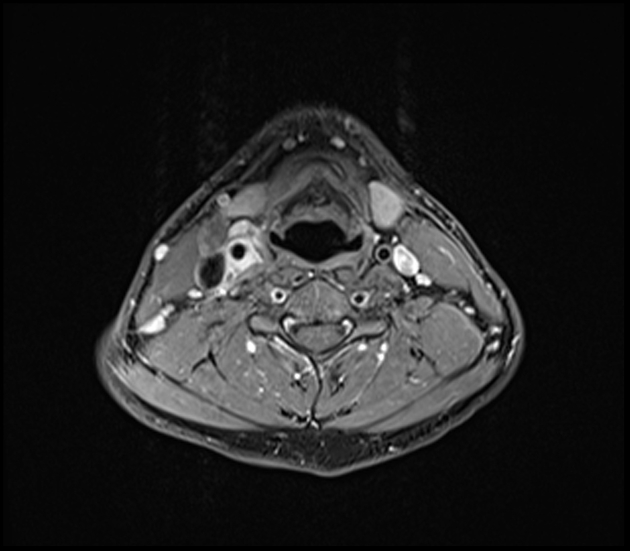
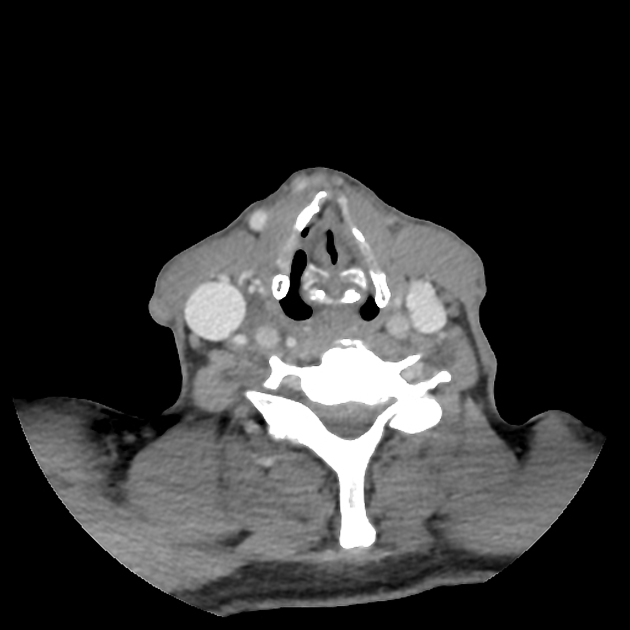
Regardless of modality (ultrasound, CT, MRI), typical features of carotidynia include 1,2:
region: distal common carotid artery, bulb, and proximal internal carotid artery
lumen: mild narrowing
-
wall
eccentric thickening of the carotid wall/perivascular tissues
enhancement (CT, and more so MRI)
transient fatty plaque during healing 1
surrounding soft tissues: fat stranding
"King Kong carotid" has been suggested by some neuroradiologists as an imaging sign of TIPIC syndrome. The eccentric thickening of the pericarotidian tissues with minimal narrowing of the vessel lumen is reminiscent of the hand of King Kong in the original motion picture incompletely encircling Ann Darrow without squeezing her too hard. Coincidentally, the actress who played the role of Ann Darrow was named Fay Wray, which has relevance to the eponymous name for this condition, Fay syndrome 15.
Treatment and prognosis
Carotidynia is usually self-limiting, spontaneously resolving within 2 weeks. Resolution can be expedited with non-steroidal anti-inflammatory drugs (NSAIDs) or steroids 1.
History and etymology
It was first described in 1927 by American neurologist Temple Fay (1895-1963) 7.
Differential diagnosis
The differential includes other vascular causes of neck pain, including 1:
-
large vessel vasculitides
Other wider clinical differential considerations include 2:
submandibular gland diseases
head and neck tumors




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.