Cerebellar mutism syndrome, also known as post-operative pediatric cerebellar mutism syndrome (pCMS), usually develops after resection of midline cerebellar or intraventricular tumors in the posterior cranial fossa. Typical features of this condition are transient mutism, ataxia, hypotonia and irritability.
On this page:
Terminology
The nomenclature of this syndrome has historically been confusing, due to a variety of terms including akinetic mutism, cerebellar cognitive and affective syndrome, posterior fossa syndrome, transient cerebellar mutism and cerebellar mutism syndrome. In 2016, an international consensus formulated a new definition of “post-operative pediatric cerebellar mutism syndrome” (pCMS) as the preferred term for this condition 2,4.
Epidemiology
Postoperative cerebellar mutism syndrome ranges from 7%-50% of children after posterior fossa surgery 1. Although this clinical entity is mainly in children, there are also rare reports of cerebellar mutism in adults 2.
Risk factors
- tumor type (mainly medulloblastoma) 1-4
- infiltration/compression of the brainstem 1-4
- cerebellar vermian/midline location 1-4
- high fourth ventricle location 2,4
- tumor size >5 cm 1
Other uncommon causes of this syndrome include posterior fossa hematomas, arteriovenous malformations, traumatic cerebellar injury and infections 2,5.
Clinical presentation
Cerebellar mutism syndrome usually occurs one to two days but sometimes until seven days following surgery of a posterior fossa tumor in the pediatric patient 1-5. A typical feature is a transient mutism, which is commonly associated with emotional lability, cranial neuropathies, oropharyngeal dysfunction/dysphagia and motor disorders, which include ataxia, hypotonia, flaccid hemiparesis and hypokinesia 1-4.
The mutism is transient and usually lasts between a few weeks to six months 1,3. The recovery phase might last two years and some patients may have permanent impairments of speech and language (dysarthria, dysfluency or slowed speech rate) or other cognitive abnormalities 1-3.
Pathology
The most likely explanation for cerebellar mutism syndrome is a bilateral post-surgical injury (edema or vascular insufficiency) to any component of the proximal cerebellar pathway 1-4, which is also known as the dentate-thalamo-cortical tract 3,4. Disruption of neural circuitry along this tract can result in the cerebellar-cerebral diaschisis, which leads to dysfunction of supratentorial brain areas due to a lack of excitatory input from the cerebellum 1-4.
Radiographic features
MRI
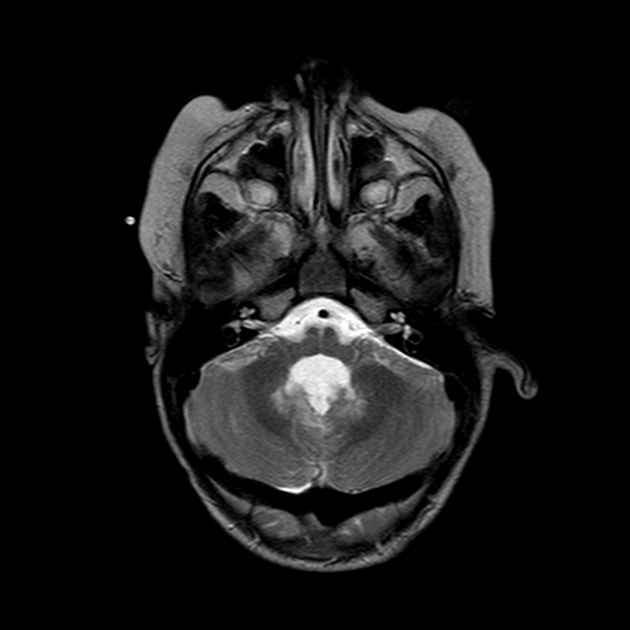
Postoperative MRI brain usually shows signal abnormalities within the superior cerebellar peduncles and dentate nuclei 3.
- T2: hyperintense signal within the superior cerebellar peduncles and dentate nuclei 3
- MR tractography: may show disruption of the dentate-thalamo-cortical tract 4
Treatment and prognosis
Counseling of the parents and the patients about this condition, supportive care, early rehabilitative therapies and neuropsychological follow-up are the most significant parts of the management of patients with cerebellar mutism syndrome 2,4.
History and etymology
In 1939, Bailey described some components of this condition for the first time 5. Cairns in 1948, and Daly and Love in 1958 reported cases of patients with symptoms of “akinetic mutism” following posterior fossa surgery. The first description of the term cerebellar mutism was in 1985, by Rekate 2,3. Since then, several articles were published describing this syndrome.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.