Coronary arteriovenous fistulas (CAVFs) are rare coronary artery anomalies whereby there is a fistula between a coronary artery and, most commonly, the right side of the cardiac circulation.
On this page:
Terminology
Although a CAVF, in the strictest sense of the term, implies a communication between the coronary arteries and coronary venous system, the term has been adopted and accepted to refer to any communication between the coronary arteries and other cardiac or vascular structures 1. Furthermore, large CAVFs have sometimes been known as ‘cor medusae’ in the literature 2.
Epidemiology
CAVFs are rare, being present in approximately 0.002% of the population 3,4.
Clinical presentation
Patients may be asymptomatic 1,3-5, but may also have a range of clinical features:
angina, especially on exertion 1,3-5
dyspnea, especially on exertion 1,3-5
cardiac murmur heard continuously in systole and diastole, decreases in intensity during inspiration 1,3-5
Complications
coronary artery or fistula rupture causing cardiac tamponade 3,4
acute myocardial infarction due to fistula thrombosis 3,4
Pathology
The most common origins for the CAVF are the RCA (50%) and LAD (42%) while the most common drainage sites are the relatively low-pressure right ventricle (41%), right atrium (26%), or pulmonary artery (17%) 3,4. However, any coronary artery may be an origin and the fistula may less commonly drain into the coronary sinus, superior vena cava, or left-sided cardiac chambers 3,4.
Due to the most common drainage sites being in the right side of the cardiac circulation, CAVFs often cause a left-to-right shunt and result in the ‘coronary artery steal’ phenomenon 3-5. This coronary artery steal results in less blood being delivered to the myocardium at the origin of the fistula causing continual myocardial ischemia and the development of the aforementioned clinical presentation 3-5.
Etiology
CAVFs are most commonly congenital, but can also be rarely acquired 3,4. Risk factors and etiologies for acquired CAVFs include 4:
pathology-related: acute myocardial infarction, hypertrophic cardiomyopathy, dilated cardiomyopathy, coronary artery aneurysm rupture into adjacent structures 4
iatrogenic: percutaneous coronary intervention, coronary artery bypass grafting, cardiac transplant, pacemaker placement 4
chest trauma 4
Classification
They can be classified according to their origin, drainage site, or complexity; the number of fistulous tracts; or the presence of accompanying anomalies.
One method of classifying coronary arterial fistulae is as 8
coronary cameral fistula: which coronary arteries drain into a cardiac chamber
-
coronary arteriovenous fistulae
coronary artery-to-coronary sinus (or other cardiac vein) fistula
complex coronary fistula: multiple origin and drainage sites, with complex communications between
Radiographic features
Imaging can demonstrate not only the CAVF, but also the numerous complications (as listed below).
Plain radiograph
Often unremarkable, but may have signs of congestive heart failure (e.g. cardiomegaly) 4.
Angiography (DSA)
Coronary artery angiography is an invasive imaging modality for evaluating CAVFs and has long been considered to be the gold-standard 3,4,6,7. Angiography is able to provide details regarding the origin, drainage, size, and course of CAVFs 3,4,6,7.
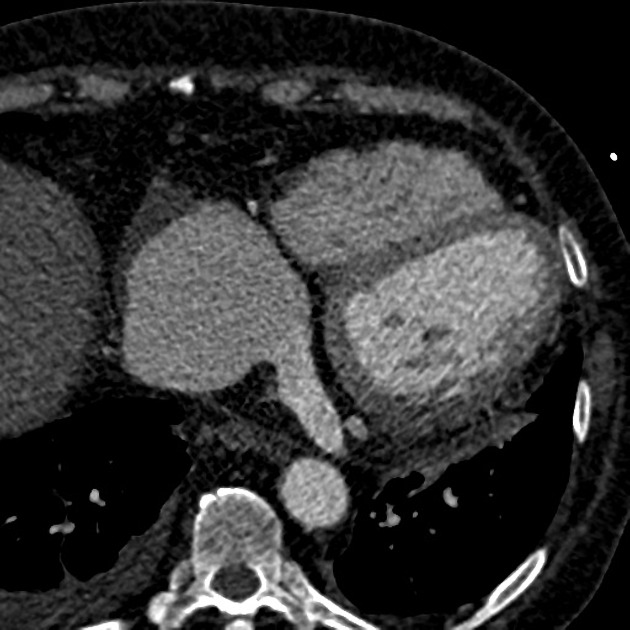
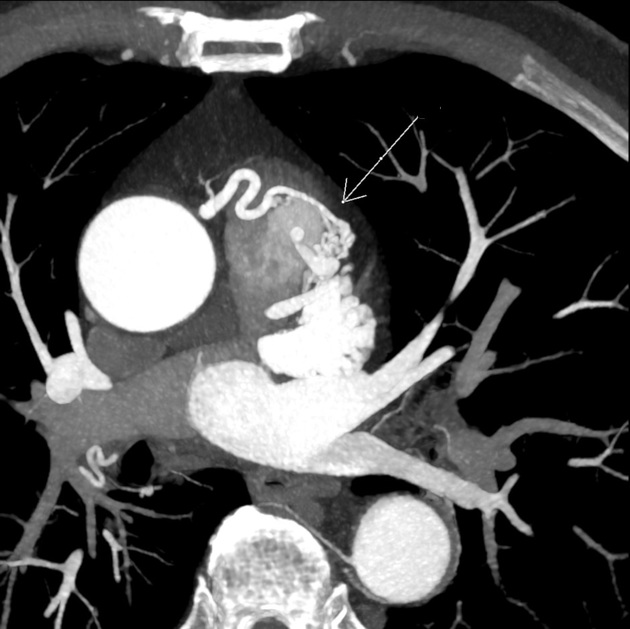
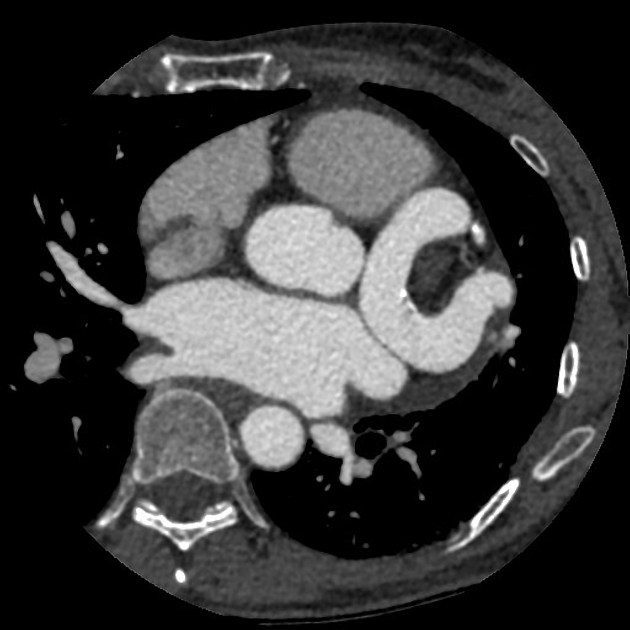
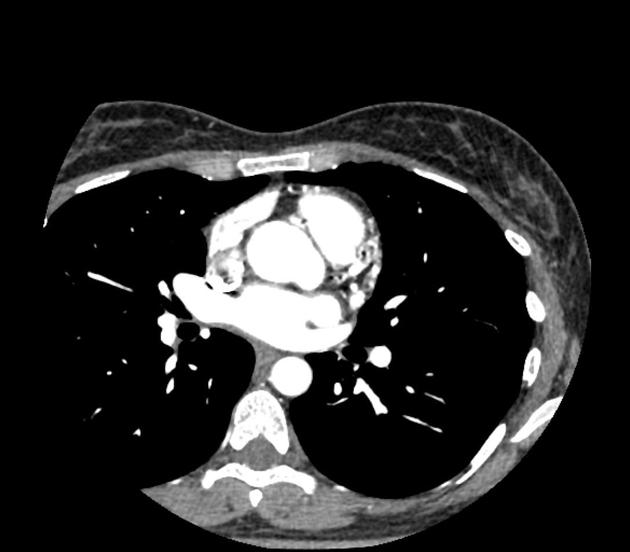
CT
Electrocardiographically-gated CT is able to not only detect the same characteristics of CAVFs as demonstrated by coronary artery angiography, but also has the additional benefit of being easily accessible and non-invasive 3,7. Thus, CT is increasingly considered to be the ideal imaging modality for evaluating CAVFs instead of angiography 3,7.
Treatment and prognosis
Although there have been reports of spontaneous closure of the fistula due to thrombus, generally symptomatic patients require closure via either transcatheter embolization or surgical ligation 4. Patients with known CAVFs should also receive prophylactic anti-platelet therapy and antibiotic prophylaxis against bacterial infective endocarditis 4.
Patients who have undergone a closure procedure tend to have an excellent prognosis 4.




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.