Dural arteriovenous fistulas (dAVF) are a heterogeneous collection of conditions that share arteriovenous shunts from dural vessels. They present variably with hemorrhage or venous hypertension and can be challenging to treat.
On this page:
Epidemiology
Most dural arteriovenous fistulas present in adulthood and account for 10-15% of all cerebral vascular malformations 6.
Associations
Clinical presentation
Clinical presentation is highly variable and depends on the location of the supplying and draining vessels, as well as the presence of complications (see below). Presentations include 4:
pulsatile tinnitus
cranial nerve palsies
seizures
orbital symptoms (see caroticocavernous fistula)
-
symptoms of venous hypertension
raised intracranial pressure
focal neurological deficits
Pathology
Dural arteriovenous fistulas are usually acquired and in most instances are idiopathic 6. In patients with a documented antecedent cause, most occur as a result of neovascularization induced by a previously thrombosed dural venous sinus (typically the transverse sinus). Other causes include trauma and previous craniotomy. It is likely that at least some patients with apparently idiopathic fistulae had prior asymptomatic thrombosis, particularly as inherited prothrombotic conditions (e.g. antithrombin, protein C, and protein S deficiencies) have been associated with the development of dural arteriovenous fistulas 6.
Typically, they are supplied by multiple feeders from arteries that supply the relevant part of the meninges and regional scalp vessels that often give transosseous branches:
-
supratentorial and lateral: (external carotid artery)
superficial temporal artery (transosseous branches)
-
anterior cranial fossa: (internal carotid artery)
ethmoidal branches of the ophthalmic artery
-
cavernous sinus: (internal and external carotid arteries)
-
posterior cranial fossa: (vertebral and external carotid arteries)
vertebral arteries (both dural and muscular branches)
Location
-
most common
least likely to have retrograde leptomeningeal venous drainage
cavernous sinus (indirect caroticocavernous fistula)
other venous sinuses
-
typically only ICA supply due to meningeal supply of this region
frequently associated with retrograde leptomeningeal venous drainage
tentorium: frequently associated with retrograde leptomeningeal venous drainage
Classification
Two classification systems are most commonly used 6:
Both classifications revolve around the knowledge that venous drainage pattern correlates with increasingly aggressive neurological clinical course. The single most important feature for prognosis is the presence of retrograde leptomeningeal venous drainage (i.e. into the cortical veins or deep cerebral veins). The Borden classification is a simplified version of the Cognard system but loses granularity 5,6.
Radiographic features
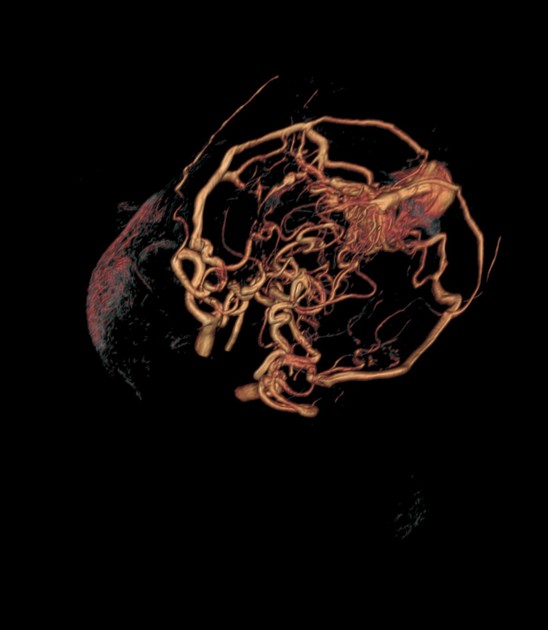
CT
Diagnosis can be difficult on non-contrast CT but should be thought of when an intracranial hemorrhage is in an unusual location or age group. With contrast, particularly with CT angiography, a diagnosis can often be made if care is taken. Findings that may be evident include:
abnormally enlarged and tortuous vessels in the subarachnoid space, corresponding to dilated cortical vein
an enlarged external carotid artery or enlarged transosseous vessels
abnormal dural venous sinuses including arterialization of contrast phase in the affected sinus due to arteriovenous shunting
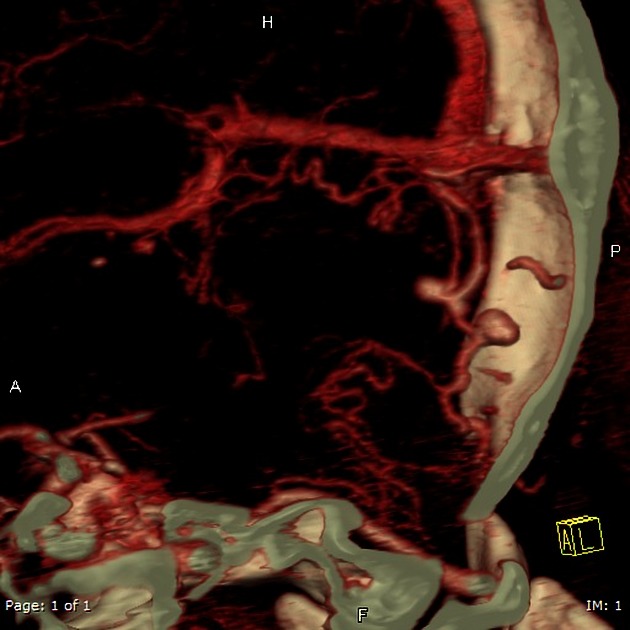
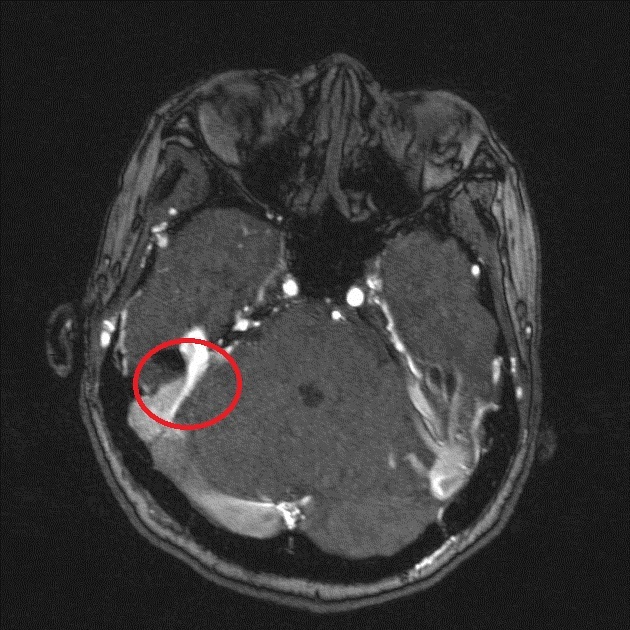
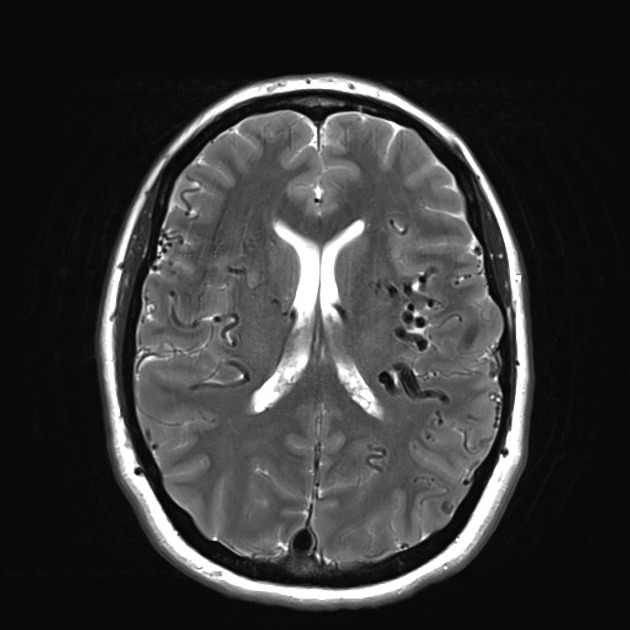
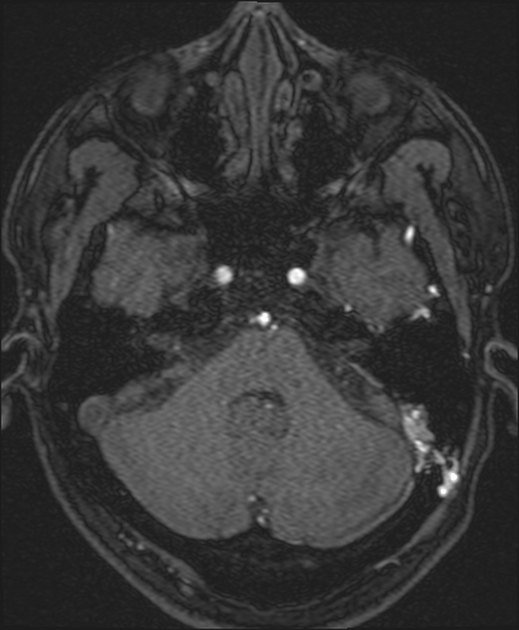
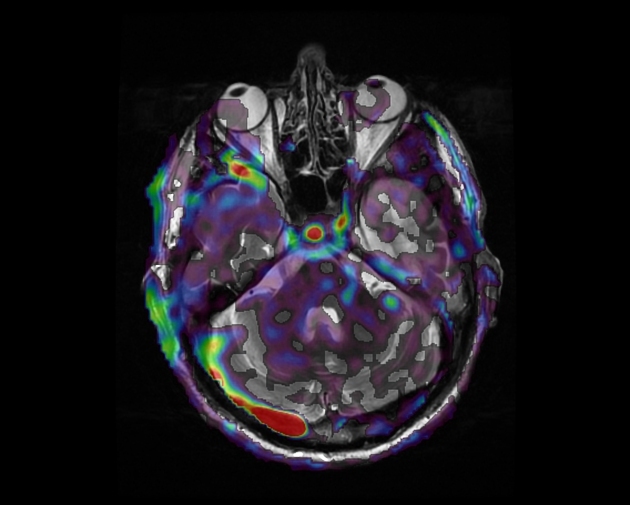
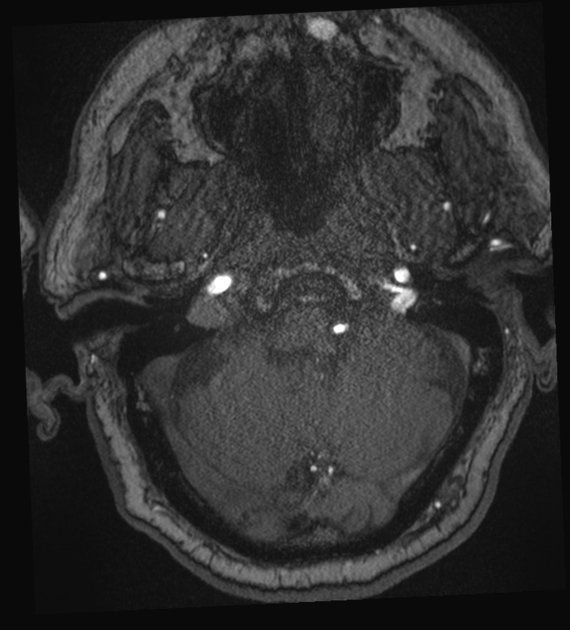
MRI
On routine non-vascular imaging, the diagnosis can be difficult in patients without retrograde leptomeningeal venous drainage although sometimes enlarged arterial feeders or dilated pial vessels in the subarachnoid space, best seen on T2 weighted imaging, can be a clue to the diagnosis.
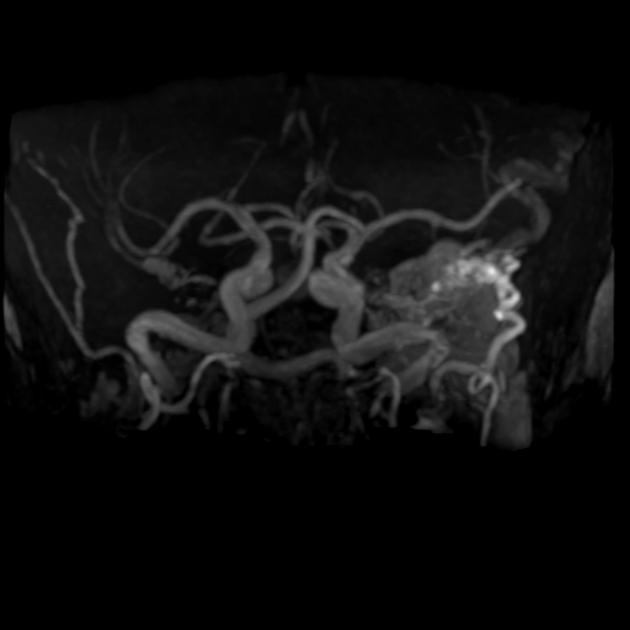
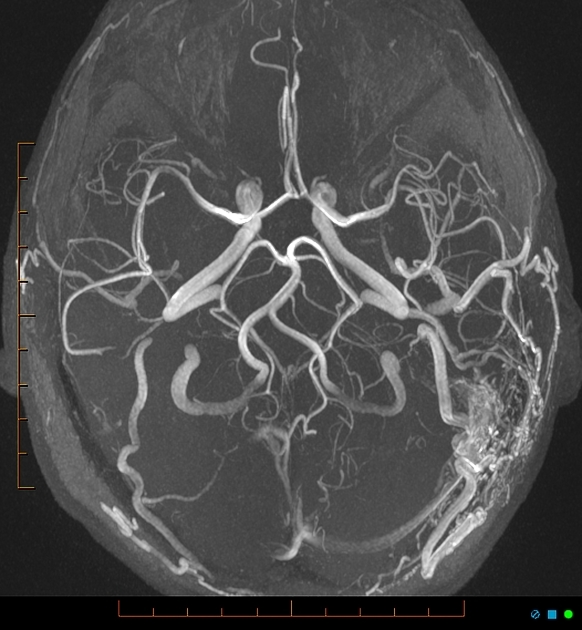
MR angiography is, however, fairly sensitive and specific with both time-of-flight angiography and time-resolved angiography to be able to imply or directly visualize arteriovenous shunting into dural sinuses or cortical veins and delineate enlarged feeding arteries 8,9.
When interpreting time-of-flight angiography, care must be taken, however, to avoid misinterpreting superiorly flowing venous blood as arterialized flow. This is particularly an issue in the left jugular bulb where retrograde (cranial) venous flow can ascend into the sigmoid sinus and inferior petrosal sinus mimicking arteriovenous shunting 10.
In patients with retrograde leptomeningeal venous drainage, edema is present in approximately half of the patients, although it may also be seen in patients who do not have retrograde leptomeningeal drainage on angiography 3. These regions of white matter edema may also enhance and are indicative of an aggressive fistula with a high rate of hemorrhage 3.
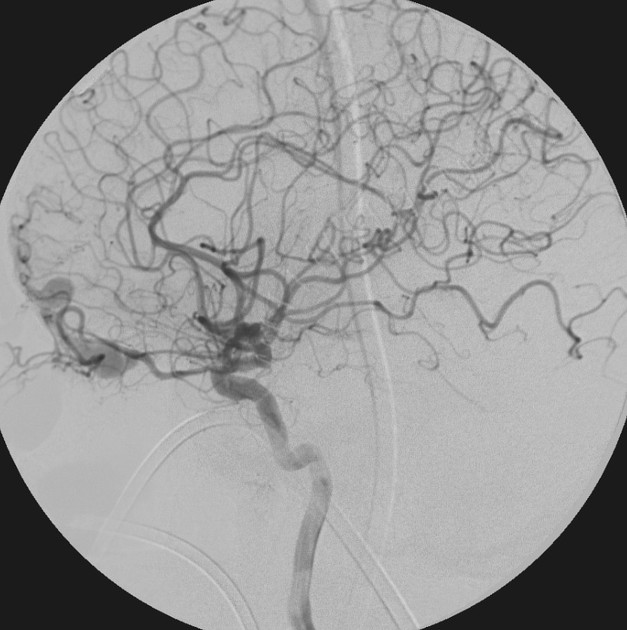
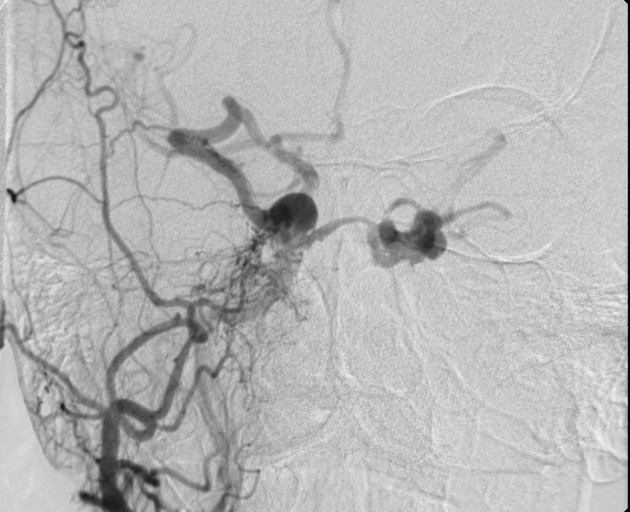
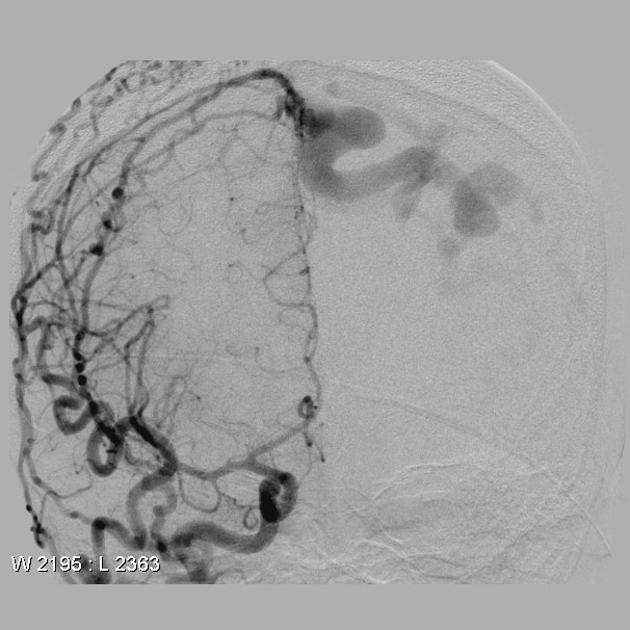
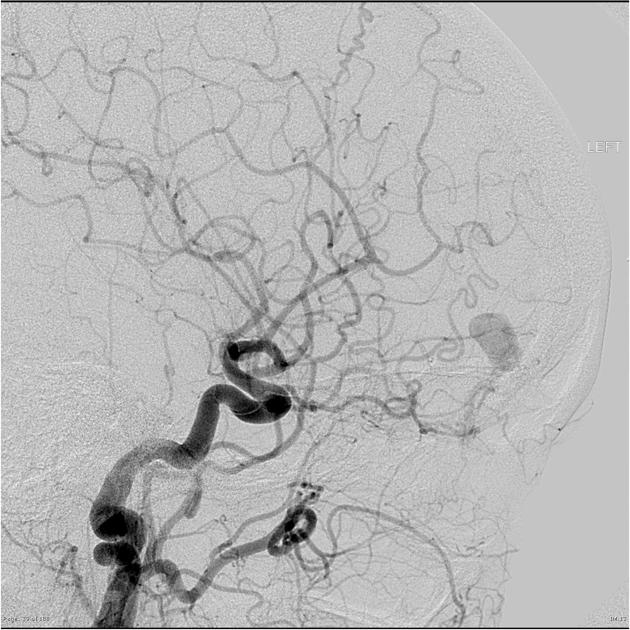
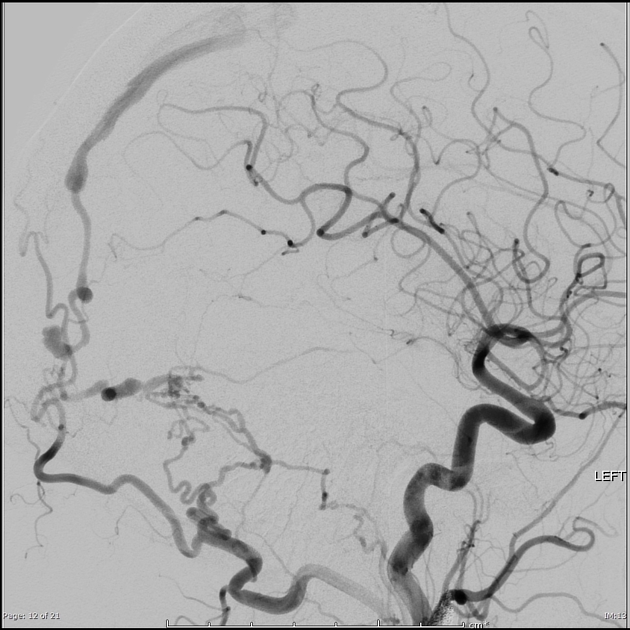
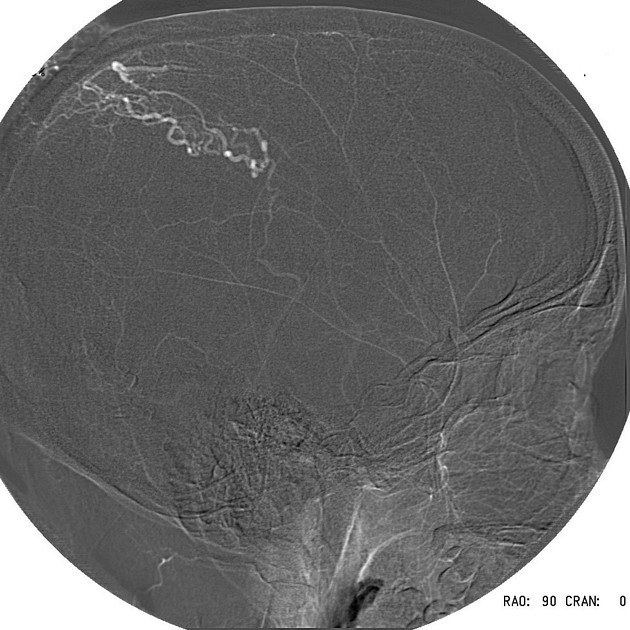
Angiography (DSA)
Catheter digital subtraction angiography demonstrates arteriovenous shunting most typically with multiple feeders and with no intervening nidus. DSA remains the gold standard in both diagnosis and accurate classification of dural arteriovenous fistulas, allowing not only systematic evaluation of feeding vessels (and thus planning for potential intervention), but also demonstrating the presence and extent of retrograde leptomeningeal venous drainage. Due to often extensive supply, a six vessel selective angiogram is required (bilateral ICA, ECA and vertebral artery injections).
Treatment and prognosis
Treatment largely depends on the classification of the fistula and the age and comorbidities of the patient, as well as the presence of symptoms directly attributable to the fistula.
conservative (especially Borden type I and Cognard types I and IIa)
-
higher grades (Borden types II and III, Cognard types IIb-V) have an annual mortality rate of ~10% and an annual risk of intracranial hemorrhage of ~8% 6, so treatment should be considered:
endovascular
surgical resection
stereotactic radiosurgery
Complications
The likelihood of complications depends on the venous drainage (reflected in both the Cognard and Borden classification systems), and not the arterial supply.
-
hemorrhage
-
venous congestion/hypertension and edema




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.