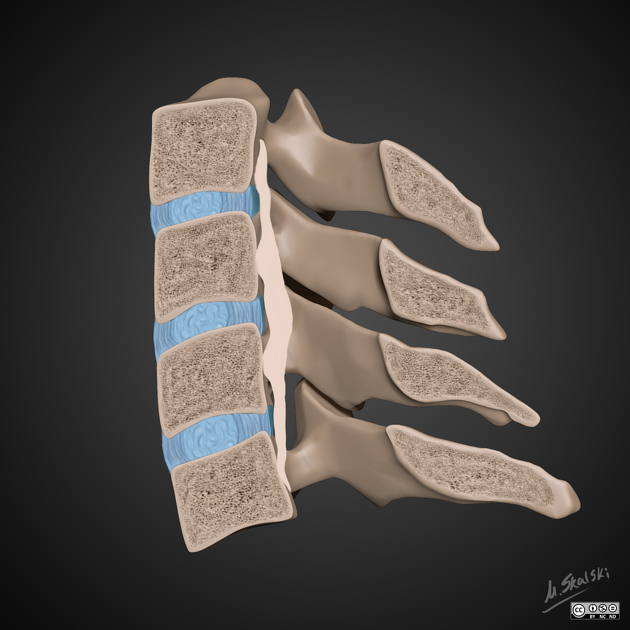
Ossification of the posterior longitudinal ligament (OPLL) refers to bone formation within the posterior longitudinal ligament of the spinal column.
On this page:
Epidemiology
There is a recognized greater prevalence in males and in the elderly 3. OPLL is twice as common in men compared with women.
The incidence is higher in East Asian populations (2.4%) compared to Caucasians (0.2-0.7%). The disorder is recognized as the leading cause of cervical myelopathy in Japan.
Associations
OPLL is often associated with several other entities:
DISH may be seen in up to 12% of elderly male Caucasians, with OPLL seen in about half of these, suggesting the incidence among Caucasians may be higher than the figures above.
Clinical presentation
Patients may be asymptomatic, or have evidence of radiculopathy and/or myelopathy 11. If present, symptoms usually manifest in the 4th-6th decades of life 7,8.
Pathology
The exact pathogenesis of OPLL is unclear 3.
Location
This typically seen in the mid cervical spine and results in central canal stenosis, predisposing the patient to cord injury from minor trauma:
cervical: 75%
thoracic: 15%
lumbar: 10%
Classification
The most commonly used classification is that proposed by the Investigation Committee for Ossification of the Spinal Ligaments, part of the Japanese Ministry of Health, Labor and Welfare 12,13:
continuous: a long lesion extending over several vertebral bodies
segmental: one or several separate lesions behind the vertebral bodies
mixed: a combination of continuous and segmental types
localized/focal/circumscribed: mainly located posterior to a disc space
Radiographic features
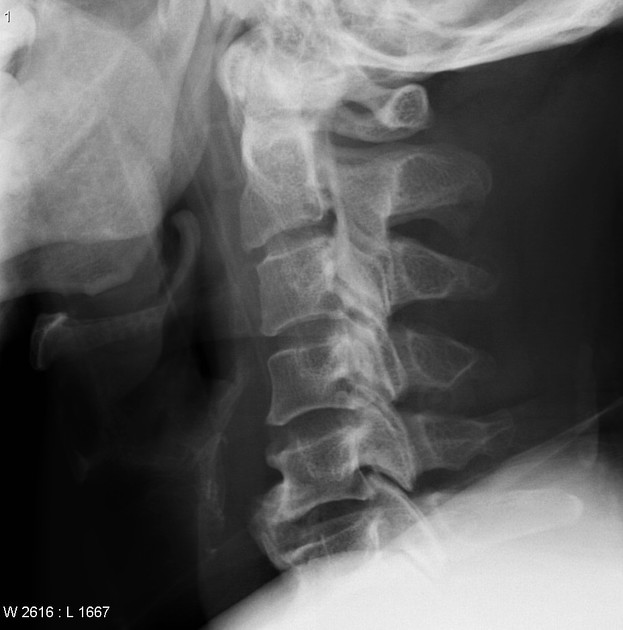
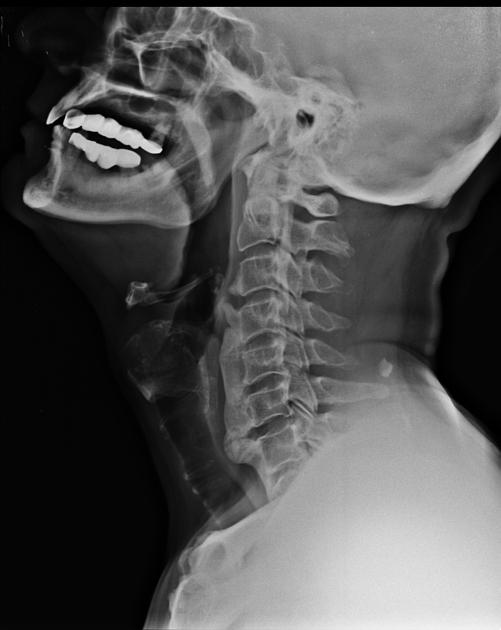
Plain radiograph
Continuous ossification of the posterior longitudinal ligament is visible as linear density posterior to the vertebral body cortex, within the ventral spinal canal.
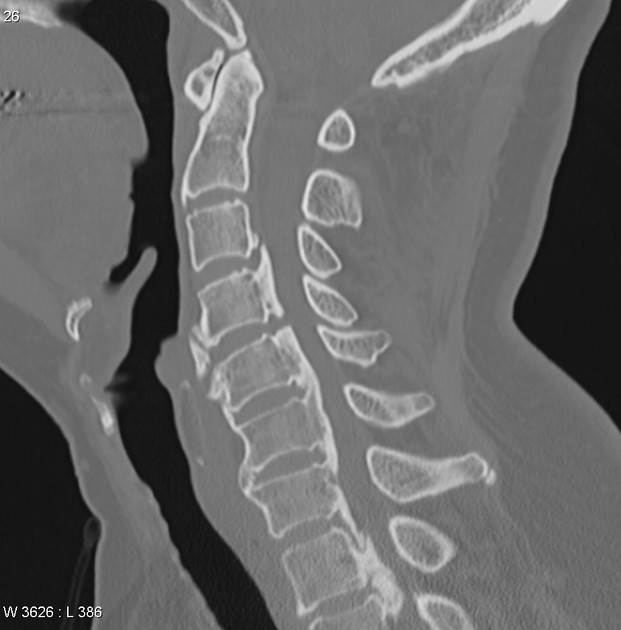
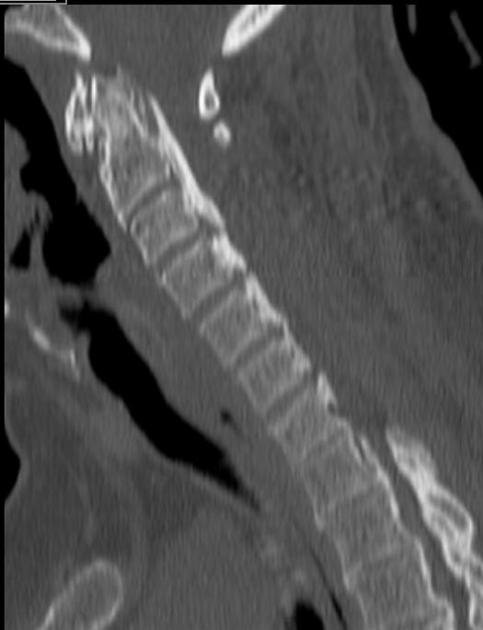
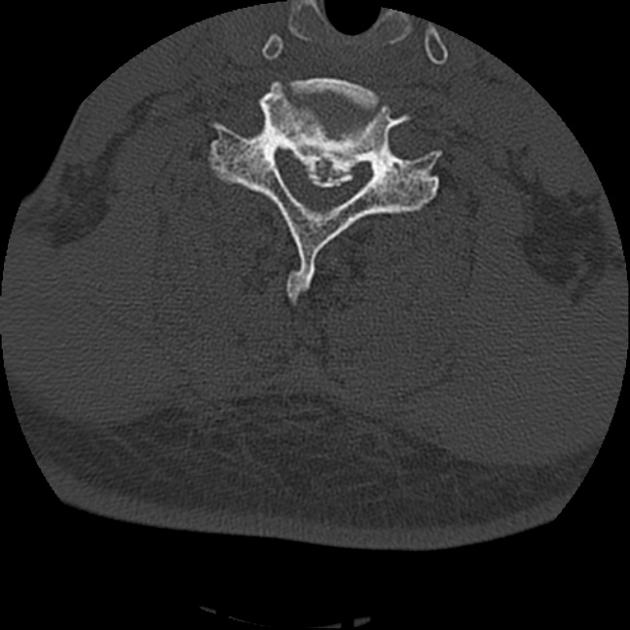
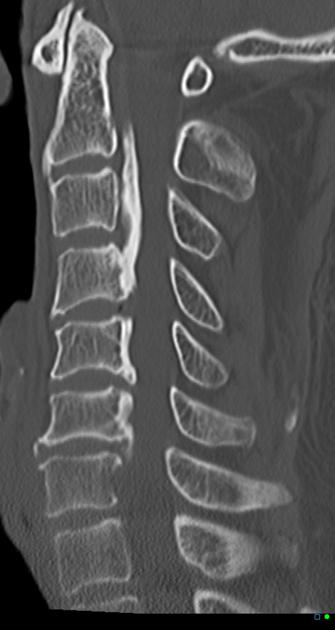
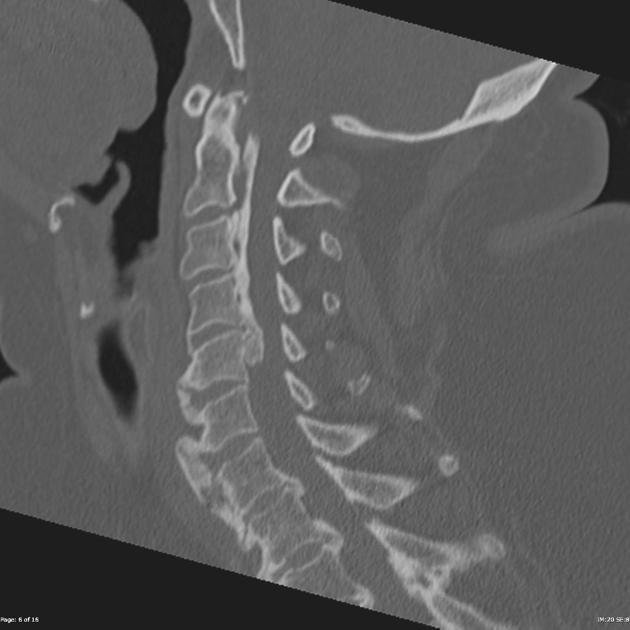
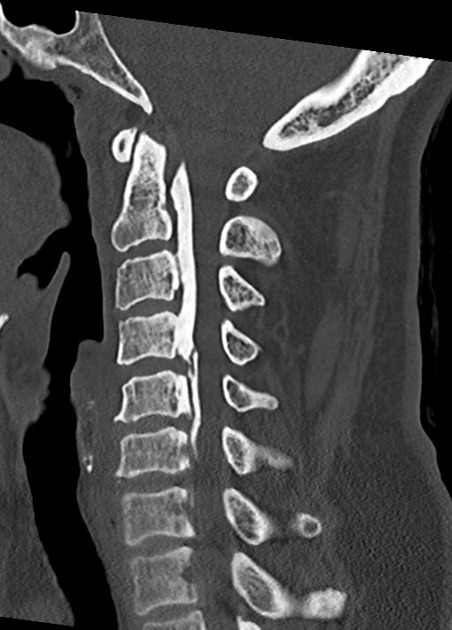
CT
CT is the best modality to depict ossification of the posterior longitudinal ligament and is often obtained for this purpose in cases of cervical spinal stenosis. Ossification can appear continuous (spanning multiple segments), segmental (discontinuous along vertebral bodies), and/or localized (spanning just the disc level). The ossification appears confluent with but often thicker and denser than cortical bone of the vertebral body.
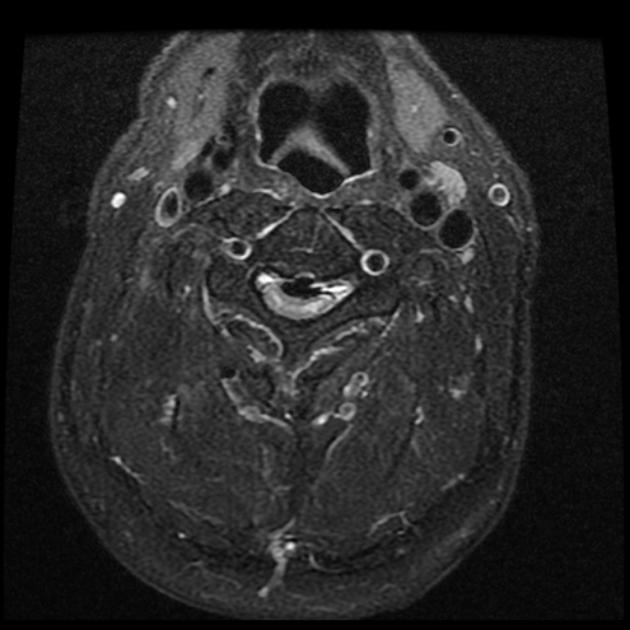
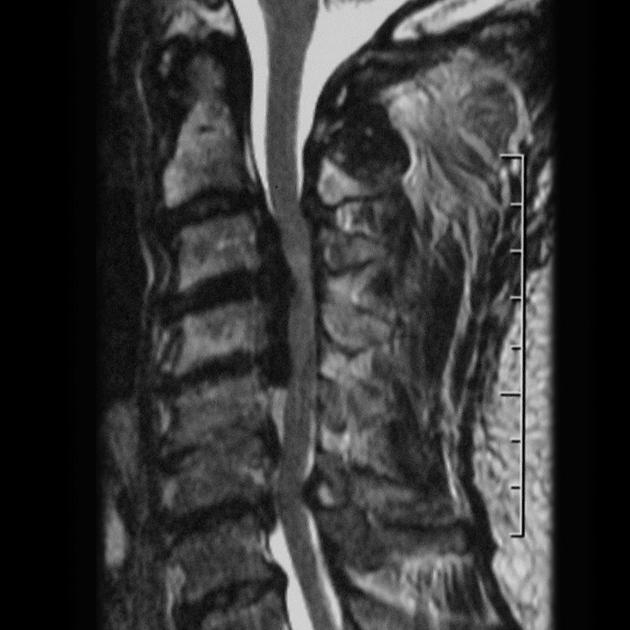
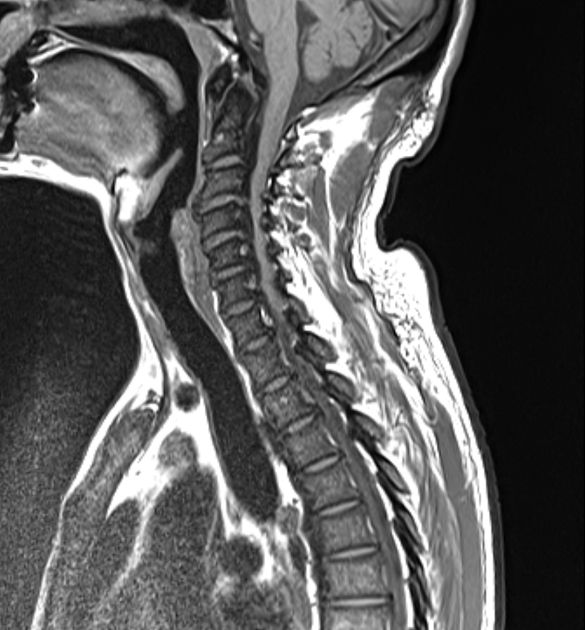
MRI
Ossification of the posterior longitudinal ligament appears hypointense on T1 and T2-weighted images. However, hypertrophy of the ligament without ossification can also have this appearance.
T2-weighted sequences are considered the most effective in the evaluation of spinal cord compression due to both the ossification and abnormal signal intensity of the spinal cord 5.
Treatment and prognosis
Management can range from conservative to surgical removal. Surgical options can include an anterior, posterior or combined approach. An anterior approach (e.g. plated multilevel anterior discectomy and fusion, anterior cervical corpectomy with fusion) may provide more direct decompression and best improve myelopathy, although may cause greater soft-tissue morbidity. Posterior approaches (e.g. laminectomy and fusion and laminoplasty) may be better tolerated in older patients 8.








 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.