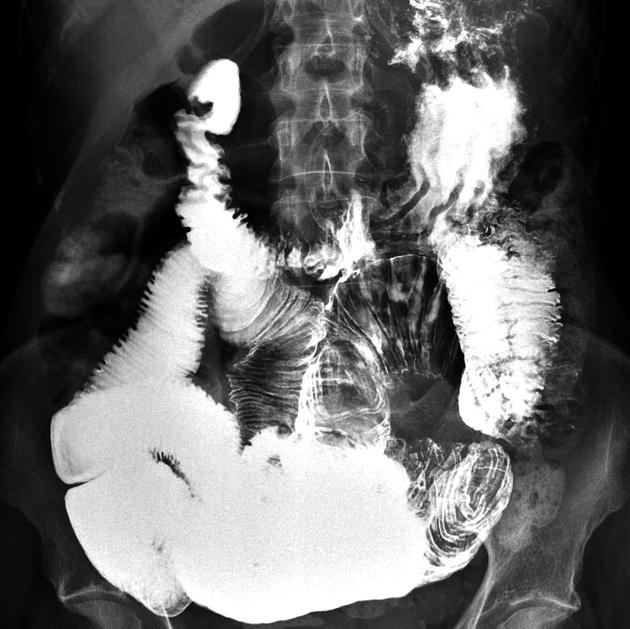
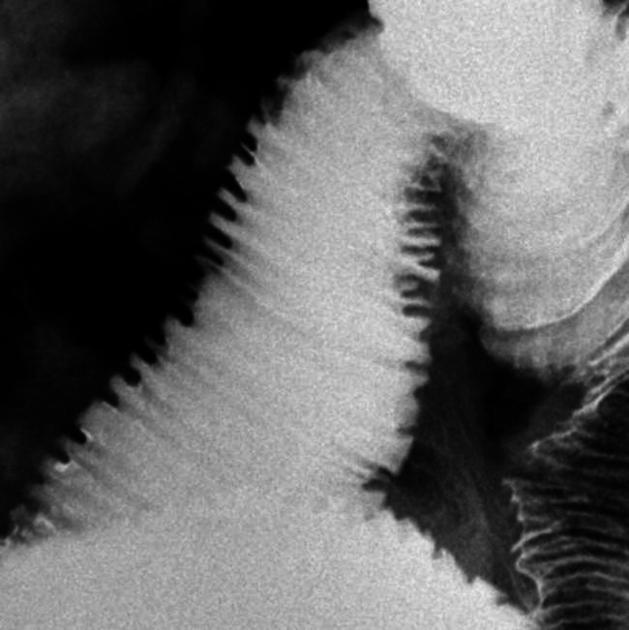
Small bowel follow-through is a fluoroscopic technique designed to obtain high-resolution images of the small bowel. The motility of the small bowel can also be grossly evaluated.
Indications
The small bowel follow-through can be useful for the evaluation of:
strictures
masses
extraluminal tethering
abnormal motility
Limitations of the small bowel follow-through include:
intermittent passage of contrast through the pylorus breaks up the contrast column
mild strictures and small masses may be difficult to see
The small bowel follow-through is inferior to enteroclysis for evaluation of small bowel pathology, but enteroclysis has drawbacks that prevent it from being more widely used (such as higher radiation dose and etc.).
Procedure
A small bowel follow through is a single contrast study (oral contrast, either barium or water-soluble contrast). It is often performed after an upper GI fluoroscopic study, as the contrast column moves from the stomach and duodenum into the small bowel. A small bowel follow through may also be performed by itself, without the upper GI investigation of the esophagus, stomach, and proximal duodenum, but this is less common.
Equipment
-
barium specially prepared for the small bowel (e.g. low density 30-50% weight/volume)
if concerned about a small bowel leak, water-soluble contrast should be used
high-density barium used for double-contrast upper GI studies is suboptimal for evaluation of distal small bowel loops
formulations including sorbitol are suboptimal for evaluation of small bowel detail 3
leaded apron and thyroid shield (unless you are using remote room technology)
palpation paddle and/or lead-lined glove
Technique
There are multiple different techniques that have evolved for performing a small bowel follow through. The following technique is one conventional approach.
patient starts fasting at midnight. Study is scheduled for the next morning
first, a single contrast upper GI is performed
after this, the patient drinks an additional 1-2 cups and waits outside the fluoroscopy suite
after 15-30 minutes, a spot radiograph of the abdomen is obtained and the patient is re-evaluated with fluoroscopy
-
spot radiograph with fluoroscopic re-evaluation is continued every 15-45 minutes until the enteric contrast reaches the terminal ileum and enters the ascending colon
patient is usually positioned during interval fluoroscopy for better evaluation of small bowel loops and paddle palpation is used to spread out bowel loops.
normal small bowel transit ranges between 30-120 minutes
Variations
If desired, the peroral pneumocolon technique may be attempted at the end of a small bowel follow through. The colon is insufflated with gas to try to reflux gas into the terminal ileum and allow double contrast images (gas and ingested oral contrast) of the terminal ileum.
Some practitioners use metoclopramide to increase small bowel motility and shorten the exam. The compromise is that evaluation of bowel distension and native bowel motility is decreased.
Some practitioners use a modified bowel preparation to try to clear the right colon.
Therapeutic
The administration of oral contrast is a common management strategy for patients presenting with small bowel obstruction. Whilst there is no clear evidence that oral contrast reduces the need for surgery, it has been shown to predict which patients can be managed conservatively and also reduces the length of admission.
The presence of oral contrast in the large bowel at 24 hours post-administration has been shown to predict the resolution of small bowel obstruction with 97% sensitivity and 96% specificity 4.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.