Theca lutein cysts, also known as hyperreactio luteinalis, are a type of functional ovarian cyst. They are typically multiple and seen bilaterally.
On this page:
Epidemiology
Associations
They have a very high association with gestational trophoblastic disease.
Other reported associations include:
diabetes mellitus
clomiphene intake
ovulation induction
-
rarely
pregnancy with background chronic renal failure 2
normal uncomplicated pregnancy 5
Pathology
They are thought to originate due to excessive amounts of circulating gonadotrophins such as beta-hCG. Hyperplasia of the theca interna cells is the predominant characteristic on histology. The ovarian parenchyma is often markedly edematous and frequently contains foci of luteinized stromal cells.
Radiographic features
The clinical context is vital in correct imaging interpretation.
General
The cysts are usually large (2-3 cm) and the ovaries often have a typical multilocular cystic appearance across all imaging techniques 4.
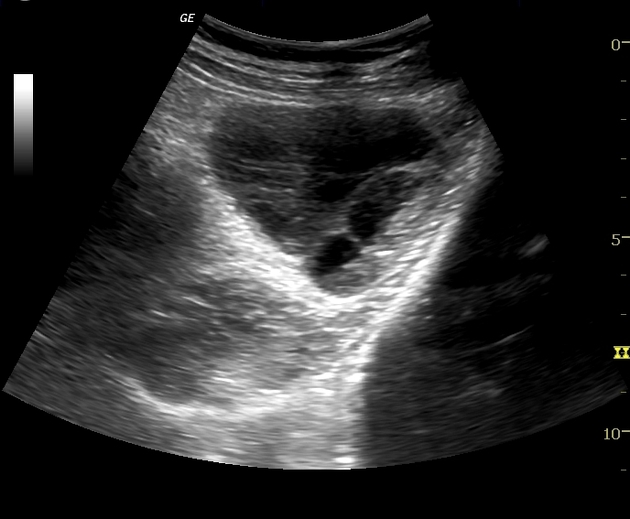
Ultrasound
Bilateral enlarged, multicystic ovaries. The cysts are classically thin walled and have clear contents. There is large amount of solid component which is possibly the residual ovarian stroma.
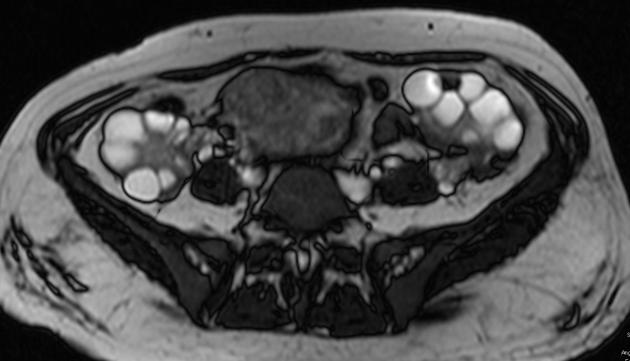
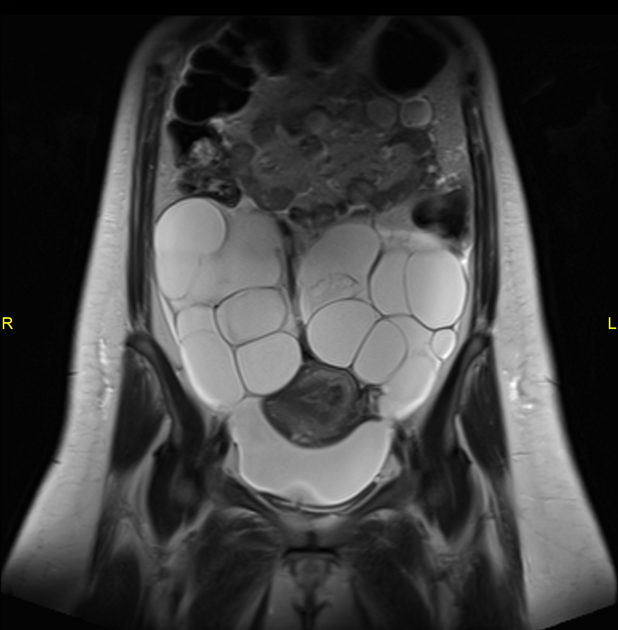
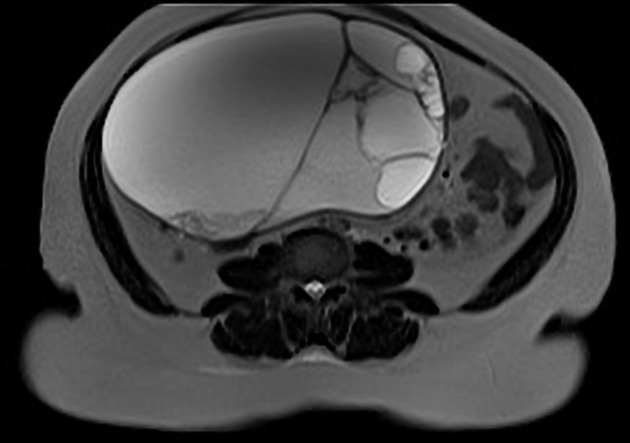
MRI
Typically seen as bilateral (occasionally unilateral) ovarian enlargement with multiple cysts which are generally of uniform size.
The residual parenchyma within the enlarged ovaries have been reported to show 6:
T1 C+ (Gd): intense contrast enhancement
T2: intermediate signal intensity
DWI: high signal
Treatment and prognosis
Following evacuation of a molar pregnancy, the associated theca lutein cysts resolve by 2-4 months.
There are reported cases of normal pregnancies associated with hyperreactio leutinalis that resolved gradually post delivery.
Surgical emergency is only if ovarian torsion occurs.
Differential diagnosis
For large multiple bilateral ovarian cysts consider:
-
ovarian hyperstimulation syndrome: can also be an association
often has a history of ovulation induction
may have free pelvic fluid
-
a more solid component may be present noted
ovarian tumor markers +/- beta HCG levels may be elevated ref





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.