Tracheobronchial amyloidosis refers to tracheal and/or bronchial involvement in amyloidosis. It is sometimes classified as a subtype of pulmonary amyloidosis.
On this page:
Epidemiology
It is a rare manifestation with some reports suggesting less than 100 published cases around the time of writing 5.
Clinical presentation
As opposed to those with a more distal disease, patients with involvement of the proximal tracheobronchial tree can have marked diseased air flow, air trapping, and fixed upper airway obstruction on pulmonary function tests.
Pathology
It can be primary or secondary. In the primary form, the disease is confined to the trachea and bronchial tree.
Radiographic features
Plain radiograph
Plain film findings are often non-specific, difficult and may even be normal in up to 25% of cases 2. There can be nodular and irregular narrowing of the tracheal lumen. Lobar or segmental collapse may be seen as a secondary feature due to endobronchial obstruction from amyloid deposition.
CT
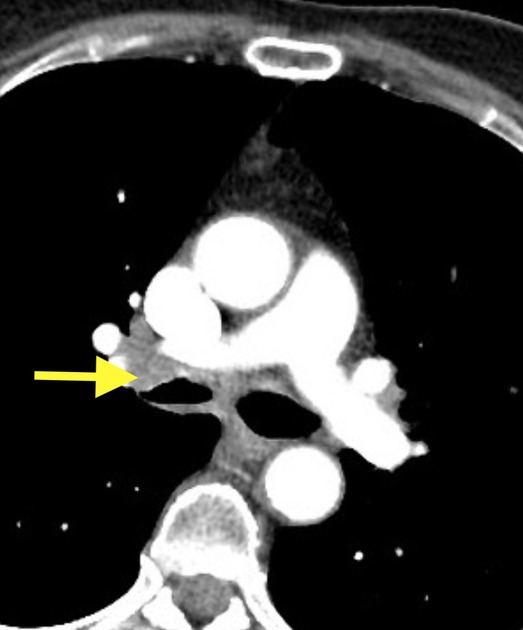
May show mucosal thickening +/- calcification involving segments of the trachea and bronchi. The affected portions of the airway can also be narrowed.
When it involves the trachea, the posterior membrane is also classically involved 2. CT is also considered to be useful in assessing the extra-luminal extent of disease 5.
The distribution of the disease may be either focal or diffuse 9.
Occasionally the disease may manifest as a raised, tumor-like mass of amyloid material (amyloid pseudotumor / amyloidoma).
Treatment and prognosis
The condition tends to have a progressive course where up to 30% of patients may not survive beyond 7-12 years post-diagnosis 5. The prognosis is thought to be worse with proximal or severe mid airways disease (as opposed to more distal pulmonary amyloidosis). Bronchoscopic debridement and laser treatments have sometimes been considered as therapeutic options but at the time of writing are not thought to prevent progressive airways narrowing 5. Local excision, however, may be temporarily effective 6. Other options have included radiation therapy (with occasional successful case reports 6-7).
Differential diagnosis
Tracheobronchial abnormalities that spare the posterior wall:
-
tracheobronchopathia osteochondroplastica
thickening is irregular and nodular
submucosal ossifications and calcifications can be seen extending from the tracheal cartilage rings
-
spares posterior membranous tracheal wall
more likely smooth, hyperdense mural thickening 8
patients usually have other clinical findings of cartilaginous inflammation 8
Tracheobronchial abnormalities that also involve the posterior wall:
-
granulomatosis with polyangiitis (GPA)
circumferential involvement
the subglottic trachea is the most commonly affected area (involvement down to the main bronchi is possible)
ulcerations of the trachea are possible
-
post-intubation tracheal stenosis
focal involvement
irregular and concentric stenosis




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.