Aortic valve stenosis is the most common valvulopathy and describes narrowing of the opening of the aortic valve between the aorta and the left ventricle.
On this page:
Epidemiology
Aortic stenosis is the most common valvulopathy, present in up to one-quarter of all patients with chronic valvular heart disease 1,2. The condition has a male predilection in a 4:1 ratio 1, and the incidence of degenerative aortic valve disease, the most common etiology of aortic stenosis, is increasing 1,2.
Clinical presentation
The classic triad of symptoms caused by aortic stenosis is angina pectoris, dyspnea, and syncope, however, any left-predominant clinical features of heart failure may be present 1,2. Generally, these symptoms do not become prominent until significant stenosis is present (<1 cm2) 1.
Clinical examination classically reveals a narrow pulse pressure, a slow-rising peripheral pulse, pulsus parvus et tardus (weak and delayed pulse) in the carotid pulse, a pressure-loaded ("heaving") apex beat, and a crescendo-decrescendo mid-systolic (or ejection systolic) murmur that is heard on precordial auscultation 1,2. The murmur associated with aortic stenosis also characteristically radiates to the carotid arteries, and may also radiate to the apex which can mimic the murmur of mitral valve regurgitation, known as the Gallavardin phenomenon 3.
Numerous clinical maneuvers can be used to distinguish aortic stenosis from the similar-sounding murmurs of hypertrophic obstructive cardiomyopathy and pulmonary valve stenosis, such as the Valsalva maneuver and auscultation during inspiration respectively 1.
Pathology
Aortic stenosis in adults is most commonly caused by degenerative calcification, especially in the setting of congenital aortic valve disease (most commonly a bicuspid aortic valve), chronic trileaflet deterioration, or previous rheumatic heart disease affecting the aortic valve 1,2. This degenerative calcification shares many similarities to the process of atherosclerosis, and many of the risk factors are the same, such as low HDL, diabetes mellitus, smoking, hypertension, chronic kidney disease, and metabolic syndrome 1,2.
The end-product of this atherosclerotic-like process is thickening of the valve leaflets (initially just "aortic sclerosis") due to activation of inflammatory cascades, endothelial dysfunction, and valvular lipid accumulation 1,2. Ultimately, the valvular myofibroblasts differentiate into osteoblasts resulting in calcium deposition on the valve ("calcific aortic stenosis") 1,2. This process progressively causes a reduction in aortic valve area, resulting in progressive stenosis 1,2.
This stenosis causes a left ventricular outflow tract (LVOT) obstruction. The turbulent blood flow from this LVOT obstruction explains the timing of the murmur and the various peripheral signs associated with aortic stenosis 1,2. Moreover, this LVOT obstruction causes a systolic gradient to form between the aorta and left ventricle 1,2. This gradient may progressively increase without any significant changes to left ventricular function because of compensatory left ventricular hypertrophy, appreciated clinically by the pressure-loaded apex beat 1,2.
However, this adaptive mechanism eventually fails and systolic and diastolic function declines and irreversible myocardial fibrosis develops. It is at this point that patients manifest clinical features of heart failure 1,2.
Etiology
There are numerous other predisposing factors and causes of aortic stenosis. These can be classified by their anatomical position (supravalvular vs valvular vs subvalvular) and whether they are congenital or acquired etiologies 1,2,4. Of note, supravalvular and subvalvular aortic stenosis often do not have the same degenerative pathogenesis as valvular aortic stenosis 1.
-
supravalvular
congenital: isolated or in syndromic association (e.g. Williams syndrome)
acquired: post-surgical or sequela of aortitis (e.g. syphilitic aortitis, Takayasu arteritis, etc.)
-
valvular
-
congenital (congenital aortic valve stenosis): the most frequent cause of aortic valve stenosis age in patients between 15 and 65 of age and often arises in associated with anomalous valves
bicuspid aortic valve: deformed aortic valves with two functional leaflets or cusps which are often unequal in size (60%); a calcified bicuspid aortic valve is considered the most frequent form of adult aortic valve stenosis
tricuspid aortic valve: aortic valves with three functional leaflets or cusps which are often unequal in size (30%)
unicommissural/unicuspid aortic valve: dome-like aortic valve with stenosis at a very young age (10%)
quadricuspid aortic valve (rare): generally predisposes to aortic valve regurgitation instead of aortic stenosis
-
acquired
rheumatic heart disease: rarely isolated aortic valve stenosis, thickened, shortened cusps, fused commissures, occurs always with aortic regurgitation
senile calcific aortic stenosis/degenerative aortic stenosis: as discussed above
radiation-induced heart disease: generally a decade or more after exposure to mediastinal radiotherapy
-
-
subvalvular
-
congenital
hypertrophic subaortic stenosis associated with hypertrophic obstructive cardiomyopathy, generally not considered true aortic stenosis
-
Radiographic features
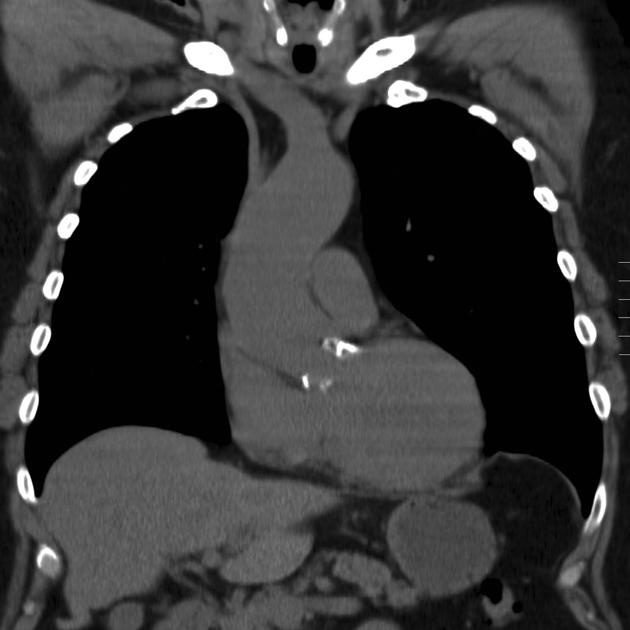
Plain radiograph
The appearance on chest radiograph is variable depending on the stage and severity of the disease 2,5.
In early disease, the chest radiograph can be entirely normal or it may show dilatation of the ascending aorta with normal heart size. Differentiation with hypertension can usually be made as in hypertension the entire descending aorta is enlarged 2,5.
However, late in the disease, the chest radiograph may reveal valvular calcifications (if valvular aortic stenosis) and/or cardiomegaly with features of heart failure, such as pulmonary venous congestion and pulmonary interstitial/alveolar edema 2,5. At this stage, especially in the absence of valvular calcifications, it is not possible to differentiate aortic stenosis from other causes of heart failure 2,5.
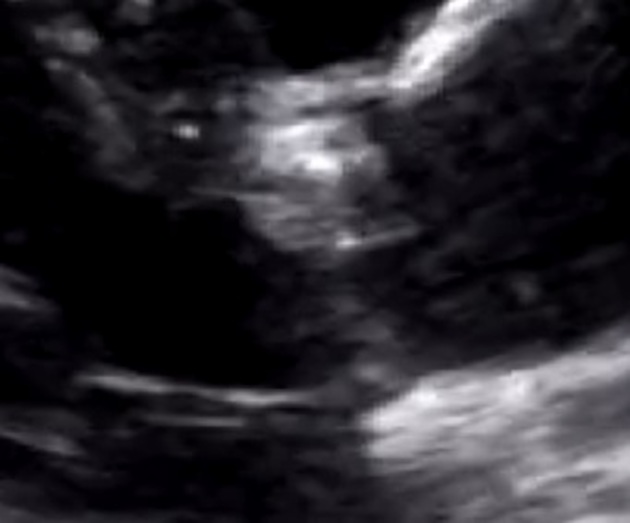
Ultrasound
Echocardiography
Echocardiography is useful for evaluating the anatomical location of the stenosis, either supravalvular, valvular, or subvalvular, for assessing the aortic valve area and jet velocity, and for assessing the left ventricle. Various parameters are used in order to determine severity, such as 2,6:
-
aortic sclerosis
aortic jet velocity ≤2.5 m/s
-
mild aortic stenosis
aortic jet velocity 2.6-2.9 m/s
mean gradient is <20 mmHg
aortic valve area (AVA) >1.5 cm2
aortic valve area indexed to body surface area (AVA/BSA) >0.85 cm2/m2
-
moderate aortic stenosis
aortic jet velocity 3.0-4.0 m/s
mean gradient 20-40 mmHg
AVA 1.0-1.5 cm2
AVA/BSA 0.60-0.85 cm2/m2
-
severe aortic stenosis
aortic jet velocity >4 m/s
mean gradient >40 mmHg
AVA <1 cm2
AVA/BSA <0.60 cm2/m2
In cases where there is a low AVA and also a low mean gradient, this may either indicate true severe aortic stenosis or pseudo-severe aortic stenosis due to low cardiac output 6. In these cases, low-dose dobutamine may be given to differentiate between these two entities 6.
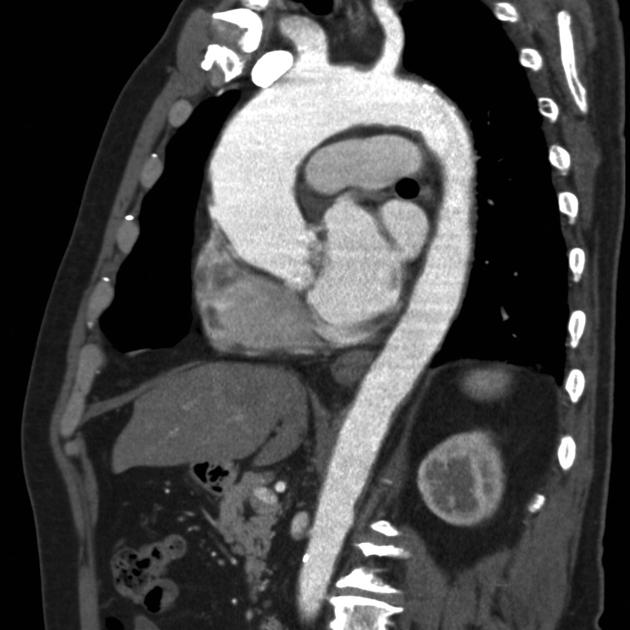
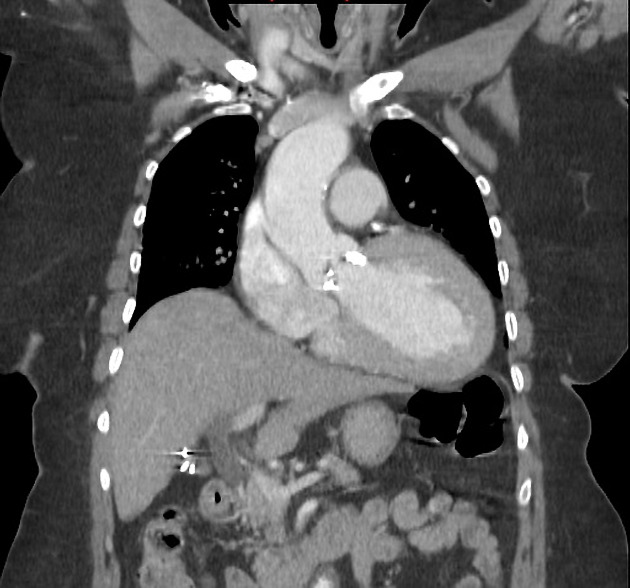
CT
Cardiac CT confirms, with greater detail, findings on plain radiograph 7-10. Moreover, it is able to determine an aortic valve calcification score, whereby a high aortic valve calcification score may indicate severe aortic stenosis, particularly in patients with non-rheumatic acquired calcific aortic stenosis 7-10.
Post-stenotic dilatation of the ascending aorta may be present 11.
MRI
Cardiac MRI (CMR) is able to provide a more detailed structural and dynamic assessment of the aortic valve and left ventricle, in particular 5,7:
-
structural assessment on spin-echo MR sequence
post stenotic dilatation of ascending aorta
symmetrical left ventricular hypertrophy wall thickness (≥12 mm)
increased LV mass
-
dynamic assessment on cine GRE or b-SSEP
thickened valve leaflets with reduced excursion during systole
size and extent of the high-velocity jet into the ascending aorta
hyperdynamic LV contraction in compensated state
Treatment and prognosis
The decision to treat aortic stenosis is based on the severity 1,2. Management involves a combination of lifestyle and pharmacotherapy measures (a similar armamentarium to that used in heart failure), balloon valvuloplasty, and aortic valve replacement 1,2.
Aortic valve replacement can be in the form of:
transcatheter aortic valve implantation (TAVI): percutaneously inserted valve that is deployed within the stenotic native valve, useful in frailer patients but long-term resilience unclear at this stage
conventional aortic valve replacement: involves midline sternotomy, cardiopulmonary bypass, and replacement with a metal or bioprosthetic valve, still the treatment of choice in younger patients
Complications
sudden cardiac death from arrhythmia
See also
-
general aortic valve pathologies:
aortic valve stenosis (and aortic valve sclerosis)
-
specific aortic valve pathologies:





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.