CT myelography (CTM) is a myelography technique used mainly to assess for potential spinal canal stenosis when MRI is contraindicated or when dynamic imaging is required.
On this page:
Images:
History
CT myelography was first performed in 1976 2 and became the gold standard for imaging the spinal canal and cord until the advent of MRI which has, largely, replaced it. However, ever-increasing CT resolution and the development of dynamic CT myelographic techniques have seen it gain importance in a select group of conditions and remain a viable alternative for patients who cannot have an MRI 1.
Indications
Common indications of CT myelography are many common conditions (e.g. spinal canal stenosis) that would normally be imaged with MRI in patients who for some reason cannot have an MRI.
Typically a conventional (non-dynamic) CT myelogram is performed in this instance (see below).
Additionally, dynamic CT myelography has become an important examination in a variety of conditions even when MRI is available. These include 1:
intrathecal cysts, e.g. spinal arachnoid cyst, spinal neurenteric cyst
-
identifying the cause of spontaneous intracranial hypotension
spinal CSF leaks (meningeal diverticula, dural tears, nerve root sleeve leaks)
arachnoiditis 1,4,5
Contraindications
In addition to general contraindications for lumbar puncture, iodinated contrast media allergy may be a relative or absolute contraindication depending on severity 5.
Procedure
Pre-procedural evaluation
As well as those for a lumbar puncture, specific to myelography include:
some authors 5,6 recommend that medications that lower the seizure threshold (e.g. some antidepressants, antipsychotics, antinausea, and pain medications) should be considered to be witheld for 24-48 hours prior in consultation with the prescribing doctor
prior imaging for anatomy, prior surgery, suspected spinal stenosis, etc. 5
Technique
Technique will depend on whether a conventional (non-dynamic) or dynamic CT myelogram is being performed.
In both instances, a water-soluble non-ionic iodinated contrast should be used for CT myelography to a maximum dose of 3 g iodine to avoid neurotoxicity 4,5. Spontaneous CSF flow in the needle hub should be observed prior to contrast instillation 6. CSF opening pressure and CSF collection can also be performed at the time of thecal puncture 4,5.
Conventional CT myelography
Initially, iodinated contrast is instilled into the thecal sac most commonly via a lumbar puncture, although a C1-2 puncture can be performed 5. The lumbar puncture may initially be via fluoroscopy and the patient then transported to CT, however, the use of CT fluoroscopy for a CT-guided lumbar puncture is becoming more common.
The volume and concentration of contrast media is variably described 5,9:
cervical CT myelography: 10 mL of 300 mg iodine/mL
whole spine CT myelography: 15-17 mL of 240 mg iodine/mL
lumbar spine myelography: 15-17 mL of 180 mg iodine/mL or 10 mL of 300 mg iodine/mL 5,9
The patient should be rolled several times prior to CT image acquisition and high resolution thin slice (0.5-0.625 mm) image acquisition is recommended 4,5. A review on table is important to ensure adequate contrast mixing in the CSF has been achieved.
Delayed images may be required if a slow-flow CSF leak is suspected 4.
Dynamic CT myelography
Dynamic CT myelography is primarily utilized to visualize CSF leaks or CSF-venous fistulas and its aim is to visualize dense contrast as it first exists the thecal sac.
The positioning of the patient will depend on the likely source of CSF leak as determined by previously performed MRI (see spontaneous intracranial hypotension).
When CSF epidural collection is ventral or ventral and dorsal, then a ventral dural defect (e.g. from a calcified thoracic disc) is most likley and thus the patient should be positioned prone 7.
If CSF pooling was seen laterally or along the nerve roots, then the patient should be positioned in a lateral decubitus with the side of the CSF collection down.
If no CSF pooling or leak was identified on MRI of the spine, but clinical symptoms and MRI of the brain are consistent with spontaneous intracranial hypotension then a CSF-venous fistula is likely. The ideal technique in this scenario remains to be fully described 8. Alternatives include: prone dynamic CT myelogram and, if negative, followed by immediate roll into lateral decubitus (allowing contrast to pool dependently); lateral decubitus dynamic CT myelogram with roll into the opposite lateral decubitus; separate injections, one for each side.
In all cases the patient should be slightly head down (Trendelenburg position) to approximately 15-20° 7. This is achieved by using a foam wedge(s) 7.
How much contrast is injected and in how many doses is an area of active research with the aim being to maximize diagnostic yield while reducing radiation dose as much as possible.
Some protocols require multiple sequential acquisitions, potentially of the entire spine, during continuous injection of contrast (13 mL, non-ionic contrast 300 mg iodine/mL) 10. Other protocols try to limit dose by using smaller volume of contrast injection with review of the initial scan and additional scans performed if required 7.
Additionally, the use of intrathecal bolous tracking can help in correctly timing the first acquisition 12.
Complications
lumbar puncture-related, e.g. bleeding, infection, post lumbar puncture headache
iodinated contrast media allergy: appears to be rare 6
seizures: appears to be rare 6
spinal cord or conus medullaris injection 6
vasogenic cerebral edema 11



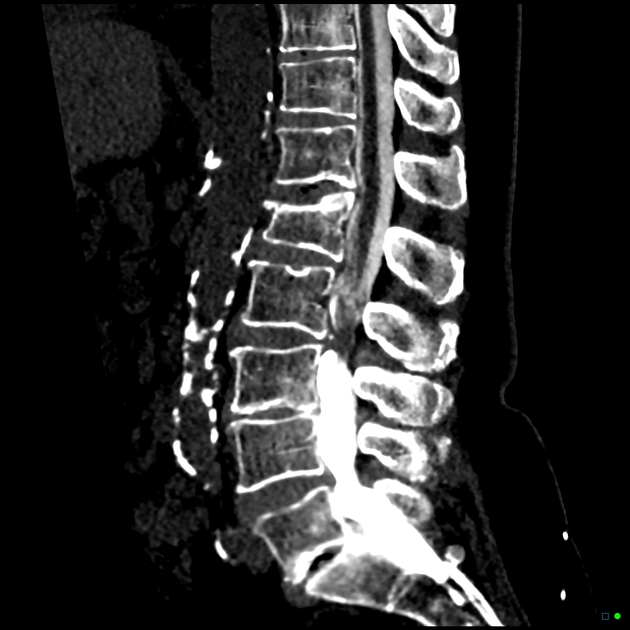
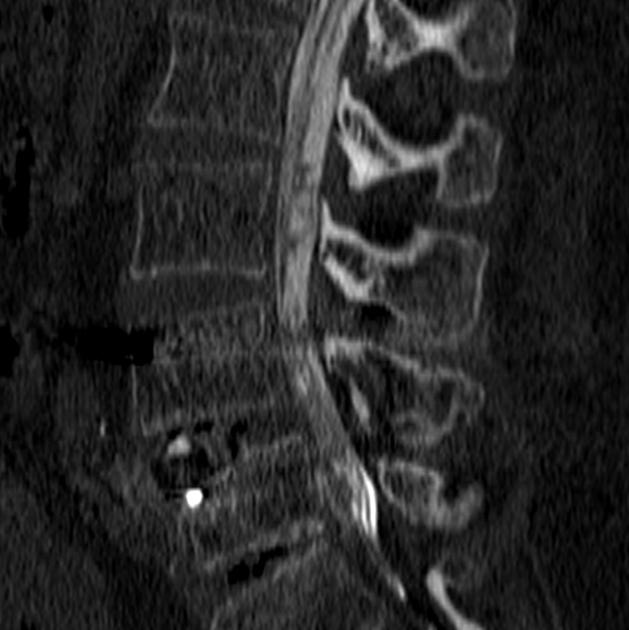
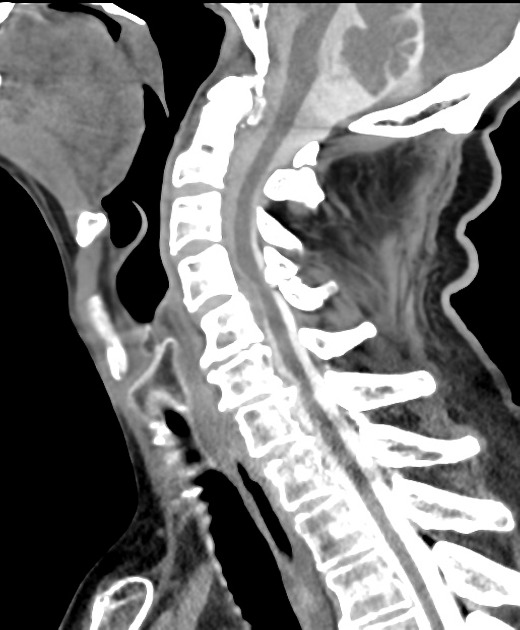
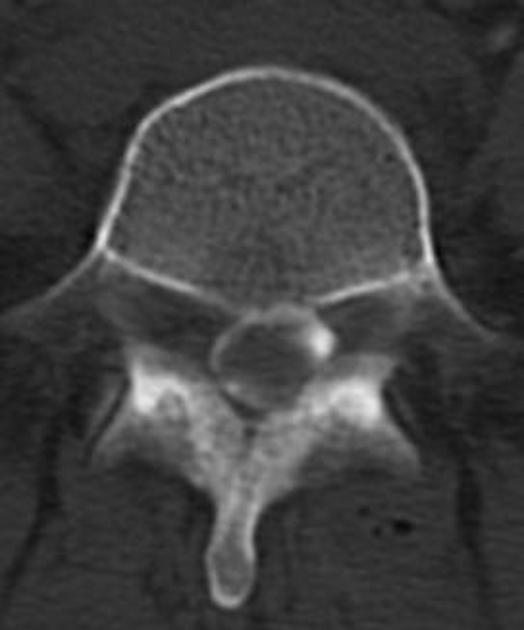


 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.