Hepatopulmonary syndrome (HPS) is a clinical syndrome defined by the presence of the following:
liver disease
-
dilation of pulmonary vasculature
may involve pulmonary capillaries, pulmonary arteriovenous malformations (AVMs), or pleural arteriovenous malformations
-
abnormalities in oxygenation
elevation in the alveolar-arterial (A-a) oxygen gradient with or without hypoxemia on room air
On this page:
Epidemiology
It is estimated to be present in ~15% of adults with liver cirrhosis.
Clinical presentation
Patients will classically present with varying degrees of positional dyspnea, alleviated by recumbency and aggravated by assuming a seated position. Patients may bear the stigmata of concomitant liver disease, most commonly with a component of portal hypertension. The presence of severe hypoxemia with a measured partial pressure of arterial oxygen under 60 mmHg is particularly suggestive, as are spider nevi, clubbing of the digits, and cyanosis.
Examination may also reveal:
hepatosplenomegaly
ascites, pedal edema
-
hyperdynamic circulation
with an elevated cardiac output, decreased systemic vascular resistance, wide pulse pressure
-
hypoxemia
-
more profound when assuming a seated position
with similarly positional dyspnea constitutes the platypnea-orthodeoxia syndrome
may be absent due to compensation in mild disease, necessitating measurement of an A-a gradient
-
Pathology
The characteristic vascular anomalies are attributed to a variety of mechanisms, including disregulation of pulmonary angiogenesis, an increase in pulmonary nitric oxide formation, and endothelial dysfunction.
Radiographic features
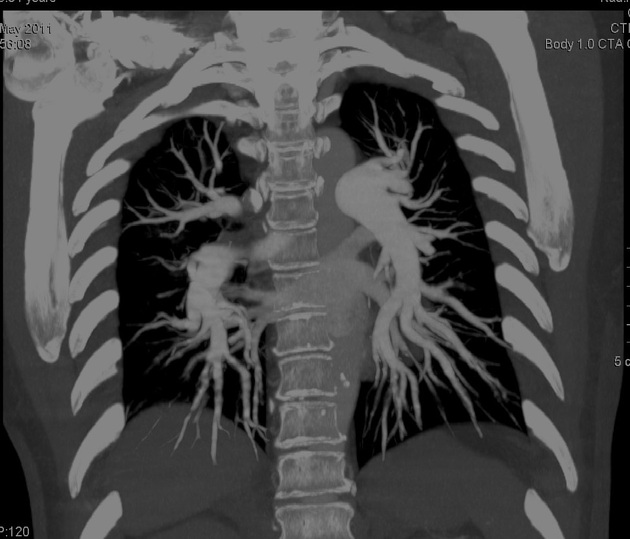
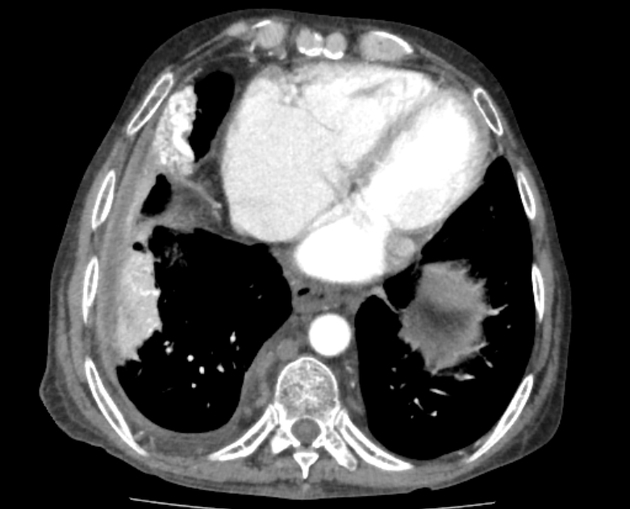
The radiologic manifestations of this disease include distal vascular dilatation associated with an abnormally large number of visible terminal vessel branches, which are always concentrated in the lower lung zones.
Plain radiograph
Chest x-ray may include bibasal medium-sized (1.5-3 mm) nodular or reticulonodular opacities 2,4.
CT
May show peripheral arteriolar dilatation on CT with an increased number of terminal branches extending towards the pleura.
Two patterns have been described on CTPA 6:
-
type I
most common (~85%)
manifests as distal vascular dilatation with subpleural telangiectasia
features include multiple, slightly dilated subpleural vessels that do not taper normally and therefore extend to the pleural surface
-
type II
less common (~15%)
seen as individual arteriovenous malformations on angiograms and nodular dilatation of peripheral pulmonary vessels
Ultrasound
Echocardiography
Contrast-enhanced transthoracic echocardiography using agitated saline is a sensitive means of diagnosis, and will demonstrate passage of microbubbles into the left atrium within 3-6 cardiac cycles from opacification of the right atrium. The anatomic location of shunting will remain occult with this method 8. Transesophageal (TEE) studies may be more sensitive and allow direct visualization of microbubble influx in the left atrium from the pulmonary veins. The presence of esophageal varices, which have a high incidence in this population, warrant caution if transesophageal echocardiography is to be performed 9.
Nuclear medicine
A Tc-99m MAA (micro-aggregated albumin) lung scan is a useful method to detect intrapulmonary vascular dilatation. A scan showing uptake of radionuclide over the kidneys, brain, or both, suggests shunting through the lung caused by an intrapulmonary shunt. The perfusion lung scan is a simple, safe, non-invasive and effective method to evaluate intrapulmonary vascular dilatation associated with right-to-left shunts.
See also
-
pulmonary complications of cirrhosis and portal hypertension
hepatopulmonary syndrome (HPS)
portopulmonary hypertension (POPH)
hepatic hydrothorax (HH)




 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.