Hypertrophic olivary degeneration is a rare condition characterized by a unique pattern of trans-synaptic degeneration. Typically it is caused by a lesion in the brainstem/cerebellum interrupting the triangle of Guillain and Mollaret (a.k.a. dentatorubro-olivary pathway), resulting in hypertrophy of the inferior olivary nucleus.
On this page:
Clinical presentation
Oculopalatal tremor is a distinctive part of the presentation of hypertrophic olivary degeneration, although is also seen in many other brainstem and cerebellar conditions 4. Oculopalatal tremor comprises ocular, palatal and other muscular involuntary movements 7-9.
-
palatal tremor/myoclonus (symptomatic palatal tremor/myoclonus) 7-9
rhythmic 1-3 Hz involuntary movement of the soft palate and uvula potentially extending to involve the pharynx and larynx
often persists during sleep
no associated audible clicking
not always be present, but when it is present, it is pathognomonic
oscillopsia may be present due to the pendular nystagmus caused by the ocular myoclonus 4,8
upper extremity tremor (Holmes tremor) may also be present 4,8
facial, cervical, intercostal, and diaphragmatic tremor/myoclonus may also be present 7,8
Pathology
Hypertrophic olivary degeneration is bilateral in ~75% of cases 10. It should be noted, however, that in a significant proportion of patients (~45% in one study) no causative lesion will be identified in the triangle of Guillain and Mollaret, more commonly in cases of bilateral hypertrophic olivary degeneration 5.
Etiology
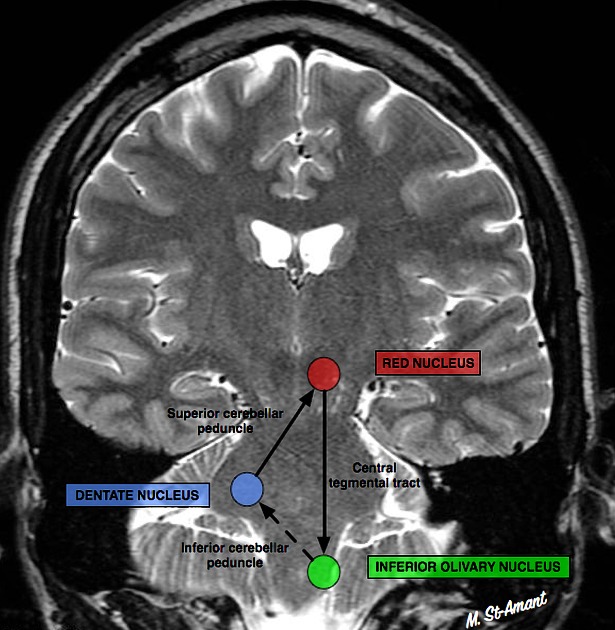
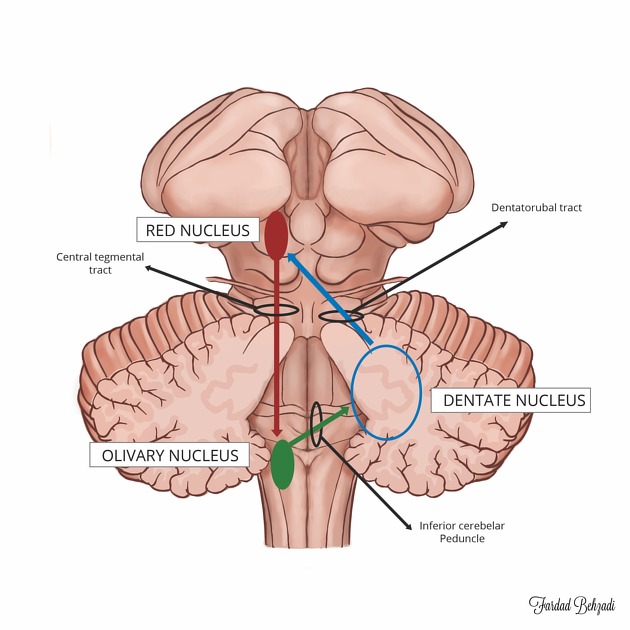
The connection between the red nucleus, ipsilateral inferior olivary nucleus and the contralateral dentate nucleus forms the triangle of Guillain and Mollaret. Interruption of either connection between the dentate nucleus and contralateral red nucleus (dentatorubral tract, superior cerebellar peduncle) or the connection between the red nucleus and ipsilateral inferior olivary nucleus (central tegmental tract) leads to changes in the olive. The olive receives inhibitory (GABAergic) signals within the dentato-rubro-olivary pathway, with transneuronal degeneration causing enlargement rather than atrophy.
Pathologically, this is characterized by "transsynaptic degeneration resulting in vacuolation of the neurons" and an increase in astrocytes. Isolated lesions of the inferior cerebellar peduncle do not cause hypertrophic olivary degeneration, as anatomically there are no direct connections between the inferior olivary nucleus and the contralateral dentate nucleus (fibers from the inferior olivary nucleus project to the cerebellar cortex via the olivocerebellar tracts and then to the dentate nucleus).
Oculopalatal tremor results from disinhibition of the inferior olivary nucleus, following the pathology in dentato-rubro-olivary pathway which is further modulated by the cerebellum 4.
Temporal evolution
The changes observed within the medulla occur in a predictable sequence after the inciting insult and underpin the imaging features 1.
0-2 days: no olivary changes
2-7 days: olivary amiculum (the white matter surrounding the olivary nucleus) degeneration
3 weeks: olivary hypertrophy due to neuronal hypertrophy
~8.5 months: maximal olivary enlargement due to both neuronal and astrocytic hypertrophy
after 9.5 months: olivary pseudohypertrophy due to neuronal dissolution with the development of gemistocytic astrocytes
a few years: olivary atrophy due to neuronal disappearance and degeneration of the olivary amiculum
Radiographic features
MRI is the only reliable modality to identify hypertrophic olivary degeneration and is ideal for identifying a potential causative lesion.
MRI
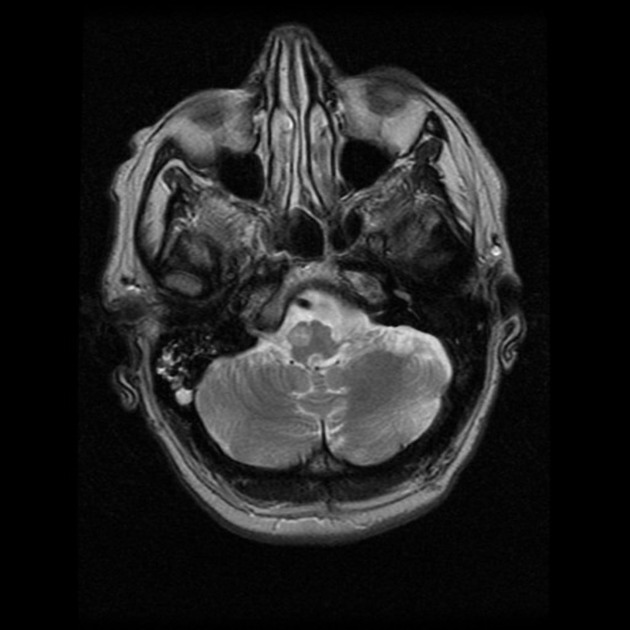
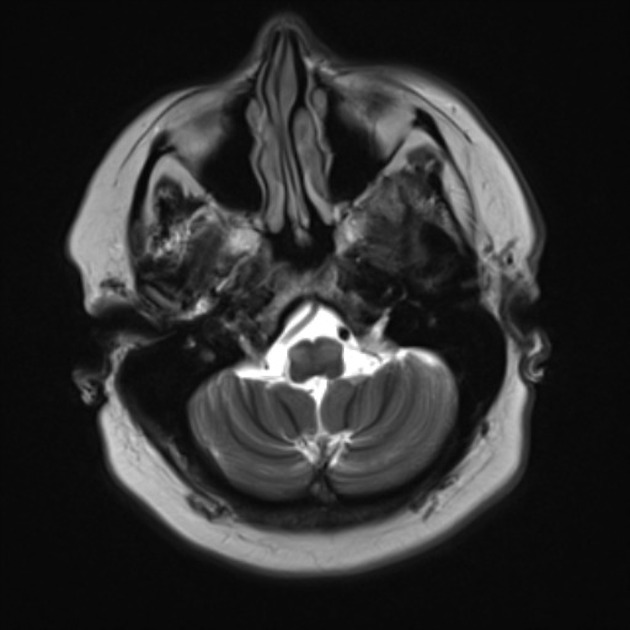
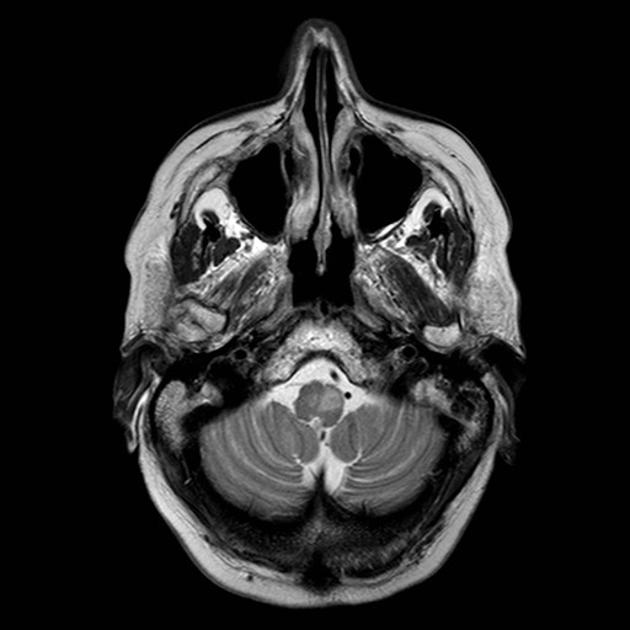
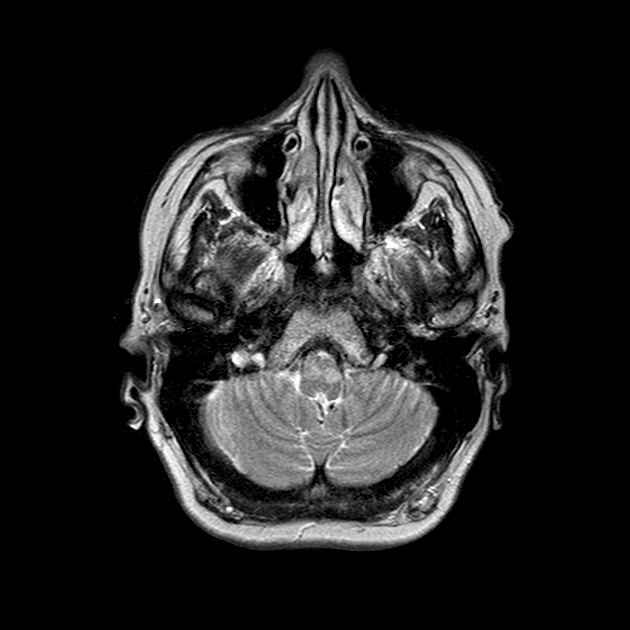
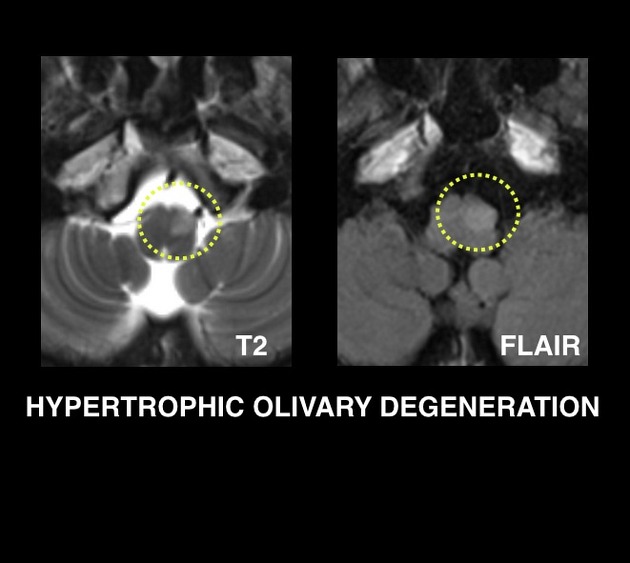
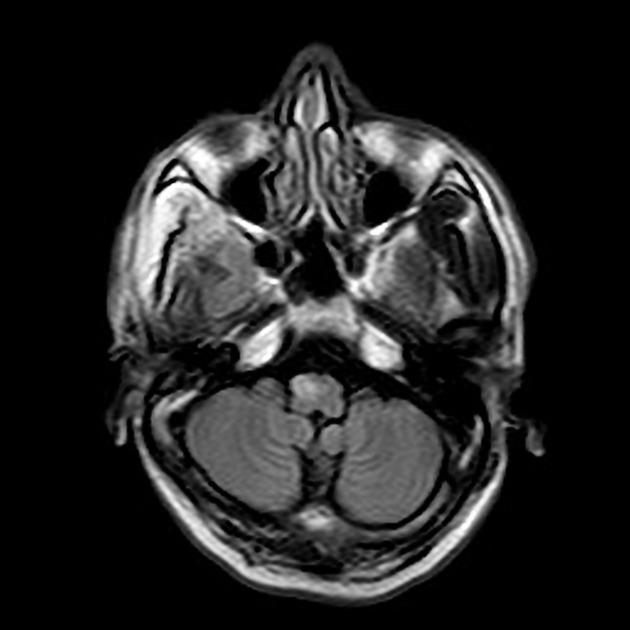
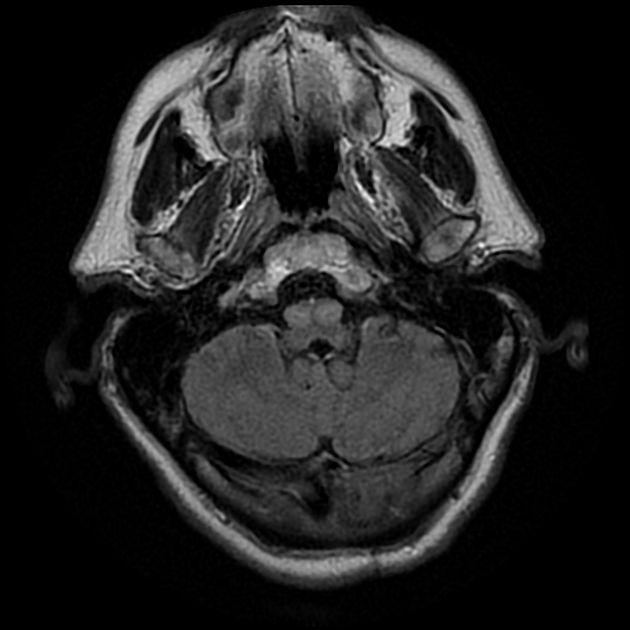
It takes a number of days for the earliest changes to be visible, appearing as an increase in T2 signal surrounding and then involving the inferior olivary nucleus. Towards the end of the first month the inferior olive begins to swell and T2 signal increases. This becomes maximal at approximately 9 months after the inciting injury 1. Over the following 2 to 4 years olivary swelling gradually subsides, but T2 hyperintensity persists resulting in an atrophic hyperintense olive.
The ipsilateral red nucleus may also lose the expected normal hypointensity on SWI 6.
Enhancement and restricted diffusion are not features of hypertrophic olivary degeneration 8.
Treatment and prognosis
Management is primarily directed towards the underlying cause 9. Otherwise, pharmacological symptomatic treatment of oculopalatal myoclonus (e.g. sodium valproate, clonazepam) tends to not be successful 8,9.
Differential diagnosis
General imaging differential considerations include:
infarction
metastases
lymphoma
infection, including tuberculosis
Clinical differential considerations include:





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.