A single contrast enema is a method of imaging the colon with fluoroscopy and is similar in concept to the double contrast barium enema. "Single contrast" refers to imaging with a positive contrast medium, either barium or water-soluble contrast, without the addition of air or CO2.
On this page:
Images:
Indications
The single contrast technique may be preferred over the double contrast technique when
-
the patient is unable to turn quickly/effectively
double contrast technique requires rapid changes in patient position
when only the position and length of a stricture is required
evaluation for acute diverticulitis (and CT unavailable for whatever reason)
evaluating for a colonic fistula
evaluation for postoperative leak after colon surgery
to detect the presence of Hirschsprung disease (using water soluble contrast enema) in neonates 1
Contraindications
There are few contraindications. If evaluation of the colonic mucosa is what is clinically desired, then a double contrast barium enema is preferred. If screening for colon cancer, then CT colonography is preferred.
Water-soluble contrast should be used when evaluating for postoperative leak.
Procedure
Equipment
-
rectal tube (e.g. Miller) for the administration of contrast
tape is often useful to tape the tube to the patient and prevent it from backing out
enema bag and IV pole
One of the most important considerations for a single contrast barium enema is the density of the barium sulfate or water-soluble contrast. If it is too dense, then not only will the fluoroscopic tube "burn out" the background image and obscure overlapping loops, it will also obscure smaller (and sometimes large!) colonic lesions. You want contrast that is dense enough to see filling defects, but not too dense. Where this optimal density lies is dependent on one's fluoroscopic equipment and available contrast solutions. In general, 20% w/v is not a bad target. Water-soluble contrast media (e.g. Gastrografin) should also be diluted to approximately 20%.
Barium sulfate often comes in 100% w/v solutions, so a way to get to 20% w/v density is
400 mL of 100% w/v barium added to 1600 mL of water (2000 mL total)
Some radiologists also prefer giving the patient 1 mg of glucagon (IV or SC) before the exam to relax the colon, but this is not mandatory and has questionable utility.
If the patient has trouble holding the balloon in the rectum (and assuming there is no obvious rectal/anal problem such as severe proctitis or tumor), then the balloon on the enema tip can be inflated to keep the tube in place.
Technique
The following technique is for a standard single contrast exam. If the exam is for a postoperative leak or for evaluation of a known lesion, it can be modified.
-
scout views
AP abdomen
AP pelvis
left lateral pelvis
Then bring the enema bag on the IV pole up and let the contrast flow in under gravity.
left lateral view of the rectum
left lateral view of the rectosigmoid junction
LPO of mid sigmoid
RPO of rectosigmoid junction
(optional R lateral rectum)
RPO of descending colon and splenic flexure
barium flows through the transverse colon and into the ascending colon, LPO of the hepatic flexure
AP views of the transverse colon
-
the contrast should continue to flow until it reaches the cecum and the ileocecal valve (and possibly the appendix) can be seen
AP and/or oblique views of the ascending colon, cecum, and possibly the terminal ileum
During the exam, palpation should be performed to press out the contrast at the head of the contrast column. This allows for some evaluation of the mucosa. This is harder to do when the colon is completely full of contrast. It may be impossible to compress the colonic flexures underneath the ribs.
The sequence above is a suggestion. When performing the exam, the key points are to
ensure you image the entire colon
ensure you adequately evaluate any suspicious areas
Don't slavishly follow a protocol sequence. If you need to break out of an imaging sequence to accomplish either of these goals...then do it!
At the end of the exam, empty the contrast out of the colon and then obtain
-
post evacuation radiograph
consider post evacuation compression and spot radiographs of suspicious areas
Postprocedural care
The patient should be encouraged to stay hydrated and warned that, if using barium, not to be alarmed if white material comes out in future stools.


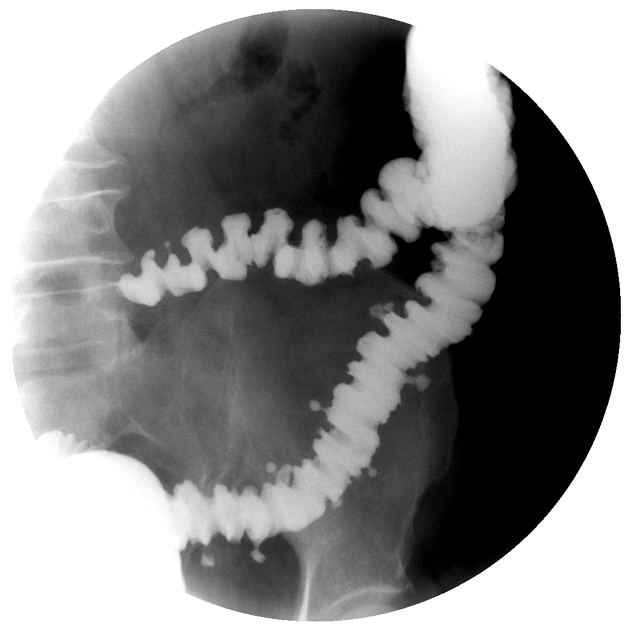


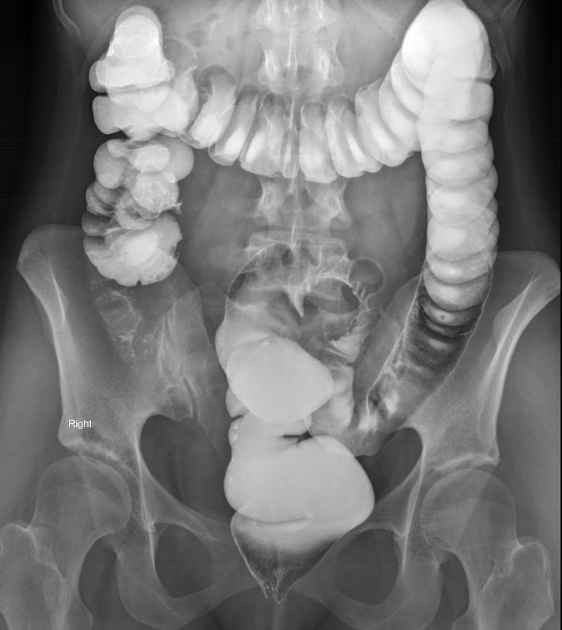


 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.