Suprasellar cistern lipomas are uncommon, usually incidental findings, with characteristic imaging features and very limited differential diagnosis. A proportion of these lesions can peripherally ossify, in which case they are referred to as osteolipomas 4.
For a general discussion of intracranial lipomas please refer to the general article: intracranial lipoma.
On this page:
Epidemiology
Suprasellar cistern lipomas have an incidence of approximately 0.4% 3 and account for ~15% of all intracranial lipomas, third in frequency after pericallosal lipomas and quadrigeminal cistern lipomas 1.
Clinical presentation
Unlike the more common pericallosal lipomas, which are usually associated with dysgenesis or hypogenesis of the corpus callosum and other congenital malformations (and associated symptoms), suprasellar lipomas are usually asymptomatic and are only found incidentally either at autopsy or when the brain is imaged for other reasons.
Radiographic features
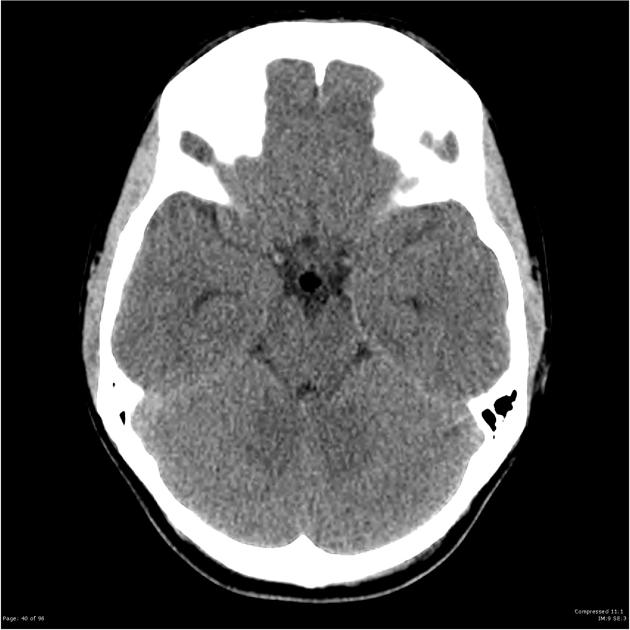
CT
Suprasellar lipomas appear as small fat density regions in the suprasellar cistern, with matching negative density measurements (-30 to -100 HU). If calcification is present then the term osteolipoma should be used 4.
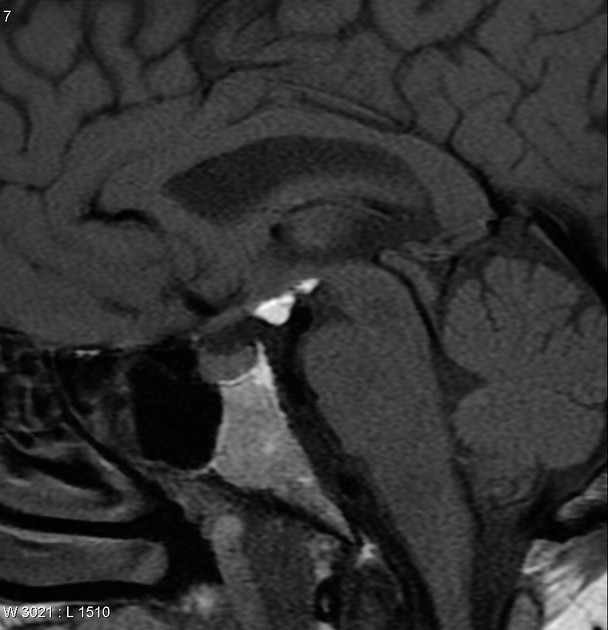
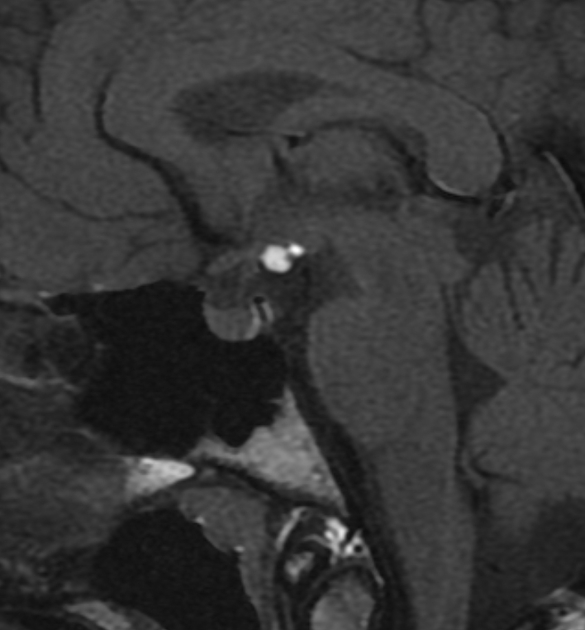
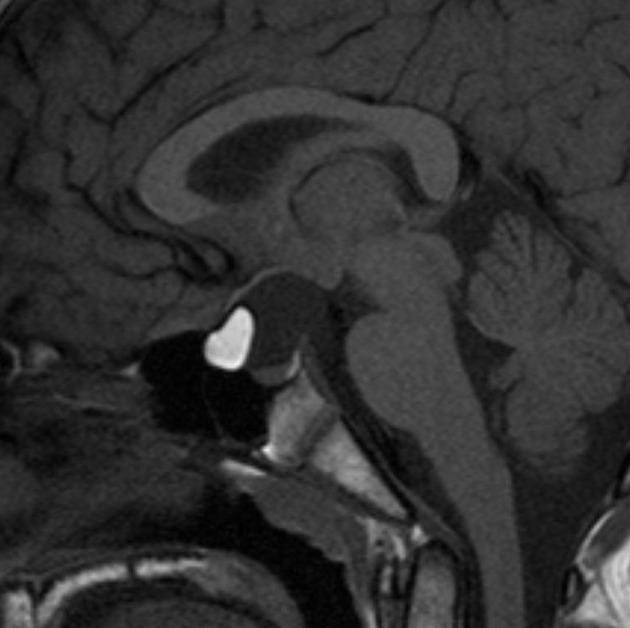
MRI
MRI is the modality of choice for assessing these lesions as not only does it have exquisite sensitivity and specificity for the detection and characterization of fatty lesions (provided fat-saturated sequences are performed), but it is also able to demonstrate local anatomy.
The sine qua non of intracranial lipomas is nodular tissue which follows fat on all sequences including fat-suppressed sequences, and does not demonstrate solid enhancing components 1,2.
The tissue is usually applied to the floor of the third ventricle immediately behind the infundibulum of the pituitary gland, in close proximity to the hypothalamus, tuber cinereum and mammillary bodies.
Differential diagnosis
The differential diagnosis for a suprasellar cistern lipoma is very limited and is essentially that of pituitary region masses with intrinsic high T1. As CT and fat-saturated sequences (or presence of chemical shift artifact) are usually able to confirm that the mass is fatty the differential is narrowed further:
-
dermoid: mature teratoma
- less common
- often more heterogeneous in signal (due to the presence of hair desquamated cells, etc)
- often there is evidence of previous rupture with fat droplets scattered in the subarachnoid space
-
teratoma: immature teratoma
- similar to dermoid, but usually have a solid enhancing or cystic component
-
osteolipoma
- ossification of a lipoma









 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.