Lipomas are benign tumors composed of mature adipocytes. They are the most common soft tissue tumor, seen in ~2% of the population.
On this page:
Epidemiology
Patients typically present in adulthood (5th-7th decades).
Associations
In some cases, multiple lipomas are associated with syndromes and other diseases, including:
obesity 10
Diagnosis
Diagnostic criteria according to the WHO classification of soft tissue and bone tumors (5th edition) 10:
essential: yellow-tan circumscribed mass; uniform proliferation of mature adipose tissue with atypical hyperchromatic stromal cells
desirable: absence of giant marker/ring chromosomes / MDM2 amplification
Clinical presentation
Typically lipomas are subcutaneous in location and present in adulthood as a soft painless mass in the trunk or proximal extremities. They are likely to have been present for many years and may change size with weight fluctuation.
Pathology
The etiology of lipomas is unknown 10. In 5-15% of patients, lipomas are multiple, and ~33% of these will be familial 5.
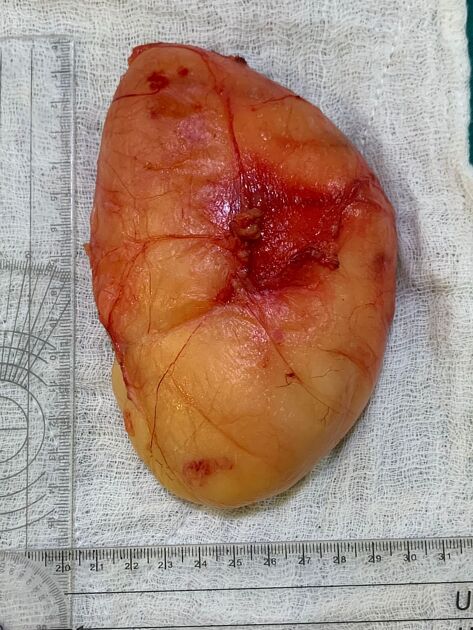
Macroscopic appearance
Benign lipomas are circumscribed soft masses, usually encapsulated, and composed almost entirely of fat. Superficial lipomas are usually <5 cm whereas deep lipomas can be >20 cm 10. A small amount of non-adipose components are often present, representing fibrous septa, areas of fat necrosis, blood vessels, and interposed muscle fibers. Any non-adipose components must be carefully assessed to exclude a more aggressive component. Lipomas containing metaplastic cartilage or bone are called chondrolipomas or osteolipomas respectively 10.
Microscopic appearance
Histology demonstrates mature adipocytes with no cellular atypia or pleomorphism 4.
Intramuscular lipomas have nearly identical histology to superficial lipomas; however, intramuscular lesions tend to invade the adjacent musculature and commonly lack a capsule. These are sometimes known as infiltrating lipomas. In contradistinction, intermuscular lipomas do not exhibit local invasion and tend to be lobular or dumbbell-shaped, easily separated from adjacent soft tissues during surgical resection 6,7.
Location
Most lipomas are superficial in the subcutaneous tissues 10. A minority of lipomas are found in deeper locations and include intramuscular, intermuscular, intrathoracic, and retroperitoneal lipomas.
-
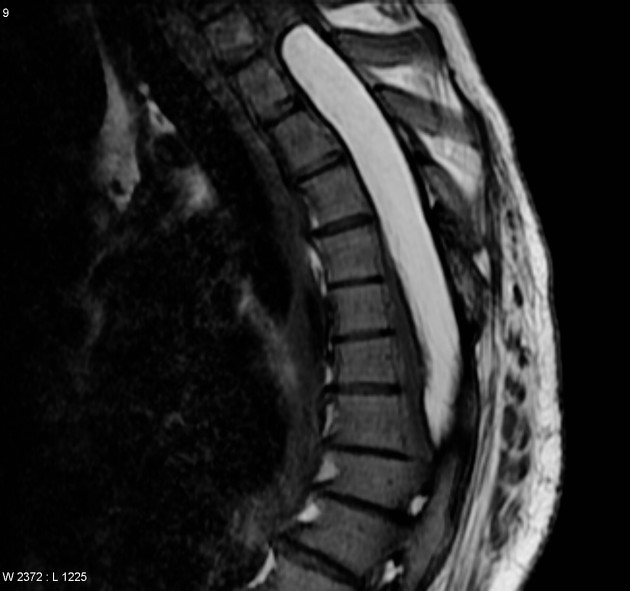
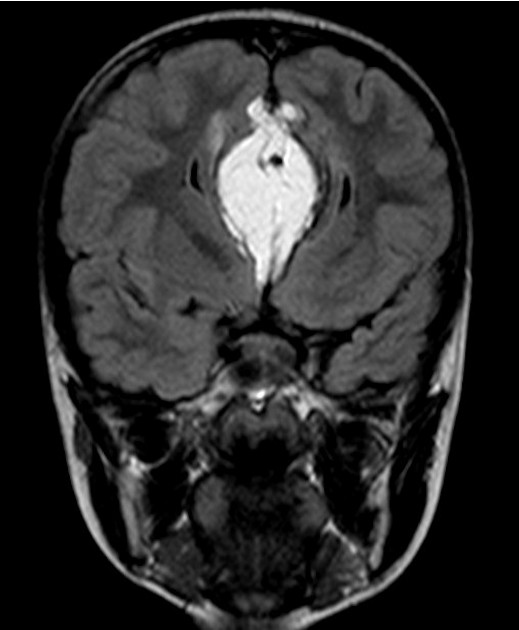
central nervous system and spine
-
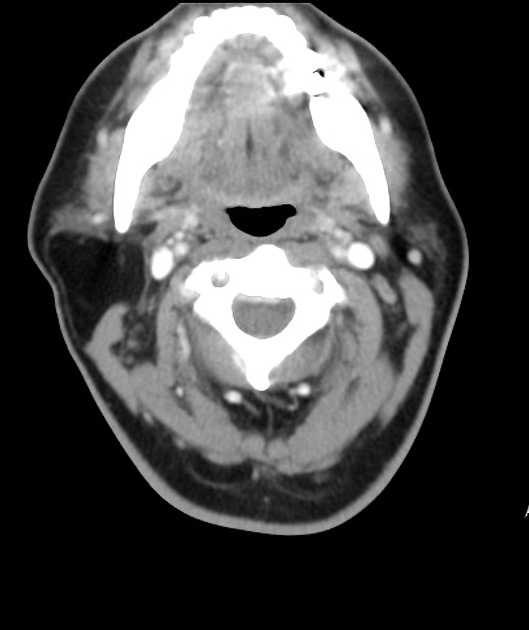
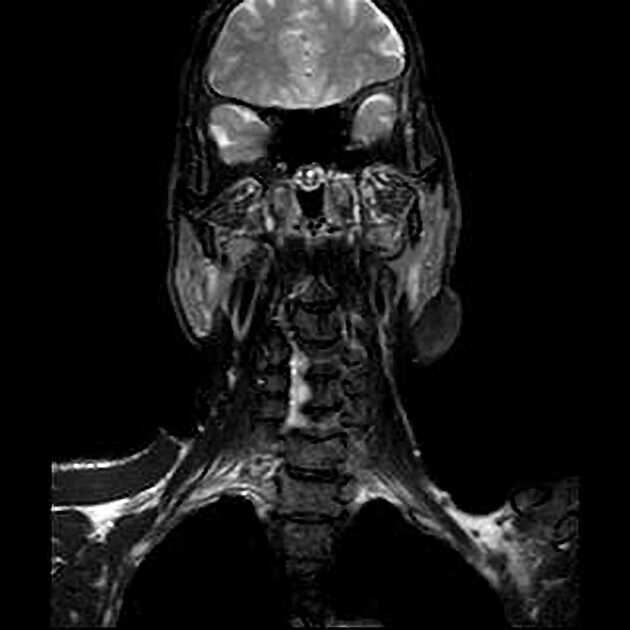
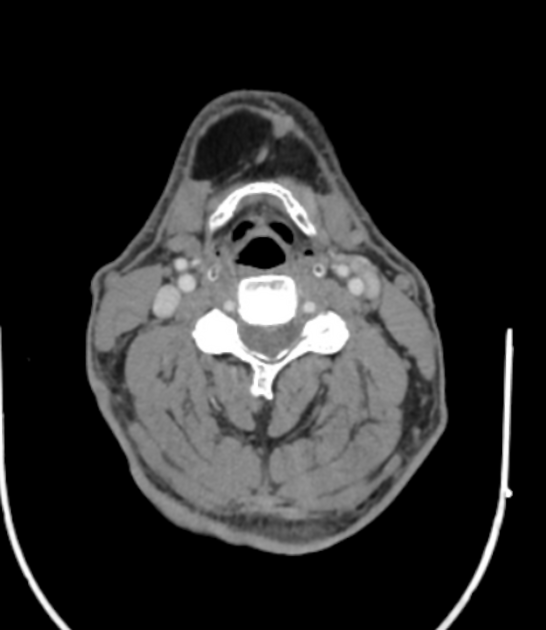
head and neck
-
thoracic
-
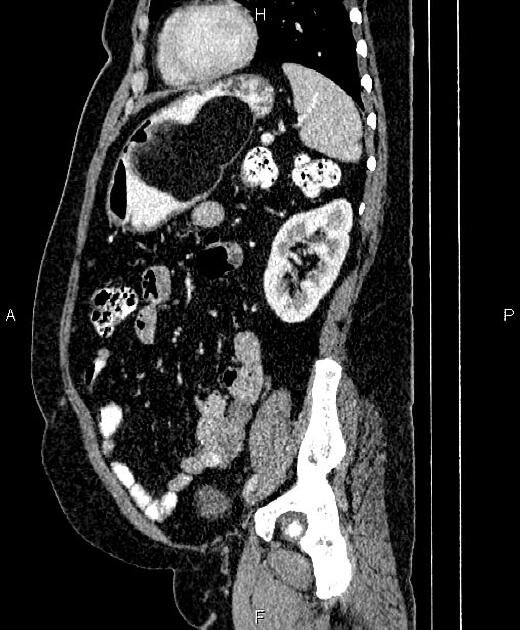
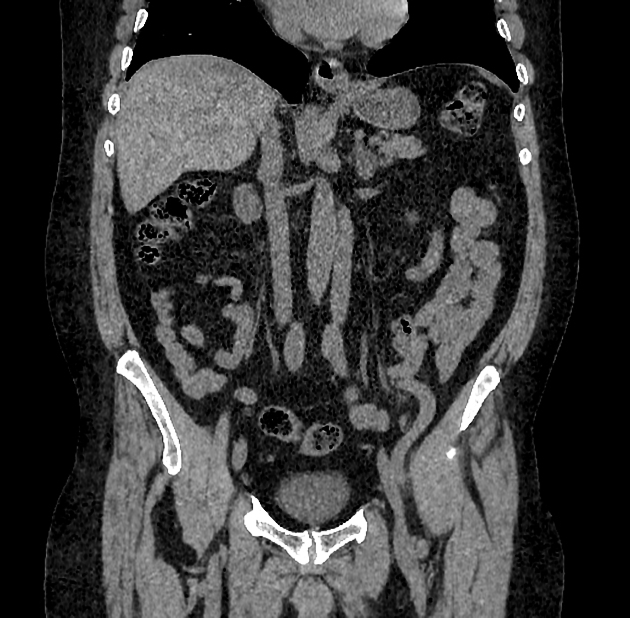
abdominopelvic
-
urogenital
-
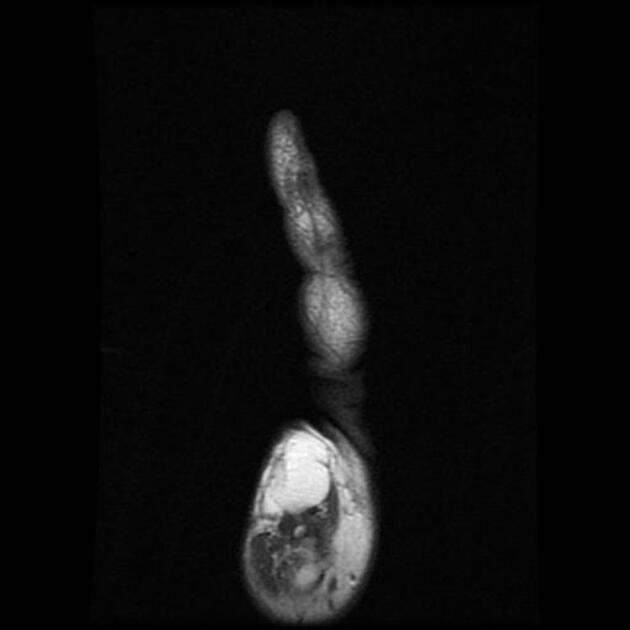
musculoskeletal
-
vascular
Radiographic features
Superficial lipomas are typically well-circumscribed ovoid masses with homogeneous imaging characteristics of fat. A thin capsule, very thin septations (<2 mm), and scattered small areas of soft tissue density are common; however, avidly enhancing, thick/nodular septa or evidence of local invasion are suggestive of malignancy.
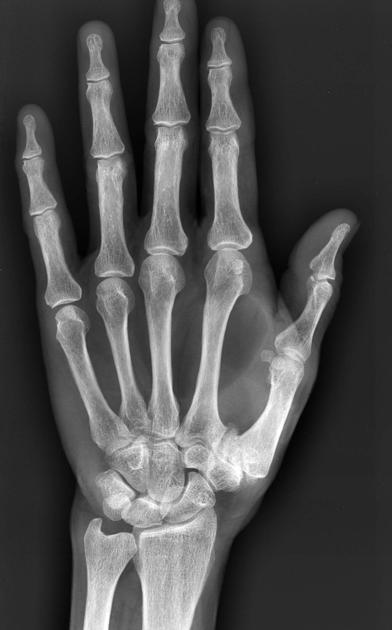
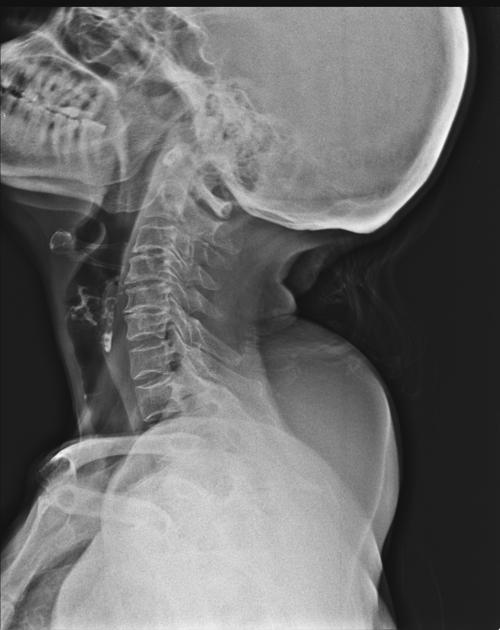
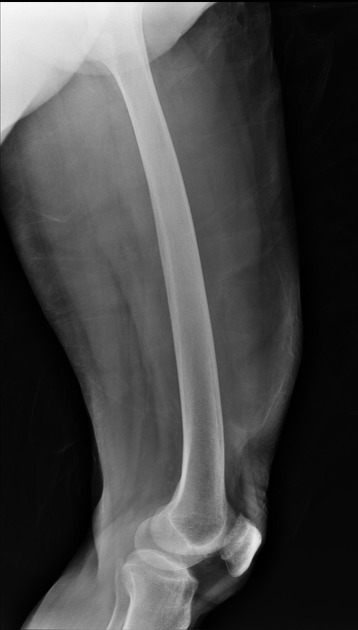
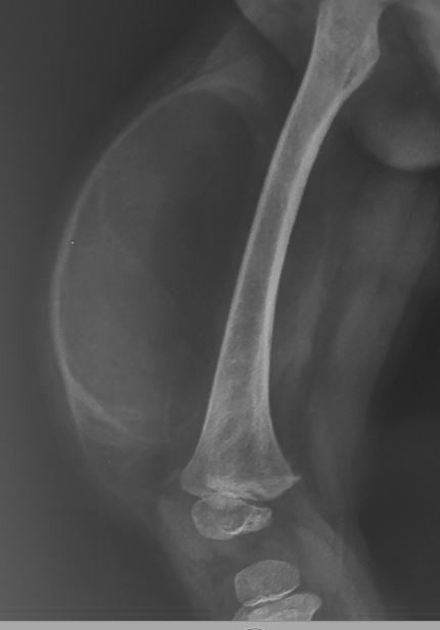
Plain radiograph
Large lipomas may be appreciated as a region of low density exerting mass effect. Calcification may be present in up to 11% of cases, although more commonly associated with well-differentiated liposarcoma 5.
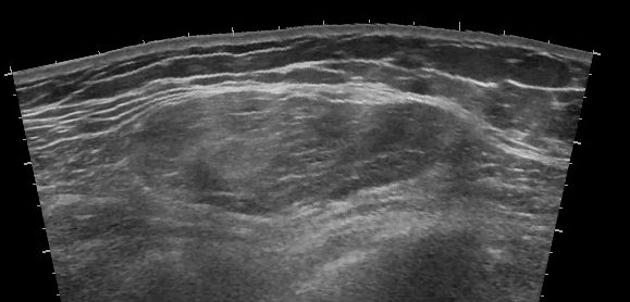
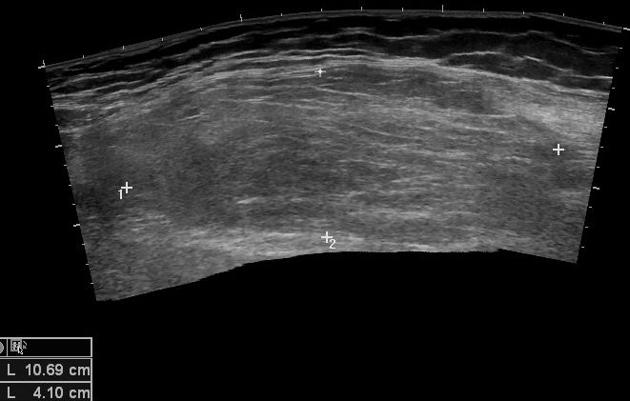
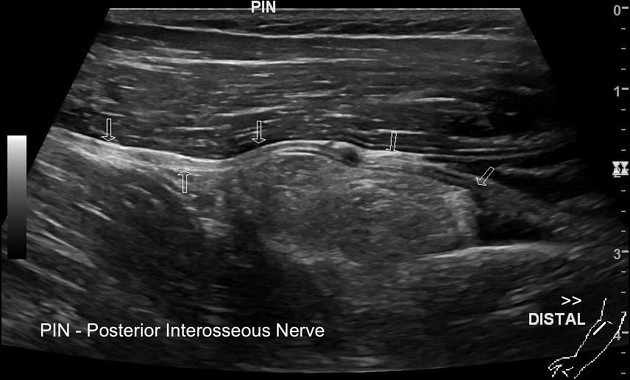
Ultrasound
Lipomas appear as variably echogenic masses on ultrasound. If encapsulated, the capsule may be difficult to identify on ultrasound 5. There is a wide range of appearances of biopsy-proven lipomas, with wide inter-reader variability 8 :
hyperechoic: 20-52%
isoechoic: 28-60%
hypoechoic: 20%
Superficial lipomas most commonly are isoechogenic and homogenous 11.
They can also display other ultrasound features 9:
no acoustic shadowing
no or minimal color Doppler flow
Heterogeneous echotexture, more than minimal color Doppler flow, or large size is suspicious for liposarcoma.
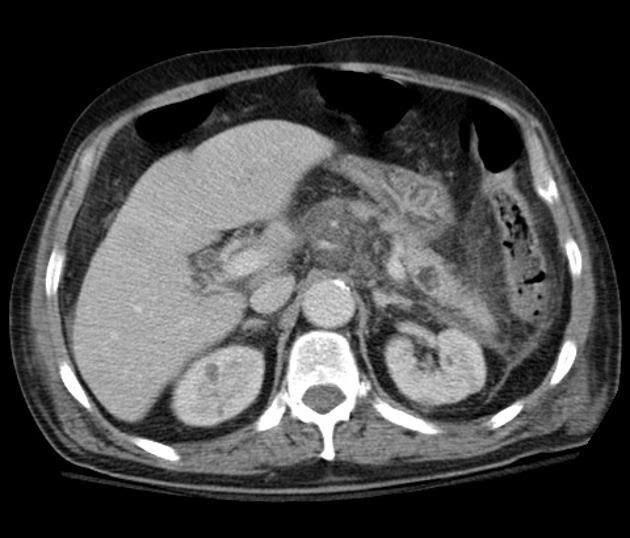
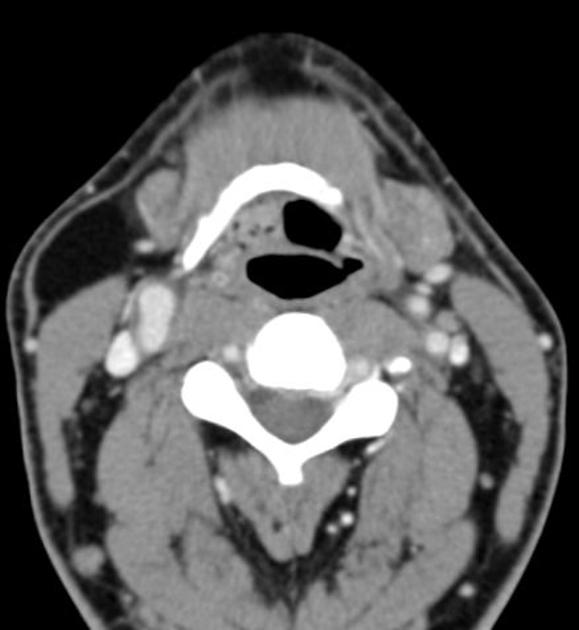
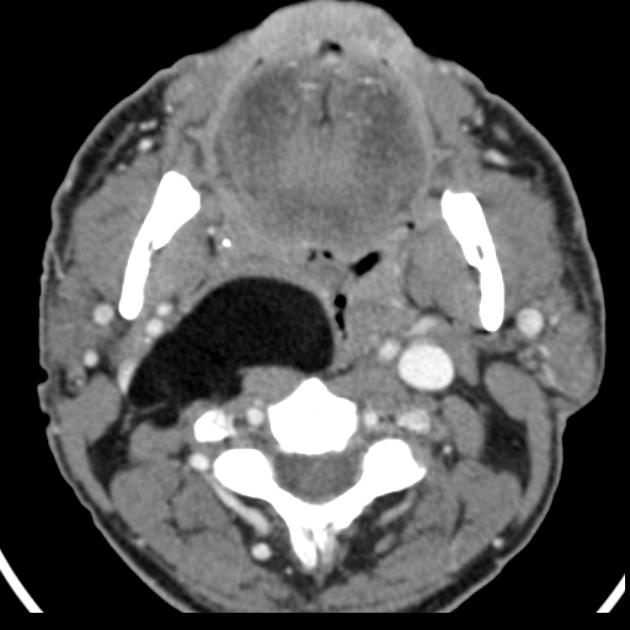
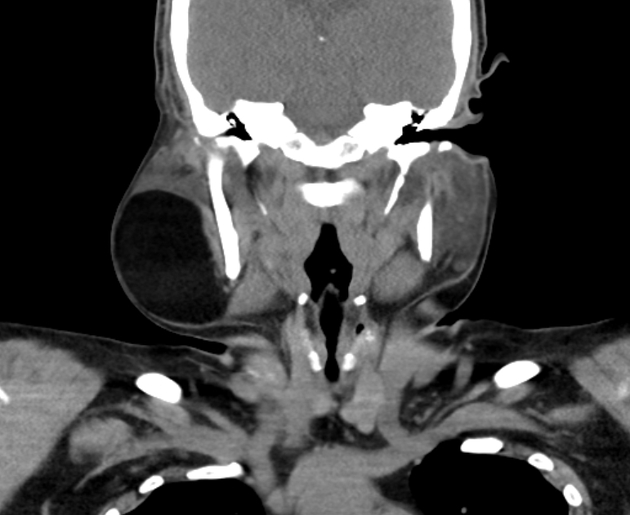
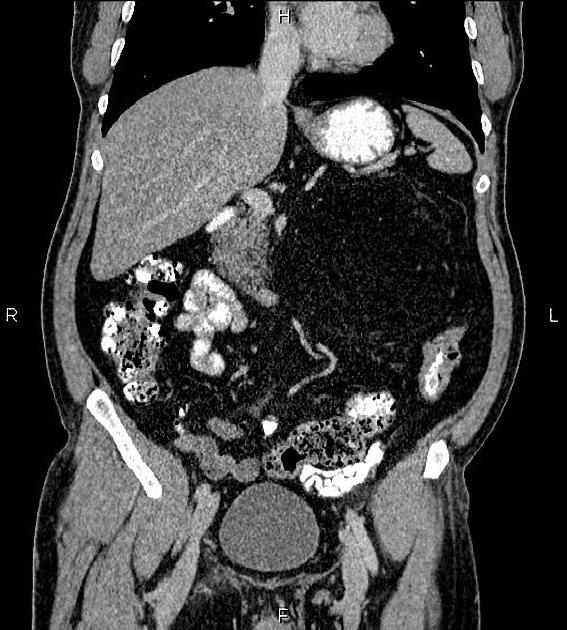
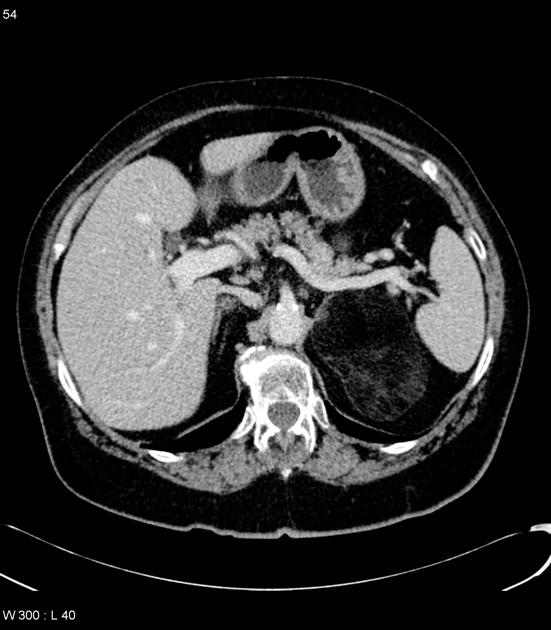
CT
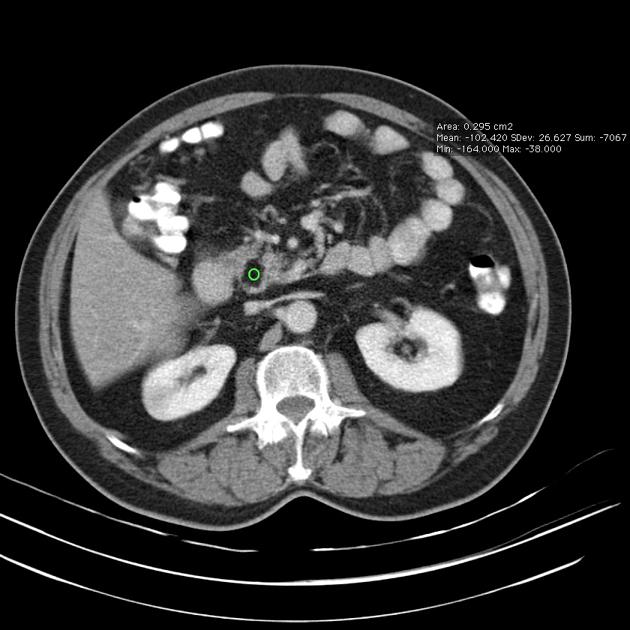
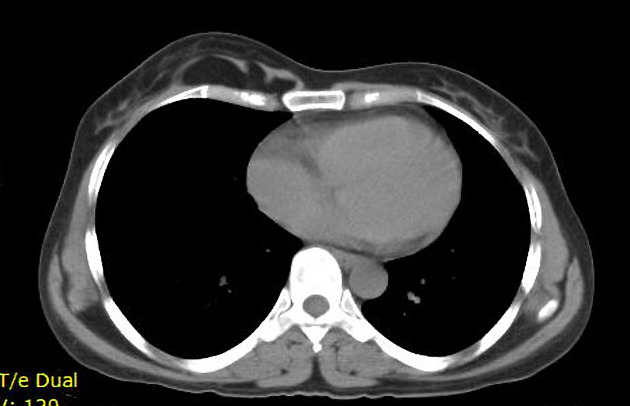
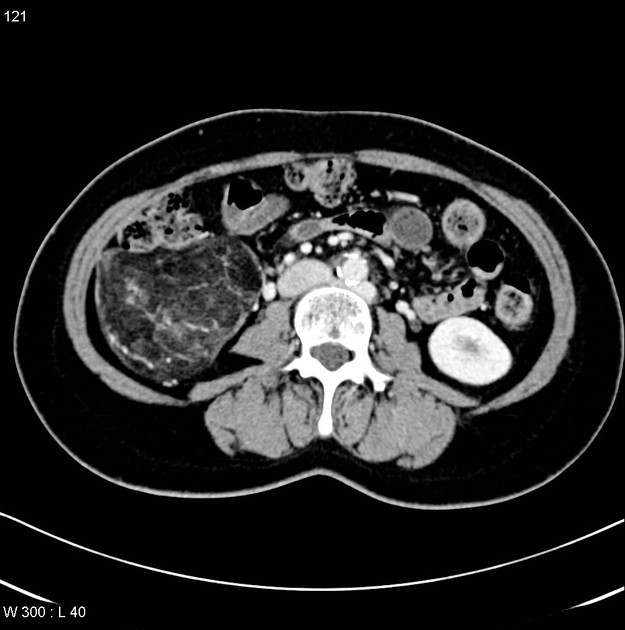
Classic appearances are of a superficial circumscribed, low attenuation mass (typically approximately -65 to -120 HU) 3-5 with minimal internal soft-tissue component. Again, areas of calcification may be present although are more frequently associated with well-differentiated liposarcoma 5.
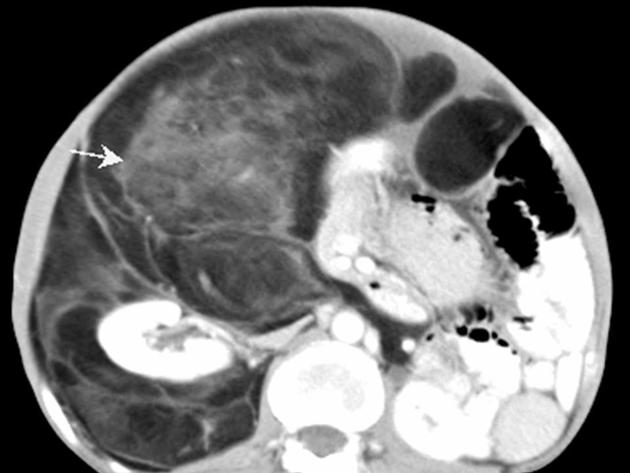
Deeper or larger lesions may have scattered areas of internal soft-tissue density, often more apparent on CT versus MRI. These may represent areas of fat necrosis, fibrous tissue, blood vessels, or muscle fibers; these lesions cannot be confidently differentiated from liposarcoma by imaging.
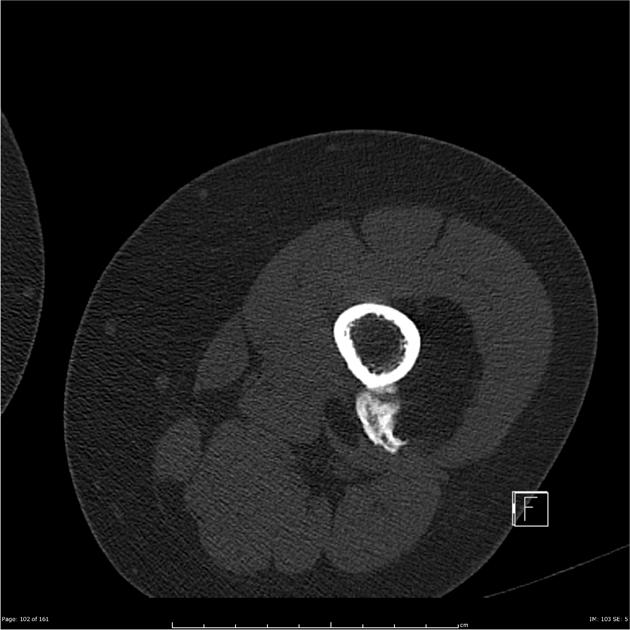
Intramuscular lipomas may invade and interdigitate with the associated skeletal muscle, resulting in a characteristic striated appearance that may help distinguish them from liposarcoma 5.
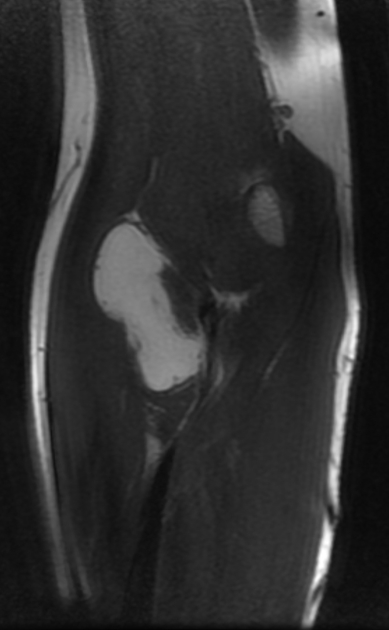
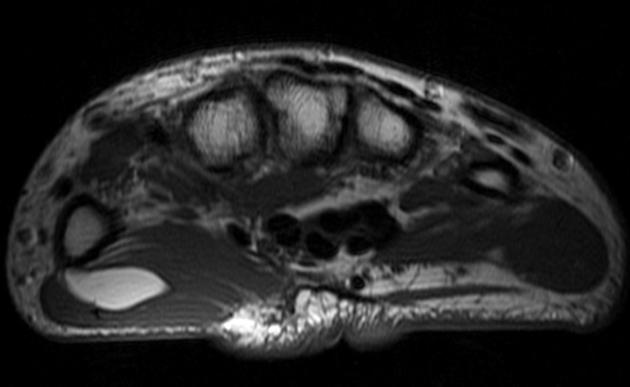
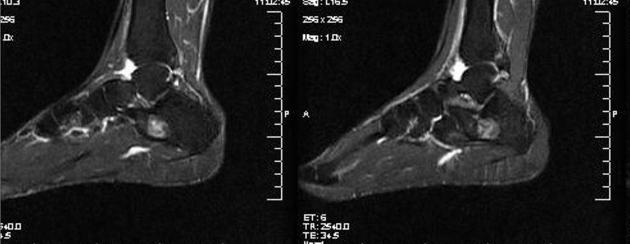
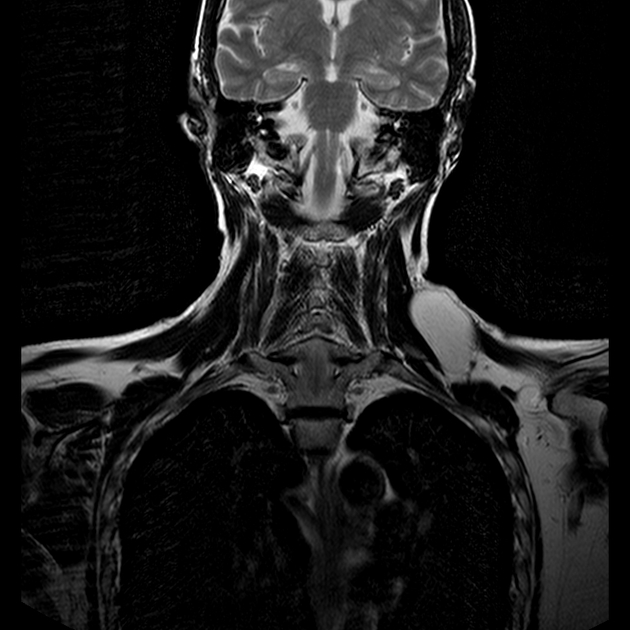
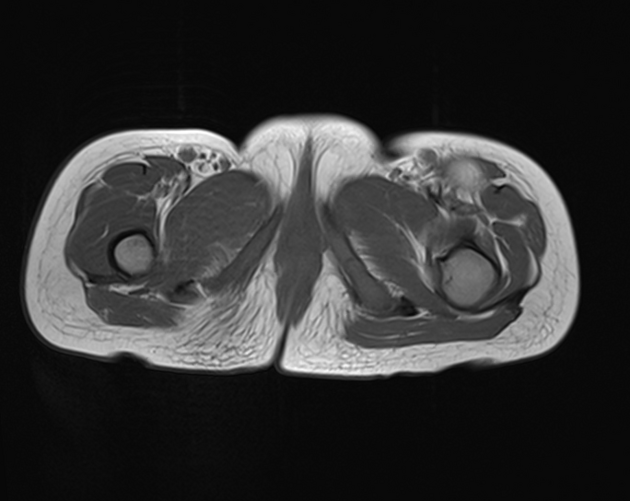
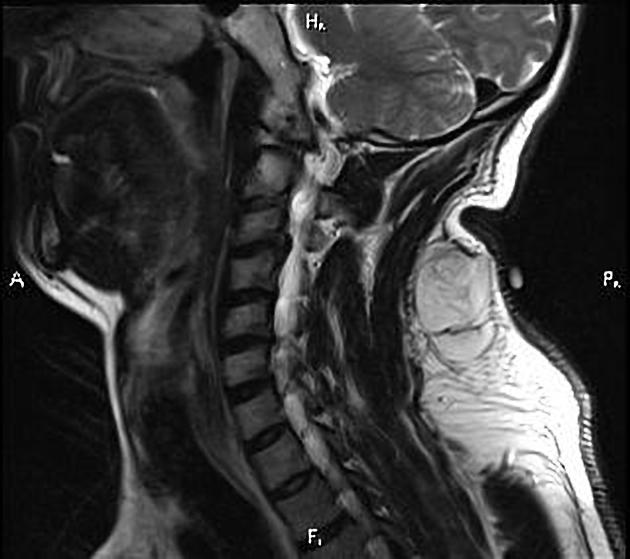
MRI
MRI is the modality of choice for imaging lipomas, not only to confirm the diagnosis, which is usually strongly suggested by ultrasound and CT but also to better assess for atypical features suggesting liposarcoma. Additionally, MRI is better able to demonstrate the surrounding anatomy.
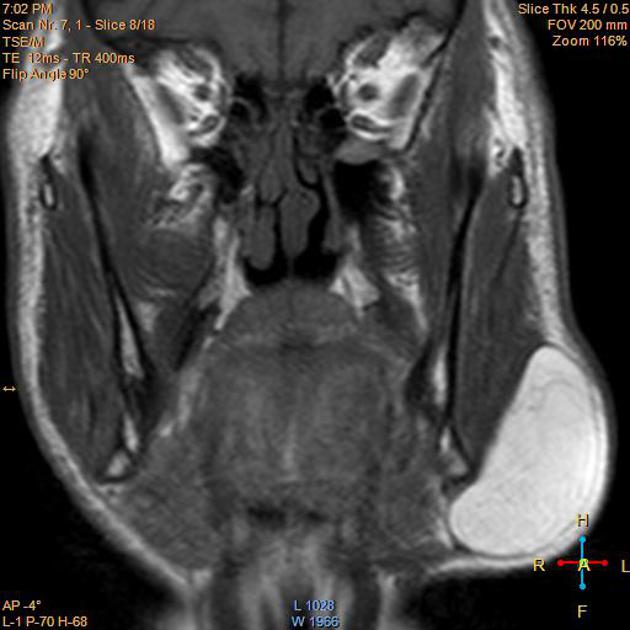
As expected, lipomas follow subcutaneous fat signal on all sequences:
-
T1
high signal
saturates on fat-saturated sequences
no or minimal enhancement
-
T2
high signal on FSE T2
saturates on fat-saturated sequences: persistent areas of high T2 signal are worrisome
When no suspicious features are present, the diagnosis of lipoma can be made with confidence with MRI being 100% specific 1. Similarly, if suspicious features are present, then the sensitivity of MRI is 100% 1, although specificity is lower, as some masses with atypical features will nonetheless be lipomas.
Radiology report
Size and location should be described. Location not only includes the anatomical site but whether the mass is superficial or deep, intramuscular, etc. When reporting lipomas on MRI, the article lipoma vs well-differentiated liposarcoma covers the differentiating factors well.
Treatment and prognosis
If all characteristics are those of a simple lipoma, and no local symptoms such as pain are present, then no treatment is generally required. However, resection for cosmesis is also a reasonable indication. If any concern exists, then biopsy or excision is required, with care taken about the approach in case the lesion is malignant. Recurrence rates of 4-5% are reported (most in deeper lesions) 5.
Differential diagnosis
In general, there is little differential for a classic soft tissue lipoma. The main differential is:
liposarcoma: low-grade tumors are difficult to differentiate from lipomas, and can have a relatively benign clinical course but suffer from a high rate of recurrence 1
normal adipose tissue
In certain locations, other fatty masses should be considered:
retroperitoneum, e.g. liposarcoma, adrenal myelolipoma, angiomyolipoma
thorax, e.g. thymolipoma, elastofibroma dorsi
Practical points
deep lipomatous masses should be assessed carefully, as they are more likely to be malignant and retroperitoneal fatty masses should be considered a well-differentiated liposarcoma until proven otherwise 5
















 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.