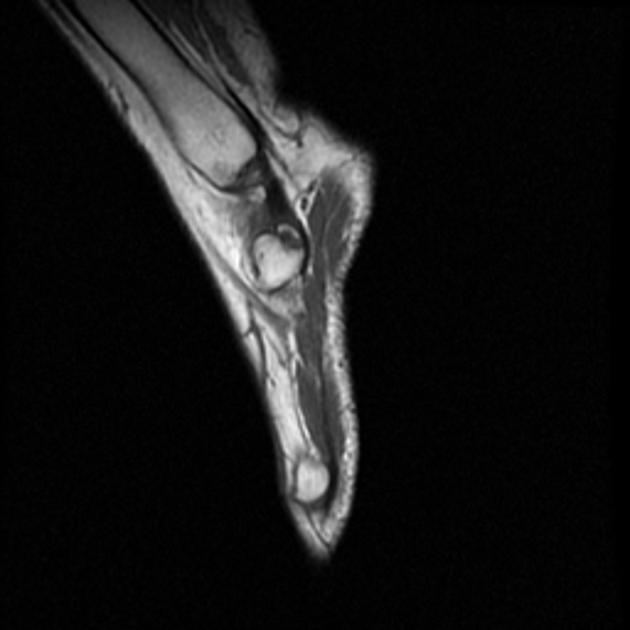
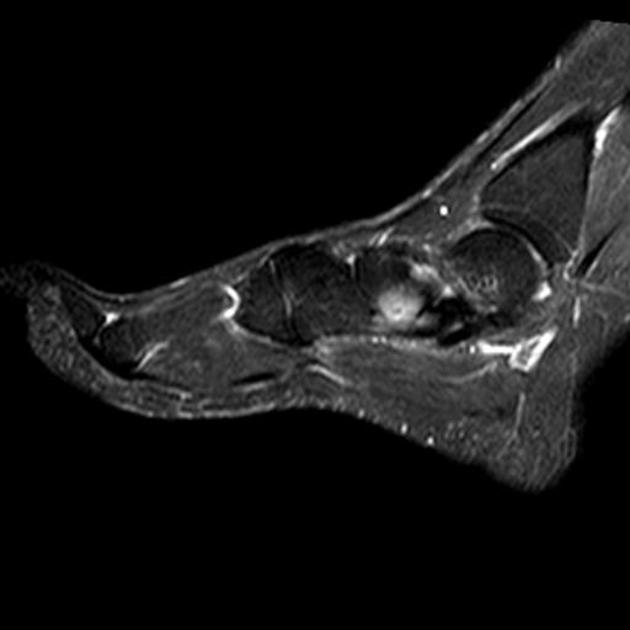
An accessory navicular is a large accessory ossicle that can be present adjacent to the medial side of the navicular bone. The tibialis posterior tendon often inserts with a broad attachment into the ossicle. Most cases are asymptomatic but in a small proportion, it may cause painful tendinosis due to traction between the ossicle and the navicular. Such changes are best seen on MRI.
On this page:
Epidemiology
the prevalence of an accessory navicular bone is ~10% (range 4-21%), although may be substantially higher (~45%) in Asian populations 9
first appears in adolescence
more common in female patients
reported bilateral prevalence is ~70% (range 50-90%)
Clinical presentation
Most of the time it is asymptomatic and found incidentally on radiographs, although medial side foot pain (accessory navicular syndrome) is the most common presenting feature of the accessory navicular bone. The pain is aggravated by walking, running and weight-bearing activities. When large, it can protrude medially and cause friction against the footwear.
Gross anatomy
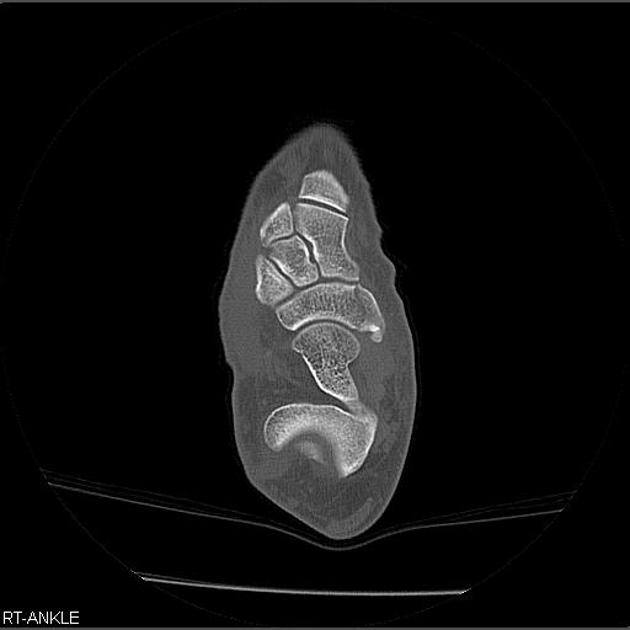
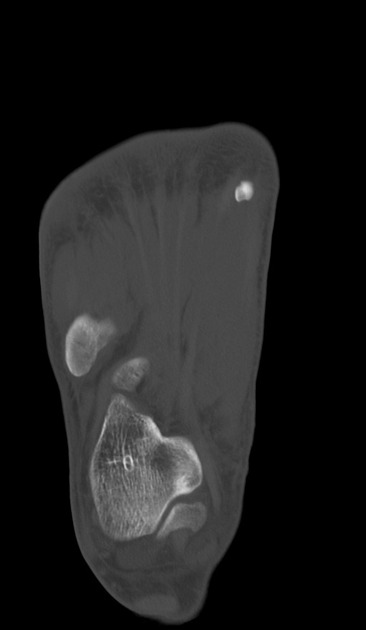
An accessory navicular bone is located posterior to the posteromedial tuberosity of the tarsal navicular bone.
Classification
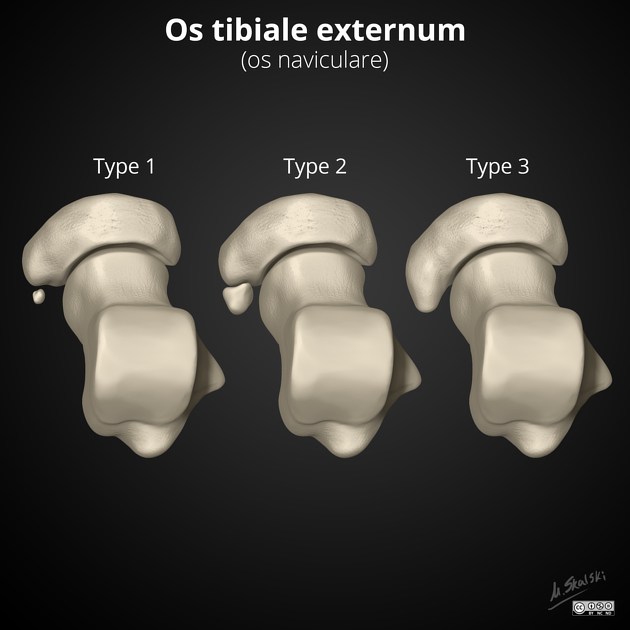
This classification was proposed by Emil Geist 7 in 1914 and remains the most widely used classification system (c. 2021). The Geist classification divides these into three types:
-
type 1 accessory navicular bone (os tibiale externum, os naviculare secundarium)
2-3 mm sesamoid bone embedded within the distal portion of the posterior tibial tendon
no cartilaginous connection to the navicular tuberosity and may be separated from it by up to 5 mm
accounts for 30% of accessory navicular bones
usually asymptomatic
-
type 2 accessory navicular bone (prehallux, bifurcate hallux)
accounts for ~55% (range 50-60%) of all accessory navicular bones
triangular or heart-shaped
typically measures around 12 mm
connected to the navicular tuberosity by a 1-2 mm thick layer of either fibrocartilage or hyaline cartilage
eventual osseous fusion to the navicular tuberosity may take place
-
type 3 accessory navicular bone
an especially prominent navicular tuberosity called a cornuate navicular
thought to represent a fused type 2 and is occasionally symptomatic as a result of painful bunion formation over the bony protuberance
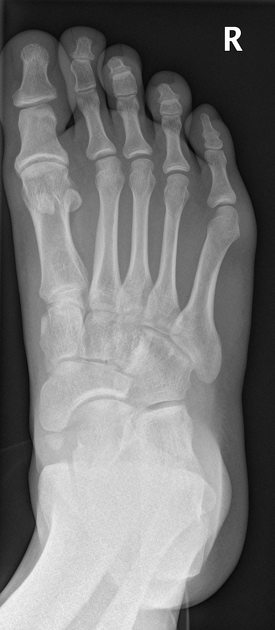
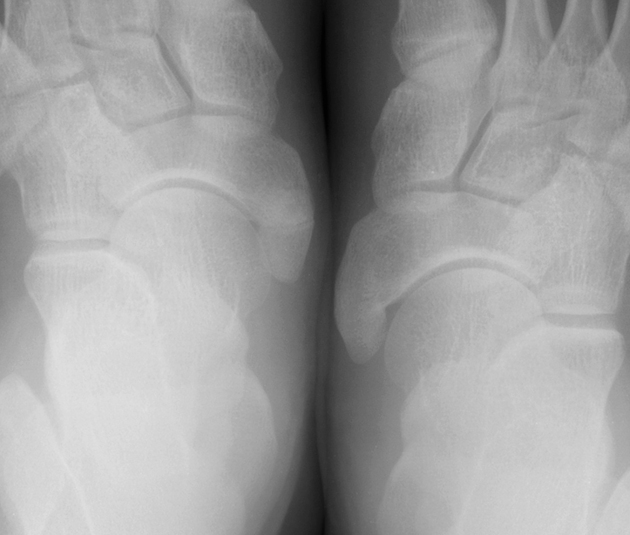
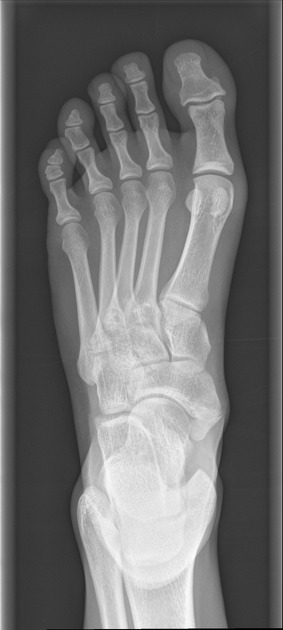
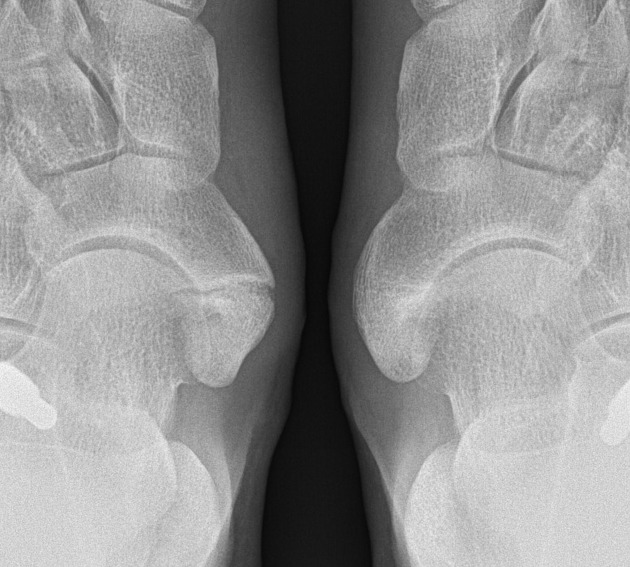
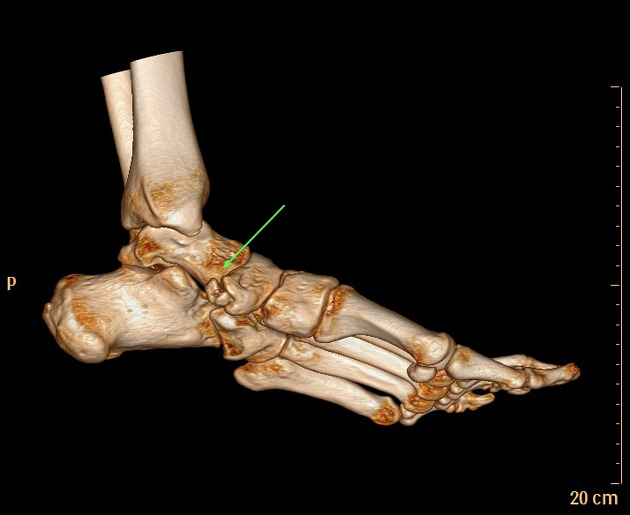
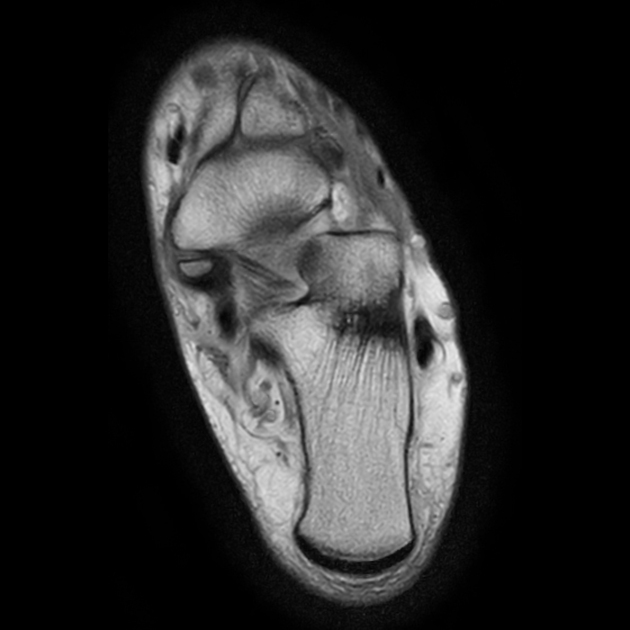
Radiographic features
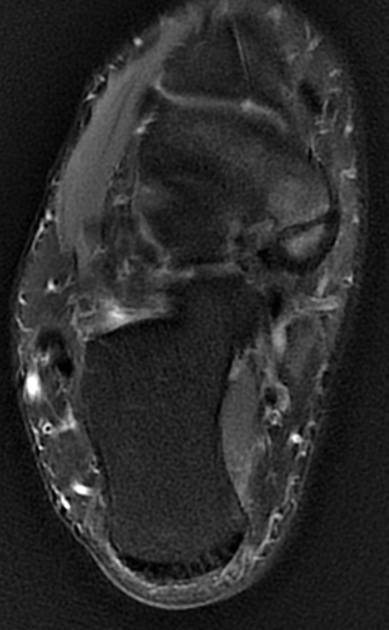
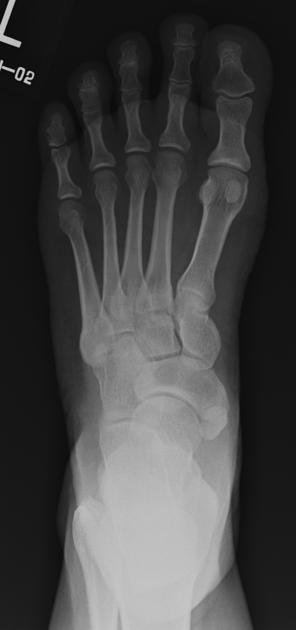
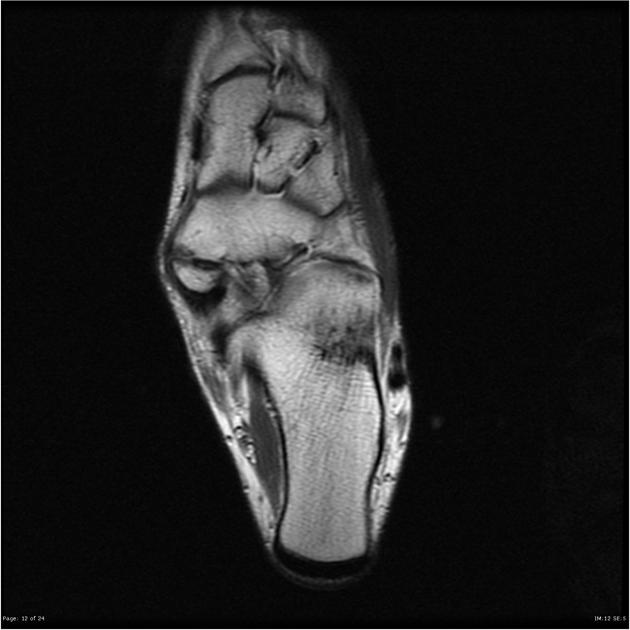
Radiographs show a medial navicular eminence that is best visualized on the lateral-oblique view. Symptomatic accessory navicular bones may appear as a 'hot spot' on bone scan and on MRI bone marrow edema can be seen.
Treatment and prognosis
Acute pain can be managed by corticosteroid injection and immobilization of the foot for 2-3 weeks. For refractory cases, surgical management can be considered.
History and etymology
The accessory navicular bone and first variant of the Geist classification was first described by the Swiss physician Gaspard (Caspar) Bauhin in 1605 6,7 the second variation by the German anatomist and pathologist Hubert von Luschka in 1858 7, and the last variant, as well as the classification itself, were described by the American orthopedic surgeon Emil Geist in 1914 7,10.









 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.