Asthma is a relatively common condition that is characterized by at least partially reversible inflammation of the airways and reversible airway obstruction due to airway hyperreactivity. It can be acute, subacute or chronic.
On this page:
Epidemiology
Asthma is one of the most common chronic diseases in the world. According to the 2022 Global Asthma Report, it is estimated that around 262 million people in the world have asthma 17 and the estimated mean prevalence of clinical asthma in the UK is 18.2% 18.
Asthma may occur at any age, but most patients with asthma experience their first symptoms before the age of 5 years old.
In some patients this may precipitate at a later age - see late onset asthma
Associations
Clinical presentation
The classical symptoms of asthma are wheeze, shortness of breath, chest tightness or difficulty breathing and cough. These symptoms are typically variable and can be absent for long periods of time, with possible episodic exacerbations often triggered by factors such as exercise, allergen or irritant exposure, cold air or viral respiratory infections.
The diagnosis of asthma is clinical and relies on the recognition of a characteristic pattern or respiratory symptoms and signs in the absence of an alternative explanation. Features that increase the probability of asthma are:
more than one of the following symptoms: wheeze, cough, difficulty breathing and chest tightness
episodic symptoms that are worse at night and in the early morning, and occur in response to certain triggers, e.g. exercise, allergen exposure, cold air
personal history of an atopic disorder or family history of an atopic disorder and/or asthma
widespread wheeze on auscultation
Lung function tests are useful in the evaluation of a patient with asthma to assess the presence, severity and reversibility of the airflow obstruction. On spirometry an FEV1/FEV ratio less than 0.7 confirms obstruction. In asthmatic patients, there is usually a large bronchodilator response (typically an increase of at least 12-15% in FEV1) 3, and it is also typically an abnormally high variability of the peak expiratory flow. A normal spirometry, particularly if performed when the patient is asymptomatic, does not exclude the diagnosis of asthma.
Additional investigations such as tests of atopy (blood eosinophil count, serum IgE and allergen skin prick tests) may be of value in selected patients.
Pathology
Etiology
Inflammation plays a major role in asthma and involves multiple cell types and mediators. The factors that initiate the inflammatory process are complex and still under investigation. Genetic factors (such as cytokine response profiles) and environmental exposures (such as allergens, pollution, infections, microbes, stress) at a crucial time in the development of the immune system are known to be involved.
Location
It mainly involves the medium-sized and small bronchi 6.
Subtypes
Microscopic appearance
Asthma is histologically characterized by the presence of chronic inflammation of the airways. The bronchi are thickened by a combination of edema, bronchial wall smooth muscle hyperplasia and an increase in the size of the mucous glands associated with the airways. Crystalline granules called Charcot-Leyden crystals form in eosinophils. Spiral-shaped mucous plugs (Curschmann's spirals) are seen in the sputum 15.
Radiographic features
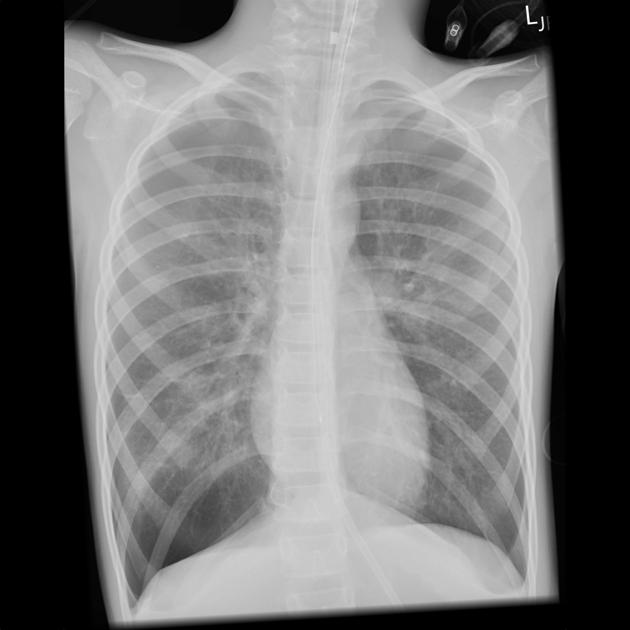
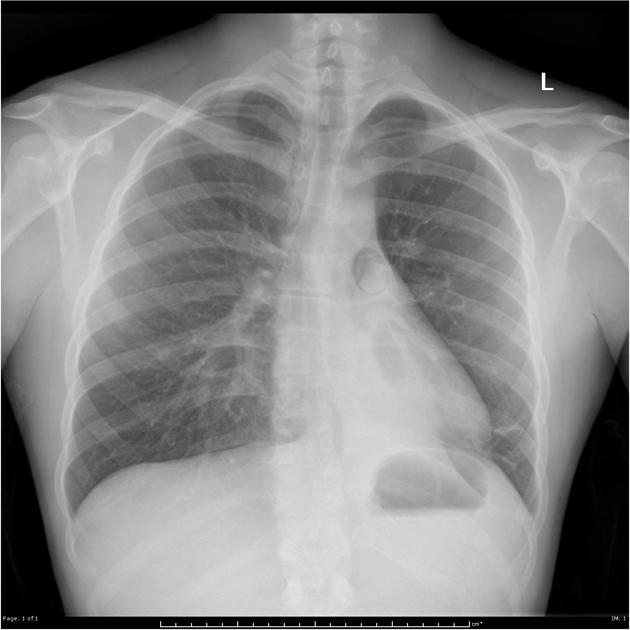
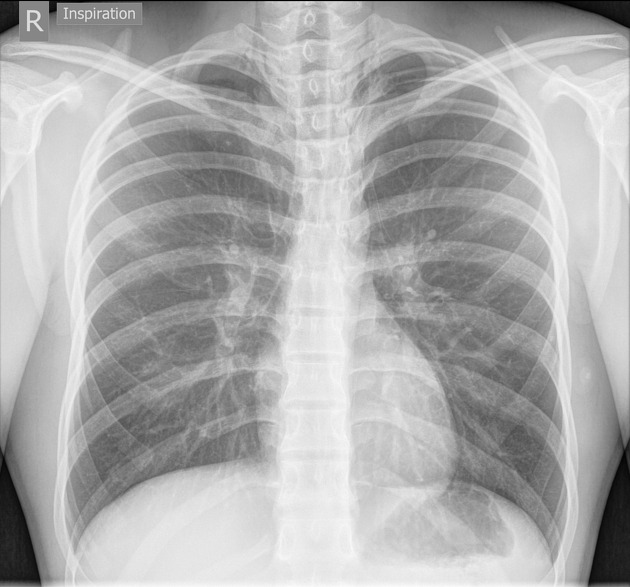
Plain radiograph
Plain chest radiographs can be normal in up to 75% of patients with asthma.
Reported features of asthma include:
bronchial wall thickening: peribronchial cuffing (non-specific finding but may be present in ~48% of cases with asthma 1)
pulmonary edema (rare): pulmonary edema due to asthma (usually occurs with acute asthma)
CT
CT is usually used to detect the presence of complicated associated conditions such as allergic bronchopulmonary aspergillosis (ABPA) and not to directly diagnose asthma.
Reported HRCT features of asthma are non-specific as individual features, they include 2:
expiratory air trapping
inspiratory decreased lung attenuation
small centrilobular opacities 6,8
bronchial luminal narrowing: reduced bronchoarterial-diameter ratio 7
subsegmental bronchiectasis: may be present in ~28-62% of asthmatics 8,12
Treatment and prognosis
The goal of the treatment is to control the symptoms, prevent exacerbations and loss of lung function and reduce associated mortality.
Drugs used to control asthma depend on the severity of the disease. Short-acting β2-agonists can be used in patients with mild occasional symptoms. Inhaled steroids (oral steroids might be required in severe cases) and long-acting β2-agonists can be used for long-term control. Oxygen, short-acting β2-agonists, inhaled anticholinergics and systemic steroids are used in acute exacerbations.
Mechanical ventilation may be necessary for severe exacerbations that do not respond to medical treatment. Non-pharmacological measures, such as smoking cessation and avoidance of occupational sensitizers, are also important.
Asthma is a disease with variable progression and severity of symptoms over time. The prognosis depends on the severity of the disease and the degree of control with treatment. Some patients can be symptom-free for long periods, whereas a few patients with severe persistent asthma develop progressive loss of lung function. Death due to asthma is very rare.
Complications
There are several conditions that can complicate asthma; they include 1,6,16:
pneumomediastinum and related subcutaneous emphysema
syndrome of inappropriate antidiuretic hormone secretion (SIADH) 20





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.