Gunshot injuries are a type of penetrating trauma that often require imaging assessment, and this evaluation has both clinical relevance (assessment of organ damage, surgical planning, and prognostication), and often also forensic implications.
For a more detailed description of ballistics, see fundamentals of ballistics.
On this page:
Epidemiology
Incidence of gunshot injuries to the head is increasing in some countries, due to the ease of accessibility to firearms. In the civilian population, suicide and criminal activity account for the majority of cases and young male adults remain the most at risk 8.
Pathology
Mechanism
Some understanding of the factors that influence wounding capacity and pattern of injury may aid in imaging assessment. The main contributing factors are the type of firearm and projectile characteristics, and the inherent characteristics of the wounded tissues.
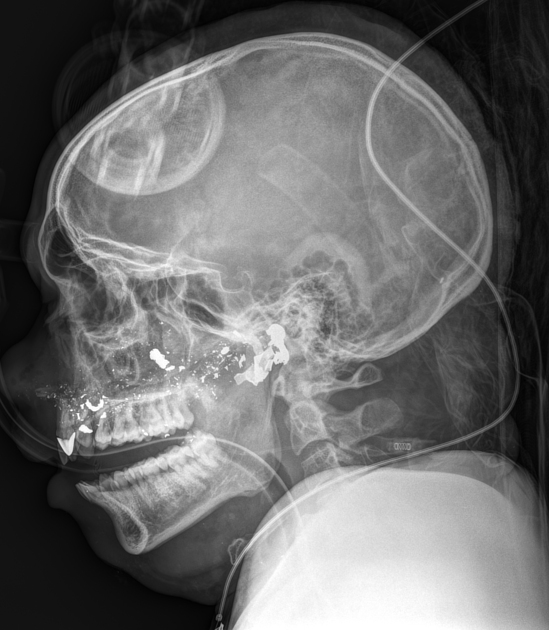
There are five major gunshot injuries of the head 8:
penetrating: entry wound with no exit would
perforating: entry and exit wound with tract through the brain parenchyma
tangential: strikes the head obliquely without penetrating the brain parenchyma but may result in scalp injury, skull fractures or parenchymal contusions
ricochet: penetrating projectile that bounces off the inner table of the skull
careening: penetrates the skull and travels with its trajectory external to the parenchyma potentially injuring the dural venous sinuses
Type of firearm
The type of firearm influences the velocity of the projectile and given that kinetic energy is proportion to mass and velocity (Ek = 0.5mv2), projectile velocity is a major contributor to the energy imparted to tissues and hence, to wounding capacity.
The most common weapons encountered in a civilian setting are 1:
rifles: highest velocity injuries (because longer barrel means that the bullet has more time to accelerate)
handguns: medium to low-velocity injuries
-
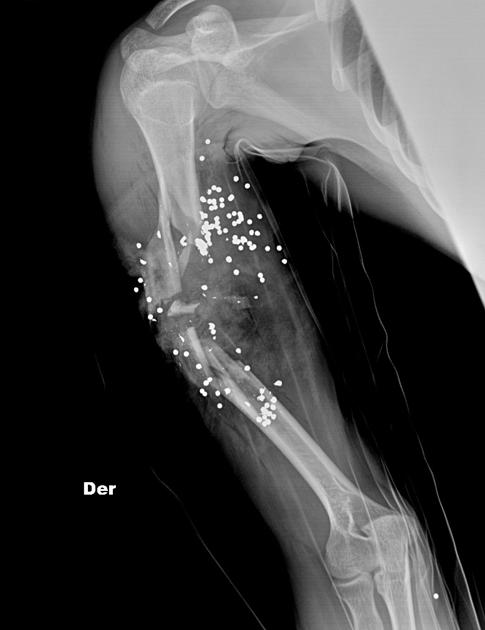
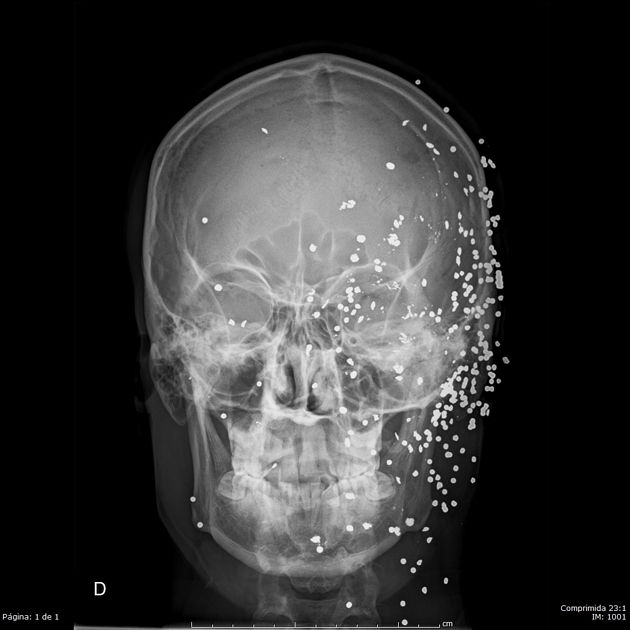
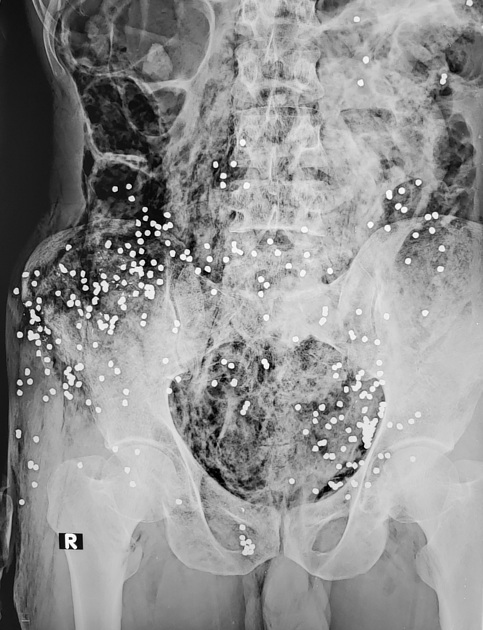
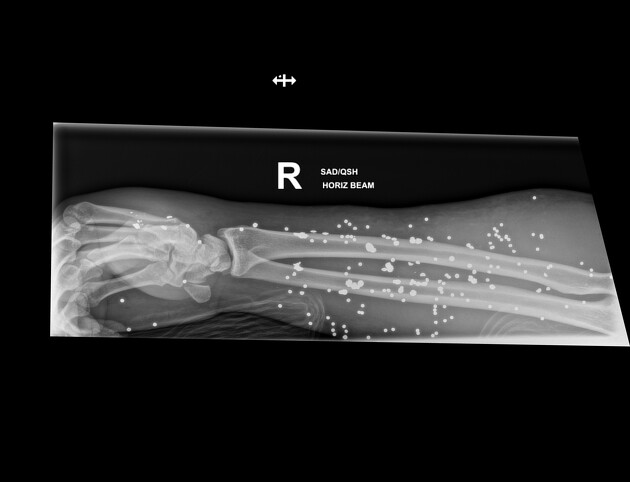
shotguns: have a different mechanism of injury altogether
whereas a rifle or handgun fires a single bullet with each shot, a shotgun fires a cartridge of pellets, which disperse on leaving the barrel and rapidly decelerate
this means that at long range, shotgun injuries are often multiple but superficial, and rarely life-threatening
however, at short range, the combined energy of the pellets can lead to devastating injury, far more severe than from a bullet fired at the same range
Projectile characteristics
These characteristics of bullet behavior have a significant impact on wounding capacity 1:
-
deformation
encased (jacketed) bullets used in higher velocity firearms tend to deform (“mushroom”) on impact
a deformed bullet decelerates faster, hence increasing local tissue damage
-
tumbling
when a bullet hits its target, it loses its directional stability and can rotate around its short axis; for this reason, non-deformed bullets may sometimes be seen pointing towards the entry wound
-
fragmentation
generally, occurs on the impact of a non-jacketed or semi-jacketed bullet
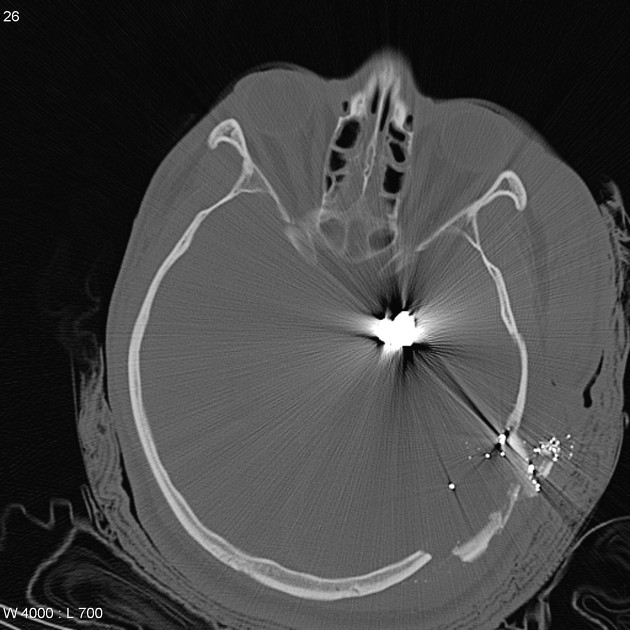
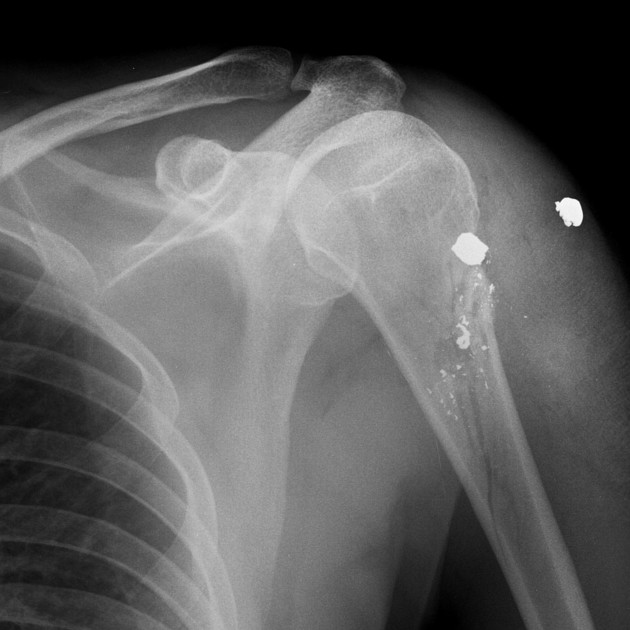
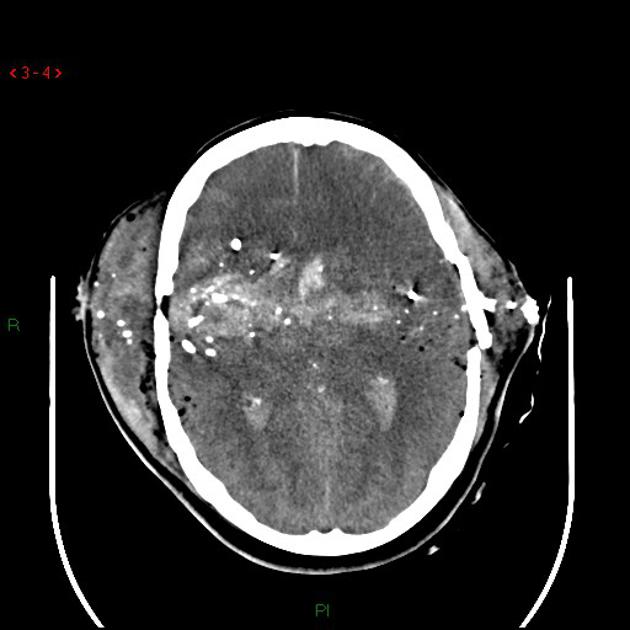
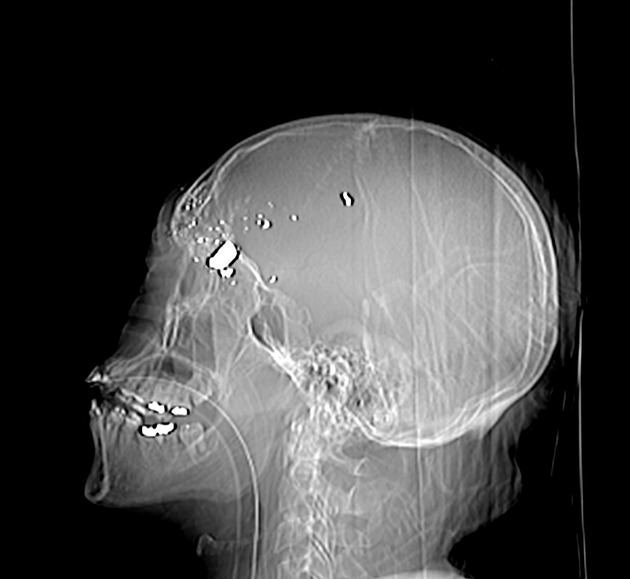
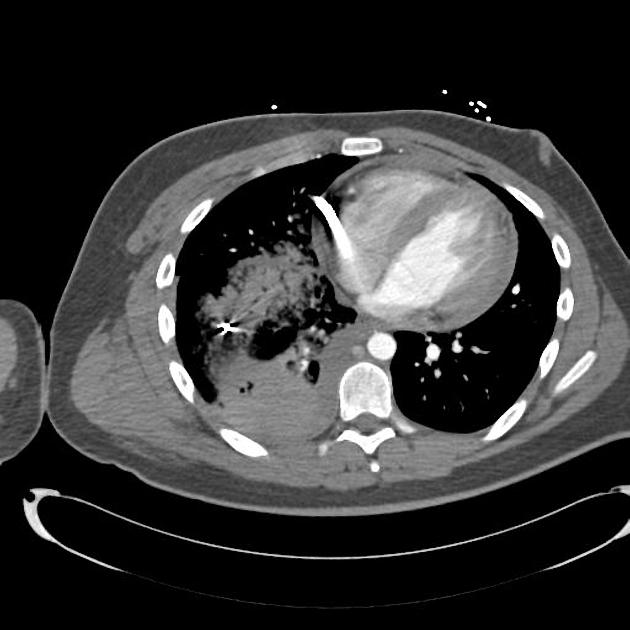
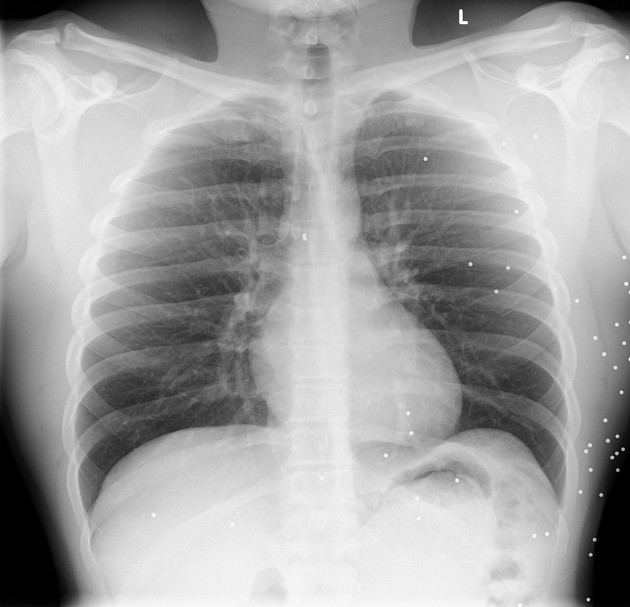
fragmentation often leads to a telltale distribution of fragments spreading along the bullet course, with the most markedly fragmented and widely distributed pattern from high-velocity rifle rounds being called the "lead snowstorm" 1
fragmentation gives important information about the mechanism and direction of injury
Caliber and weight also have some effect on wounding capacity, though not as much as the above factors.
Tissue characteristics
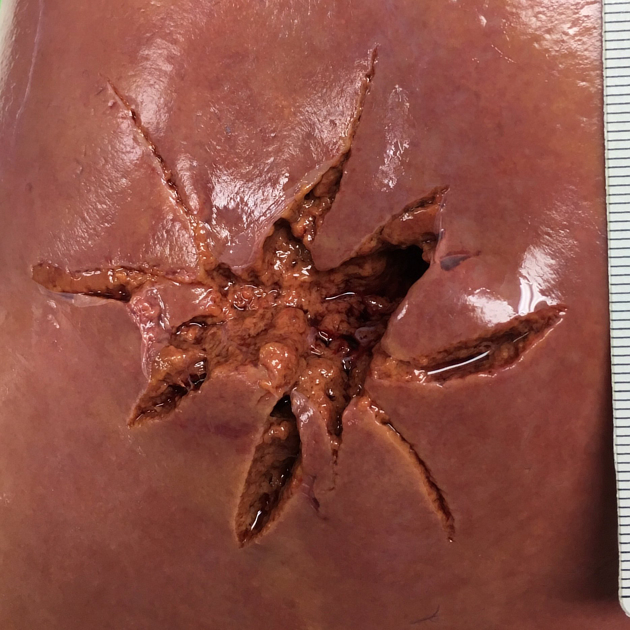
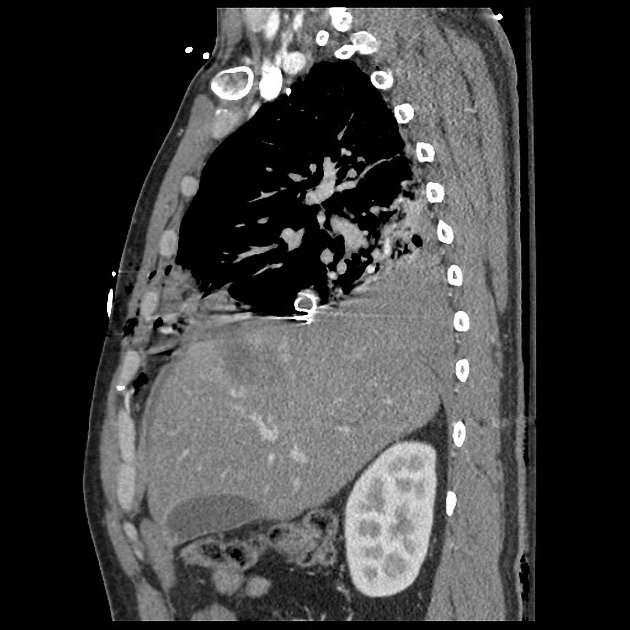
Bullet injury is more severe in friable organs such as liver and brain due to temporary cavitation at a distance from the bullet path. Both dense (e.g. bone) and loose tissues (e.g. subcutaneous fat) are more resistant to damage. Bone can significantly alter the behavior of the projectile and its wounding capacity by slowing it down and changing its path.
Radiographic features
Imaging assessment of a gunshot injury includes:
-
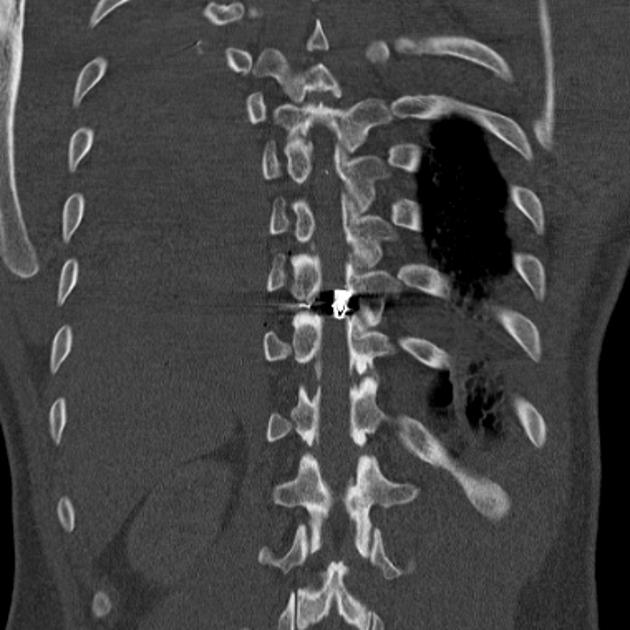
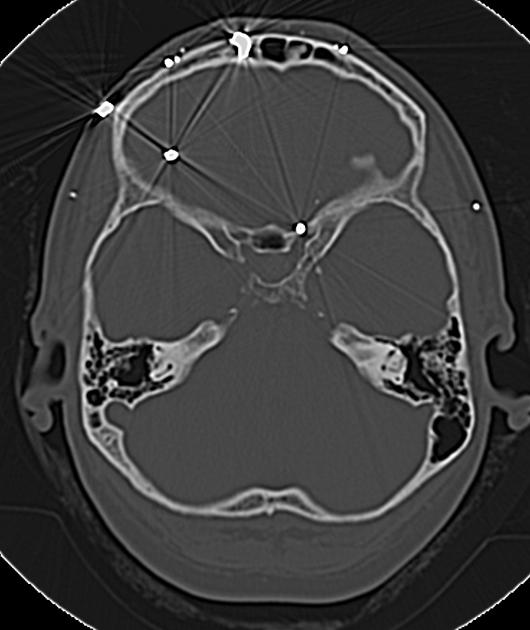
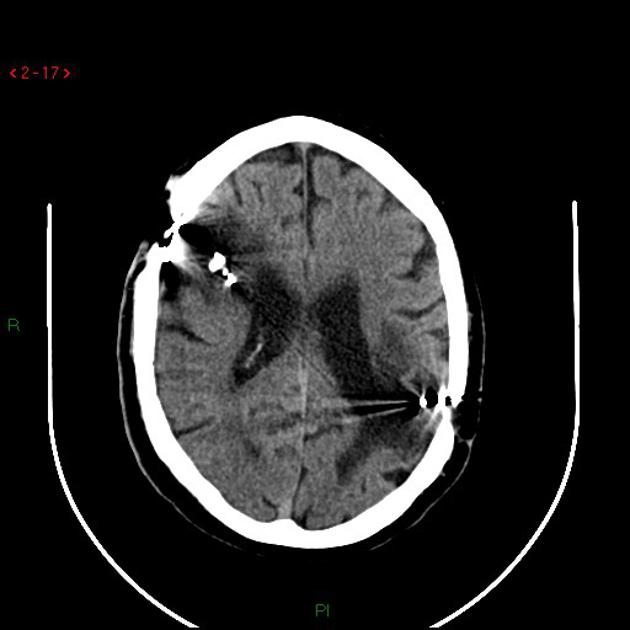
identification of wound tracks by the presence of gas, hemorrhage, bone or metal in a linear distribution
directionality of fragments and bevelling of the bone toward the direction of travel may establish bullet path and help differentiate entry vs exit wound 1
-
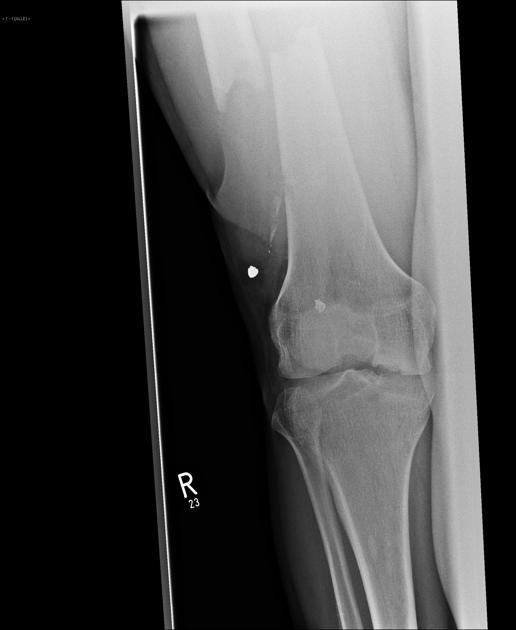
localization of projectile: orientation (tumbling) and fragments
final location may be at a distance from the entry wound due to the tracking of bullets along with soft tissue layers, or deflection by anatomical structures (e.g. bone) - such tracking suggests low-velocity injury
-
if a projectile is not identified on available imaging, a search must be made for
an exit wound
projectile outside the field of view (i.e. may need further imaging)
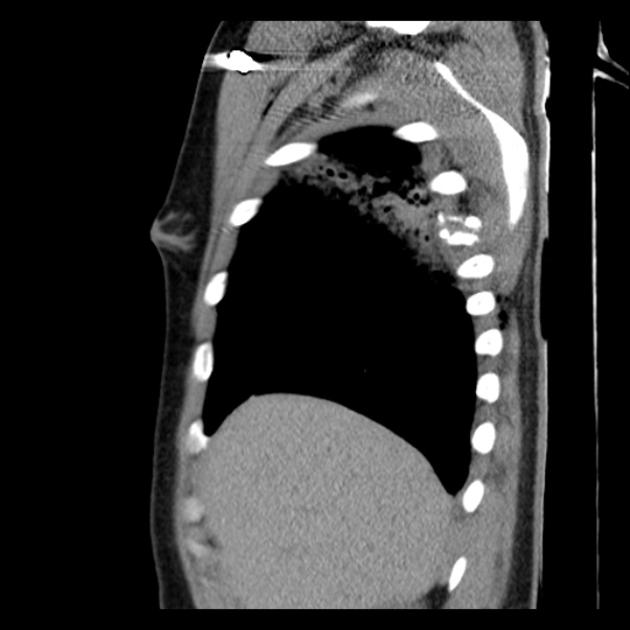
assessment of internal injuries including involvement of critical structures, active hemorrhage, etc.
consider the possibility of embolized fragments/shot pellets
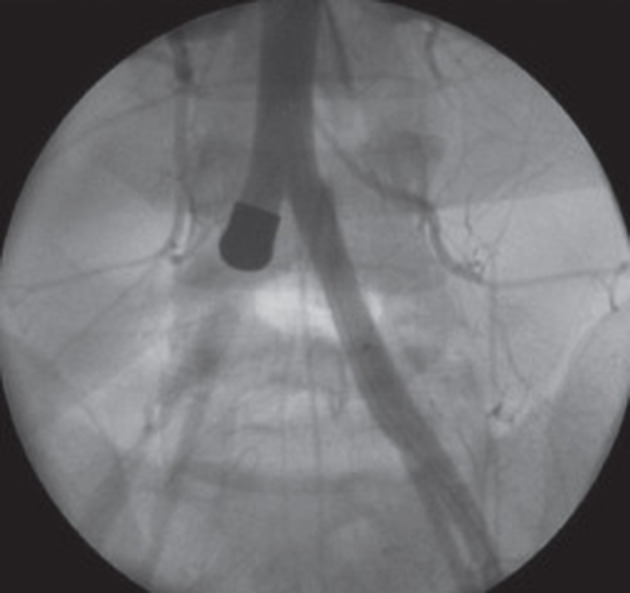
Angiography (DSA)
May be useful for diagnosis, hemostasis and infrequently the management of embolized fragments.
MRI
MRI is not generally necessary (and potentially hazardous) in the evaluation of acute gunshot injuries.
MRI has relevance to this topic mostly because in a patient referred for an MR scan, a history of previous gunshot injury raises safety considerations. The primary consideration relates to the potential for fragment displacement by the magnetic field 7.
Heating of metallic fragments is also of some concern, but to a lesser extent, and is not considered further in this article.
Factors that influence the risk of projectile fragment displacement include:
ferromagnetic properties of the projectile
size and shape of the fragment
location in the body
duration of implantation
strength of the magnet
In general, most bullet fragments that may be encountered in a civilian setting are not ferromagnetic. There are however exceptions, including retained shrapnel in war veterans, certain types of shotgun pellets (especially those used for duck hunting in the United States) and some bullet jackets.
Careful consideration of risk-benefit is therefore recommended in all patients with previous gunshot injuries, particularly if the fragments are adjacent to or within vital structures 6.









 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.