Intra-aortic balloon pumps (IABP) are used in the intensive care setting to provide hemodynamic assistance to patients in cardiogenic shock.
On this page:
Function and physiology
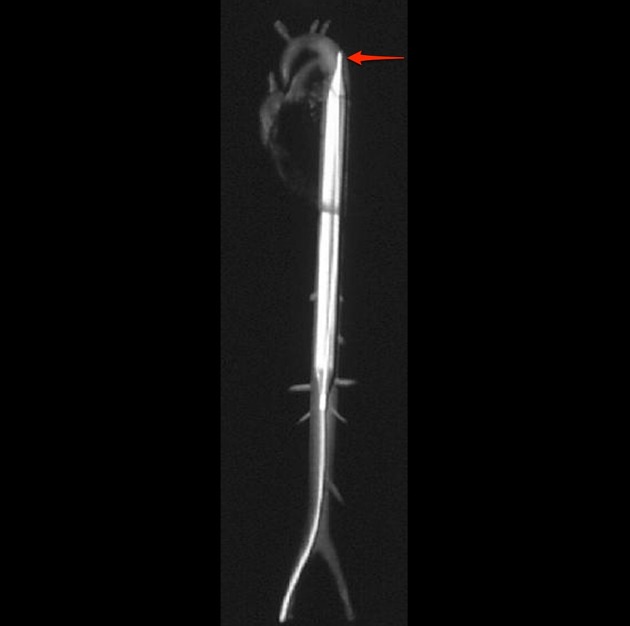
The device is comprised of a catheter introduced via a femoral artery sheath, which extends retrogradely to the proximal descending thoracic aorta. A balloon is located at the end of the catheter, spanning 26-28 cm in length, which is rapidly inflated at the beginning of diastole and rapidly deflated at the end of diastole. The balloon is inflated with helium.
As the balloon forcibly inflates it displaces blood both forwards and backward, known as diastolic augmentation. As such it provides not only additional forward momentum to the blood in the distal descending aorta but more importantly increases perfusion to the vessels arising from the aortic arch and ascending aorta, most importantly the coronary arteries which are perfused primarily during diastole 1,2.
This has a dual effect: it firstly decreases left ventricular afterload through a vacuum effect, decreasing myocardial oxygen requirements, and secondly increases myocardial perfusion (during diastole) 1,2.
Radiographic features
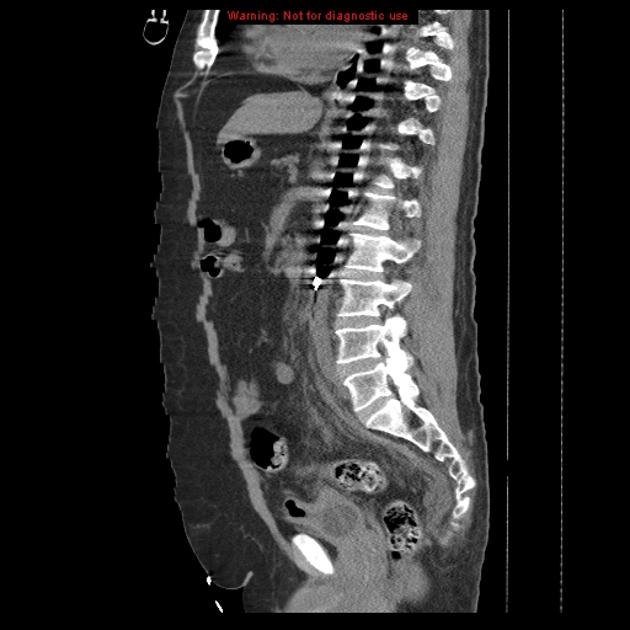
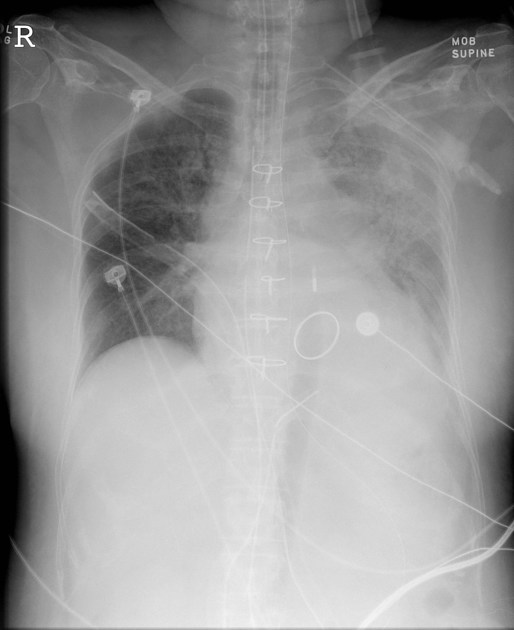
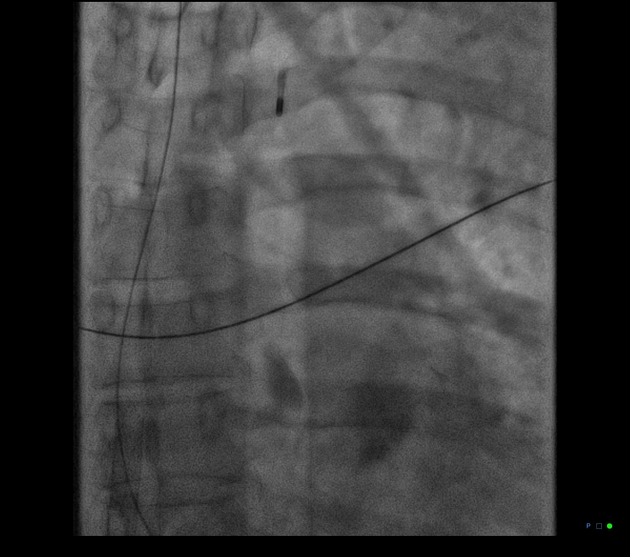
Some catheters are radiolucent except for a distal radiopaque marker. If the film is obtained during diastole then the balloon can be seen as a radiolucent oblong aligned with the thoracic aorta 1.
The balloon should be located in the proximal descending aorta, just below the origin of the left subclavian artery. On a chest radiograph, it should be at the level of the AP window. This ideally results in the balloon terminating just above the splanchnic vessels 3.
Complications
Complications may occur in around 30% of cases 4 and can be divided into those relating to balloon function and those related to balloon positioning.
-
malpositioning: considered the commonest complication
aortic dissection (1%) 4 or large vessel arterial dissection during insertion
too high (case 6): obstruction of the left subclavian artery
too low (case 7): obstruction of the splanchnic arteries
-
function
platelet and red blood cell destruction
distal embolization (this can be to the brain if the positioning is too proximal), including from thrombosis at the insertion site or from helium embolus in the case of balloon rupture 5
Additionally, the catheter is quite large and the resultant common femoral artery defect can be difficult to close with routine compression. This may result in formation of a false aneurysm.










 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.