Seminal vesicle invasion (SVI) is referred to as the secondary involvement of the seminal vesicles and ductus deferens by neoplasms not originating from the seminal vesicles themselves and are much more common than their primary counterparts. Involvement of the seminal vesicles stages prostate cancer as T3b of the TNM staging system.
On this page:
Terminology
Seminal vesicle invasion refers to a tumor infiltrate originating from external tumor cells, in a broader sense seminal vesicle infiltration can also be due to inflammation.
Epidemiology
By far the most common tumor, leading to seminal vesicle invasion, is prostate cancer 1-3. On much rarer occasions other tumors, e.g. bladder cancer, rectal cancer can lead to seminal vesicle invasion 1. The incidence of seminal vesicle invasion of prostate cancer has been reported to be around 10% 4.
Associations
Seminal vesicle invasion is commonly associated with and considered a form of extraprostatic extension of prostate cancer 3.
Clinical presentation
Symptoms of seminal vesicle invasion are very unspecific, hematospermia might be a clinical symptom that could be indicative of seminal vesicle invasion, e.g. in the proper clinical context of prostate cancer, but can also occur in many innocuous conditions 1.
As for prostate cancer, clinical nomograms for the prediction of seminal vesical invasion have been developed, including the following parameters 5,6:
- high prostate-specific antigen (PSA)
- presence of prostate cancer in a biopsy core from the base
- high ipsilateral biopsy Gleason grade
- high ipsilateral percentage core involvement
Pathology
The pathological correlate of malignant seminal vesicle invasion is a tumor infiltration of the muscular wall of the seminal vesicles 7.
Subtypes
Different suggested routes or subtypes of seminal vesicle invasion have been described. For prostate cancer, they include the following 1,2:
- tumor extension through the ejaculatory ducts
- direct spread or tumor extension, e.g. from the prostatic base or from the adjacent fatty tissue
- isolated tumor deposits
Radiographic features
General imaging features of seminal vesicle invasion include the following 1-3,8:
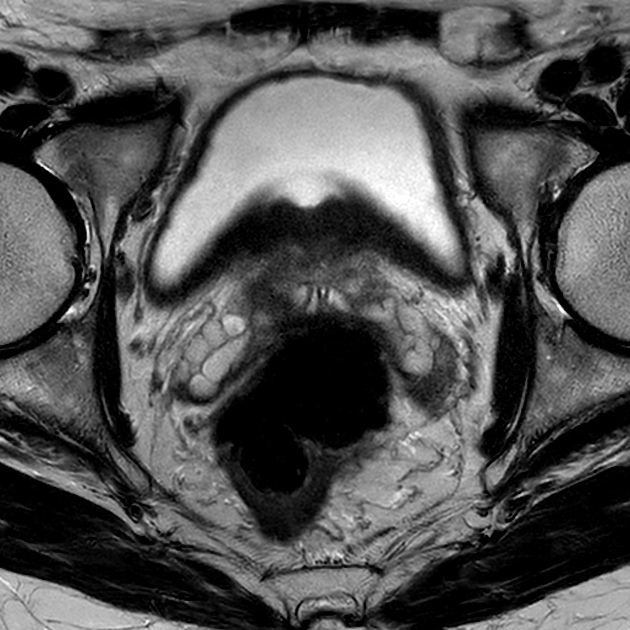
- seminal vesicle enlargement or mass
- loss of the normal seminal vesicle architecture
- irregular seminal vesicle boundaries and infiltration of the adjacent fat planes
- loss of the prostate-seminal vesicle angle
Ultrasound
Ultrasound might reveal a mass extending into the seminal vesicles or show loss of the prostate-seminal vesicle angle 1.
CT
Similar to ultrasound, CT might reveal a soft tissue density mass extending into one of the seminal vesicles and/or obliteration of the angle prostate-seminal vesicle angle 1.
MRI
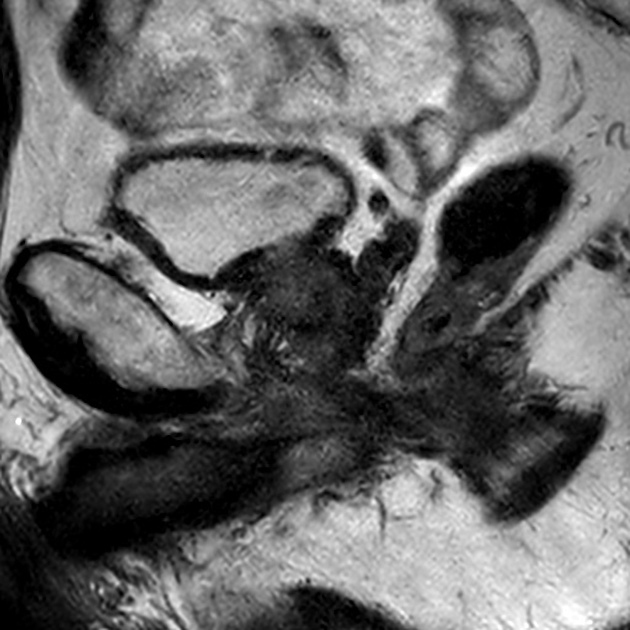
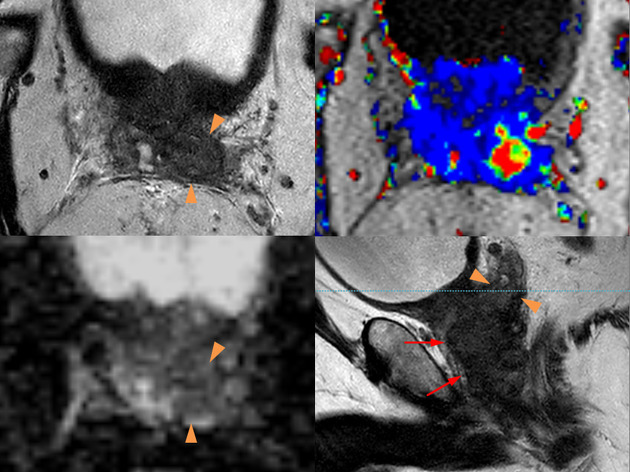
The most accurate imaging modality for the assessment of seminal vesicle invasion is MRI 1-3,8. Sensitivities and specificities have been reported in the range of 45%-71% and 66%-95% 1-3. Apart from the above-mentioned findings, MRI features include tumor infiltration or focal tumor deposits with the following signal characteristics 1,2:
Signal characteristics
-
T2
- focal low signal intensity areas
- loss of the interface to the adjacent seminal vesicle walls
-
T1
- iso to hypointense
- no corresponding high signal intensity
-
DWI
- diffusion restriction with high intensity on >b1000 images
- low ADC values
- DCE (Gd): focal or nodular or irregular wall enhancement with fast wash-in similar to prostatic lesions
Radiology report
The radiological report should include a description of the following:
- direct signs of seminal vesicle invasion
- route of infiltration (ejaculatory ducts, direct extension, tumor deposits)
- location of infiltration (proximal/distal part)
- statement on which seminal vesicle or if both are involved
- primary tumor location (e.g. base of the prostate)
Treatment and prognosis
Seminal vesicle invasion defines the T3b stage of the TNM staging system of prostate cancer.
The mainstay in management in that situation is hypofractionated radiotherapy with image-guided intensity-modulated radiotherapy (IMRT) or conventional radiotherapy if the first is not possible. In addition, the patient should receive androgen deprivation therapy. Combination with brachytherapy as well as chemotherapy with docetaxel might be considered 4,9.
As for bladder and rectal cancer seminal vesicle invasion equates to T4a and T4b stage respectively.
Differential diagnosis
Conditions that can mimic the presentation and/or the appearance of seminal vesicle invasion include 1:
- hemorrhage
- seminal vesiculitis
- primary neoplasms
- adenocarcinoma/squamous cell carcinoma
- tumors of mesenchymal origin e.g. leiomyoma
- lymphoma
Practical points
Similar to the assessment of the standard prostate best diagnostic clues can be retrieved from the evaluation of high-resolution T2 weighted and diffusion-weighted images. Dynamic contrast enhancement can confirm the finding but is of very limited additional value to native imaging 2.





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.