Trigeminal neuralgia, also known as tic douloureux, corresponds to a clinical manifestation of sudden severe paroxysms of excruciating pain on one side of the face which usually lasts a few seconds to a few minutes, involving one or more branches of the trigeminal nerve (CN V). Neurovascular compression is the most prevalent cause. Other causes include compression due to cerebellopontine angle (CPA) tumors or cysts, perineural tumor spread, and multiple sclerosis.
On this page:
Epidemiology
The incidence of trigeminal neuralgia is approximately 4.3 per 100,000 per annum. The vast majority of cases are unilateral, with the right side of the face being affected more commonly (1.5:1); around 3% are bilateral. It peaks around age 60 to 70 years, and its prevalence increases with age 1,4.
Clinical presentation
Trigeminal neuralgia tends to present as attacks of sudden shock-like excruciating pain, which usually lasts a few seconds to about two minutes and most often involves the maxillary division. The pain is typically triggered by trivial stimuli such as talking, drinking, brushing teeth, shaving, chewing, or touching the face. However, it may also occur spontaneously 1.
Although the diagnosis of trigeminal neuralgia is almost entirely based on history, some warning signs should prompt further investigation 4:
patients under 40 years
difficulty in achieving pain control
poor response to carbamazepine
a history of any skin lesions or oral lesions that could lead to perineural spread or malignancy
associated sensory changes, deafness or other ear problems
when affecting only the ophthalmic division or when bilateral, it is suggestive of benign or malignant lesions or multiple sclerosis
concurrent or prior optic neuritis, again suggestive of multiple sclerosis
Diagnostic critera
The clinical diagnostic criteria for trigeminal neuralgia are defined by the IASP (International Association for the Study of Pain) and the ICHD/IHS (International Classification of Headache Disorders / International Headache Society) as:
paroxysmal attacks of pain lasting from a fraction of a second to two minutes, affecting one or more divisions of the trigeminal nerve
-
the pain exhibits at least one of the following characteristics:
intense, sudden, superficial or stabbing
precipitated by trigger factors or trigger areas
attacks are similar among patients
no neurological disorder is clinically evident
not attributed to another disorder, e.g. periapical dental inflammation 10
Note that if autonomic symptoms are prominent (e.g. lacrimation), the condition more likely represents a trigeminal autonomic cephalgia, such as short-lasting unilateral neuralgiform headache with cranial autonomic symptoms (SUNA) or short-lasting unilateral neuralgiform headache attacks with conjunctival injection and tearing (SUNCT).
Pathology
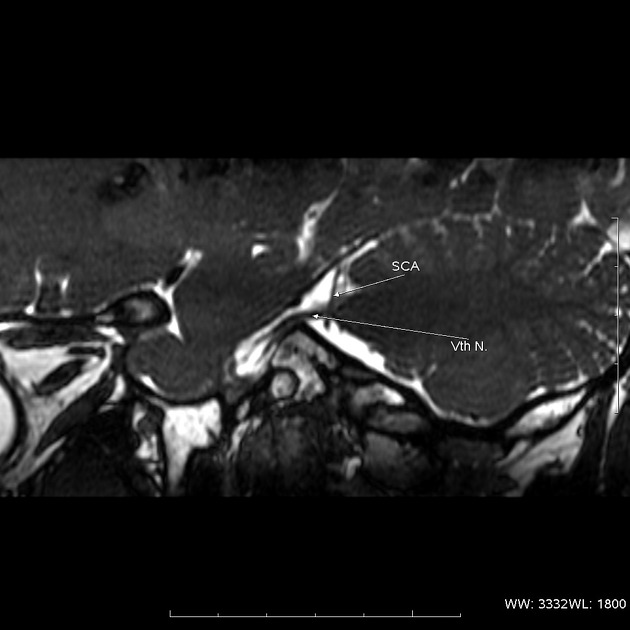
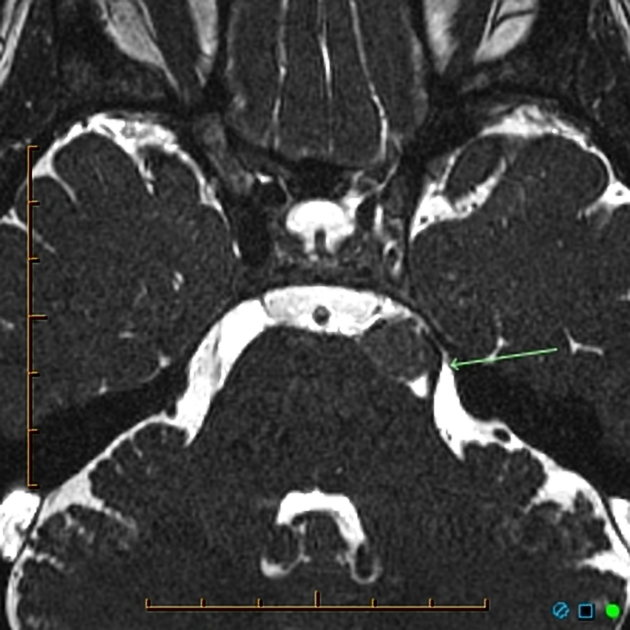
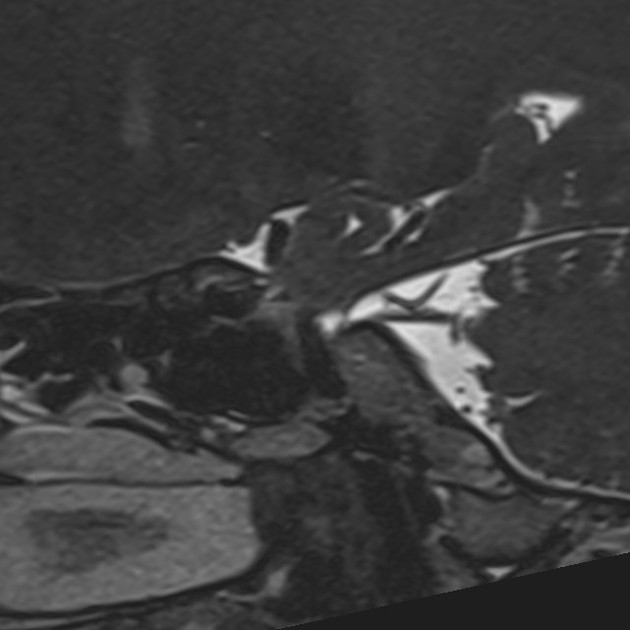
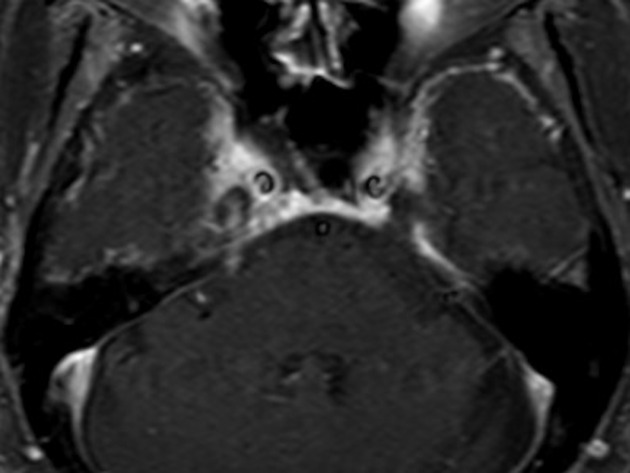
The most common cause of trigeminal neuralgia is a compressing loop of an artery (most commonly the superior cerebellar artery) or vein (most commonly the transverse pontine vein) compressing the cisternal portion of the trigeminal nerve at its transition zone 2.
The site where the nerve exits the brainstem is known as the nerve root entry zone. Typically 3-4 mm distal to this, oligodendrocytes, that supply insulating myelin to the nerve fibers, give way to Schwann cells. This is known as the transition zone and measures approximately 2 mm in length 11. The proximal cisternal portion, especially the transition zone, is far more vulnerable than any other part of the nerve 11. The reason for this, however, is not well understood. Histologically, there is associated demyelination of the compressed nerve in some cases 6.
Although rare, posterior fossa tumors can be another cause, most commonly vestibular schwannomas, meningiomas, arachnoid cysts, or epidermoid cysts 4.
Multiple sclerosis may also cause trigeminal neuralgia and, indeed, its incidence is much higher in multiple sclerosis patients than in the general population. It is thought that both pontine plaques and neurovascular compression in combination produce a "double-crush" mechanism whereby intra-pontine inflammatory demyelination and cisternal mechanical demyelination affect the same first-order neurons 20. Of interest, high T2/FLAIR signal of the intrapontine segment of the trigeminal nerve is encountered in approximately 5% of cases, often symetrically 23. The etiology of this is unclear as is whether this finding increases the likelihood of trigeminal neuralgia 23.
Radiographic features
The diagnosis of trigeminal neuralgia is based on the patient's history. Imaging is helpful in identifying trigeminal neuralgia secondary to another pathology (e.g. multiple sclerosis or tumors) as well as helping in planning for decompressive surgery.
MRI with high resolution T2 weighted imaging is the imaging modality of choice 3. CT is limited in evaluating the brainstem and the cisterns although if MRI is contraindicated, a CT cisternogram can outline the trigeminal nerves and cisternal vessels.
MRI
MRI studies should accomplish the two primary goals of imaging:
identify and quantify neurovascular compression
assess for other causes of trigeminal neuralgia
Assessing neurovascular compression
The literature is heterogenous with rates of compression varying widely depending on the definitions of contact and which MR sequences were used.
Sequences
On modern scanners, that primary sequence used to assess the anatomy of the cisternal portion of the trigeminal nerves and adjacent vessels is a high-resolution T2 weighted sequence with minimal CSF flow artefact (e.g. CISS, FIESTA, SPACE) 22. This is usually supplemented with time of flight MR angiography which allows for co-registration of arteries in the cisterns with vessels seen on T2 imaging 22. See trigeminal neuralgia protocol.
Grading
Over the years, as imaging has improved, the definition of contact has changed and a variety of terms used including compression, contact, distortion, deformation etc... 22.
Location
Whether the location of contact along the cisternal course of the nerve is relevant, has also been debated in the literature over the years 22. It is believed that the segment of the nerve that is most sensitive to contact is the transition zone between oligodendroglial-derived myelin to Schwann cells. As this cannot be identified on imaging, it is important to mention how far anterior to the trigeminal nerve root entry zone the vessel compressing the nerve is located. The majority of transitional zones extend no further than 3-4 mm anterior to the nerve root entry zone, and this has therefore been suggested as a reasonable cut-off between vessels that are likely symptomatic versus those that are more likely incidental 11.
It should be noted, however, that occasionally compression of the nerve in the anterior cisternal segment can also be symptomatic and many asymptomatic patients have vessels contacting the proximal nerve. As such, it is not possible to dogmatically state whether a vessel is symptomatic or not 11.
Assessing other causes
A trigeminal neuralgia protocol, should include a variety of sequences (FLAIR, T2, T1 pre and post contrast, DWI/ADC) which will depend on local preference and patient demographics. However, an evidence-based review did not find evidence to support or refute the usefulness of MRI for this purpose 5.
Diffusion weighted imaging can be used to assess the cisternal and brainstem components of the nerve and assess ADC values, fractional anisotropy and mean diffusivity, although this not routinely performed 12.
Treatment and prognosis
The initial treatment of trigeminal neuralgia is medical, with drugs such as carbamazepine, oxcarbazepine, lamotrigine, gabapentin, pregabalin or baclofen 21. Botulinum toxin therapy may also be efficacious 21.
Large surgical series have confirmed that microvascular decompression of the trigeminal nerve root is also an efficient and durable treatment for trigeminal neuralgia 4.
Other surgical treatments include:
Gamma Knife radiosurgery focused at the trigeminal root in the posterior fossa
rhizotomies: controlled destruction of the trigeminal ganglion or root by various means - thermal, chemical, or mechanical
trigeminal nerve stimulator: considered "off-label" use (2019) in the USA 9
History and etymology
John Fothergill (1712–1780), an English physician, described a series of fourteen cases of trigeminal neuralgia in a paper in 1773, hence its well-known eponym 14,15,17. Although, it is now thought that the condition had been described in the 2nd century by both the legendary Greek physician Galen (c.129-200) 18 and Aretaeus of Cappadocia 19, and also by Avicenna in the 11th century 14,15.
Practical points
-
presentation
many imaging requests may incorrectly give a history of trigeminal neuralgia when what the patient actually has is trigeminal neuropathy (any symptom attributable to the nerve in contrast to trigeminal neuralgia which has very specific criteria: sudden, severe paroxysmal attacks of pain).
constant, dull, burning pain or paresthesia of the face is not trigeminal neuralgia and would not be expected to relate to neurovascular compression and should instead prompt a search for other pathologies like perineural tumor spread
-
MRI protocol
ideally should include sequences of the face and skull base to enable full assessment of the trigeminal divisions for any pathology, in particular, for perineural tumor spread
whole brain FLAIR images to assess for demyelination as a cause are also recommended
-
approach
a suggested approach is to look for all other causes of trigeminal neuropathy first (CP angle tumors, skull base and face pathology, white matter lesions etc.)
focus on the transisitional zone for neurovascular compression
co-register MRA and thin T2 (e.g. CISS)





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.