Ganglioneuromas are fully differentiated neuronal tumors that do not contain immature elements and potentially occur anywhere along with the peripheral autonomic ganglion sites.
On imaging, usually, they present as well-defined solid masses and can be quite large at presentation. Generally, they are hypoattenuating to muscle on CT and have a heterogeneous intermediate signal on both T1 and T2-weighted MRI sequences. Contrast enhancement ranges from none to heterogeneous enhancement, calcification may be present in less than a quarter of cases.
On this page:
Epidemiology
Ganglioneuromas tend to occur in the pediatric population and are often asymptomatic. At the time of diagnosis, 60% of patients are under the age of 20 years 11. The median age at diagnosis is 7 years, and there is a slight female predominance. This is in contrast to neuroblastoma which occurs in patients younger than 3 years old.
Associations
- multiple endocrine neoplasia type IIb 5,6: particularly with mucosal ganglioneuromas
Clinical presentation
Ganglioneuromas are usually asymptomatic and often discovered incidentally as they are slow growing and usually endocrinologically inactive 11.
Pathology
Like neuroblastomas and ganglioneuroblastomas, ganglioneuromas are derived from the primordial neural crest cells that form the sympathetic nervous system. Pathologically, they are composed of ganglion cells, Schwann cells and fibrous tissue. They do not contain neuroblasts, intermediate cells, or mitotic figures and necrosis is not a feature 12.
Ganglioneuromas most commonly arise in the paravertebral sympathetic chains of the posterior mediastinum (41.5%) or retroperitoneum (37.5%). Less common sites include the adrenal gland (21%) and neck (8%) 12. Paravertebral ganglioneuromas frequently extend through the neural foramina to involve the epidural space of the spinal canal 13. Intradural extramedullary ganglioneuromas have been reported but are extremely rare 10.
Ganglioneuromas may occur de novo or may arise from maturing neuroblastomas and ganglioneuroblastomas. They may also arise in neuroblastomas and ganglioneuroblastomas that have been treated with chemotherapy 12.
There are rare reports of metastatic ganglioneuromas. It is believed that these tumors represent metastases of neuroblastomas or ganglioneuroblastomas that have subsequently matured to ganglioneuromas. These patients have an excellent prognosis 12.
Location
Can potentially occur anywhere along the peripheral autonomic ganglion sites. The posterior paraspinal mediastinum is one of the commonest locations (see paraspinal ganglioneuroma) 2 (~40%). Occurrence in the retroperitoneum, neck and adrenal glands is also relatively common.
Radiographic features
Lesions are well-defined and can be quite large at presentation.
Plain radiograph
On paraspinal ganglioneuromas, in particular, a posterior mediastinal mass may seen causing rib spreading and foraminal erosion. A retroperitoneal mass and scoliosis may also be present.
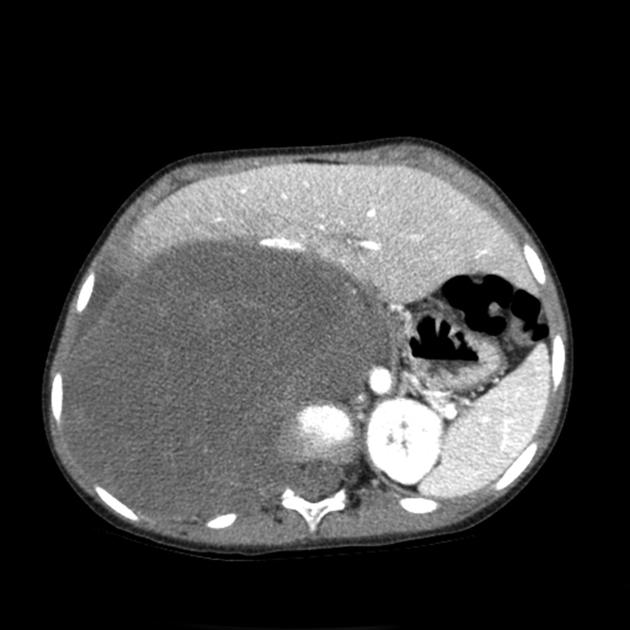
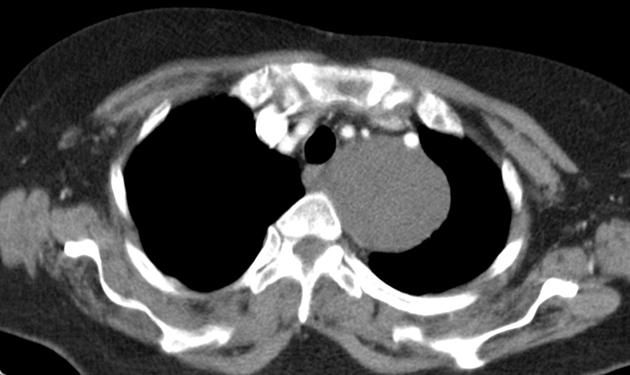
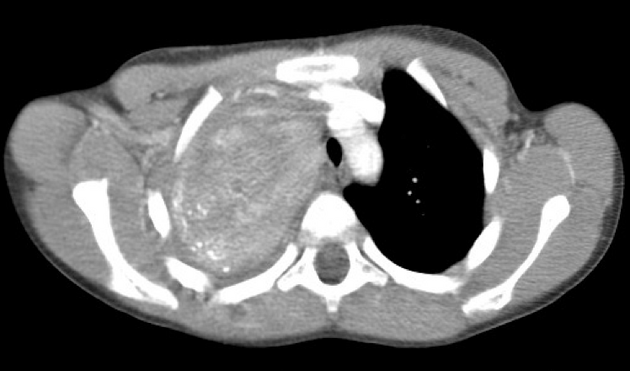
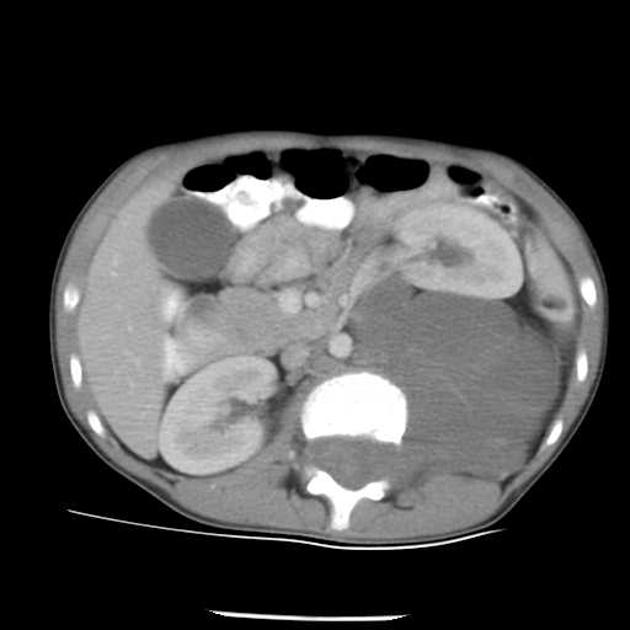
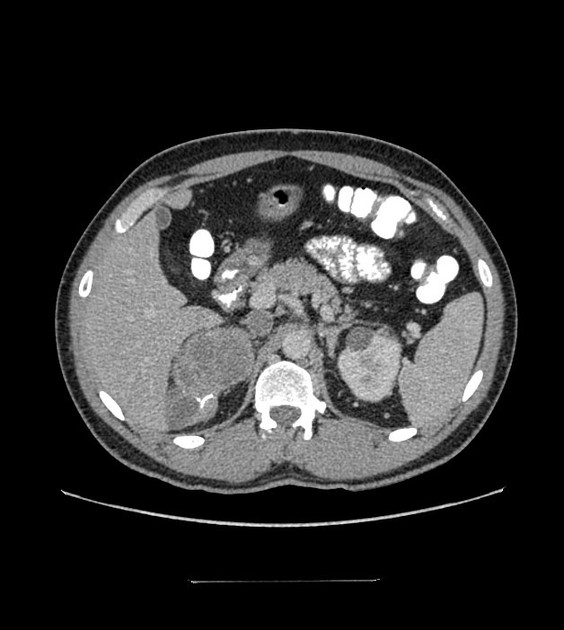
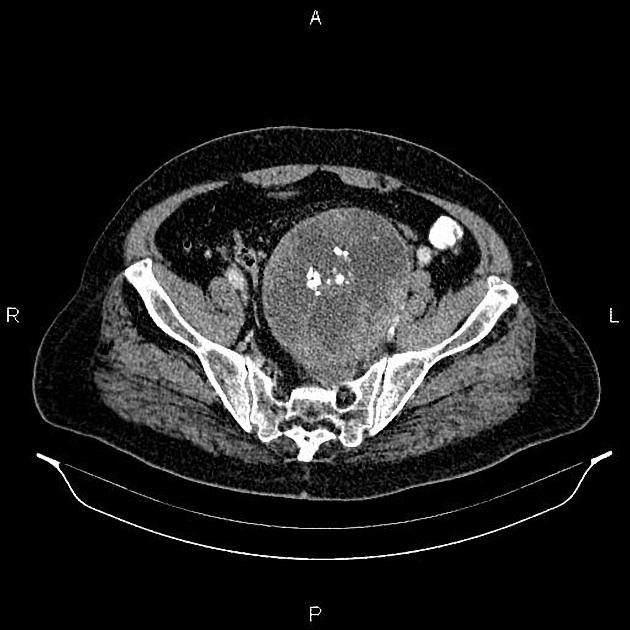
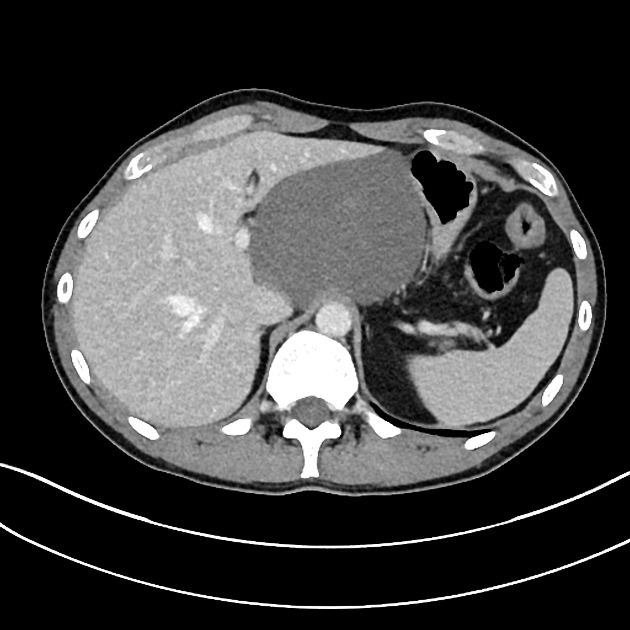
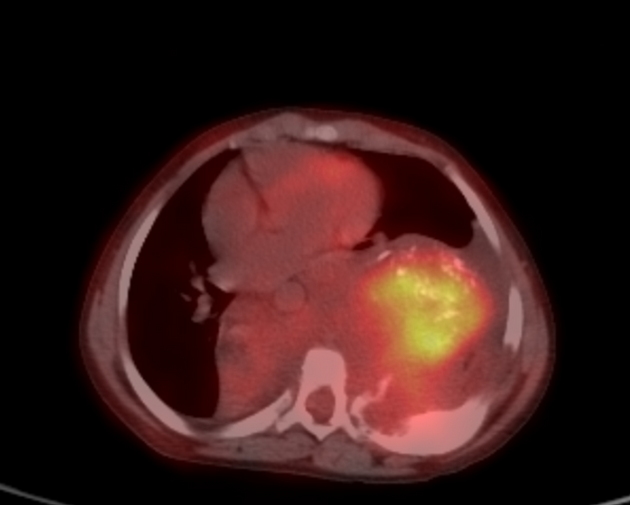
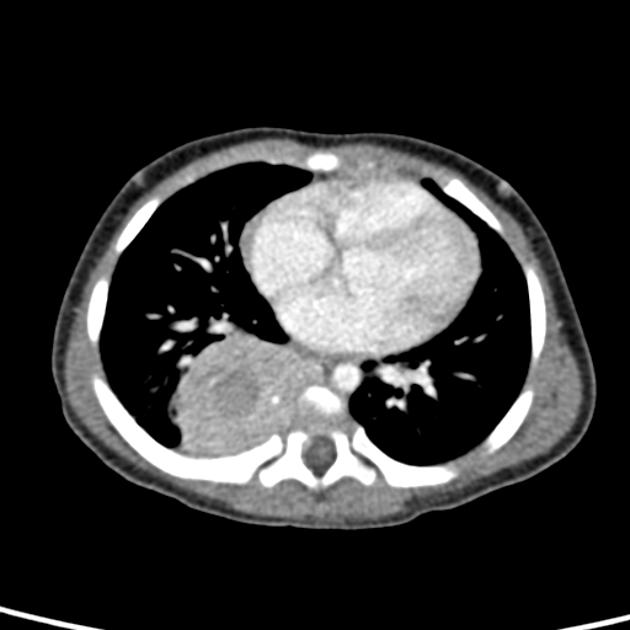
CT
Typically seen as well-circumscribed, solid, encapsulated masses that are iso to hypoattenuating to muscle 8. The lesion may also demonstrate calcifications (~20% 2,4) which are typically fine and speckled but may be coarse.
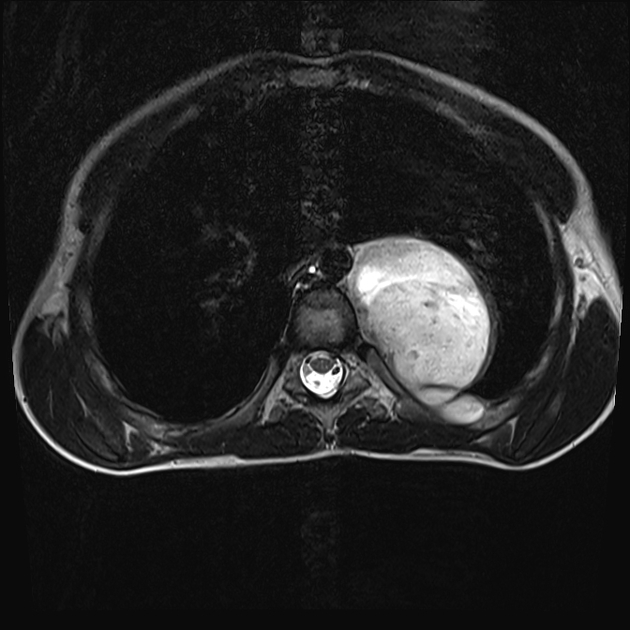
MRI
Ganglioneuromas are well-circumscribed masses. They may appear encapsulated, although a true capsule is infrequent 12. Reported signal characteristics include:
- T1: tends to have homogeneously low or intermediate signal
- T2: tends to have heterogeneously intermediate or high signal
- T1 C+ (Gd): variable ranging from none to heterogeneous enhancement
- ADC: ADC values tend to be higher than that of a neuroblastoma 9
Treatment and prognosis
Ganglioneuromas are typically slow growing tumors.
Treatment consists of complete surgical resection when possible. Complete resection ensures thorough sampling of the tumor so that a confident diagnosis of ganglioneuroma can be made 12.
Prognosis is usually excellent, however, local recurrence has been reported.
Differential diagnosis
The differential depends on location; for thoracic lesions, consider the differential for a posterior mediastinal mass.
Differentials for paraspinal ganglioneuromas include:
- spinal neuroblastoma and ganglioneuroblastoma
- often cannot be differentiated from ganglioneuroma based on imaging characteristics
- metastases usually indicate neuroblastoma or ganglioneuroblastoma
- compared with ganglioneuromas, tumor calcification in neuroblastomas is more common (80-90%) and often amorphous and of a rough pattern
- spinal schwannoma and neurofibroma
- centered on neural foramen
- primarily seen in middle-aged adults







 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.