Schmorl nodes, also known as intravertebral disc herniations, refer to protrusions of the cartilage of the intervertebral disc through the vertebral body endplate and into the adjacent vertebra. The protrusions may contact the marrow of the vertebra, leading to inflammation.
On this page:
Epidemiology
Quiescent Schmorl nodes are extremely common found in around 75% of autopsies, at all ages, more frequently in males 9.
Clinical presentation
Chronic Schmorl nodes are usually asymptomatic, and their etiological significance for back pain is controversial. Acute Schmorl nodes, in contrast, are uncommon and are associated with inflammation and symptoms 9.
Schmorl nodes are among the diagnostic criteria of Scheuermann disease 6. A limbus vertebra is closely related to a Schmorl node as well.
Pathology
It is believed that Schmorl nodes develop following back trauma, although this is incompletely understood. Nucleus pulposus pressure on the weakest part of the endplate or vertebral development process during early life may be a possible explanation 7.
Radiographic features
In the acute stage, Schmorl nodes can be difficult to diagnose on plain radiography or detect due to sclerosis around the margin of the herniation not having had time to develop.
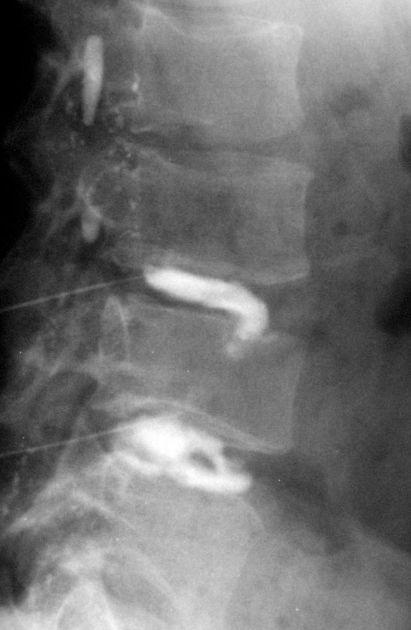
Plain radiograph
Usually, they are small nodular lucent lesions involving the inferior endplate of lower thoracic and lumbar vertebral bodies. However, the involvement of both the inferior and the superior endplates is not uncommon. A sclerotic margin may be present.
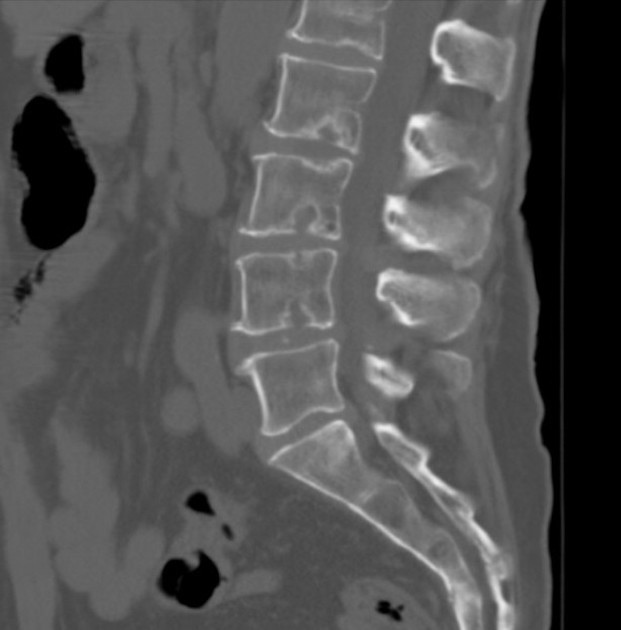
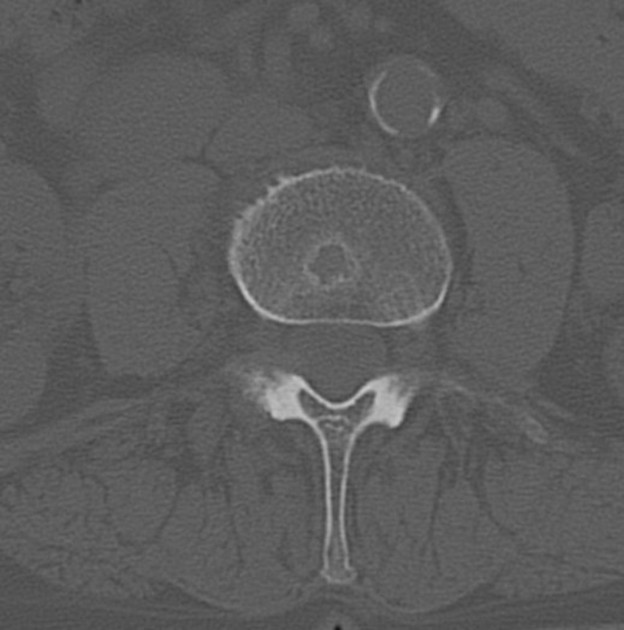
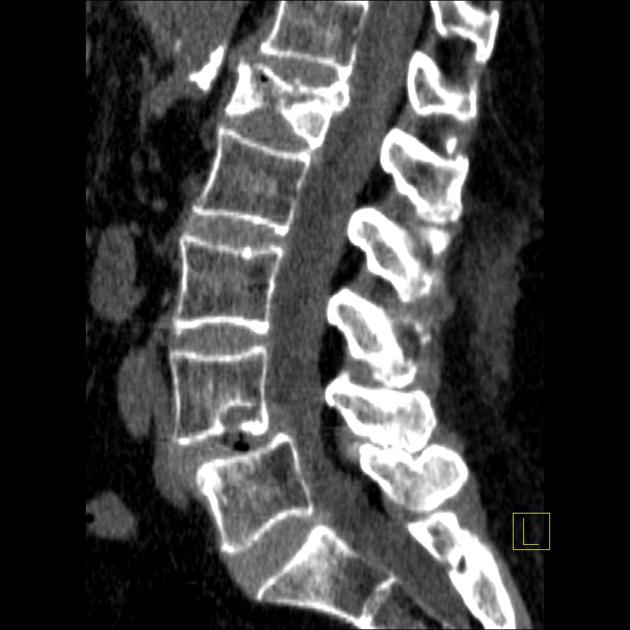
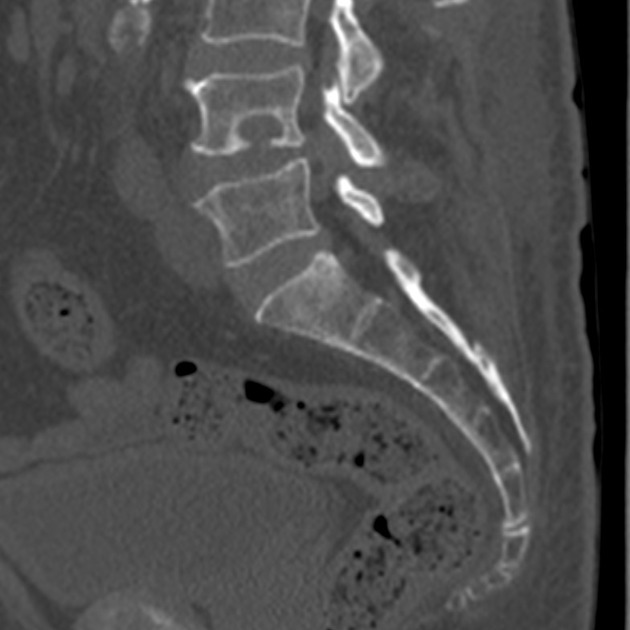
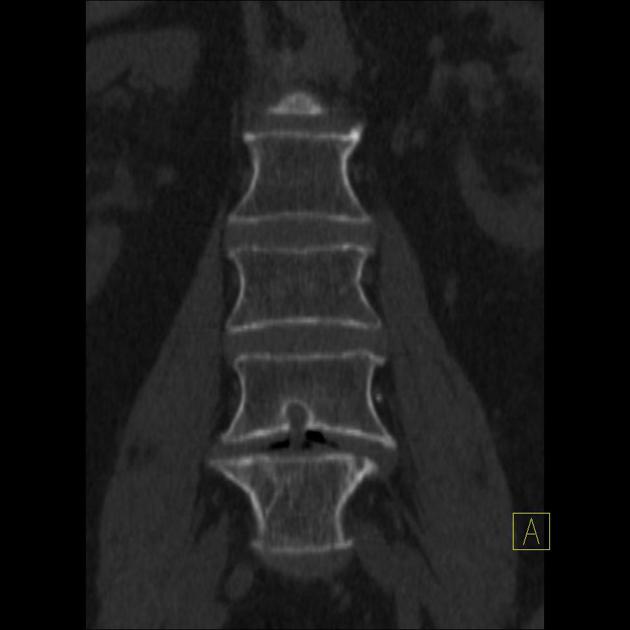
CT
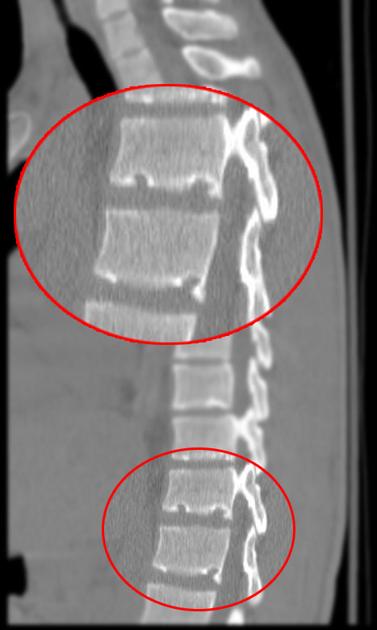
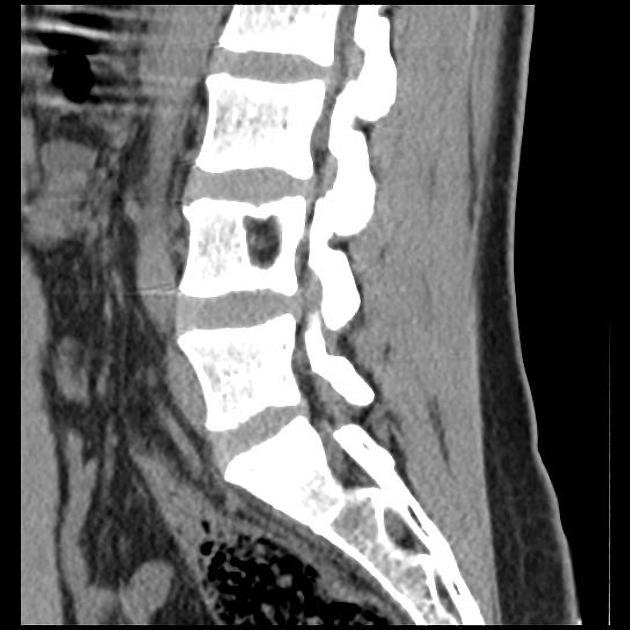
Schmorl nodes are better identified on CT images, showing the same pattern observed on radiographs.
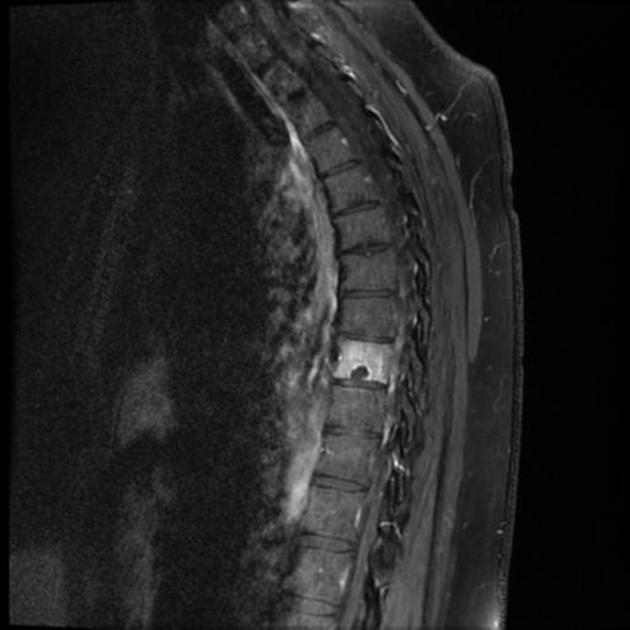
MRI
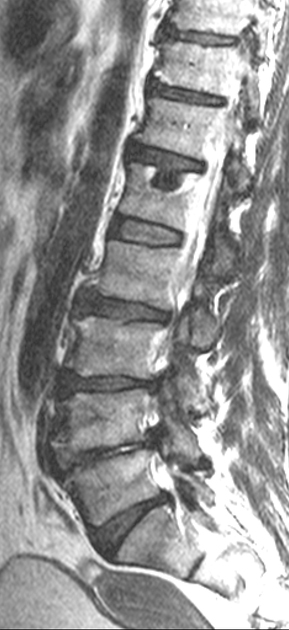
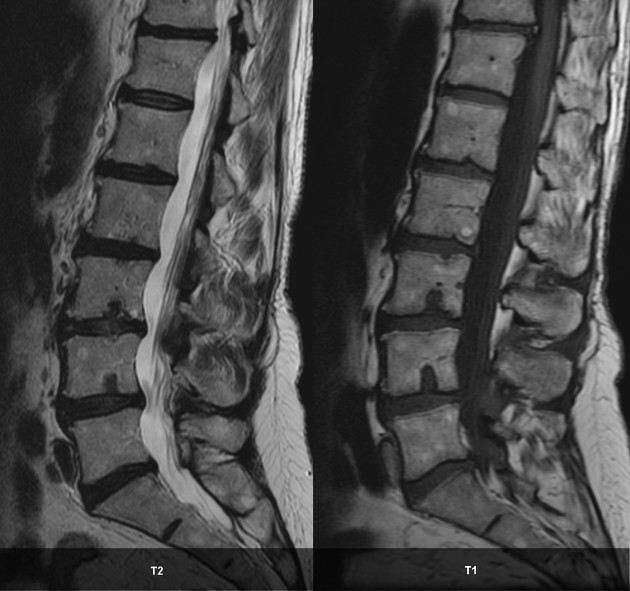
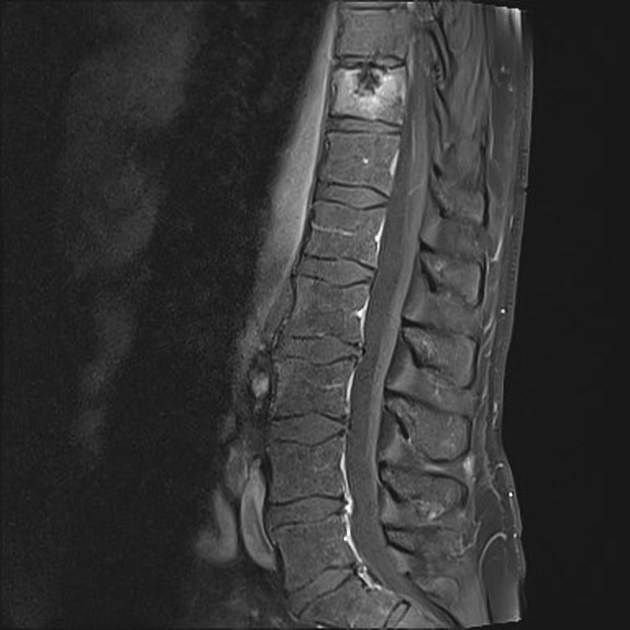
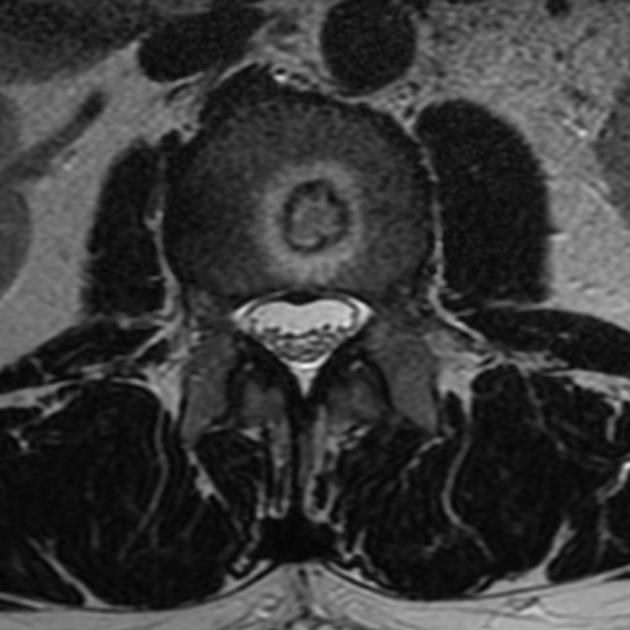
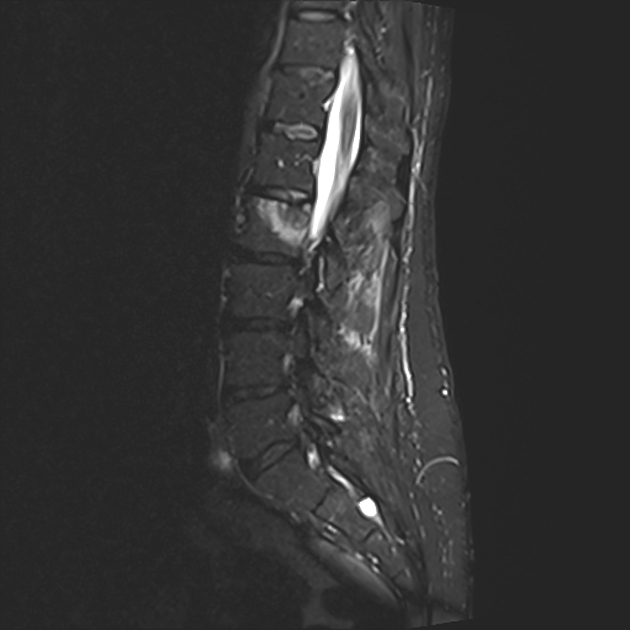
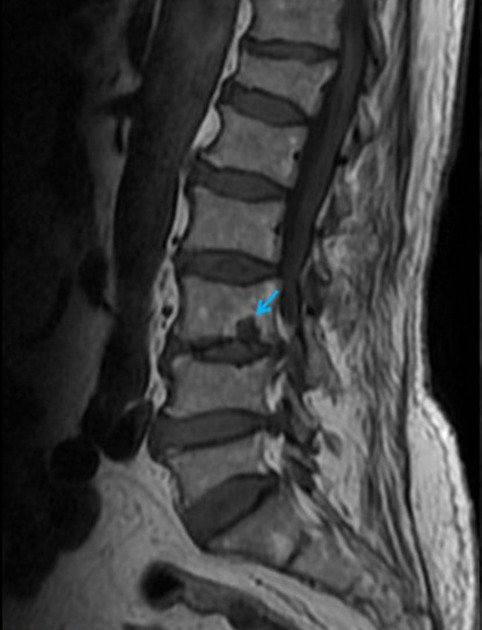
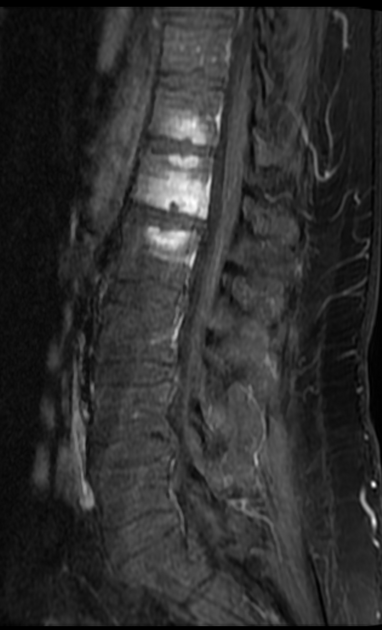
Schmorl nodes are best seen on the sagittal sequences and usually exhibit the same signal characteristics as the adjacent disc, with a thin rim of sclerosis at the margins.
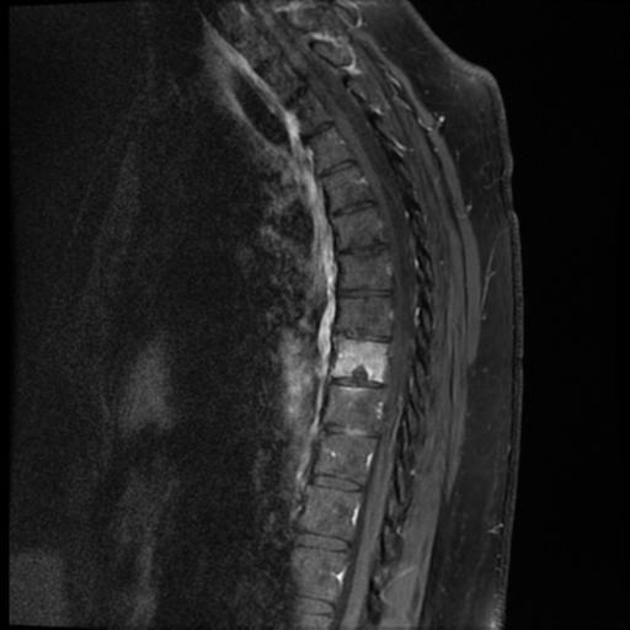
Acute herniation can appear more aggressive with surrounding bone marrow edema and peripheral enhancement 9. The gas extrusion sign may be present which refers to hypointensity in the intervertebral disc space across all pulse sequences 10. These acute features evolve gradually over months but may take over a year 9,10.
Nuclear medicine
FDG-PET
Acute Schmorl nodes have been reported to be FDG-PET avid 9.
History and etymology
It is named after Christian Georg Schmorl (1861-1932), a German pathologist who first described them in 1927 9.
Differential diagnosis
For chronic Schmorl nodes, there are few differentials as they have characteristic appearances.
For acute Schmorl nodes consider:
spondylodiscitis: compared with infection, acute Schmorl nodes will have more focal endplate changes, no fever, and no epidural or prevertebral phlegmonous changes 10
malignancy 9






 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.