Acute lymphoblastic leukemia (ALL) is a malignant disorder of the bone marrow characterized by the proliferation of the lymphoid progenitor cells, typically of the B cell lineage.
On this page:
Epidemiology
Acute lymphoblastic leukemia is the most common form of childhood leukemia, accounting for ~80% of pediatric leukemia cases 1. In adults, ALL corresponds to ~20% of leukemia cases 1. Peak age is between 3 and 7 years, with a second peak over 40 years.
Clinical presentation
The clinical features of acute lymphoblastic leukemia are non-specific. Children commonly have at least one pallor, fever, a palpable liver, a palpable spleen, or bruising on diagnosis 2. Other symptoms such as bone or joint pain, weight loss, anorexia, bleeding, abdominal pain and abdominal distension are also common.
Pathology
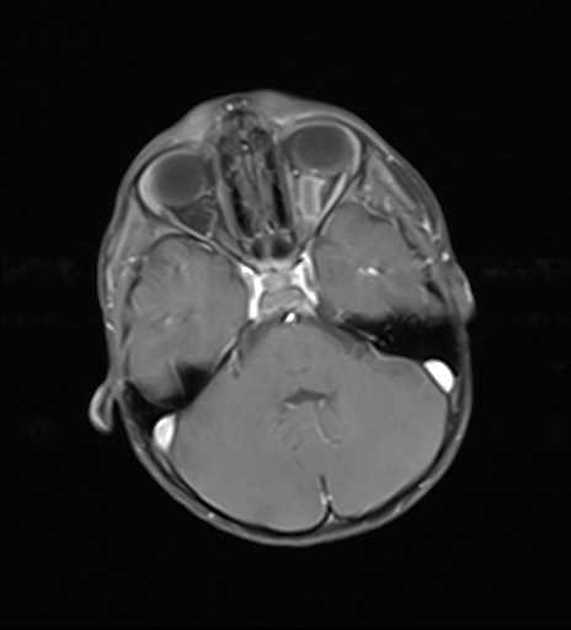
In acute lymphoblastic leukemia, the lymphoid progenitor cells, also known as lymphoblasts, do not mature due to abnormal expression of genes, often as a result of chromosomal abnormalities or chromosomal translocations (e.g. BCR-ABL1). The proliferation of the primitive cells takes up more and more marrow space at the expense of the normal hematopoietic elements, resulting in a decrease in the production of normal blood cells and bone marrow failure. Eventually, the lymphoblasts spill into the blood and can affect the liver, spleen, central nervous system, and lymph nodes.
Radiographic features
Plain radiograph
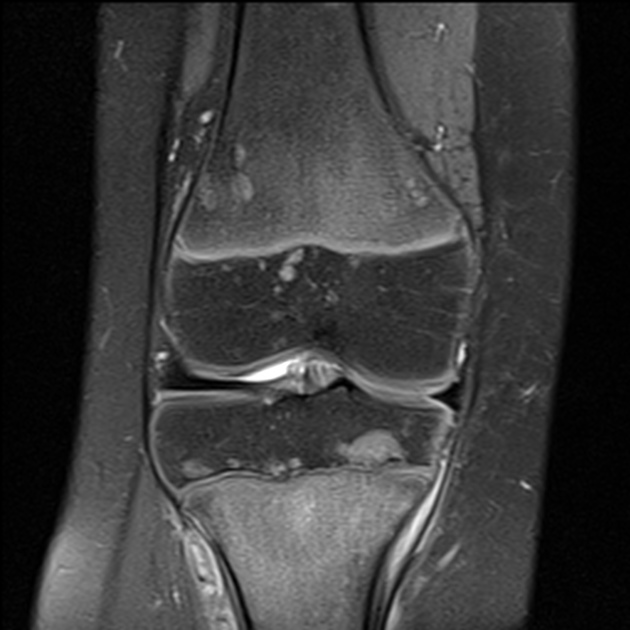
Bone lesions are common in leukemia. A metaphyseal radiolucent band is one of the most important radiological findings 3. Other radiological findings include subperiosteal new bone formation and osteolytic lesions involving the medullary cavity and cortex 1,3-5.
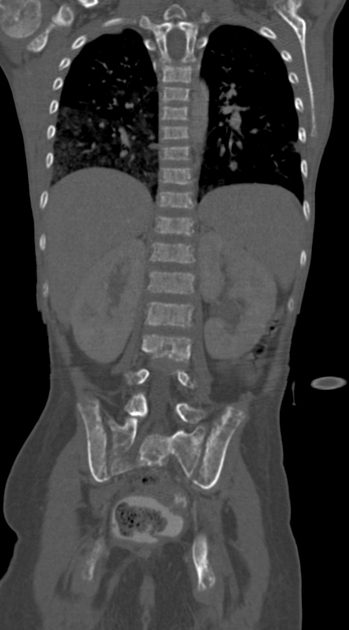
Chest radiographs may reveal a mediastinal mass.
Treatment and prognosis
The treatment for acute lymphoblastic leukemia typically has three phases:
induction therapy: combination chemotherapy is used to rapidly kill tumor cells to get the patient into remission
consolidation phase: if remission is achieved, further chemotherapy is given during this phase to treat the residual disease
-
maintenance phase: if the patient is still in remission after the consolidation phase, maintenance oral therapy is given
this may last up to three years if the patient remains in remission
The exact treatment regimens used in managing ALL are beyond the scope of this article, but depend on factors such as whether the disease is B or T cell ALL, and whether positive or negative for BCR-ABL1 fusion.
Pediatric patients with acute lymphoblastic leukemia have an overall five-year survival rate of 80% depending on their risk profile 6. However, only 30-40% of adults with ALL achieve long-term remission with the treatment regimens 7.
Differential diagnosis
For acute lymphoblastic leukemia bony abnormalities, consider:





 Unable to process the form. Check for errors and try again.
Unable to process the form. Check for errors and try again.